Abstract
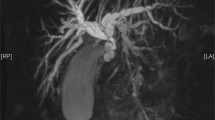
A 50-year-old woman was referred to our hospital for elevated hepatobiliary enzymes. She had a medical history of mastectomy for left breast invasive ductal carcinoma about 10 years ago, and no apparent recurrence had been observed. Contrast-enhanced computed tomography (CT) revealed soft-tissue shadows surrounding the portal vein, celiac artery, and other vessels. The lesions involved the hilar bile duct, and the upstream bile ducts were dilated. Endoscopic retrograde cholangiography showed an obstruction in the hilar bile duct, and biopsies were taken at the site of biliary stenosis. H&E staining showed that cells with strong nuclear atypia and prominent chromatin staining infiltrated in the stroma. Immunohistochemical analysis revealed that the cells were positive for CK7, GATA3 and weakly positive for CK20. Based on these results, we made the diagnosis of biliary stenosis due to retroperitoneal metastasis from breast invasive ductal carcinoma. Biliary inside stents were placed across the biliary stricture, and she received chemotherapy plus endocrine therapy for breast cancer. So far, the partial response has been maintained for 1 year since the diagnosis of retroperitoneal metastasis. Although retroperitoneal metastasis from breast cancer, especially breast invasive ductal carcinoma, is extremely rare, it could be a differential diagnosis for biliary stenosis.







Similar content being viewed by others
Abbreviations
- CT:
-
Computed tomography
- MRI:
-
Magnetic resonance imaging
- H & E:
-
Hematoxylin and eosin
- ERC:
-
Endoscopic retrograde cholangiography
- EUS:
-
Endoscopic ultrasonography
References
Chen ML, Ma ZS, Cao FL, et al. Retroperitoneal metastasis synchronous with brain and mediastinal lymph nodes metastasis from breast invasive ductal carcinoma as the first site of distant metastasis: a case report and review of literature Int J Clin Exp Pathol. 2020;13:1693–7.
Jibiki N, Shimizu Y, Hashimoto K, et al. Case of retroperitoneal metastasis of breast cancer with effective insertion of plural stents. Jpn J Cancer Chemother. 2018;45:2220–2.
Nihon-yanagi Y, Park Y, Ooshiro M, et al. A case of recurrent invasive lobular carcinoma of the breast found as metastasis to the duodenum. Breast Cancer. 2009;16:83–7.
Sugimoto H, Oda G, Yokoyama M, et al. Hydronephrosis caused by metastatic breast cancer. Case Rep Oncol. 2021;14:378–85.
Borst MJ, Ingold JA. Metastatic patterns of invasive lobular versus invasive ductal carcinoma of the breast. Surgery. 1993;114(4):637–42.
Harris M, et al. A comparison of the metastatic pattern of infiltrating lobular carcinoma and infiltrating duct carcinoma of the breast. Br J Cancer. 1984;50:23–30.
Winn JS, Baker MG, Fanous IS, et al. Lobular breast cancer and abdominal metastases: a retrospective review and impact on survival. Oncology. 2016;91:135–42.
Shakoor MT, Ayub S, Mohindra R, et al. Unique presentations of invasive lobular breast cancer: a case series. Int J Biomed Sci. 2014;10:287–93.
Cserni G. Histological type and typing of breast carcinomas and the WHO classification changes over time. Pathologica. 2020;112:25–41.
Arpino G. Infiltrating lobular carcinoma of the breast: tumor characteristics and clinical outcome. Breast Cancer Res. 2004;6:R149–56.
Lehr HA, Folpe A, Yaziji H, et al. Cytokeratin 8 immunostaining pattern and E-cadherin expression distinguish lobular from ductal breast carcinoma. Am J Clin Pathol. 2000;114:190–6.
Kim J, Hwang JH, Nam BD, et al. Mediastinal and retroperitoneal fibrosis as a manifestation of breast cancer metastasis: a case report and literature review. Medicine (Baltimore). 2018;97:e11842.
Carloss H, Saab G. Breast cancer and retroperitoneal metastasis. South Med J. 1980;73:1570–1.
Amir E, Miller N, Geddie W, et al. Prospective study evaluating the impact of tissue confirmation of metastatic disease in patients with breast cancer. J Clin Oncol. 2012;30:587–92.
Aurilio G, Monfardini L, Rizzo S, et al. Discordant hormone receptor and human epidermal growth factor receptor 2 status in bone metastases compared to primary breast cancer. Acta Oncol. 2013;52:1649–56.
Kocjan G, Smith AN. Bile duct brushings cytology: potential pitfalls in diagnosis. Diagn Cytopathol. 1997;16:358–63.
De Bellis M, Sherman S, Fogel EL, et al. Tissue sampling at ERCP in suspected malignant biliary strictures (part 1). Gastrointest Endosc. 2002;56:552–61.
Lee YN, Moon JH, Choi HJ, et al. Tissue acquisition for diagnosis of biliary strictures using peroral cholangioscopy or endoscopic ultrasound-guided fine-needle aspiration. Endoscopy. 2019;51:50–9.
Author information
Authors and Affiliations
Contributions
KM, MF, and YY participated in diagnosis and drafted this manuscript. AF and HS supervised this manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Kenta Mizukoshi, Misato Fujii, Yuki Yamauchi, Akihisa Fukuda, and Hiroshi Seno declare that they have no conflicts of interest in this article.
Human rights
All procedures followed have been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Informed consent
This study does not contain identifying information of the patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mizukoshi, K., Fujii, M., Yamauchi, Y. et al. A rare case of malignant biliary stenosis due to retroperitoneal metastasis from breast invasive ductal carcinoma. Clin J Gastroenterol 15, 199–204 (2022). https://doi.org/10.1007/s12328-021-01560-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-021-01560-x