Abstract
Introduction
Despite recent advances in endoscopic and pharmacological management, nonvariceal upper gastrointestinal bleeding (NVUGIB) is still associated with considerable mortality and morbidity that vary between countries. The European Survey of Nonvariceal Upper Gastrointestinal Bleeding (ENERGiB) reported clinical outcomes across Europe (Belgium, Greece, Italy, Norway, Portugal, Spain, and Turkey) and evaluated management strategies in a “real-world” European setting. This article presents the differences in clinical management strategies among countries participating in ENERGiB.
Methods
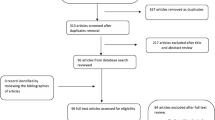
Adult patients consecutively presenting with overt NVUGIB at 123 participating hospitals over a 2-month period were included. Data relevant to the initial NVUGIB episode and for up to 30 days afterwards were collected retrospectively from patient medical records.
Results
The number of evaluable patients was 2,660; patient demographics and clinical characteristics were similar across countries. There was wide between-country variability in the area and speciality of the NVUGIB management team and unit transfer rates after the initial hospital assessment. The mean time from admission to endoscopy was <1 day only in Italy and Spain. Wide variation in the use of preendoscopy (35.0–88.7%) and relatively consistent (86.5–96.0%) postendoscopic pharmacological therapy rates were observed. There was substantial by-country variability in the rate of therapeutic procedures performed during endoscopy (24.9–47.6%). NVUGIB-related healthcare resource consumption was high and variable (days hospitalized, mean 5.4–8.7 days; number of endoscopies during hospitalization, mean 1.1–1.7).
Conclusions
ENERGiB demonstrates that there are substantial differences in the management of patients with acute NVUGIB episodes across Europe, and that in many cases the guideline recommendations for the management of NVUGIB are not being followed.
Similar content being viewed by others
References
Lewis JD, Bilker WB, Brensinger C, et al. Hospitalization and mortality rates from peptic ulcer disease and GI bleeding in the 1990s: relationship to sales of nonsteroidal anti-inflammatory drugs and acid suppression medications. Am J Gastroenterol. 2002;97:2540–2549.
Lassen A, Hallas J, Schaffalitzky de Muckadell OB. Complicated and uncomplicated peptic ulcers in a Danish county 1993–2002: a population-based cohort study. Am J Gastroenterol. 2006;101:945–953.
van Leerdam ME, Vreeburg EM, Rauws EA, et al. Acute upper GI bleeding: did anything change? Time trend analysis of incidence and outcome of acute upper GI bleeding between 1993/1994 and 2000. Am J Gastroenterol. 2003;98:1494–1499.
Zhao Y, Encinosa W. Hospitalizations for Gastrointestinal Bleeding in 1998 and 2006. HCUP Statistical Brief #65, 2008. Available at: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb65.pdf. Accessed Aug 24 2012.
Targownik LE, Nabalamba A. Trends in management and outcomes of acute nonvariceal upper gastrointestinal bleeding: 1993–2003. Clin Gastroenterol Hepatol. 2006;4:1459–1466.
Barkun A, Sabbah S, Enns R, et al. The Canadian Registry on Nonvariceal Upper Gastrointestinal Bleeding and Endoscopy (RUGBE): endoscopic hemostasis and proton pump inhibition are associated with improved outcomes in a real-life setting. Am J Gastroenterol. 2004;99:1238–1246.
Loperfido S, Baldo V, Piovesana E, et al. Changing trends in acute upper-GI bleeding: a populationbased study. Gastrointest Endosc. 2009;70:212–224.
Muller T, Barkun AN, Martel M. Non-variceal upper GI bleeding in patients already hospitalized for another condition. Am J Gastroenterol. 2009;104:330–339.
Cipolletta L, Bianco MA, Rotondano G, et al. Outpatient management for low-risk nonvariceal upper GI bleeding: a randomized controlled trial. Gastrointest Endosc. 2002;55:1–5.
Marmo R, Koch M, Cipolletta L, et al. Predictive factors of mortality from nonvariceal upper gastrointestinal hemorrhage: a multicenter study. Am J Gastroenterol. 2008;103:1639–1647.
Sandel MH, Kolkman JJ, Kuipers EJ, et al. Nonvariceal upper gastrointestinal bleeding: differences in outcome for patients admitted to internal medicine and gastroenterological services. Am J Gastroenterol. 2000;95:2357–2362.
Viviane A, Alan BN. Estimates of costs of hospital stay for variceal and nonvariceal upper gastrointestinal bleeding in the United States. Value Health. 2008;11:1–3.
Sung JJ, Tsoi KK, Ma TK, et al. Causes of mortality in patients with peptic ulcer bleeding: a prospective cohort study of 10,428 cases. Am J Gastroenterol. 2010;105:84–89.
Lau JY, Sung J, Hill C, et al. Systematic review of the epidemiology of complicated peptic ulcer disease: incidence, recurrence, risk factors and mortality. Digestion. 2011;84:102–113.
Lanas A, Aabakken L, Fonseca J, et al. Clinical predictors of poor outcomes among patients with nonvariceal upper gastrointestinal bleeding in Europe. Aliment Pharmacol Ther. 2011;33:1225–1233.
Rockall TA, Logan RF, Devlin HB, et al. Risk assessment after acute upper gastrointestinal haemorrhage. Gut. 1996;38:316–321.
Blatchford O, Murray WR, Blatchford M. A risk score to predict need for treatment for upper-gastrointestinal haemorrhage. Lancet. 2000;356:1318–1321.
Barkun AN, Bardou M, Kuipers EJ, et al. International consensus recommendations on the management of patients with nonvariceal upper gastrointestinal bleeding. Ann Intern Med. 2010;152:101–113.
Al-Sabah S, Barkun AN, Herba K, et al. Costeffectiveness of proton-pump inhibition before endoscopy in upper gastrointestinal bleeding. Clin Gastroenterol Hepatol. 2008;6:418–425.
Tsoi KK, Lau JY, Sung JJ. Cost-effectiveness analysis of high-dose omeprazole infusion before endoscopy for patients with upper-GI bleeding. Gastrointest Endosc. 2008;67:1056–1063.
Author information
Authors and Affiliations
Corresponding author
Additional information
To view enhanced content go to www.advancesintherapy.com
Address at time of study
Rights and permissions
About this article
Cite this article
Lanas, A., Aabakken, L., Fonseca, J. et al. Variability in the Management of Nonvariceal Upper Gastrointestinal Bleeding in Europe: An Observational Study. Adv Therapy 29, 1026–1036 (2012). https://doi.org/10.1007/s12325-012-0069-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-012-0069-x