Abstract
Introduction
Ivabradine has opened up new possibilities for treating stable angina and chronic heart failure by lowering heart rate. Ivabradine lowers heart rate by selectively inhibiting the I f current in the sinoatrial node. This study aimed to determine whether the decrease in heart rate achieved with ivabradine was accompanied by hemodynamic changes that might lead to an enhancement of endothelial function.
Methods
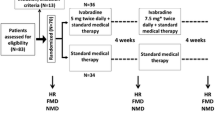
Thirty patients with stable angina pectoris were included in the study. Ivabradine (5 mg bid) was added to the recommended standard treatment. Endothelial function was assessed at baseline and after 3 months of ivabradine therapy, with an Endo-PAT 2000 device (Itamar Medical, Israel). This device was recently developed for the noninvasive assessment for endothelial dysfunction. We evaluated reactive hyperemia index (RHI), which reflects endothelial function, and augmentation index (AI), which provides an indication of arterial stiffness.
Results
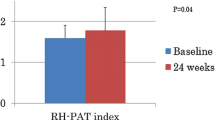
The study population consisted of 25 (83.3%) men and five (16.7%) women. The mean age of the patients was 65.4 ± 6.7 years. Twenty-eight (93.3%) patients had a history of myocardial infarction (ST-segment elevation myocardial infarction or non-ST-segment elevation myocardial infarction), 23 (76.6%) had undergone revascularization (percutaneous coronary intervention or coronary artery bypass graft), 16 (53.3%) had type 2 diabetes mellitus, and 29 (96.6%) had arterial hypertension. The mean resting heart rate decreased significantly, from 77 ± 7 bpm at the start of the study to 65 ± 6 bpm after treatment (P < 0.0001). Endothelial function was found to have improved significantly after 3 months of ivabradine therapy. Mean RHI before treatment was 1.54 ± 0.30, suggesting probable endothelial dysfunction, whereas mean RHI at the end of the study was 1.83 ± 0.36 (P < 0.0001). AI also improved significantly on treatment, from 21 ± 20% to 10 ± 21% (P < 0.0001).
Conclusion
The addition of ivabradine to the treatment regimen of patients with stable angina pectoris both lowered heart rate and improved endothelial function. However, broader, randomized, double-blind, placebo-controlled clinical trials are required to confirm these findings.
Funding
Sponsorship for this study was funded by a VEGA grant no. 1/0858/11. Article processing charges were funded by Servier.



Similar content being viewed by others
References
Thollon C, Cambarrat C, Vian J, et al. Electrophysiological effects of S 16257, a novel sino-atrial node modulator, on rabbit and guinea-pig cardiac preparations: comparison with UL-FS 49. Br J Pharmacol. 1994;112(1):37–42.
Montalescot G, Sechtem U, Achenbach S, et al. ESC Guidelines on the management of stable coronary artery disease. The Task Force on the Management of Stable Coronary Artery Disease of the European Society of Cardiology. Eur Heart J. 2013;34(38):2949–3003.
Tardif JC, Ford I, Tendera M, et al. Efficacy of ivabradine, a new selective If inhibitor, compared with atenolol in patients with chronic stable angina. Eur Heart J. 2005;26(23):2529–36.
Tardif JC, Ponikowski P, Kahan T, et al. Efficacy of the If current inhibitor ivabradine in patients with chronic stable angina receiving beta-blocker therapy: a 4-month, randomized, placebo-controlled trial. Eur Heart J. 2009;30(5):540–8.
Fox K, Ford I, Steg PG, et al. Ivabradine for patients with stable coronary artery disease and left-ventricular systolic dysfunction (BEAUTIFUL): a randomised, double-blind, placebo-controlled trial. Lancet. 2008;372(9641):807–16.
Heusch G. Heart rate in the pathophysiology of coronary blood flow and myocardial ischaemia: benefit from selective bradycardic agents. Br J Pharmacol. 2008;153(8):1589–601.
Custodis F, Schirmer SH, Baumhäkel M, et al. Vascular pathophysiology in response to increased heart rate. J Am Coll Cardiol. 2010;56(24):1973–83.
Itamar Medical User Manual, Software version 3.2.4. Available online. http://www.itamar-medical.com/images/Endo_PAT%20user%20manual%20for%203%202%204.pdf. Accessed 15 Jan 2012.
Hamburg NM, Keyes MJ, Larson MG, et al. Cross-sectional relations of digital vascular function to cardiovascular risk factors in the Framingham heart study. Circulation. 2008;117:2467–74.
Bonetti PO, Pumper GM, Higano ST, et al. Noninvasive identification of patients with early coronary atherosclerosis by assessment of digital reactive hyperemia. J Am Coll Cardiol. 2004;44(11):2137–41.
Ferré R, Plana N, Merino J, et al. Effects of therapeutic lifestyle changes on peripheral artery tonometry in patients with abdominal obesity. Nutr Metab Cardiovasc Dis. 2010;22(2):95–105. doi:10.1016/j.numecd.2010.04.008.
Lian BQ, Keaney JF Jr. Predicting ischemic heart disease in women: the value of endothelial function. J Am Coll Cardiol. 2010;55(16):1688–96.
Rubinshtein R, Kuvin JT, Soffler M, et al. Assessment of endothelial function by noninvasive peripheral arterial tonometry predicts late cardiovascular adverse events. EHJ. 2010;31(9):1142–8.
Moerland M, Kales AJ, Schrier L, et al. Evaluation of the EndoPAT as a tool to assess endothelial fuction. Int J Vasc Med. 2012;2012:904141.
Woo JS, Jang WS, Kim HS, et al. Comparison of peripheral arterial tonometry and flow-mediated vasodilation for assessment of the severity and complexity of coronary artery disease. Coron Artery Dis. 2014;25(5):421–6.
Suessenbacher A, Dorler J, Wanitschek M, et al. Prognostic value of peripheral arterial tonometry in patients with coronary artery disease and a high cardiovascular risk profile. J Atheroscler Thromb. 2014;21:230–8.
Jochmann N, Schröter F, Knebel F, et al. Effect of ivabradine-induced heart rate reduction on flow-mediated dilatation measured with high-sensitivity ultrasound in patients with stable coronary heart disease. Cardiovasc Ultrasound. 2014;12:5.
Nerla R, Di Franco A, Milo M, et al. Differential effects of heart rate reduction by atenolol or ivabradine on peripheral endothelial function in type 2 diabetic patients. Heart. 2012;98(24):1812–6.
Villano A, Di Franco A, Nerla R, et al. Effects of ivabradine and ranolazine in patients with microvascular angina pectoris. Am J Cardiol. 2013;112(1):8–13.
Skalidis EI, Hamilos MI, Chlouverakis G, Zacharis EA, Vardas PE. Ivabradine improves coronary flow reserve in patients with stable coronary artery disease. Atherosclerosis. 2011;215(1):160–5.
Gloekler S, Traupe T, Stoller M, Schild D, Steck H, Khattab A, Vogel R, Seiler C. The effect of heart rate reduction by ivabradine on collateral function in patients with chronic stable coronary artery disease. Heart. 2014;100(2):160–6.
Reil JC, Tardif JC, Ford I, Lloyd SM, O’Meara E, Komajda M, Borer JS, Tavazzi L, Swedberg K, Böhm M. Selective heart rate reduction with ivabradine unloads the left ventricle in heart failure patients. J Am Coll Cardiol. 2013;62(21):1977–85.
Reil JC, Hohl M, Reil GH, Granzier HL, Kratz MT, Kazakov A, Fries P, Müller A, Lenski M, Custodis F, Gräber S, Fröhlig G, Steendijk P, Neuberger HR, Böhm M. Heart rate reduction by If-inhibition improves vascular stiffness and left ventricular systolic and diastolic function in a mouse model of heart failure with preserved ejection fraction. Eur Heart J. 2013;34(36):2839–49.
Albaladejo P, Carusi A, Apartian A, Lacolley P, Safar ME. BenetosA. Effect of chronic heart rate reduction with ivabradine on carotid and aortic structure and function in normotensive and hypertensive rats. J Vasc Res. 2003;40:320–8.
Albaladejo P, Challande P, Kakou A, et al. Selective reduction of heart rate by ivabradine: effect on the visco-elastic arterial properties in rats. J Hypertens. 2004;22:1739–45.
Volterrani M, Cice G, Caminiti G, et al. Effect of Carvedilol, Ivabradine or their combination on exercise capacity in patients with Heart Failure (the CARVIVA HF trial). Int J Cardiol. 2011;151(2):218–24.
Heusch G, Skyschally A, Gres P, et al. Improvement of regional myocardial blood flow and function and reduction of infarct size with ivabradine: protection beyond heart rate reduction. Eur Heart J. 2008;29(18):2265–75.
Drouin A, Gendron ME, Thorin E, et al. Chronic heart rate reduction by ivabradine prevents endothelial dysfunction in dyslipidaemic mice. Br J Pharmacol. 2008;154(4):749–57.
Custodis F, Baumhäkel M, Schlimmer N, et al. Heart rate reduction by ivabradine reduces oxidative stress, improves endothelial function, and prevents atherosclerosis in apolipoprotein E-deficient mice. Circulation. 2008;117(18):2377–87.
Schirmer SH, Baumhakel M, Custodis F, et al. Heart-rate reduction by If-channel inhibition with ivabradine restores collateral artery growth in hypercholesterolemic atherosclerosis. Eur Heart J. 2012;33(10):1223–31.
Heusch G, Skyschally A, Schulz R. Cardioprotection by ivabradine through heart rate reduction and beyond. J Cardiovasc Pharmacol Ther. 2011;16:281–4.
Canet E, Lerebours G, Vilaine JP. Innovation in coronary artery disease and heart failure: clinical benefits of pure heart rate reduction with ivabradine. Ann N Y Acad Sci. 2011;1222:90–9.
Ferrari R, Campo G, Gardini E, et al. Specific and selective If inhibition: expected clinical benefits from pure heart rate reduction in coronary patients. Eur Heart J Suppl. 2005;7(suppl H):H16–21.
Acknowledgments
Sponsorship for this study was funded by a VEGA grant no. 1/0858/11. Article processing charges were funded by Servier. All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval to the version to be published.
Disclosures
L Jedlickova, L. Merkovska, L. Jackova, M. Janicko, J. Fedacko, B. Novakova, D. Pella, A. Chmelarova, J. Majernik have nothing to disclose.
Compliance with ethics guidelines
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964, as revised in 2013. Informed consent was obtained from all patients for being included in the study.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Jedlickova, L., Merkovska, L., Jackova, L. et al. Effect of Ivabradine on Endothelial Function in Patients with Stable Angina Pectoris: Assessment with the Endo-PAT 2000 Device. Adv Ther 32, 962–970 (2015). https://doi.org/10.1007/s12325-015-0253-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-015-0253-x