Abstract
Introduction
To describe anterior segment optical coherence tomography angiography (AS-OCTA) imaging to monitor corneal vascularisation (CoNV) and scar reduction after combined fine-needle diathermy (FND) with subconjunctival ranibizumab.
Methods
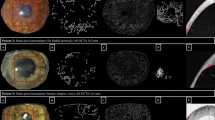
Prospective clinical study of six eyes from six subjects with corneal scar and CoNV which underwent combined FND with subconjunctival ranibizumab. All eyes were imaged using slit-lamp photography (SLP) and AS-OCTA (Optovue, Inc., Fremont, CA, wavelength: 840 nm) before and after the operation, with two independent masked assessors analysing all images. Main outcome measures were changes in median corneal scar area and vessel density (AS-OCTA) comparing pre- and postoperative imaging up to month 3 and 6.
Results
The mean age of the subjects was 60 ± 23 years, with three males and three females. CoNV and corneal scarring involving the visual axis were present in all eyes, secondary to previous infective keratitis (n = 3), severe blepharokeratoconjunctivitis (n = 2), or chemical injury (n = 1). Follow-up time frame ranged from 2 to 6 months postoperation. There was a reduction in median corneal scar area from 30.2 mm2 (IQR 18.7–38.5) before surgery to 14.8 mm2 (IQR 7.1–19.6) after surgery, with a median reduction of 37.1% (IQR = − 3.1–86.9, p = 0.046). There was also a reduction in median cornea vessel density (AS-OCTA) from 20.8% (IQR 16.1–20.8) before surgery to 17.6% (IQR 14.0–17.6) after surgery, with a median reduction of 15.1% (IQR 13.2–15.1, p < 0.001).
Conclusions
Combined imaging of SLP and AS-OCTA is useful for monitoring treatment response of corneal scarring and CoNV after combined FND with subconjunctival Ranibizumab.



Similar content being viewed by others
References
Azar DT. Corneal angiogenic privilege: angiogenic and antiangiogenic factors in corneal avascularity, vasculogenesis, and wound healing (an American Ophthalmological Society thesis). Trans Am Ophthalmol Soc. 2006;104:264–330.
Chang JH, Gabison EE, Kato T, Azar DT. Corneal neovascularization. Curr Opin Ophthalmol. 2001;12(4):242–9.
Feizi S, Azari AA, Safapour S. Therapeutic approaches for corneal neovascularization. Eye Vis (Lond). 2017;4:28.
Sharif Z, Sharif W. Corneal neovascularization: updates on pathophysiology, investigations & management. Rom J Ophthalmol. 2019;63(1):15–22.
Armitage WJ, Goodchild C, Griffin MD, Gunn DJ, Hjortdal J, Lohan P, Murphy CC, Pleyer U, Ritter T, Tole DM, Vabres B. High-risk corneal transplantation: Recent developments and future possibilities. Transplantation. 2019;103(12):2468.
Stevenson W, Cheng SF, Dastjerdi MH, Ferrari G, Dana R. Corneal neovascularization and the utility of topical VEGF inhibition: ranibizumab (Lucentis) vs bevacizumab (Avastin). Ocul Surf. 2012;10(2):67–83.
Pillai CT, Dua HS, Hossain P. Fine needle diathermy occlusion of corneal vessels. Invest Ophthalmol Vis Sci. 2000;41(8):2148–53.
Le VN, Hou Y, Bock F, Cursiefen C. Supplemental anti Vegf A-therapy prevents rebound neovascularisation after fine needle diathermy treatment to regress pathological corneal (LYMPH) angiogenesis. Sci Rep. 2020;10(1):1–8.
Koenig Y, Bock F, Kruse FE, Stock K, Cursiefen C. Angioregressive pretreatment of mature corneal blood vessels before keratoplasty: fine-needle vessel coagulation combined with anti-VEGFs. Cornea. 2012;31:887–92.
Elbaz U, Mireskandari K, Shen C, Ali A. Corneal fine needle diathermy with adjuvant bevacizumab to treat corneal neovascularization in children. Cornea. 2015;34(7):773–7.
Hussain R, Savant V. Fine-needle diathermy with simultaneous subconjunctival bevacizumab. Semin Ophthalmol. 2017;32(5):550–2.
Zou L, Lai H, Zhou Q, Xiao F. Lasting controversy on ranibizumab and bevacizumab. Theranostics. 2011;1:395.
Koenig Y, Bock F, Horn F, Kruse F, Straub K, Cursiefen C. Short-and long-term safety profile and efficacy of topical bevacizumab (Avastin®) eye drops against corneal neovascularization. Graefes Arch Clin Exp Ophthalmol. 2009;247(10):1375–82.
Gaudreault J, Fei D, Rusit J, Suboc P, Shiu V. Preclinical pharmacokinetics of Ranibizumab (rhuFabV2) after a single intravitreal administration. Invest Ophthalmol Vis Sci. 2005;46(2):726–33.
Ferrari G, Dastjerdi MH, Okanobo A, Cheng SF, Amparo F, Nallasamy N, Dana R. Topical ranibizumab as a treatment of corneal neovascularization. Cornea. 2013;32(7):992.
Chen Y, Wiesmann C, Fuh G, Li B, Christinger HW, McKay P, Vos AM, Lowman HB. Selection and analysis of an optimized anti-VEGF antibody: crystal structure of an affinity-matured Fab in complex with antigen. J Mol Biol. 1999;293:865–81.
Kim JH, Seo HW, Han HC, Lee JH, Choi SK, Lee D. The effect of bevacizumab versus ranibizumab in the treatment of corneal neovascularization: a preliminary study. Korean J Ophthalmol. 2013;27(4):235–42.
Cheng SF, Ferrari G, Okanobo A, et al. Sustained efficacy of topical bevacizumab in the treatment of corneal neovascularization (NV). Invest Ophthalmol Vis Sci. 2011;154(6):940–48.e1.
Anijeet DR, Zheng Y, Tey A, Hodson M, Sueke H, Kaye SB. Imaging and evaluation of corneal vascularization using fluorescein and indocyanine green angiography. Invest Ophthalmol Vis Sci. 2012;53:650–8.
Kirwan RP, Zheng Y, Tey A, Anijeet D, Sueke H, Kaye SB. Quantifying changes in corneal neovascularization using fluorescein and indocyanine green angiography. Am J Ophthalmol. 2012;154:850–8.
Di Lee W, Devarajan K, Chua J, Schmetterer L, Mehta JS, Ang M. Optical coherence tomography angiography for the anterior segment. Eye Vision. 2019;6(1):4.
Ong HS, Tey KY, Ke M, et al. A pilot study investigating anterior segment optical coherence tomography angiography as a non-invasive tool in evaluating corneal vascularisation. Sci Rep. 2021;11:1212.
Feizi S, Azari AA, Safapour S. Therapeutic approaches for corneal neovascularization. Eye Vision. 2017;4(1):28.
Ahn YJ, Hwang HB, Chung SK. Ranibizumab injection for corneal neovascularization refractory to bevacizumab treatment. Korean J Ophthalmol. 2014;28(2):177–80.
Sener E, Yuksel N, Yildiz DK, Yilmaz B, Ozdemir O, Caglar Y, Degirmenci E. The impact of subconjuctivally injected EGF and VEGF inhibitors on experimental corneal neovascularization in rat model. Curr Eye Res. 2011;36(11):1005–13.
Alldredge OC, Krachmer JH. Clinical types of corneal transplant rejection. Their manifestations, frequency, preoperative correlates, and treatment. Arch Ophthalmol. 1981;99:599–604.
Hos D, Le VN, Hellmich M, Siebelmann S, Roters S, Bachmann BO, Cursiefen C. Risk of corneal graft rejection after high-risk keratoplasty following fine-needle vessel coagulation of corneal neovascularization combined with bevacizumab: a pilot study. Transplant Direct. 2019;5(5):e452.
Le VN, Schneider AC, Scholz R, Bock F, Cursiefen C. Fine needle-diathermy regresses pathological corneal (lymph) angiogenesis and promotes high-risk corneal transplant survival. Sci Rep. 2018;8(1):1–8.
Oie Y, Nishida K. Evaluation of corneal neovascularization using optical coherence tomography angiography in patients with limbal stem cell deficiency. Cornea. 2017;36(Suppl 1):S72–5.
Cai Y, Del Barrio JL, Wilkins MR, Ang M. Serial optical coherence tomography angiography for corneal vascularization. Graefes Arch Clin Exp Ophthalmol. 2017;255(1):135–9.
Ang M, Baskaran M, Werkmeister RM, et al. Anterior segment optical coherence tomography. Prog Retin Eye Res. 2018;66:132–56. https://doi.org/10.1016/j.preteyeres.2018.04.002.
Fung SS, Stewart RM, Dhallu SK, Sim DA, Keane PA, Wilkins MR, Tuft SJ. Anterior segment optical coherence tomographic angiography assessment of acute chemical injury. Am J Ophthalmol. 2019;1(205):165–74.
Liu Z, Karp CL, Galor A, Bayyat GJ, Jiang H, Wang J. Role of optical coherence tomography angiography in the characterization of vascular network patterns of ocular surface squamous neoplasia. Ocular Surf. 2020. https://doi.org/10.1136/bjophthalmol-2015-307706.
Ang M, Cai Y, MacPhee B, Sim DA, Keane PA, Sng CC, Egan CA, Tufail A, Larkin DF, Wilkins MR. Optical coherence tomography angiography and indocyanine green angiography for corneal vascularisation. Br J Ophthalmol. 2016;100(11):1557–63.
Ang M, Cai Y, Shahipasand S, Sim DA, Keane PA, Sng CC, Egan CA, Tufail A, Wilkins MR. En face optical coherence tomography angiography for corneal neovascularisation. Br J Ophthalmol. 2016;100(5):616–21.
Faraj LA, Elalfy MS, Said DG, Dua HS. Fine needle diathermy occlusion of corneal vessels. Br J Ophthalmol. 2014;98(9):1287–90.
Acknowledgements
We thank Ms. Teo Kai Ying from Singapore Eye Research Institute for her assistance in obtaining the AS-OCTA images for the study.
Funding
This work was funded by grants from the National Medical Research Council (CG/C010A/2017; OFIRG/0048/2017; OFLCG/004c/2018), Singapore. Funding support from the Singapore Eye Research Institute was used to fund the Journal’s rapid service fee.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Author Contributions
Conceptualisation, methodology, and funding acquisition: M.A. Formal analysis and writing of manuscript: V.F, C.T. Image analysis: K.M.Y. Review and editing of the manuscript: M.A, J.M, and L.S.
Disclosures
Foo Hui Xian Valencia, Ke Mengyuan, Chelsea Tan Qiu Lin, Leopold Schmetterer, Jodhbir S Mehta, and Marcus Ang have nothing to disclose.
Compliance with Ethics Guidelines
Our study followed the principles of the Declaration of Helsinki of 1964, with approval obtained from the SingHealth ethics committee (IRB number: 2018/1435). Informed written consent was obtained from all study participants.
Data Availability
The datasets generated during and analysed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Foo, V.H.X., Ke, M., Tan, C.Q.L. et al. Anterior Segment Optical Coherence Tomography Angiography Assessment of Corneal Vascularisation After Combined Fine-Needle Diathermy with Subconjunctival Ranibizumab: A Pilot Study. Adv Ther 38, 4333–4343 (2021). https://doi.org/10.1007/s12325-021-01849-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-021-01849-w