Abstract
Introduction
A sharp increase in blood pressure, increase in atrial pressure and atrial strain, left ventricular diastolic dysfunction, and left ventricular hypertrophy (LVH) lead to heterogeneity and instability in atrial conduction. The resulting physiopathological situation may elevate maximum Pwave duration (Pmax) and P-wave dispersion (PWD) in electrocardiography. The objective of our study was to explore the effect of the sudden change in atrial hemodynamics on Pmax and PWD, which may indicate the risk of atrial fibrillation (AF) development in hypertensive urgency.
Methods
The study included patients diagnosed as hypertensive urgency (systolic blood pressure ≥180 mmHg, diastolic blood pressure ≥110 mmHg). Nitroprusside was started at a dose of 0.2 μg/kg/min, and the ensuing dose was arranged according to blood pressure. Echocardiography and electrocardiography were used to noninvasively measure changes in diastolic function and PWD and Pmax, respectively.
Results
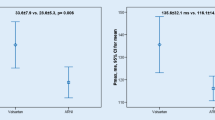
The study enrolled 102 patients (mean age 57.9±11.6 years; 32 [31.4%] males, and 70 [68.6%] females). Pmax decreased from 99.9±11.1 msec (95% confidence intervals [CI] 97.7, 102) to 88.5±9.3 msec (95% CI 86.6, 90.3) (P<0.001), while PWD decreased from 60.1±7.4 msec (95% CI 58.7, 61.6) to 43.9±6.7 msec (95% CI 42.5, 45.2) (P<0.001). In addition, most patients had LVH and diastolic dysfunction. After nitroprusside treatment improvements in indicators of diastolic functions such as E/A ratio, deceleration time, and isovolumetric relaxation time were observed.
Conclusion
The change observed in Pmax and PWD in hypertensive urgency may be associated with the rapid change in blood pressure and atrial strain, sympathetic nervous system activation, relative myocardial ischemia, and left ventricular diastolic dysfunction. Rapid regulation of blood pressure with nitroprusside brought about a marked decrease in Pmax and PWD in our patients. This improvement was interpreted as atrial conduction acquiring a stable and homogeneous character, which may reduce the risk of AF development in hypertensive urgency.
Similar content being viewed by others

References
Kaplan NM. Primary hypertension: natural history, special population and evaluation. In: Kaplan NM. Clinical Hypertension. Baltimore, MD: Williams & Wilkins; 1998:101–132.
Kincaid-Smith P, McMichael J, Murphy EA. The clinical course and pathology of hypertension with papilledema (malignant hypertension). Q J Med. 1958;27:117–153.
Bechgaard P, Kopp H, Nielson J. One thousand hypertensive patients followed from 16–22 years. Acta Med Scand Suppl. 1956;312:175–184.
Kannel WB, Wolf PA, Benjamin EJ, Levy D. Prevalence, incidence, prognosis and predisposing conditions for atrial fibrillation: population-based estimates. Am J Cardiol. 1998;82:2N–9N.
Levy S. Factors predisposing to the development of atrial fibrillation. Pacing Clin Electrophysiol. 1997;20:2670–2674.
Cha YM, Redfield MM, Shen WK, Gersh BJ. Atrial fibrillation and ventricular dysfunction: a vicious electromechanical cycle. Circulation. 2004;109:2839–2843.
Aytemir K, Amasyali B, Abali G, et al The signal-averaged P-wave duration is longer in hypertensive patients with history of paroxysmal atrial fibrillation as compared to those without. Int J Cardiol. 2005;103: 37–40.
Yilmaz R, Demirbag R. P-wave dispersion in patients with stable coronary artery disease and its relationship with severity of the disease. J Electrocardiol. 2005;38:279–284.
Tukek T, Akkaya V, Demirel S, et al Effect of valsalva maneuver on surface electrocardiographic P-wave dispersion in paroxysmal atrial fibrillation. Am J Cardiol. 2000;85:896–899.
Murphy J, Lavie CJ, Bresnahan DR. Nitroprusside. Messerli FH, ed. Cardiovascular Drug Therapy. 2nd edition. New Orleans, LA: W.B. Saunders Company; 1998:858–865.
Rogers EW, Feigenbaum H, Weyman AE. Echocardiography for quantification of cardiac chambers. In: Yu PN, Goodwin JF, eds. Progress in Cardiology. Philadelphia, PA: Lea & Febiger; 1979:807.
Folland ED, Parisi EF, Moynihan PF, Jones DR, Feldman CL, Tow D. Assessment of left ventricular ejection fractions by realtime, two-dimensional echocardiography. A comparison of cineangiographic and radionuclide techniques. Circulation. 1979;60:760–766.
European Study Group on Diastolic Heart Failure Working Group. How to diagnose diastolic heart failure. Eur Heart J. 1998;19:990–1003.
Devereux RB, Reichek N. Echocardiographic determination of left ventricular mass in man. Anatomic validation of the method. Circulation. 1977;55:613–618.
Devereux RB, De simone G, Schlussel CY. Echocardiographic left ventricular mass predicts risk of developing subsequent borderline hypertension. J Am Coll Cardiol. 1990;15:210–218.
Dilaveris PE, Gialafos EJ, Sideris SK, et al Simple electrocardiographic markers for the prediction of paroxysmal idiopathic atrial fibrillation. Am Heart J. 1998;135:733–738.
Çaǧlil K, Ergün K, Lafçil G, Gedik HS, Ulaş MM. QT and P wave dispersion[in Turkish]. Ankara Üniversitesi Tip Fakültesi Mecmuasi. 2005;58:42–46.
Turhan H, Yetkin E, Sahin O, et al Comparison of P-wave duration and dispersion in patients aged > or = 65 years with those aged < or = 45 years. J Electrocardiol. 2003;36:321–326.
Senen K, Turhan H, Riza Erbay R, et al P-wave duration and P-wave dispersion in patients with dilated cardiomyopathy. Eur J Heart Fail. 2004;6:567–569.
Tukek T, Akkaya V, Atilgan D, et al Effect of left atrial size and function on P-wave dispersion: a study in patients with paroxysmal atrial fibrillation. Clin Cardiol. 2001;24:676–680.
Ozer N, Aytemir K, Atalar E, et al P wave dispersion in hypertensive patients with paroxysmal AF. Pacing Clin Electrophysiol. 2000;23:1859–1862.
Dagli N, Karaca I, Yavuzkir M, Balin M, Arslan N. Are maximum P wave duration and P wave dispersion a marker of target organ damage in the hypertensive population? Clin Res Cardiol. 2008;97:98–104.
Brilla CG, Funck RC, Rupp H. Lisinoprilmediated regression of myocardial fibrosis in patients with hypertensive heart disease. Circulation. 2000;102:1388–1393.
Li D, Fareh S, Leung TK, Nattel S. Promotion of atrial fibrillation by heart failure in dogs: atrial remodeling of a different sort. Circulation. 1999;100:87–95.
Cha YM, Dzeja PP, Shen WK, et al Failing atrial myocardium: energetic deficits accompany structural remodeling and electrical instability. Am J Physiol Heart Circ Physiol. 2003;284:H1313–H1320.
Cheema AN, Ahmed MW, Kadish AH, Goldberger JJ. Effects of autonomic stimulation and blockade on signal-averaged P wave duration. J Am Coll Cardiol. 1995;26:497–502.
Coumel P. Paroxysmal atrial fibrillation: a disorder of autonomic tone? Eur Heart J. 1994;15(suppl. A):9–16.
Mattioli AV, Zennaro M, Bonatti S, Bonetti L, Mattioli G. Regression of left ventricular hypertrophy and improvement of diastolic function in hypertensive patients treated with telmisartan. Int J Cardiol. 2004;97:383–388.
Lip GY. The left atrium in hypertension, an appendage often forgotten. J Hum Hypertens. 1997;11:145–147.
Calhoun DA, Bakir S, Oparil S. Etiology and pathogenesis of essential hypertension. In: Crawford MH, DiMarco JP, eds. Cardiology. London: Mosby; 2001:31-1–31-10.
Lammers WJ, Kirchhof C, Bonke FI, Allessie MA. Vulnerability of rabbit atrium to reentry by hypoxia. Role of inhomogeneity in conduction and wavelength. Am J Physiol. 1992;262:H47–H55.
Fareh S, Villemaire C, Nattel S. Importance of refractoriness heterogeneity in the enhanced vulnerability to atrial fibrillation induction caused by tachycardia-induced atrial electrical remodeling. Circulation. 1998;98:2202–2229.
Dagli N, Karaca I. Hipertansif olgularda nebivolol tedavisinin P dispersiyonu üzerine etkisi [in Turkish]. Firat Tip Dergisi. 2006;11:154–159.
Tuncer M, Gunes Y, Guntekin U, Gumrukcuoglu HA, Eryonucu B. Shortterm effects of cilazapril and atenolol on P-wave dispersion in patients with hypertension. Adv Ther. 2008;25:99–105.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Karaca, I., Durukan, P., Dagli, N. et al. The effect of rapid blood pressure control on P-wave dispersion in hypertensive urgency. Adv Therapy 25, 1303–1314 (2008). https://doi.org/10.1007/s12325-008-0120-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-008-0120-0