Abstract
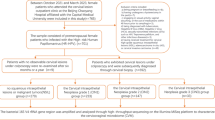
Vaginal microbiome composition was demonstrated to be associated with cervical disease. The colonization characteristics of vaginal microbes and their association with the different cervical disease status, especially cervical cancer (CC), are rarely investigated. In this cross-sectional study, we characterized the vaginal microbiome of women with different status of cervical diseases, including 22 NV + (normal tissue with HPV infection), low-grade squamous intraepithelial lesion (LSIL, n = 45), high-grade squamous intraepithelial lesion (HSIL, n = 36) and CC (n = 27) using bacterial 16S DNA sequencing. Thirty HPV-negative women with normal tissue were used as the control group. We found that higher diversity of microbiome with gradual depletion of Lactobacillus, especially L. crispatus, was associated with the severity of cervical disease. High-risk HPV16 infection was associated with higher microbiome diversity and depletion of Lactobacillus in high-grade cervical diseases (i.e. HSIL and CC). The CC group was characterized by higher levels of Fannyhessea vaginae, Prevotella, Bacteroides, Finegoldia, Vibrio, Veillonella, Peptostreptococcus, and Dialister. Co-occurrence network analyses showed that negative correlations were exclusively observed between Lactobacillus and other bacteria, and almost all non-Lactobacillus bacteria were positively correlated with each other. In particular, the most diverse and complex co-occurrence network of vaginal bacteria, as well as a complete loss of L. crispatus, was observed in women with CC. Logistic regression model identified HPV16 and Lactobacillus as significant risk and protective factors for CC, respectively. These results suggest that specific Lactobacillus species (e.g. L. crispatus and L. iners) can be used as important markers to target prevention measures prioritizing HPV16-infected women and other hrHPV-infected women for test, vaccination and treat initiatives.




Similar content being viewed by others
Data Availability
The raw data of 16S rRNA gene sequences were deposited in the CNSA (https://db.cngb.org/cnsa/) of CNGBdb (project number CNP0002796) under the accession numbers CNS0527767- CNS0527926.
References
Akram, N., Imran, M., Noreen, M., Ahmed, F., Atif, M., Fatima, Z., & Waqar, A. B. (2017). Oncogenic role of tumor viruses in humans. Viral Immunology, 30, 20–27.
Amabebe, E., & Anumba, D. O. C. (2018). The vaginal microenvironment: The physiologic role of Lactobacilli. Frontiers in Medicine, 5, 181.
Anahtar, M. N., Byrne, E. H., Doherty, K. E., Bowman, B. A., Yamamoto, H. S., Soumillon, M., Padavattan, N., Ismail, N., Moodley, A., Sabatini, M. E., et al. (2015). Cervicovaginal bacteria are a major modulator of host inflammatory responses in the female genital tract. Immunity, 42, 965–976.
Aroutcheva, A., Gariti, D., Simon, M., Shott, S., Faro, J., Simoes, J. A., Gurguis, A., & Faro, S. (2001). Defense factors of vaginal lactobacilli. American Journal of Obstetrics and Gynecology, 185, 375–379.
Audirac-Chalifour, A., Torres-Poveda, K., Bahena-Román, M., Téllez-Sosa, J., Martínez-Barnetche, J., Cortina-Ceballos, B., López-Estrada, G., Delgado-Romero, K., Burguete-García, A. I., Cantú, D., et al. (2016). Cervical microbiome and cytokine profile at various stages of cervical cancer: A pilot study. PLoS ONE, 11, e0153274.
Bolger, A. M., Lohse, M., & Usadel, B. (2014). Trimmomatic: A flexible trimmer for Illumina sequence data. Bioinformatics, 30, 2114–2120.
Boskey, E. R., Cone, R. A., Whaley, K. J., & Moench, T. R. (2001). Origins of vaginal acidity: High D/L lactate ratio is consistent with bacteria being the primary source. Human Reproduction, 16, 1809–1813.
Caporaso, J. G., Kuczynski, J., Stombaugh, J., Bittinger, K., Bushman, F. D., Costello, E. K., Fierer, N., Peña, A. G., Goodrich, J. K., Gordon, J. I., et al. (2010). QIIME allows analysis of high-throughput community sequencing data. Nature Methods, 7, 335–336.
Carrero, Y., Mosquera, J., Callejas, D., & Alvarez-Mon, M. (2015). In situ increased chemokine expression in human cervical intraepithelial neoplasia. Pathology, Research and Practice, 211, 281–285.
Cheng, L., Norenhag, J., Hu, Y. O. O., Brusselaers, N., Fransson, E., Ährlund-Richter, A., Guðnadóttir, U., Angelidou, P., Zha, Y., Hamsten, M., et al. (2020). Vaginal microbiota and human papillomavirus infection among young Swedish women. Npj Biofilms and Microbiomes., 6, 39.
Curty, G., de Carvalho, P. S., & Soares, M. A. (2019). The role of the cervicovaginal microbiome on the genesis and as a biomarker of premalignant cervical intraepithelial neoplasia and invasive cervical cancer. International Journal of Molecular Sciences, 21, 222.
Garrett, W. S. (2015). Cancer and the microbiota. Science, 348, 80–86.
Graham, S. V. (2017). The human papillomavirus replication cycle, and its links to cancer progression: A comprehensive review. Clinical Science, 131, 2201–2221.
Kroon, S. J., Ravel, J., & Huston, W. M. (2018). Cervicovaginal microbiota, women’s health, and reproductive outcomes. Fertility and Sterility, 110, 327–336.
Łaniewski, P., Ilhan, Z. E., & Herbst-Kralovetz, M. M. (2020). The microbiome and gynaecological cancer development, prevention and therapy. Nature Reviews Urology, 17, 232–250.
Li, Y., Cao, L., Han, X., Ma, Y., Liu, Y., Gao, S., & Zhang, C. (2022). Altered vaginal eukaryotic virome is associated with different cervical disease status. Virologica Sinica. https://doi.org/10.1016/j.virs.2022.12.004
Lin, W., Zhang, Q., Chen, Y., Dong, B., Xue, H., Lei, H., Lu, Y., Wei, X., & Sun, P. (2022). Changes of the vaginal microbiota in HPV infection and cervical intraepithelial neoplasia: A cross-sectional analysis. Scientific Reports, 12, 2812.
Mitra, A., MacIntyre, D. A., Lee, Y. S., Smith, A., Marchesi, J. R., Lehne, B., Bhatia, R., Lyons, D., Paraskevaidis, E., Li, J. V., et al. (2015). Cervical intraepithelial neoplasia disease progression is associated with increased vaginal microbiome diversity. Scientific Reports, 5, 16865.
Norenhag, J., Du, J., Olovsson, M., Verstraelen, H., Engstrand, L., & Brusselaers, N. (2019). The vaginal microbiota human papillomavirus and cervical dysplasia: a systematic review and network meta-analysis. BJOG an International Journal of Obstetrics and Gynaecology., 127, 171–180.
Quast, C., Pruesse, E., Yilmaz, P., Gerken, J., Schweer, T., Yarza, P., Peplies, J., & Glöckner, F. O. (2013). The SILVA ribosomal RNA gene database project: Improved data processing and web-based tools. Nucleic Acids Research, 41, D590–D596.
Rampersaud, R., Planet, P. J., Randis, T. M., Kulkarni, R., Aguilar, J. L., Lehrer, R. I., & Ratner, A. J. (2011). Inerolysin, a cholesterol-dependent cytolysin produced by Lactobacillus iners. Journal of Bacteriology, 193, 1034–1041.
Ravel, J., Gajer, P., Abdo, Z., Schneider, G. M., Koenig, S. S., McCulle, S. L., Karlebach, S., Gorle, R., Russell, J., Tacket, C. O., et al. (2011). Vaginal microbiome of reproductive-age women. Proceedings of the National Academy of Sciences of the USA, 108, 4680–4687.
Rognes, T., Flouri, T., Nichols, B., Quince, C., & Mahé, F. (2016). VSEARCH: A versatile open source tool for metagenomics. PeerJ, 4, e2584.
Schwabe, R. F., & Jobin, C. (2013). The microbiome and cancer. Nature Reviews Cancer, 13, 800–812.
Segata, N., Izard, J., Waldron, L., Gevers, D., Miropolsky, L., Garrett, W. S., & Huttenhower, C. (2011). Metagenomic biomarker discovery and explanation. Genome Biology, 12, R60.
So, K. A., Yang, E. J., Kim, N. R., Hong, S. R., Lee, J. H., Hwang, C. S., Shim, S. H., Lee, S. J., & Kim, T. J. (2020). Changes of vaginal microbiota during cervical carcinogenesis in women with human papillomavirus infection. PLoS ONE, 15, e0238705.
Torcia, M. G. (2019). Interplay among vaginal microbiome, immune response and sexually transmitted viral infections. International Journal of Molecular Sciences, 20, 226.
Usyk, M., Zolnik, C. P., Castle, P. E., Porras, C., Herrero, R., Gradissimo, A., Gonzalez, P., Safaeian, M., Schiffman, M., & Burk, R. D. (2020). Cervicovaginal microbiome and natural history of HPV in a longitudinal study. PLoS Pathogens, 16, e1008376.
Walther-António, M. R., Chen, J., Multinu, F., Hokenstad, A., Distad, T. J., Cheek, E. H., Keeney, G. L., Creedon, D. J., Nelson, H., Mariani, A., et al. (2016). Potential contribution of the uterine microbiome in the development of endometrial cancer. Genome Medicine, 8, 122.
Witkin, S. S., & Linhares, I. M. (2017). Why do lactobacilli dominate the human vaginal microbiota? BJOG an International Journal of Obstetrics and Gynaecology., 124, 606–611.
Xu, R., Liu, P., Zhang, T., Wu, Q., Zeng, M., Ma, Y., Jin, X., Xu, J., Zhang, Z., & Zhang, C. (2021a). Progressive deterioration of the upper respiratory tract and the gut microbiomes in children during the early infection stages of COVID-19. Journal of Genetics and Genomics, 48, 803–814.
Xu, R., Lu, R., Zhang, T., Wu, Q., Cai, W., Han, X., Wan, Z., Jin, X., Zhang, Z., & Zhang, C. (2021b). Temporal association between human upper respiratory and gut bacterial microbiomes during the course of COVID-19 in adults. Communications Biology, 4, 240.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Ethical Statements
The collection of samples was approved by the Ethics Committees of Obstetrics and Gynecology Hospital of Fudan University (No. 2021–103). Written informed consents were obtained from all patients before sample collection.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ma, Y., Li, Y., Liu, Y. et al. Vaginal Microbiome Dysbiosis is Associated with the Different Cervical Disease Status. J Microbiol. 61, 423–432 (2023). https://doi.org/10.1007/s12275-023-00039-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12275-023-00039-3