Abstract
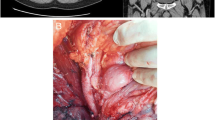
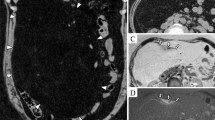
On computed tomography scanning, a 63-year-old man with vomiting and anorexia was discovered to have a mass in the pancreatic body and a retroperitoneal mass extending to the right lobe of the liver. An esophagogastroduodenoscopy revealed an advanced gastric carcinoma in the middle gastric body, and a biopsy specimen revealed a poorly differentiated adenocarcinoma. The pancreatic and retroperitoneal masses were considered metastatic lesions of gastric cancer, and a biopsy was taken from the pancreatic lesion using endoscopic ultrasound-guided fine-needle aspiration (EUS-FNA). The histology of the EUS-FNA pancreatic specimen revealed atypical spindle-shaped cells and increased stromal collagen fibrosis, and liposarcoma was considered. Conversely, a percutaneous ultrasound-guided biopsy was taken for the retroperitoneal lesion, and the histology revealed that it was a dedifferentiated liposarcoma. On the basis of histopathological and imaging findings, the retroperitoneal liposarcoma was identified as the primary lesion, the pancreatic lesion as a metastasis of the primary liposarcoma, and the gastric carcinoma as an independent tumor. As far as we know, there have only been three reports of metastatic pancreatic liposarcoma diagnosed via EUS-FNA. In this case, the patient also had gastric cancer, and EUS-FNA was helpful in differentiating metastatic pancreatic tumors from gastric cancer.







Similar content being viewed by others
Data Availability
We will provide data when requested by editors or readers, within the copyright of the journal.
References
Reddy S, Wolfgang LC. The role of surgery in the management of isolated metastases to the pancreas. Lancet Oncol. 2009;10:287–93.
Triantpoulou C, Kolliakou E, Karoumpalis I, et al. Metastatic disease to the pancreas: an imaging challenge. Insights Imaging. 2012;3:165–72.
Masetti M, Zanini N, Martuzzi F, et al. Analysis of prognostic factors in metastatic tumors of the pancreas; a single-center experience and review of the literature. Pancreas. 2010;39:135–43.
Wakatsuki T, Irisawa A, Bhutani MS, et al. Comparative study of diagnostic value of cytologic sampling by endoscopic ultrasonography-guided fine-needle aspiration and that by endoscopic retrograde pancreatography for the management of pancreatic mass without biliary stricture. J Gastroenterol Hepatol. 2005;20:1707–11.
Vilmann P, Jacobsen GK, Henriksen FW, et al. Endoscopic ultrasonography with guided fine needle aspiration biopsy in pancreatic disease. Gastrointest Endosc. 1992;38:172–3.
Sugimoto M, Takagi T, Hikichi T, et al. Conventional versus contrast-enhanced harmonic endoscopic ultrasonography-guided fine-needle aspiration for diagnosis of solid pancreatic lesions: a prospective randomized trial. Pancreatology. 2015;15:538–41.
Suzuki R, Takagi T, Sugimoto M, et al. Endoscopic ultrasound-guided fine needle aspiration for pancreatic cancer. Fukushima J Med Sci. 2018;64:111–5.
Banafea O, Mghanga PF, Zhao J, et al. Endoscopic ultrasonography with fine-needle aspiration for histological diagnosis of solid pancreatic masses: a meta-analysis of diagnostic accuracy studies. BMC Gastroenterol. 2016;16:108.
Carboni F, Ettorre GM, Lorusso R, et al. Isolated pancreatic metastasis of extremity myxoid liposarcoma: report of a case. Jpn J Clin Oncol. 2006;36:662–4.
Fabbri C, Luigiano C, Collina G, et al. EUS-FNA diagnosis of single pancreatic metastasis of liposarcoma. Gastrointest Endosc. 2009;69:974–6.
Varghese L, Ngae MY, Wilson AP, et al. Diagnosis of metastatic pancreatic mesenchymal tumors by endoscopic ultrasound-guided fine-needle aspiration. Diagn Cytopathol. 2009;37:792–802.
Hikichi T, Irisawa A, Bhutani MS, et al. Endoscopic ultrasound-guided fine-needle aspiration of solid pancreatic masses with rapid on-site cytological evaluation by endosonographers without attendance of cytopathologists. J Gastroenterol. 2009;44:322–8.
Adler H, Redmond CE, Heneghan HM, et al. Pancreatomy for metastatic disease: a systematic review. Eur J Surg Oncol. 2014;40:379–86.
Alomari AK, Ustun B, Aslanian HR, et al. Endoscopic ultrasound-guided fine-needle aspiration diagnosis of secondary tumors involving the pancreas: An institution’s experience. Cytojournal. 2016;13:1.
Gilbert CM, Monaco SE, Cooper ST, et al. Endoscopic ultrasound-guided fine-needle aspiration of metastases to the pancreas: a study of 25 cases. Cytojournal. 2011;8:7.
Smith AL, Odronic SI, Springer BS, et al. Solid tumor metastases to the pancreas diagnosed by FNA: a single-institution experience and review of the literature. Cancer Cytopathol. 2015;123:347–55.
Eloubeidi MA, Tamhane AR, Buxbaum JL. Unusual, metastatic, or neuroendocrine tumor of the pancreas: a diagnosis with endoscopic ultrasound guided fine-needle aspiration and immunohistochemistry. Saudi J Gastroenterol. 2012;18:99–105.
Matthyssens LE, Creytens D, Ceelen WP. Retroperitoneal liposarcoma: current insights in diagnosis and treatment. Front Surg. 2015;2:4.
Evans HL. Liposarcoma. A study of 55 cases with a reassessment of its classification. Am J Surg Pathol. 1979;3:507–23.
Dalal KM, Kattan MW, Antonescu CR, et al. Subtype specific prognostic nomogram for patients with primary liposarcoma of the retroperitoneum, extremity, or trunk. Ann Surg. 2006;244:381–91.
Singer S, Antonescu CR, Riedel E, et al. Histologic subtype and margin of resection predict pattern of recurrence and Survival for retroperitoneal liposarcoma. An Surg. 2003;238:358–71.
WHO Classification of tumours, 5th ed, vol 3, Soft Tissue and Bone Tumours (ed by WHO Classification of Tumours Editorial Board), IARC, Lyon, 2020.
Nijhuis PH, Sars PR, Plaat BE, et al. Clinico-pathological data and prognostic factors in completely resected AJCC stage I-III liposarcomas. Ann Surg Oncol. 2000;7:535–43.
Liu Z, Fan WF, Li GC, et al. Huge primary dedifferentiated pancreatic liposarcoma mimicking carcinosarcoma in a young female: a case report. World J Clin Cases. 2019;7:1344–50.
Naik PR, Kumar P, Kumar PV. Primary pleomorphic liposarcoma of liver: a rare case and review of the literature. Case Rep Hepatol. 2013;2013: 398910.
Terunuma Y, Takahashi K, Doi M, et al. Primary pleomorphic liposarcoma of the liver: a case report and literature review. Surg Case Rep. 2021;7:244.
Guellec SL, Chibon F, Ouali M, et al. Are peripheral purely undifferentiated pleomorphic sarcomas with MDM2 amplification dedifferentiated liposarcomas? Am J Surg Pathol. 2014;38:293–304.
Chen J, Hang Y, Gao Q, et al. Surgical diagnosis and treatment of primary retroperitoneal liposarcoma. Front Surg. 2021;8: 672669.
Henricks WH, Chu YC, Goldblum JR, et al. Dedifferentiated liposarcoma: a clinicopathological analysis of 155 cases with a proposal for an expanded definition of dedifferentiation. Am J Surg Pathol. 1997;21:271–81.
Thway K, Jones RL, Noujaim J, et al. Dediffarentiated liposarcoma: updates on morphology, genetics, and therapeutic strategies. Adv Anat Pathol. 2016;23:30–40.
Takahashi Y, Irisawa A, Bhutani MS, et al. Two cases of retroperitoneal liposarcoma diagnosed using endoscopic ultrasound-guided fine-needle aspiration (EUS-FNA). Diagn Ther Endosc. 2009;2009: 673194.
Acknowledgements
We would like to express our gratitude to the entire endoscopy medical staff for their assistance with the endoscopic procedures. Additionally, we are deeply grateful to Dr. Yasuko Murakawa of the Department of Cancer Chemotherapy, Miyagi Cancer Center, who was in charge of the patient’s chemotherapy and provided endoscopic images after chemotherapy.
Author information
Authors and Affiliations
Contributions
NA, TH, and YW conceived and designed this case report. NA, YW, YT, RK, TY, and HK performed the endoscopic procedures and patient management. Kazuo Watanabe conducted the pathological evaluation. NA, TH, and YW wrote the first draft of the manuscript. MK and HO commented on the previous version of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Naoto Abe, Takuto Hikichi, Yuichi Waragai, Yuta Takahashi, Ryoichiro Kobashi, Takumi Yanagita, Hiromi Kumakawa, Kazuo Watanabe, Masao Kobayakawa, and Hiromasa Ohira declare no conflicts of interest for this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Abe, N., Hikichi, T., Waragai, Y. et al. Retroperitoneal liposarcoma with pancreatic metastasis and gastric cancer: a case report. Clin J Gastroenterol 16, 164–170 (2023). https://doi.org/10.1007/s12328-022-01742-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-022-01742-1