Abstract
Background
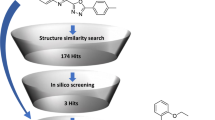
Breast cancer is one of the most lethal types of cancer in women worldwide. The human epidermal growth factor receptor 2 (HER2) is considered as a validated target in breast cancer therapy. Previously, we have used quantitative structure activity relationship QSAR equations and their associated pharmacophore models to screen for new promising HER2 structurally diverse inhibitory leads which were tested against HER2-overexpressing SKOV3 ovarian cancer cell line.
Objective
In this study, we sought to explore the effect of most active ligands against different normal and breast cancer cell lines that represent different breast cancer subtypes with distinguished expression levels in HER2 and HER1.
Methods
We have tested the promising compounds against SKBR3, MDA-MB-231, MCF7, human fibroblast, and MCF10 cell lines. To understand the inhibitory effects of the active ligands against HER2 over expressed breast cancer cell lines, all inhibitors and the control compound, lapatinib, were docked into the active site of HER2 enzyme performed using Ligand Fit docking engine and PMF scoring function.
Results
Five ligands exhibited promising results with relatively low IC50 values on cells that amplify HER2 and high IC50 on those that do not express such a receptor. The most potent compound (compound 13) showed an IC50 of 0.046 µM. To test their toxicity against normal cells, the active compounds were tested against both normal fibroblast and normal breast cancer cell MCF-10 and relatively high IC50 values were scored. The IC50 values on HER2 over-expressed breast cancer and normal fibroblast cells provided a promising safety index. Docking results showed the highest similarity in the binding site between the most active ligand and the lapatinib.
Conclusion
Our pharmacophore model resulted in a high potent ligand that shows high potency against HER2 positive breast cancer and relatively low toxicity towards the normal human cells.
Graphic abstract






Similar content being viewed by others
References
Tsang RY, Sadeghi S, Finn RS. Lapatinib, a dual-targeted small molecule inhibitor of EGFR and HER2, in HER2-amplified breast cancer: from bench to bedside. Clin Med Insights Ther. 2011;2011(3):1–13.
Arteaga CL, Engelman JA. ERBB receptors: from oncogene discovery to basic science to mechanism-based cancer therapeutics. Cancer Cell. 2014;25:282–303.
Delord JP, Allal C, Canal M, Mery E, Rochaix P, Hennebelle I, et al. Selective inhibition of HER2 inhibits AKT signal transduction and prolongs disease-free survival in a micrometastasis model of ovarian carcinoma. Ann Oncol. 2005;16:1889–977.
Kunz C, Borghouts C, Buerger C, Groner B. Peptide aptamers with binding specificity for the intracellular domain of the ErbB2 receptor interfere with AKT signaling and sensitize breast cancer cells to Taxol. Mol Cancer Res. 2006;4:983–98.
Menard S, Casalini P, Campiglio M, Pupa SM, Tagliabue E. Role of HER2/neu in tumor progression and therapy. Cell Mol Life Sci. 2004;61:2965–78.
Schlessinger J. Cell signaling by receptor tyrosine kinases. Cell. 2000;103:211–25.
Scholl S, Beuzeboc P, Pouillart P. Targeting HER2 in other tumor types. Ann Oncol. 2001;12(Suppl 1):S81–7.
Hynes NE, Lane HA. ERBB receptors and cancer: the complexity of targeted inhibitors. Nat Rev Cancer. 2005;5:341–54.
Santin AD, Bellone S, Roman JJ, McKenney JK, Pecorelli S. Trastuzumab treatment in patients with advanced or recurrent endometrial carcinoma overexpressing HER2/neu. Int J Gynaecol Obstet. 2008;102:128–31.
Krishnamurti U, Silverman JF. HER2 in breast cancer: a review and update. Adv Anat Pathol. 2014;21:100–7.
Scaltriti M, Verma C, Guzman M, Jimenez J, Parra JL, Pedersen K, et al. Lapatinib, a HER2 tyrosine kinase inhibitor, induces stabilization and accumulation of HER2 and potentiates trastuzumab-dependent cell cytotoxicity. Oncogene. 2009;28:803–14.
Sergina NV, Rausch M, Wang D, Blair J, Hann B, Shokat KM, et al. Escape from HER-family tyrosine kinase inhibitor therapy by the kinase-inactive HER3. Nature. 2007;445:437–41.
Tzahar E, Waterman H, Chen X, Levkowitz G, Karunagaran D, Lavi S, et al. A hierarchical network of interreceptor interactions determines signal transduction by Neu differentiation factor/neuregulin and epidermal growth factor. Mol Cell Biol. 1996;16:5276–87.
Iqbal N, Iqbal N. Human epidermal growth factor receptor 2 (HER2) in cancers: overexpression and therapeutic implications. Mol Biol Int. 2014;2014:852748.
Yarden Y, Sliwkowski MX. Untangling the ErbB signalling network. Nat Rev Mol Cell Biol. 2001;2:127–37.
Olayioye MA, Graus-Porta D, Beerli RR, Rohrer J, Gay B, Hynes NE. ErbB-1 and ErbB-2 acquire distinct signaling properties dependent upon their dimerization partner. Mol Cell Biol. 1998;18:5042–51.
Mitri Z, Constantine T, O'Regan R. The HER2 receptor in breast cancer: pathophysiology, clinical use, and new advances in therapy. Chemother Res Pract. 2012;2012:743193.
Ponde N, Brandao M, El-Hachem G, Werbrouck E, Piccart M. Treatment of advanced HER2-positive breast cancer: 2018 and beyond. Cancer Treat Rev. 2018;67:10–20.
Andrulis IL, Bull SB, Blackstein ME, Sutherland D, Mak C, Sidlofsky S, et al. neu/erbB-2 amplification identifies a poor-prognosis group of women with node-negative breast cancer. Toronto Breast Cancer Study Group. J Clin Oncol. 1998;16:1340–9.
Holliday DL, Speirs V. Choosing the right cell line for breast cancer research. Breast Cancer Res. 2011;13:215.
Asif HM, Sultana S, Ahmed S, Akhtar N, Tariq M. HER-2 positive breast cancer—a mini-review. Asian Pac J Cancer Prev. 2016;17:1609–15.
Tsurutani J, West KA, Sayyah J, Gills JJ, Dennis PA. Inhibition of the phosphatidylinositol 3-kinase/Akt/mammalian target of rapamycin pathway but not the MEK/ERK pathway attenuates laminin-mediated small cell lung cancer cellular survival and resistance to imatinib mesylate or chemotherapy. Cancer Res. 2005;65:8423–32.
Loibl S, Gianni L. HER2-positive breast cancer. Lancet. 2017;389:2415–29.
Zalloum H, Tayyem R, Irmaileh BA, Bustanji Y, Zihlif M, Mohammad M, et al. Discovery of new human epidermal growth factor receptor-2 (HER2) inhibitors for potential use as anticancer agents via ligand-based pharmacophore modeling. J Mol Graph Model. 2015;61:61–84.
Kumler I, Tuxen MK, Nielsen DL. A systematic review of dual targeting in HER2-positive breast cancer. Cancer Treat Rev. 2014;40:259–70.
Piccart-Gebhart MJ, Procter M, Leyland-Jones B, Goldhirsch A, Untch M, Smith I, et al. Trastuzumab after adjuvant chemotherapy in HER2-positive breast cancer. N Engl J Med. 2005;353:1659–72.
Romond EH, Perez EA, Bryant J, Suman VJ, Geyer CE Jr, Davidson NE, et al. Trastuzumab plus adjuvant chemotherapy for operable HER2-positive breast cancer. N Engl J Med. 2005;353:1673–84.
Tsang RY, Sadeghi S, Finn RS. Lapatinib, a dual-targeted small molecule inhibitor of Egfr and Her2, in Her2-amplified breast cancer: from bench to bedside. Clin Med Insights Ther. 2011;3:1–13.
Baselga J, Tripathy D, Mendelsohn J, Baughman S, Benz CC, Dantis L, et al. Phase II study of weekly intravenous recombinant humanized anti-p185HER2 monoclonal antibody in patients with HER2/neu-overexpressing metastatic breast cancer. J Clin Oncol. 1996;14:737–44.
Gradishar WJ. HER2 therapy—an abundance of riches. N Engl J Med. 2012;366:176–8.
Gajria D, Chandarlapaty S. HER2-amplified breast cancer: mechanisms of trastuzumab resistance and novel targeted therapies. Expert Rev Anticancer Ther. 2011;11:263–75.
Slamon D, Pegram M. Rationale for trastuzumab (herceptin) in adjuvant breast cancer trials. Semin Oncol. 2001;28:13–9.
Callahan R, Hurvitz S. Human epidermal growth factor receptor-2-positive breast cancer: current management of early, advanced, and recurrent disease. Curr Opin Obstet Gynecol. 2011;23:37–433.
Wood ER, Truesdale AT, McDonald OB, Yuan D, Hassell A, Dickerson SH, et al. A unique structure for epidermal growth factor receptor bound to GW572016 (Lapatinib): relationships among protein conformation, inhibitor off-rate, and receptor activity in tumor cells. Cancer Res. 2004;64:6652–9.
de Azambuja E, Bedard PL, Suter T, Piccart-Gebhart M. Cardiac toxicity with anti-HER-2 therapies: what have we learned so far? Target Oncol. 2009;4:77–88.
Fink MY, Chipuk JE. Survival of HER2-positive breast cancer cells: receptor signaling to apoptotic control centers. Genes Cancer. 2013;4:187–95.
Aertgeerts K, Skene R, Yano J, Sang BC, Zou H, Snell G, et al. Structural analysis of the mechanism of inhibition and allosteric activation of the kinase domain of HER2 protein. J Biol Chem. 2011;286:18756–65.
O'Shaughnessy J, Blackwell KL, Burstein H, Storniolo AM, Sledge G, Baselga J, et al. A randomized study of Lapatinib alone or in combination with trastuzumab in heavily pretreated HER2+ metastatic breast cancer progressing on trastuzumab therapy. J Clin Oncol. 2008;26(15_suppl):1015.
Engel RH, Kaklamani VG. HER2-positive breast cancer: current and future treatment strategies. Drugs. 2007;67:1329–41.
Baselga J, Coleman RE, Cortes J, Janni W. Advances in the management of HER2-positive early breast cancer. Crit Rev Oncol Hematol. 2017;119:113–22.
Figueroa-Magalhaes MC, Jelovac D, Connolly R, Wolff AC. Treatment of HER2-positive breast cancer. Breast. 2014;23:128–36.
OMEGA (version 2.5.1.4). Santa Fe, New Mexico, USA: OpenEye Scientific Software Inc.; 2013.
Takimoto CH. Anticancer drug development at the US National Cancer Institute. Cancer Chemother Pharmacol. 2003;52(Suppl 1):S29–33.
Knox C, Law V, Jewison T, Liu P, Ly S, Frolkis A, et al. DrugBank 3.0: a comprehensive resource for 'omics' research on drugs. Nucleic Acids Res. 2011;39:D1035–41.
Dijkers PF, Medema RH, Pals C, Banerji L, Thomas NS, Lam EW, et al. Forkhead transcription factor FKHR-L1 modulates cytokine-dependent transcriptional regulation of p27(KIP1). Mol Cell Biol. 2000;20:9138–48.
Datta SR, Dudek H, Tao X, Masters S, Fu H, Gotoh Y, et al. Akt phosphorylation of BAD couples survival signals to the cell-intrinsic death machinery. Cell. 1997;91:231–41.
Cardone MH, Roy N, Stennicke HR, Salvesen GS, Franke TF, Stanbridge E, et al. Regulation of cell death protease caspase-9 by phosphorylation. Science. 1998;282:1318–21.
Thierry L, Hoffmann D. Pharmacophores and pharmacophore searches. Hoboken: Wiley; 2006. p. 395.
Kirchmair J, Wolber G, Laggner C, Langer T. Comparative performance assessment of the conformational model generators omega and catalyst: a large-scale survey on the retrieval of protein-bound ligand conformations. J Chem Inf Model. 2006;46:1848–61.
Kirchmair J, Laggner C, Wolber G, Langer T. Comparative analysis of protein-bound ligand conformations with respect to catalyst's conformational space subsampling algorithms. J Chem Inf Model. 2005;45:422–30.
Charafe-Jauffret E, Ginestier C, Monville F, Finetti P, Adelaide J, Cervera N, et al. Gene expression profiling of breast cell lines identifies potential new basal markers. Oncogene. 2006;25:2273–84.
Neve RM, Chin K, Fridlyand J, Yeh J, Baehner FL, Fevr T, et al. A collection of breast cancer cell lines for the study of functionally distinct cancer subtypes. Cancer Cell. 2006;10:515–27.
Lacroix M, Leclercq G. Relevance of breast cancer cell lines as models for breast tumours: an update. Breast Cancer Res Treat. 2004;83:249–89.
Kacan T, Altun A, Altun GG, Kacan SB, Sarac B, Seker MM, et al. Investigation of antitumor effects of sorafenib and lapatinib alone and in combination on MCF-7 breast cancer cells. Asian Pac J Cancer Prev. 2014;15:3185–9.
Acknowledgements
We wish to thank the Deanship of Scientific Research at the University of Jordan and Scientific Research Support Fund (SRF), Amman, Jordan, for financial support. We would like also to acknowledge the Developmental Therapeutics Program, Division of Cancer Treatment and Diagnosis, National Cancer Institute (https://www.dtp.cancer.gov) for providing us with the NCI compounds.
Funding
This study was funded by Deanship of Scientific Research at the University of Jordan and Scientific Research Support Fund (SRF), Amman, Jordan.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The author(s) declare that they have no competing interests.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Zalloum, H., AbuThiab, T., Hameduh, T. et al. Comparative anti-proliferative effects of potential HER2 inhibitors on a panel of breast cancer cell lines. Breast Cancer 27, 213–224 (2020). https://doi.org/10.1007/s12282-019-01011-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12282-019-01011-z