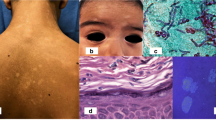
Abstract
Pityriasis versicolor (PV) is caused by the fungus Malassezia, especially by Malassezia globosa. The predisposing factors for PV are heat, humidity, hyperhidrosis, oral contraceptives, stress, application of oily preparations, and treatment with corticosteroids. PV is found mainly on the seborrheic areas of the trunk, shoulders, upper aspects of the arms, and neck, but it may spread to the face, scalp, submammary areas, axillae, groin, skin folds, and buttocks. It is characterized by hyperpigmented, hypopigmented, or erythematous (versicolor), round-to-oval, finely scaling, thin plaques. Other less frequent clinical variants are papular, atrophic, imbricata, and pityriasis rubra pilaris-like presentations. The diagnosis of PV is usually made clinically with the aid of Wood’s light or dermoscopy. Direct microscopic examination, culture, biopsy, and molecular studies are among the laboratory diagnostic methods. Topical therapy is the treatment of choice for most patients. Systemic imidazole therapy is usually reserved for widespread or resistant cases.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Pedrosa AF, Lisboa C, Gonçalves RA. Malassezia infections: a medical conundrum. J Am Acad Dermatol. 2014;71:170–6.
Renati S, Cukras A, Bigby M. Pityriasis versicolor. BMJ. 2015;350:h1394.
Santana JO, Azevedo FL, Campos Filho PC. Pityriasis versicolor: clinical-epidemiological characterization of patients in the urban area of Buerarema-BA, Brazil. An Bras Dermatol. 2013;88:216–21.
Rodoplu G, Saracli MA, Gümral R, Taner YS. Distribution of Malassezia species in patients with pityriasis versicolor in Turkey. J Mycol Med. 2014;24:117–23.
Metin A, Dilek N, Demirseven DD. Fungal infections of the folds (intertriginous areas). Clin Dermatol. 2015;33:437–47.
Harada K, Saito M, Sugita T, Tsuboi R. Malassezia species and their associated skin diseases. J Dermatol. 2015;42:250–7.
Kim SY, Lee YW, Choe YB, Ahn KJ. Progress in Malassezia research in Korea. Ann Dermatol. 2015;27:647–57.
Heidrich D, Daboit TC, Stopiglia CD, Magagnin CM, Vetoratto G, Amaro TG, et al. Sixteen years of pityriasis versicolor in metropolitan area of Porto Alegre, Southern Brazil. Rev Inst Med Trop Sao Paulo. 2015;57:277–80.
Hawkins DM, Smidt AC. Superficial fungal infections in children. Pediatr Clin North Am. 2014;61:443–55.
Kallini JR, Riaz F, Khachemoune A. Tinea versicolor in dark-skinned individuals. Int J Dermatol. 2014;53:137–41. Only few articles on the manifestation of skin diseases on dark skin.
Varada S, Dabade T, Loo DS. Uncommon presentations of tinea versicolor. Dermatol Pract Concept. 2014;4:93–6. It is important to know the less frequent presentations of PV.
Cullingham K, Hull PR. Atrophying pityriasis versicolor. CMAJ. 2014;186:776. A rare variant that might be misdiagnosed if not known.
Blasco-Morente G, Garrido-Colmenero C, Pérez López I, Tercedor-Sánchez J. Wood’ light in dermatology: an essential technique. PIEL [Barc]. 2014;29:487–94.
Romano C, Feci L, Mancianti F, Fimiani M. Perineal and genital pityriasis versicolor due to Malassezia globosa. J Eur Acad Dermatol Venereol. 2015;29:1857–8. Rare variants that might be misdiagnosed if not known.
Didehdar M, Mehbod AS, Eslamirad Z, Mosayebi M, Hajihossein R, Ghorbanzade B, et al. Identification of Malassezia species isolated from patients with pityriasis versicolor using PCR-RFLP method in Markazi Province, Central Iran. Iran J Public Health. 2014;43:682–6.
Talaee R, Katiraee F, Ghaderi M, Erami M, Kazemi Alavi A, Nazeri M. Molecular identification and prevalence of Malassezia species in pityriasis versicolor patients from Kashan, Iran. Jundishapur J Microbiol. 2014;7:e11561.
Rad F, Nik-Khoo B, Yaghmaee R, Gharibi F. Terbinafine 1% cream and ketoconazole 2% cream in the treatment of pityriasis versicolor: a randomized comparative clinical trial. Pak J Med Sci. 2014;30:1273–6.
Ibekwe PU, Ogunbiyi AO, Besch R, Ruzicka T, Sárdy M. The spectrum of Malassezia species isolated from students with pityriasis vesicolor in Nigeria. Mycoses. 2015;58:203–8.
Zhou H, Tang XH, De Han J, Chen MK. Dermoscopy as an ancillary tool for the diagnosis of pityriasis versicolor. J Am Acad Dermatol. 2015;73:e205–6. A new ancillary tool for diagnosis.
Payle B, Serrano L, Bieley HC, Reyes BA. Albert’s solution versus potassium hydroxide solution in the diagnosis of tinea versicolor. Int J Dermatol. 1994;33:182–3.
del Boz J, Padilla-España L, Crespo-Erchiga V. Sample taking and direct examination in dermatomycoses. Actas Dermosifiliogr. 2016;107:65–7. Highlights the importance of correct sampling for direct examination.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Jose Manuel Rios-Yuil declares that he has no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Fungal Infections of Skin and Subcutaneous Tissue
Rights and permissions
About this article
Cite this article
Rios-Yuil, J.M. Pityriasis Versicolor: Clinical Spectrum and Diagnosis. Curr Fungal Infect Rep 10, 121–125 (2016). https://doi.org/10.1007/s12281-016-0261-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12281-016-0261-6