Abstract
Introduction
Anemia is one of the most common complications of chronic kidney disease (CKD). As a result of the side effects of high doses of recombinant human erythropoietin (rhEPO) and the differences in the standard dose of the injectable iron, this study aimed to evaluate the effect of high and low intravenous iron supplementation on hematinic parameters and EPO requirements in patients under hemodialysis.
Methods
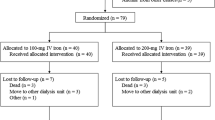
This multicenter, randomized, double-blind clinical trial was conducted on 60 patients with CKD admitted to Sina and 29 Bahman hospitals in Tabriz, Iran in 2019–2020 to undergo hemodialysis. In the two studied groups, low (100 mg/week) and high (400 mg/week) doses of iron were administered and subjects were followed up for 6 months. The incidence of acute myocardial ischemia, stroke, and mortality during 6 months was recorded.
Results
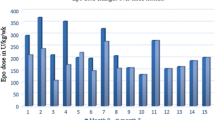
The required rhEPO dosage (mg/week) to maintain hemoglobin levels between 10 and 12 g/dL in the high-dose iron group was significantly decreased during the follow-up period (52,129.03 ± 23,810 vs. 45,760 ± 20,978.71, P ≤ 0.028). Transferrin saturation (TSAT) index had a significant upward trend after iron injection and significant correlations with the serum levels of Fe (r ≥ 0.353, P ≤ 0.007), ferritin (r ≥ 0.315, P ≤ 0.016), and total iron binding capacity (r ≥ 0.219, P < 0.050) during the follow-up period in the studied groups.
Conclusion
High-dose intravenous iron (400 mg/week) can reduce the mean dose of rhEPO requirements and increase the TSAT index over a period of 6 months in hemodialysis patients. High-dose IV iron administration can decrease cardiovascular events in hemodialysis patients with iron deficiency anemia.


Similar content being viewed by others
References
Cooper A, Mikhail A, Lethbridge MW, Kemeny DM, Macdougall IC. Pentoxifylline improves hemoglobin levels in patients with erythropoietin-resistant anemia in renal failure. J Am Soc Nephrol. 2004;15(7):1877–82. https://doi.org/10.1097/01.asn.0000131523.17045.56.
Shiferaw WS, Akalu TY, Aynalem YA. Risk factors for anemia in patients with chronic renal failure: a systematic review and meta-analysis. Ethiop J Health Sci. 2020;30(5):829–42. https://doi.org/10.4314/ejhs.v30i5.23.
Hanna RM, Streja E, Kalantar-Zadeh K. Burden of anemia in chronic kidney disease: beyond erythropoietin. Adv Ther. 2020;38(1):52–75.
Lankhorst CE, Wish JB. Anemia in renal disease: diagnosis and management. Blood Rev. 2010;24(1):39–47.
Ghasemi F, Abdi A, Salari N, Tohidi MR, Faraji A. Comparing the effects of intravenous and subcutaneous erythropoietin on blood indices in hemodialysis patients. Sci Rep. 2019;9(1):1–8.
Macdougall IC, Strauss WE, McLaughlin J, Li Z, Dellanna F, Hertel J. A randomized comparison of ferumoxytol and iron sucrose for treating iron deficiency anemia in patients with CKD. J Am Soc Nephrol. 2014;9(4):705–12. https://doi.org/10.1097/01.asn.0000131523.17045.56.
McMurray JJ, Parfrey PS, Adamson JW, et al. Kidney disease: improving global outcomes (KDIGO) anemia work group. KDIGO clinical practice guideline for anemia in chronic kidney disease. Kidney Int Supp. 2012;2(4):279–335.
Saglimbene V, Palmer SC, Craig JC, et al. Low versus high dose erythropoiesis-stimulating agents in hemodialysis patients with anemia: a randomized clinical trial. PLoS One. 2017;12(3):e0172735.
Gupta N, Wish JB. Erythropoietin and its cardiovascular effects. In: Rangaswami J, Lerma EV, Ronco C, editors. Cardio-nephrology. Cham: Springer; 2017. p. 119–28.
Macdougall IC, White C, Anker SD, et al. Randomized trial comparing proactive, high-dose versus reactive, low-dose intravenous iron supplementation in hemodialysis (PIVOTAL): study design and baseline data. Am J Nephrol. 2018;48(4):260–8.
Kim T, Streja E, Soohoo M, et al. Serum ferritin variations and mortality in incident hemodialysis patients. Am J Nephrol. 2017;46(2):120–30.
Kassianides X, Hazara AM, Bhandari S. Improving the safety of intravenous iron treatments for patients with chronic kidney disease. Expert Opin Drug Saf. 2021;20(1):23–35.
Thomas DR. Anemia and quality of life: unrecognized and undertreated. Oxford: Oxford University Press; 2004.
Winther S, Finer N, Sharma A, Torp-Pedersen C, Andersson C. Association of anemia with the risk of cardiovascular adverse events in overweight/obese patients. Int J Obes (Lond). 2014;38(3):432–7. https://doi.org/10.1038/ijo.2013.111.
Martinsson A, Andersson C, Andell P, Koul S, Engström G, Smith JG. Anemia in the general population: prevalence, clinical correlates and prognostic impact. Eur J Epidemiol. 2014;29(7):489–98. https://doi.org/10.1007/s10654-014-9929-9.
Streja E, Kovesdy CP, Greenland S, et al. Erythropoietin, iron depletion, and relative thrombocytosis: a possible explanation for hemoglobin-survival paradox in hemodialysis. Am J Kidney Dis. 2008;52(4):727–36. https://doi.org/10.1053/j.ajkd.2008.05.029.
Johnson DW, Pollock CA, Macdougall ICJN. Erythropoiesis-stimulating agent hyporesponsiveness. Nephrology (Carlton). 2007;12(4):321–30. https://doi.org/10.1111/j.1440-1797.2007.00810.x.
Ratcliffe LE, Thomas W, Glen J, et al. Diagnosis and management of iron deficiency in CKD: a summary of the NICE guideline recommendations and their rationale. Am J Kidney Dis. 2016;67(4):548–58. https://doi.org/10.1053/j.ajkd.2015.11.012.
Yamamoto H, Nishi S, Tomo T, et al. 2015 Japanese Society for Dialysis Therapy: guidelines for renal anemia in chronic kidney disease. Ren Replace Ther. 2017;3(1):1–46.
Sato M, Hanafusa N, Tsuchiya K, Kawaguchi H, Nitta K. Impact of transferrin saturation on all-cause mortality in patients on maintenance hemodialysis. Blood Pur. 2019;48(2):158–66.
Koo HM, Kim CH, Doh FM, et al. The relationship of initial transferrin saturation to cardiovascular parameters and outcomes in patients initiating dialysis. PLoS One. 2014;9(2):e87231.
Kuragano T, Joki N, Hase H, et al. Low transferrin saturation (TSAT) and high ferritin levels are significant predictors for cerebrovascular and cardiovascular disease and death in maintenance hemodialysis patients. PLoS One. 2020;15(9):e0236277.
Macdougall IC, White C, Anker SD, et al. Intravenous iron in patients undergoing maintenance hemodialysis. N Engl J Med. 2019;380(5):447–58. https://doi.org/10.1056/NEJMoa1810742.
Macdougall IC, Bhandari S, White C, et al. Intravenous iron dosing and infection risk in patients on hemodialysis: a prespecified secondary analysis of the PIVOTAL trial. J Am Soc Nephrol. 2020;31(5):1118–27. https://doi.org/10.1681/ASN.2019090972.
Hougen I, Collister D, Bourrier M, et al. Safety of intravenous iron in dialysis: a systematic review and meta-analysis. Clin J Am Soc Nephrol. 2018;13(3):457–67. https://doi.org/10.2215/CJN.05390517.
Kassianides X, Gordon A, Sturmey R, Bhandari S. The comparative effects of intravenous iron on oxidative stress and inflammation in patients with chronic kidney disease and iron deficiency: a randomized controlled pilot study. Kidney Res Clin Pract. 2021;40(1):89–98. https://doi.org/10.23876/j.krcp.20.120.
Karaboyas A, Morgenstern H, Pisoni RL, et al. Association between serum ferritin and mortality: findings from the USA, Japan and European Dialysis Outcomes and Practice Patterns Study. Nephrol Dial Transplant. 2018;33(12):2234–44. https://doi.org/10.1093/ndt/gfy190.
Daugirdas JT, Blake PG, Ing TS. Handbook of dialysis. Philadelphia: Lippincott Williams & Wilkins; 2012.
Acknowledgements
Funding
The authors thank the Kidney Research Center at Tabriz University of Medical Sciences for its support and assistance. No funding or sponsorship was received for this study or publication of this article.
Authorship
All authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published. All authors had full access to all of the data for this analysis and take complete responsibility for the integrity of the data and accuracy of the data analysis.
Authorship Contributions
Farahnoosh Farnood was involved in the conception and design of this study. Seyedeh Mina Hejazian and Saba Esmaeili collected the data. Sepideh Zununi Vahed and Seyedeh Mina Hejazian performed the data analysis and interpretation of results. Elham Ahmadian prepared the first draft of the manuscript. Sepideh Zununi Vahed and Farahnoosh Farnood did a critical revision of the manuscript. All authors read and approved the final manuscript.
Disclosures
Sepideh Zununi Vahed, Elham Ahmadian, Seyedeh Mina Hejazian, Saba Esmaeili, and Farahnoosh Farnood have nothing to disclose.
Compliance with Ethics Guidelines
This study was performed in accordance with the Helsinki Declaration of 1964 and its later amendments. This study was permitted by the Ethics Committee of Azad University of Tabriz branch (IR.IAU.TABRIZ.REC.1399.083). The study was registered with the Iran Clinical Trials Registry with identifier number IRCT20201108049311N1 (https://www.irct.ir). A consent form was signed by each of the participants and they were advised to use their regular medications during the study period.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zununi Vahed, S., Ahmadian, E., Hejazian, S.M. et al. The Impact of Intravenous Iron Supplementation on Hematinic Parameters and Erythropoietin Requirements in Hemodialysis Patients. Adv Ther 38, 4413–4424 (2021). https://doi.org/10.1007/s12325-021-01826-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-021-01826-3