Abstract
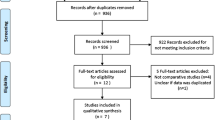
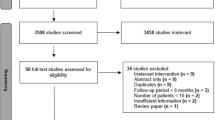
Metallic stents are being increasingly used for endoscopic drainage of peripancreatic fluid collections (PFCs) but their superiority over plastic stents has not been proven. We carried out a meta-analysis to consolidate the results from available studies and to suggest evidence-based recommendations. Studies that compared plastic and metallic stents for endoscopic drainage of PFCs and published before October 2016 were searched. Comparisons were performed for clinical success, adverse events, salvage interventions, mortality, technical success and recurrence. We included six studies with 856 patients (479 in the metallic stent group and 377 in the plastic stent group). The clinical success rate was significantly higher with metallic stents than with plastic stents (Mantel-Haenszel odds ratio [MH-OR] 3.22; 95% CI 1.87–5.54; P < 0.001). The rate of adverse events (MH-OR 0.40; 95% CI 0.24–0.65; P < 0.001) and the need for salvage procedures (MH-OR 0.31; 95% CI 0.13–0.70; P = 0.01) were also significantly lower with the use of metallic stents. Subgroup analysis for the type of PFC also found better results with the metallic stents. The results of Egger’s regression test (X-axis intercept at −0.63, P = 0.47) and funnel plot did not suggest any significant publication bias. We conclude that compared to plastic stents, the use of metallic stents for endoscopic drainage of PFCs is associated with significantly better clinical success and significantly lower rates of adverse events and the need for salvage procedures. However, further high-quality randomized trials are required to confirm these findings.









Similar content being viewed by others
References
Fotoohi M, D’Agostino HB, Wollman B, et al. Persistent pancreatocutaneous fistula after percutaneous drainage of pancreatic fluid collections: role of cause and severity of pancreatitis. Radiology. 1999;213:573–8.
Varadarajulu S, Bang JY, Sutton BS, et al. Equal efficacy of endoscopic and surgical cystogastrostomy for pancreatic pseudocyst drainage in a randomized trial. Gastroenterology. 2013;145:583–90.
Yamamoto N, Isayama H, Kawakami H, et al. Preliminary report on a new, fully covered, metal stent designed for the treatment of pancreatic fluid collections. Gastrointest Endosc. 2013;77:809–14.
Nelsen EM, Johnson EA, Walker AJ, et al. Endoscopic ultrasound-guided pancreatic pseudocyst cystogastrostomy using a novel self-expandable metal stent with antimigration system: a case series. Endosc Ultrasound. 2015;4:229–34.
Chandran S, Efthymiou M, Kaffes A, et al. Management of pancreatic collections with a novel endoscopically placed fully covered self-expandable metal stent: a national experience (with videos). Gastrointest Endosc. 2015;81:127–35.
Bapaye A, Itoi T, Kongkam P, et al. New fully covered large-bore wide-flare removable metal stent for drainage of pancreatic fluid collections: results of a multicenter study. Dig Endosc. 2015;27:499–504.
Bang JY, Hawes R, Bartolucci A, et al. Efficacy of metal and plastic stents for transmural drainage of pancreatic fluid collections: a systematic review. Dig Endosc. 2015;27:486–98.
Bang JY, Varadarajulu S. Metal versus plastic stent for transmural drainage of pancreatic fluid collections. Clin Endosc. 2013;46:500–2.
Lee BU, Song TJ, Lee SS, et al. Newly designed, fully covered metal stents for endoscopic ultrasound (EUS)-guided transmural drainage of peripancreatic fluid collections: a prospective randomized study. Endoscopy. 2014;46:1078–84.
Bapaye A, Dubale NA, Sheth KA, et al. Endoscopic ultrasonography-guided transmural drainage of walled-off pancreatic necrosis: comparison between a specially designed fully covered bi-flanged metal stent and multiple plastic stents. Dig Endosc. 2017; 29(1): 104−110.
Mukai S, Itoi T, Baron TH, et al. Endoscopic ultrasound-guided placement of plastic vs. biflanged metal stents for therapy of walled-off necrosis: a retrospective single-center series. Endoscopy. 2015;47:47–55.
Siddiqui AA, Kowalski TE, Loren DE, et al. Fully covered self-expanding metal stents versus lumen-apposing fully covered self-expanding metal stent versus plastic stents for endoscopic drainage of pancreatic walled-off necrosis: clinical outcomes and success. Gastrointest Endosc. 2017; 85(4): 758−765
Sharaiha RZ, DeFilippis EM, Kedia P, et al. Metal versus plastic for pancreatic pseudocyst drainage: clinical outcomes and success. Gastrointest Endosc. 2015;82:822–7.
Bang JY, Hasan MK, Navaneethan U, et al. Lumen-apposing metal stents for drainage of pancreatic fluid collections: when and for whom? Dig Endosc. 2017;29:83–90.
Kawakami H, Itoi T, Sakamoto N. Endoscopic ultrasound-guided transluminal drainage for peripancreatic fluid collections: where are we now? Gut Liver. 2014;8:341–55.
Varadarajulu S, Bang JY, Phadnis MA, et al. Endoscopic transmural drainage of peripancreatic fluid collections: outcomes and predictors of treatment success in 211 consecutive patients. J Gastrointest Surg. 2011;15:2080–8.
Siddiqui AA, Dewitt JM, Strongin A, et al. Outcomes of EUS-guided drainage of debris-containing pancreatic pseudocysts by using combined endoprosthesis and a nasocystic drain. Gastrointest Endosc. 2013;78:589–95.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Rajesh Panwar and Preet Mohinder Singh declare that they have no conflict of interest.
Human rights
All procedures followed have been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Informed consent
This study is a meta-analysis of already published studies and hence does not require informed consent.
Rights and permissions
About this article
Cite this article
Panwar, R., Singh, P.M. Efficacy and safety of metallic stents in comparison to plastic stents for endoscopic drainage of peripancreatic fluid collections: a meta-analysis and trial sequential analysis . Clin J Gastroenterol 10, 403–414 (2017). https://doi.org/10.1007/s12328-017-0763-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-017-0763-y