Abstract
Purpose
The purpose of this study was to investigate the accuracy of preoperative diagnostic tools for axillary lymph nodes (LNs) staging of breast cancer.
Materials and Methods
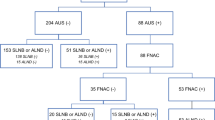
A total of 2464 consecutive patients with operable breast cancer were prospectively identified at our institution between April 2012 and March 2017. Patients with suspicious axillary LN of breast cancer were assessed using preoperative ultrasound(US) or computed tomography (CT), underwent fine-needle aspiration cytology (FNA) or core needle biopsy (CNB). The inclusion criteria for both FNA and CNB were a cortical thickness >3 mm or abnormal morphological characteristics. Patients with biopsy-proven metastasis underwent axillary lymph node dissection (ALND), and those with a negative FNA or CNB underwent sentinel lymph node biopsy (SNB). If the SNB was positive, ALND was performed. Diagnostic accuracy for SNB was calculated for both FNA and CNB. In addition, the patients in this study were divided into two groups as follows: the cN0-FNA group (suspicious LN but negative FNA) and cN0-CNB group (suspicious LN but negative CNB).
Results
A number of patients with negative US/CT findings of LNs were 1406, with 744 undergoing FNA and 272 undergoing CNB for suspicious LNs. Sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV), and accuracy were 65, 99, 99, 80, and 85% in FNA, and 87, 100, 100, 93 and 95% in CNB, respectively. SNB was performed in 172 (cN0-CNB group) of 272 CNB and 487 (cN0-FNA group) of 744 FNA patients. One hundred and seventy-two patients from the cN0-CNB group (Tis 6, T1 97, T2 66, T3 3 patients) treated with SNB were compared to 487 from the cN0-FNA group (Tis 21, T1 225, T2 233, T3 8 patients) in terms of number of LN metastasis. A number of patients with more than 3 positive SNB and positive LNs were 9 (5%) and 0 (0%) in cN0-CNB group, and 78 (16%) and 24 (5%) in cN0-FNA group, respectively. A number of patients who had complications such as haematoma and pain at the time of 7 to 14 days after CNB and FNA were 1 (0.5%) and 1 (0.5%) in cN0-CNB group, and were 0% and 0.2% in cN0-FNA group (p = 0.44), respectively.
Conclusions
The preoperative diagnosis of axillary LNs was influenced by the diagnostic tool used. CNB is a reliable method for the preoperative diagnosis of LN metastasis.

Similar content being viewed by others
References
Lucci A, McCall LM, Beitsch PD, Whitworth PW, Reintgen DS, Blumencranz PW, et al. Surgical complications associated with sentinel lymph node dissection (SLND) plus axillary lymph node dissection compared with SLND alone in the American College of Surgeons Oncology Group Trial Z0011. J Clin Oncol. 2007;25(24):3657–63.
Galimberti V, Cole BF, Zurrida S, Viale G, Luini A, Veronesi P. Axillary dissection versus no axillary dissection in patients with sentinel-node micrometastases (IBCSG 23-01): a phase 3 randomised controlled trial. Lancet Oncol. 2013;14(4):297–305.
Donker M, van Tienhoven G, Straver ME, Meijnen P, van de Velde CJ, Mansel RE. Radiotherapy or surgery of the axilla after a positive sentinel node in breast cancer (EORTC 10981–22023 AMAROS): a randomised, multicentre, open-label, phase 3 non-inferiority trial. Lancet Oncol. 2014;15(12):1303–10.
Gentilini O, Veronesi U. Abandoning sentinel lymph node biopsy in early breast cancer? A new trial in progress at the European Institute of Oncology of Milan (SOUND: sentinel node vs observation after axillary UltraSouND). Breast. 2012;21:678–81.
Cyr AE, Tucker N, Ademuyiwa F, Margenthaler JA, Aft RL, Eberlein TJ, et al. Successful completion of the pilot phase of a randomized controlled trial comparing sentinel lymph node biopsy to no further axillary staging in patients with clinical T1–T2 N0 breast cancer and normal axillary ultrasound. J Am Coll Surg. 2016;223(2):399–407.
Smidt JHW de Wilt. Clinically node negative breast cancer patients undergoing breast conserving therapy: sentinel lymph node procedure versus follow-up. https://www.boogstudycenter.nl/studie/273/2013-08-lumpectomie.html.
Susini T, Nori J, Olivieri S, Molino C, Marini G, Bianchi S, et al. Predicting the status of axillary lymph nodes in breast cancer: a multiparameter approach including axillary ultrasound scanning. Breast. 2009;18(2):103–8.
Sapino A, Cassoni P, Zanon E, Fraire F, Croce S, Coluccia C, et al. Ultrasonographically guided fine-needle aspiration of axillary lymph nodes: role in breast cancer management. Br J Cancer. 2003;88:702–6.
Clark DA. Preoperative ultrasound of axillary lymph nodes in patients with breast cancer. ANZ J Surg. 2008;78:307–8.
Altomare V, Guerriero G, Carino R, Battista C, Primavera A, Altomare A, et al. Axillary lymph node echo-guided fine-needle aspiration cytology enables breast cancer patients to avoid a sentinel lymph node biopsy: preliminary experience and a review of the literature. Surg Today. 2007;37(9):735–9.
Rautiainen S, Masarwah A, Sudah M, Sutela A, Pelkonen O, Joukainen S, et al. Axillary lymph node biopsy in newly diagnosed invasive breast cancer: comparative accuracy of fine-needle aspiration biopsy versus core needle biopsy. Radiology. 2013;269(1):54–60.
Ganott MA, Zuley ML, Abrams GS, Lu AH, Kelly AE, Sumkin JH et al. Ultrasound guided core biopsy versus fine needle aspiration for evaluation of axillary lymphadenopathy in patients with breast cancer. ISRN Oncol. 2014; undefined: 703160.
Rao R, Lilley L, Andrews V, Radford L, Ulissey M. Axillary staging by percutaneous biopsy: sensitivity of fine-needle aspiration versus core needle biopsy. Ann Surg Oncol. 2009;16(5):1170–5.
Britton PD, Goud A, Godward S, Barter S, Freeman A, Gaskarth M, et al. Use of ultrasound-guided axillary node core biopsy in staging of early breast cancer. Eur Radiol. 2009;19(3):561–9.
Deurloo EE, Tanis PJ, Gilhuijs KG, Muller SH, Kröger R, Peterse JL, et al. Reduction in the number of sentinel lymph node procedures by preoperative ultrasonography of the axilla in breast cancer. Eur J Cancer. 2003;39(8):1068–73.
Caretta-Weyer H, Sisney GA, Beckman C, Burnside ES, Salkowsi LR, Strigel RM. Impact of axillary ultrasound and core needle biopsy on the utility of intraoperative frozen section analysis and treatment decision making in women with invasive breast cancer. Am J Surg. 2012;204(3):308–14.
Cserni G, Bianchi S, Boecker W, Decker T, Lacerda M, Rank F, et al. Improving the reproducibility of diagnosing micrometastases and isolated tumor cells. Cancer. 2005;103(2):358–67.
van Deurzen CH, Cserni G, Bianchi S, Vezzosi V, Arisio R, Wesseling J, et al. Nodal-stage classification in invasive lobular breast carcinoma: influence of different interpretations of the pTNM classification. J Clin Oncol. 2010;28(6):999–1004.
Maxwell AJ, Bundred NJ, Harvey J, Hunt R, Morris J, Lim YY. A randomised pilot study comparing 13 G vacuum-assisted biopsy and conventional 14 G core needle biopsy of axillary lymph nodes in women with breast cancer. Clin Radiol. 2016;71(6):551–7.
Houssami N, Ciatto S, Turner RM, Cody HS 3rd, Macaskill P. Preoperative ultrasound-guided needle biopsy of axillary nodes in invasive breast cancer: meta-analysis of its accuracy and utility in staging the axilla. Ann Surg. 2011;254(2):243–51.
Krag DN, Anderson SJ, Julian TB, Brown AM, Harlow SP, Costantino JP, et al. Technical outcomes of sentinel lymph node resection and conventional axillary lymph node dissection in patients with clinically negative breast cancer: results from the NSAPB B-32 randomised phase III trial. Lancet Oncol. 2007;8(10):881–8.
Goyal A, Newcombe RG, Chhabra A, Mansel RE. Factors affecting failed localization and false-negative rates of sentinel node biopsy in breast cancer—results of the ALMANAC validation phase. Breast Cancer Res Treat. 2006;99(2):203–8.
Britton PD, Provenzano E, Barter S, Gaskarth M, Goud A, Moyle P, et al. Ultrasound guided percutaneous axillary lymph node core biopsy: how often is the sentinel lymph node being biopsied? Breast. 2009;18(1):13–6.
Vassallo P, Wernecke K, Roos N, Peters PE. Differentiation of benign from malignant superficial lymphadenopathy: the role of high-resolution US. Radiology. 1992;183(1):215–20.
van Rijk MC, Deurloo EE, Nieweg OE, Gilhuijs KG, Peterse JL, Rutgers EJ, et al. Ultrasonography and fine-needle aspiration cytology can spare breast cancer patients unnecessary sentinel lymph node biopsy. Ann Surg Oncol. 2006;13(1):31–5.
Damera A, Evans AJ, Cornford EJ, Wilson AR, Burrell HC, James JJ, et al. Diagnosis of axillary nodal metastases by ultrasound-guided core biopsy in primary operable breast cancer. Br J Cancer. 2003;89(7):1310–3.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors have declared no conflict of interest.
About this article
Cite this article
Nakamura, R., Yamamoto, N., Miyaki, T. et al. Impact of sentinel lymph node biopsy by ultrasound-guided core needle biopsy for patients with suspicious node positive breast cancer. Breast Cancer 25, 86–93 (2018). https://doi.org/10.1007/s12282-017-0795-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12282-017-0795-7