Abstract
Background
More than 10% of HER2-positive metastatic breast cancer (mBC) will develop Central Nervous System (CNS) metastases as first and isolated site of relapse on trastuzumab and pertuzumab first-line therapy. However, few clinical data are available to guide the best strategy in this setting.
Methods
Patients experiencing isolated CNS progression on trastuzumab and pertuzumab first-line therapy were retrospectively identified from the French Epidemiological Strategy and Medical Economics (ESME) real-life database between 2008 and 2016.
Results
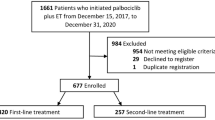
Among 995 patients treated with first-line trastuzumab and pertuzumab for HER2-positive mBC, 132 patients (13%) experienced isolated CNS progression with a median time of 12 months after mBC diagnosis. Twelves patients did not receive any treatment and were excluded from the analysis. Among the 120 patients considered, 76 (63%) received CNS-directed local therapy, 73 (60%) continued trastuzumab and pertuzumab, whereas 47 (39%) started another systemic treatment.
After a median follow-up of 21 months, there was no difference in progression-free survival for patient who continued trastuzumab–pertuzumab or switched to another systemic treatment. In multivariate analysis, trastuzumab–pertuzumab continuation was associated with longer OS (HR 0,28 IC 95%: 0,14–0,54 p < 0,001). mOS was not reached (95% 37.6-NE) and was 23.2 months (95% CI 15.5–53.6) in patients who continued trastuzumab and pertuzumab therapy and in patients who switched for another systemic therapy, respectively.
Conclusion
In this real-life cohort, trastuzumab–pertuzumab continuation after local treatment for isolated CNS progression did not negatively impact PFS and OS. Prospective trials and assessment of new strategies are warranted in this specific situation.




Similar content being viewed by others
Data availability
Data are indeed available on reasonable request.
References
Cancer [Internet]. [cité 8 févr 2021]. Disponible sur: https://www.who.int/news-room/fact-sheets/detail/cancer
Rostami R, Mittal S, Rostami P, Tavassoli F, Jabbari B. Brain metastasis in breast cancer: a comprehensive literature review. J Neurooncol mai. 2016;127(3):407–14.
Darlix A, Louvel G, Fraisse J, Jacot W, Brain E, Debled M, et al. Impact of breast cancer molecular subtypes on the incidence, kinetics and prognosis of central nervous system metastases in a large multicentre real-life cohort. Br J Cancer déc. 2019;121(12):991–1000.
Arvold ND, Lee EQ, Mehta MP, Margolin K, Alexander BM, Lin NU, et al. Updates in the management of brain metastases. Neuro-Oncol août. 2016;18(8):1043–65.
Verhaak E, Gehring K, Hanssens PEJ, Aaronson NK, Sitskoorn MM. Health-related quality of life in adult patients with brain metastases after stereotactic radiosurgery: a systematic, narrative review Support Care Cancer Off J Multinatl Assoc Support Care Cancer. Févr. 2020;28(2):473–84.
Evans AJ, James JJ, Cornford EJ, Chan SY, Burrell HC, Pinder SE, et al. Brain metastases from breast cancer: identification of a high-risk group. Clin Oncol R Coll Radiol G B août. 2004;16(5):345–9.
Chow L, Suen D, Ma KK, Kwong A. Identifying risk factors for brain metastasis in breast cancer patients: Implication for a vigorous surveillance program. Asian J Surg. 2015;38(4):220–3.
Pasquier D, Darlix A, Louvel G, Fraisse J, Jacot W, Brain E, et al. Treatment and outcomes in patients with central nervous system metastases from breast cancer in the real-life ESME MBC cohort. Eur J Cancer Oxf Engl Janv. 2020;125:22–30.
Brufsky AM, Mayer M, Rugo HS, Kaufman PA, Tan-Chiu E, Tripathy D, et al. Central nervous system metastases in patients with HER2-positive metastatic breast cancer incidence, treatment, and survival in patients from registHER. Clin Cancer Res Off J Am Assoc Cancer Res. 2011;17(14):4834–43.
Miller KD, Weathers T, Haney LG, Timmerman R, Dickler M, Shen J, et al. Occult central nervous system involvement in patients with metastatic breast cancer: prevalence, predictive factors and impact on overall survival. Ann Oncol Off J Eur Soc Med Oncol Juill. 2003;14(7):1072–7.
Swain SM, Baselga J, Miles D, Im YH, Quah C, Lee LF, et al. Incidence of central nervous system metastases in patients with HER2-positive metastatic breast cancer treated with pertuzumab, trastuzumab, and docetaxel: results from the randomized phase III study CLEOPATRA. Ann Oncol Off J Eur Soc Med Oncol Juin. 2014;25(6):1116–21.
Swain SM, Miles D, Kim SB, Im YH, Im SA, Semiglazov V, et al. Pertuzumab, trastuzumab, and docetaxel for HER2-positive metastatic breast cancer (CLEOPATRA): end-of-study results from a double-blind, randomised, placebo-controlled, phase 3 study. Lancet Oncol avr. 2020;21(4):519–30.
Yamamoto M, Serizawa T, Shuto T, Akabane A, Higuchi Y, Kawagishi J, et al. Stereotactic radiosurgery for patients with multiple brain metastases a multi-institutional prospective observational study. Lancet Oncol avr. 2014;15(4):387–95.
Brown PD, Ballman KV, Cerhan JH, Anderson SK, Carrero XW, Whitton AC, et al. Postoperative stereotactic radiosurgery compared with whole brain radiotherapy for resected metastatic brain disease (NCCTG N107C/CEC·3): a multicentre, randomised, controlled, phase 3 trial. Lancet Oncol août. 2017;18(8):1049–60.
Kalkanis SN, Kondziolka D, Gaspar LE, Burri SH, Asher AL, Cobbs CS, et al. The role of surgical resection in the management of newly diagnosed brain metastases: a systematic review and evidence-based clinical practice guideline. J Neurooncol janv. 2010;96(1):33–43.
Bailleux C, Eberst L, Bachelot T. Treatment strategies for breast cancer brain metastases. Br J Cancer janv. 2021;124(1):142–55.
Park YH, Park MJ, Ji SH, Yi SY, Lim DH, Nam DH, et al. Trastuzumab treatment improves brain metastasis outcomes through control and durable prolongation of systemic extracranial disease in HER2-overexpressing breast cancer patients. Br J Cancer. 2009;100(6):894–900.
Krop IE, Lin NU, Blackwell K, Guardino E, Huober J, Lu M, et al. Trastuzumab emtansine (T-DM1) versus lapatinib plus capecitabine in patients with HER2-positive metastatic breast cancer and central nervous system metastases: a retrospective, exploratory analysis in EMILIA. Ann Oncol Off J Eur Soc Med Oncol. 2015;26(1):113–9.
Montemurro F, Delaloge S, Barrios CH, Wuerstlein R, Anton A, Brain E, et al. Trastuzumab emtansine (T-DM1) in patients with HER2-positive metastatic breast cancer and brain metastases: exploratory final analysis of cohort 1 from KAMILLA, a single-arm phase IIIb clinical trial☆. Ann Oncol Off J Eur Soc Med Oncol. 2020;31(10):1350–8.
Murthy RK, Hamilton EP, Ferrario C, Aucoin N, Falkson CI, Chamberlain MC, et al. Clinical benefit of tucatinib after isolated brain progression: A retrospective pooled analysis of tucatinib phase 1b studies in HER2+ breast cancer. J Clin Oncol. 2018;36(15):1015–1015.
Vogelbaum MA, Brown PD, Messersmith H, Brastianos PK, Burri S, Cahill D, et al. Treatment for Brain Metastases: ASCO-SNO-ASTRO Guideline. J Clin Oncol. 2021. https://doi.org/10.1200/JCO.21.02314.
Le Rhun E, Guckenberger M, Smits M, Dummer R, Bachelot T, Sahm F, et al. EANO–ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up of patients with brain metastasis from solid tumours. Ann Oncol. 2021;32(11):1332–47.
Bartsch R, Bergen E. ASCO 2018: highlights in HER2-positive metastatic breast cancer. Memo. 2018;11(4):280–3.
Wolff AC, Hammond MEH, Allison KH, Harvey BE, Mangu PB, Bartlett JMS, et al. Human Epidermal Growth Factor Receptor 2 Testing in Breast Cancer: American Society of Clinical Oncology/College of American Pathologists Clinical Practice Guideline Focused Update. J Clin Oncol. 2018. https://doi.org/10.1200/JCO.2018.77.8738.
Gennari A, André F, Barrios CH, Cortés J, de Azambuja E, DeMichele A, Dent R, Fenlon D, Gligorov J, Hurvitz SA, Im SA, Krug D, Kunz WG, Loi S, Penault-Llorca F, Ricke J, Robson M, Rugo HS, Saura C, Schmid P, Singer CF, Spanic T, Tolaney SM, Turner NC, Curigliano G, Loibl S, Paluch-Shimon S, Harbeck N; ESMO Guidelines Committee. Electronic address: clinicalguidelines@esmo.org. ESMO Clinical Practice Guideline for the diagnosis, staging and treatment of patients with metastatic breast cancer. Ann Oncol. 2021;32(12):1475–95. https://doi.org/10.1016/j.annonc.2021.09.019.
Pestalozzi BC, Brignoli S. Trastuzumab in CSF. J Clin Oncol Off J Am Soc Clin Oncol. 2000;18(11):2349–51.
Arvanitis CD, Ferraro GB, Jain RK. The blood-brain barrier and blood-tumour barrier in brain tumours and metastases. Nat Rev Cancer janv. 2020;20(1):26–41.
Murthy RK, Loi S, Okines A, Paplomata E, Hamilton E, Hurvitz SA, et al. Tucatinib, Trastuzumab, and Capecitabine for HER2-Positive Metastatic Breast Cancer. N Engl J Med. 2020;382(7):597–609.
Lewis Phillips GD, Nishimura MC, Lacap JA, Kharbanda S, Mai E, Tien J, et al. Trastuzumab uptake and its relation to efficacy in an animal model of HER2-positive breast cancer brain metastasis. Breast Cancer Res Treat. 2017;164(3):581–91.
Kabraji S, Ni J, Lin NU, Xie S, Winer EP, Zhao JJ. Drug resistance in HER2-positive breast cancer brain metastases: blame the barrier or the brain? clin cancer res off. J Am Assoc Cancer Res. 2018;24(8):1795–804.
Lin NU, Borges V, Anders C, Murthy RK, Paplomata E, Hamilton E, et al. Intracranial Efficacy and Survival With Tucatinib Plus Trastuzumab and Capecitabine for Previously Treated HER2-Positive Breast Cancer With Brain Metastases in the HER2CLIMB Trial. J Clin Oncol Off J Am Soc Clin Oncol. 2020;38(23):2610–9.
Peters S, Camidge DR, Shaw AT, Gadgeel S, Ahn JS, Kim DW, et al. Alectinib versus Crizotinib in Untreated ALK-Positive Non–Small-Cell Lung Cancer. N Engl J Med. 2017;377(9):829–38.
Freedman RA, Gelman RS, Anders CK, Melisko ME, Parsons HA, Cropp AM, et al. TBCRC 022: A Phase II Trial of Neratinib and Capecitabine for Patients With Human Epidermal Growth Factor Receptor 2-Positive Breast Cancer and Brain Metastases. J Clin Oncol Off J Am Soc Clin Oncol. 2019;37(13):1081–9.
Saura C, Oliveira M, Feng YH, Dai MS, Chen SW, Hurvitz SA, et al. Neratinib Plus Capecitabine Versus Lapatinib Plus Capecitabine in HER2-Positive Metastatic Breast Cancer Previously Treated With ≥ 2 HER2-Directed Regimens: Phase III NALA Trial. J Clin Oncol. 2020;38(27):3138–49.
Acknowledgements
We thank the 18 French Comprehensive Cancer Centers for providing the data and each ESME local coordinator for managing the project at the local level. Moreover, we thank the ESME Scientific Group and Strategic Committee for their ongoing support. 18 Participating French Comprehensive Cancer Centers (FCCC): ; I. Curie, Paris/ Saint-Cloud, G. Roussy, Villejuif, I. Cancérologie de l’Ouest, Angers/Nantes, C. F. Baclesse, Caen, ICM Montpellier, C. L. Bérard, Lyon, C. G-F Leclerc, Dijon, C. H. Becquerel, Rouen; I. C. Regaud, Toulouse; C. A. Lacassagne, Nice; Institut de Cancérologie de Lorraine, Nancy; C. E. Marquis, Rennes; I. Paoli-Calmettes, Marseille; C. J. Perrin, Clermont Ferrand; I. Bergonié, Bordeaux; C. P. Strauss, Strasbourg; I. J. Godinot, Reims; C. O. Lambret, Lille. ESME central coordinating staff: Program director: Anne-Laure Martin. Data Management team: Coralie Courtinard, Emilie Nguyen, Olivier Payen, Irwin Piot, Dominique Schwob and Olivier Villacroux. Operational team: Nathalie Bouyer, Michaël Chevrot, Patricia D’Agostino, Pascale Danglot, Levent Dinc, Tahar Guesmia, Charlotte Herlin, Elodie Kupfer, Harmonie Oulie, Sandra Pélissier, Frédéric Roy, Gaëtane Simon and Toihiri Said.Software designer Team: Matou Diop, Blaise Fulpin, Fréja Messo, José Paredes and Alexandre Vanni.
Funding
Industrial partners (Roche, Pierre Fabre Laboratories, Pfizer, AstraZeneca, EISAI, MSD, Daiichi Sankyo, Gilead, Seagen) financially support the ESME MBC database. Unicancer manages the ESME database (i.e., data collection, management analysis, interpretation and publication of the data) independently. None of the industrial partner was involved neither in the design and conduct of the study, nor in collection, management, analysis, and interpretation of the data, nor in preparation, review, or approval of the manuscript nor in decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Laetitia Collet, Lauriane Eberst, Ludovic Gauthier, Marc Debled,, Marie-Ange Mouret-Reynier, Isabelle Desmoulins, Anthony Goncalves, Mario Campone, Jean-Marc Ferrero, Etienne Brain, Lionel Uwer, Jean-Christophe Eymard, Veronique Dieras, Gaetane Simon, Marianne LeLeheurteur, Florence Dalenc, Laurence Vanlemmens, Amelie Darlix: no disclosures. Monica Ardenos: Honoraria: Novartis, Astra Zeneca, Pfizer; Honoraria (to the institution): Roche, Astra Zeneca; Travel grant: Daichii, Pfizer; research grant: Eli-Lilly, Astra Zeneca, Consultant; advisory board (to teh institution): Novartis Loana Hrab: Travel grant: Amgen, Novartis, Pfizer, Sandoz, Pierre Fabre, Mundipharma, Roche Thomas Bachelot: Personal fees and non-financial support from Roche, Novartis, AstraZeneca, grants, Pfizer, personal fees from SeattleGenetics, outside the submitted work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Collet, L., Eberst, L., Ludovic, G. et al. Clinical outcome of patients with isolated central nervous system progression on first-line pertuzumab and trastuzumab treatment for HER2-positive metastatic breast cancer in a real-life cohort. Breast Cancer 30, 329–341 (2023). https://doi.org/10.1007/s12282-022-01427-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12282-022-01427-0