Abstract
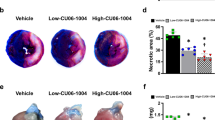
The present study was undertaken to investigate whether Cu protects vasculatures from ischemic injury in the heart. C57/B6 mice were introduced to myocardial ischemia (MI) by permanent ligation of the left anterior descending (LAD) coronary artery. Two hours post-LAD ligation, mice were intravenously injected with a Cu-albumin (Cu-alb) solution, or saline as control. At 1, 4, or 7 days post-MI, hearts were collected for further analysis. A dramatic decrease in CD31-positive endothelial cells concomitantly with abundant apoptosis, along with obstruction of blood flow, was observed in ischemic myocardium 1 day post-MI. The early Cu-alb treatment protected CD31-positive cells from apoptosis, along with a preservation of micro-vessels and a decrease in infarct size. This early vasculature preservation ensured myocardial blood perfusion and protected cardiac contractile function until 28 days post-MI. This strategy of Cu-alb treatment immediately following MI would help develop a therapeutic approach for acute heart attack patients in a clinical setting.
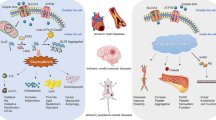
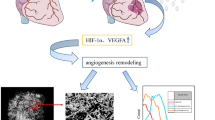
Graphical abstract





Similar content being viewed by others
Abbreviations
- AAS:
-
Atomic absorption spectrometry
- BSA:
-
Bovine serum albumin
- CCS-1:
-
Cu chaperone for superoxide dismutase-1
- Cu:
-
Copper
- Cu-alb:
-
Cu-albumin
- ECs:
-
Endothelial cells
- EF:
-
Ejection fraction
- FS:
-
Fractional shortening
- HIF-1:
-
Hypoxia-inducible factor-1
- HSA:
-
Human serum albumin
- IA:
-
Ischemic area
- LAD:
-
Left anterior descending of coronary artery
- LVEDV:
-
Left ventricular end-diastolic volume
- LVESV:
-
Left ventricular end-systolic volume
- LVIDd:
-
Left ventricular internal diameter at diastolic phase
- LVIDs:
-
Left ventricular internal diameter at systolic phase
- MI:
-
Myocardial ischemia
- OCT:
-
Optimal cutting temperature gel
- ROS:
-
Reactive oxygen species
- RM:
-
Remote myocardium from ischemia
- TUNEL:
-
Terminal deoxynucleotidyl transferase-mediated dUTP-biotin nick end labeling assay
References
Frangogiannis, N. G. (2015). Pathophysiology of myocardial infarction. Comprehensive Physiology, 5(4), 1841–1875. https://doi.org/10.1002/cphy.c150006.
Dong, Y., Chen, H., Gao, J., Liu, Y., Li, J., & Wang, J. (2019). Molecular machinery and interplay of apoptosis and autophagy in coronary heart disease. Journal of Molecular and Cellular Cardiology, 136, 27–41. https://doi.org/10.1016/j.yjmcc.2019.09.001.
McAuslan, B. R., & Reilly, W. (1980). Endothelial cell phagokinesis in response to specific metal ions. Experimental Cell Research, 130(1), 147–157. https://doi.org/10.1016/0014-4827(80)90051-8.
Hu, G. F. (1998). Copper stimulates proliferation of human endothelial cells under culture. Journal of Cellular Biochemistry, 69(3), 326–335. https://doi.org/10.1002/(sici)1097-4644(19980601)69:3<326::aid-jcb10>3.0.co;2-a.
Li, Q. F., Ding, X. Q., & Kang, Y. J. (2014). Copper promotion of angiogenesis in isolated rat aortic ring: Role of vascular endothelial growth factor. The Journal of Nutritional Biochemistry, 25(1), 44–49. https://doi.org/10.1016/j.jnutbio.2013.08.013.
Tapiero, H., Townsend, D. M., & Tew, K. D. (2003). Trace elements in human physiology and pathology. Copper. Biomedicine & Pharmacotherapy, 57(9), 386–398. https://doi.org/10.1016/s0753-3322(03)00012-x.
Fukai, T., Ushio-Fukai, M., & Kaplan, J. H. (2018). Copper transporters and copper chaperones: Roles in cardiovascular physiology and disease. American Journal of Physiology. Cell Physiology, 315(2), C186–C201. https://doi.org/10.1152/ajpcell.00132.2018.
Heller, L. J., Mohrman, D. E., & Prohaska, J. R. (2000). Decreased passive stiffness of cardiac myocytes and cardiac tissue from copper-deficient rat hearts. American Journal of Physiology. Heart and Circulatory Physiology, 278(6), H1840–H1847. https://doi.org/10.1152/ajpheart.2000.278.6.H1840.
Elsherif, L., Ortines, R. V., Saari, J. T., & Kang, Y. J. (2003). Congestive heart failure in copper-deficient mice. Experimental Biology and Medicine (Maywood, N.J.), 228(7), 811–817. https://doi.org/10.1177/15353702-0322807-06.
Rodriguez, C., & Martinez-Gonzalez, J. (2019). The role of lysyl oxidase enzymes in cardiac function and remodeling. Cells, 8(12). https://doi.org/10.3390/cells8121483.
Horn, D., & Barrientos, A. (2008). Mitochondrial copper metabolism and delivery to cytochrome c oxidase. IUBMB Life, 60(7), 421–429. https://doi.org/10.1002/iub.50.
Zuo, X., Xie, H., Dong, D., Jiang, N., Zhu, H., & Kang, Y. J. (2010). Cytochrome c oxidase is essential for copper-induced regression of cardiomyocyte hypertrophy. Cardiovascular Toxicology, 10(3), 208–215. https://doi.org/10.1007/s12012-010-9080-0.
Feng, W., Ye, F., Xue, W., Zhou, Z., & Kang, Y. J. (2009). Copper regulation of hypoxia-inducible factor-1 activity. Molecular Pharmacology, 75(1), 174–182. https://doi.org/10.1124/mol.108.051516.
Zhang, Z., Qiu, L., Lin, C., Yang, H., Fu, H., Li, R., et al. (2014). Copper-dependent and -independent hypoxia-inducible factor-1 regulation of gene expression. Metallomics, 6(10), 1889–1893. https://doi.org/10.1039/c4mt00052h.
Liu, X., Zhang, W., Wu, Z., Yang, Y., & Kang, Y. J. (2018). Copper levels affect targeting of hypoxia-inducible factor 1alpha to the promoters of hypoxia-regulated genes. The Journal of Biological Chemistry, 293(38), 14669–14677. https://doi.org/10.1074/jbc.RA118.001764.
Morrell, A., Tallino, S., Yu, L., & Burkhead, J. L. (2017). The role of insufficient copper in lipid synthesis and fatty-liver disease. IUBMB Life, 69(4), 263–270. https://doi.org/10.1002/iub.1613.
Hamilton, I. M., Gilmore, W. S., & Strain, J. J. (2000). Marginal copper deficiency and atherosclerosis. Biological Trace Element Research, 78(1-3), 179–189. https://doi.org/10.1385/BTER:78:1-3:179.
Klevay, L. M. (2000). Cardiovascular disease from copper deficiency--a history. The Journal of Nutrition, 130(2S Suppl), 489S–492S. https://doi.org/10.1093/jn/130.2.489S.
DiNicolantonio, J. J., Mangan, D., & O’Keefe, J. H. (2018). Copper deficiency may be a leading cause of ischaemic heart disease. Open Heart, 5(2), e000784. https://doi.org/10.1136/openhrt-2018-000784.
Galhardi, C. M., Diniz, Y. S., Faine, L. A., Rodrigues, H. G., Burneiko, R. C., Ribas, B. O., et al. (2004). Toxicity of copper intake: Lipid profile, oxidative stress and susceptibility to renal dysfunction. Food and Chemical Toxicology, 42(12), 2053–2060. https://doi.org/10.1016/j.fct.2004.07.020.
Hosseini, M. J., Shaki, F., Ghazi-Khansari, M., & Pourahmad, J. (2014). Toxicity of copper on isolated liver mitochondria: Impairment at complexes I, II, and IV leads to increased ROS production. Cell Biochemistry and Biophysics, 70(1), 367–381. https://doi.org/10.1007/s12013-014-9922-7.
Cervantes-Cervantes, M. P., Calderon-Salinas, J. V., Albores, A., & Munoz-Sanchez, J. L. (2005). Copper increases the damage to DNA and proteins caused by reactive oxygen species. Biological Trace Element Research, 103(3), 229–248. https://doi.org/10.1385/BTER:103:3:229.
Xie, H., & Kang, Y. J. (2009). Role of copper in angiogenesis and its medicinal implications. Current Medicinal Chemistry, 16(10), 1304–1314. https://doi.org/10.2174/092986709787846622.
Xiao, Y., Wang, T., Song, X., Yang, D., Chu, Q., & Kang, Y. J. (2020). Copper promotion of myocardial regeneration. Experimental Biology and Medicine (Maywood, N.J.), 245(10), 911–921. https://doi.org/10.1177/1535370220911604.
Jiang, Y., Reynolds, C., Xiao, C., Feng, W., Zhou, Z., Rodriguez, W., et al. (2007). Dietary copper supplementation reverses hypertrophic cardiomyopathy induced by chronic pressure overload in mice. The Journal of Experimental Medicine, 204(3), 657–666. https://doi.org/10.1084/jem.20061943.
Mroczek-Sosnowska, N., Sawosz, E., Vadalasetty, K. P., Lukasiewicz, M., Niemiec, J., Wierzbicki, M., et al. (2015). Nanoparticles of copper stimulate angiogenesis at systemic and molecular level. International Journal of Molecular Sciences, 16(3), 4838–4849. https://doi.org/10.3390/ijms16034838.
Qiu, L., Ding, X., Zhang, Z., & Kang, Y. J. (2012). Copper is required for cobalt-induced transcriptional activity of hypoxia-inducible factor-1. The Journal of Pharmacology and Experimental Therapeutics, 342(2), 561–567. https://doi.org/10.1124/jpet.112.194662.
Zhang, W., Zhao, X., Xiao, Y., Chen, J., Han, P., Zhang, J., et al. (2016). The association of depressed angiogenic factors with reduced capillary density in the Rhesus monkey model of myocardial ischemia. Metallomics, 8(7), 654–662. https://doi.org/10.1039/c5mt00332f.
Wu, Z., Zhang, W., & Kang, Y. J. (2019). Copper affects the binding of HIF-1alpha to the critical motifs of its target genes. Metallomics, 11(2), 429–438. https://doi.org/10.1039/c8mt00280k.
Kang, Y. J., & Zheng, L. (2013). Rejuvenation: An integrated approach to regenerative medicine. [Review]. Regenerative Medicine Research, 1(1), 7. https://doi.org/10.1186/2050-490X-1-7.
Cochain, C., Channon, K. M., & Silvestre, J. S. (2013). Angiogenesis in the infarcted myocardium. Antioxidants & Redox Signaling, 18(9), 1100–1113. https://doi.org/10.1089/ars.2012.4849.
Wirth, P. L., & Linder, M. C. (1985). Distribution of copper among components of human serum. Journal of the National Cancer Institute, 75(2), 277–284.
Cheng, X., Hou, J., Liu, J., Sun, X., Sheng, Q., Han, P., et al. (2017). Safety evaluation of sevoflurane as anesthetic agent in mouse model of myocardial ischemic infarction. Cardiovascular Toxicology, 17(2), 150–156. https://doi.org/10.1007/s12012-016-9368-9.
Li, K., Li, C., Xiao, Y., Wang, T., & Kang, Y. J. (2018). The loss of copper is associated with the increase in copper metabolism MURR domain 1 in ischemic hearts of mice. Experimental Biology and Medicine (Maywood, N.J.), 243(9), 780–785. https://doi.org/10.1177/1535370218773055.
Jayakumar, S., Micallef-Eynaud, P. D., Lyon, T. D., Cramb, R., Jilaihawi, A. N., & Prakash, D. (2005). Acquired copper deficiency following prolonged jejunostomy feeds. Annals of Clinical Biochemistry, 42(Pt 3), 227–231. https://doi.org/10.1258/0004563053857879.
Nair, A. B., & Jacob, S. (2016). A simple practice guide for dose conversion between animals and human. Journal of Basic and Clinical Pharmacy, 7(2), 27–31. https://doi.org/10.4103/0976-0105.177703.
Takagawa, J., Zhang, Y., Wong, M. L., Sievers, R. E., Kapasi, N. K., Wang, Y., et al. (2007). Myocardial infarct size measurement in the mouse chronic infarction model: Comparison of area- and length-based approaches. Journal of Applied Physiology (Bethesda, MD: 1985), 102(6), 2104–2111. https://doi.org/10.1152/japplphysiol.00033.2007.
Kobayashi, K., Maeda, K., Takefuji, M., Kikuchi, R., Morishita, Y., Hirashima, M., et al. (2017). Dynamics of angiogenesis in ischemic areas of the infarcted heart. Scientific Reports, 7(1), 7156. https://doi.org/10.1038/s41598-017-07524-x.
Getz, J., Lin, D., & Medeiros, D. M. (2011). The cardiac copper chaperone proteins Sco1 and CCS are up-regulated, but Cox 1 and Cox4 are down-regulated, by copper deficiency. Biological Trace Element Research, 143(1), 368–377. https://doi.org/10.1007/s12011-010-8858-z.
Frangogiannis, N. G. (2006). The mechanistic basis of infarct healing. Antioxidants & Redox Signaling, 8(11-12), 1907–1939. https://doi.org/10.1089/ars.2006.8.1907.
Zheng, L., Han, P., Liu, J., Li, R., Yin, W., Wang, T., et al. (2015). Role of copper in regression of cardiac hypertrophy. Pharmacology & Therapeutics, 148, 66–84. https://doi.org/10.1016/j.pharmthera.2014.11.014.
Varga, I., Kyselovic, J., Galfiova, P., & Danisovic, L. (2017). The non-cardiomyocyte cells of the heart. Their possible roles in exercise-induced cardiac regeneration and remodeling. Advances in Experimental Medicine and Biology, 999, 117–136. https://doi.org/10.1007/978-981-10-4307-9_8.
Narayanan, G., Bharathidevi, S. R., Vuyyuru, H., Muthuvel, B., & Konerirajapuram Natrajan, S. (2013). CTR1 silencing inhibits angiogenesis by limiting copper entry into endothelial cells. PLoS One, 8(9), e71982. https://doi.org/10.1371/journal.pone.0071982.
Li, S., Xie, H., Li, S., & Kang, Y. J. (2012). Copper stimulates growth of human umbilical vein endothelial cells in a vascular endothelial growth factor-independent pathway. Experimental Biology and Medicine (Maywood, N.J.), 237(1), 77–82. https://doi.org/10.1258/ebm.2011.011267.
Karginova, O., Weekley, C. M., Raoul, A., Alsayed, A., Wu, T., Lee, S. S., et al. (2019). Inhibition of copper transport induces apoptosis in triple-negative breast cancer cells and suppresses tumor angiogenesis. Molecular Cancer Therapeutics, 18(5), 873–885. https://doi.org/10.1158/1535-7163.MCT-18-0667.
Henry, N. L., Dunn, R., Merjaver, S., Pan, Q., Pienta, K. J., Brewer, G., et al. (2006). Phase II trial of copper depletion with tetrathiomolybdate as an antiangiogenesis strategy in patients with hormone-refractory prostate cancer. Oncology, 71(3-4), 168–175. https://doi.org/10.1159/000106066.
Moriguchi, M., Nakajima, T., Kimura, H., Watanabe, T., Takashima, H., Mitsumoto, Y., et al. (2002). The copper chelator trientine has an antiangiogenic effect against hepatocellular carcinoma, possibly through inhibition of interleukin-8 production. International Journal of Cancer, 102(5), 445–452. https://doi.org/10.1002/ijc.10740.
Brem, S., Grossman, S. A., Carson, K. A., New, P., Phuphanich, S., Alavi, J. B., et al. (2005). Phase 2 trial of copper depletion and penicillamine as antiangiogenesis therapy of glioblastoma. Neuro-Oncology, 7(3), 246–253. https://doi.org/10.1215/S1152851704000869.
Li, C., Wang, T., Xiao, Y., Li, K., Meng, X., & James Kang, Y. (2021). COMMD1 upregulation is involved in copper efflux from ischemic hearts. Experimental Biology and Medicine (Maywood, N.J.), 246(5), 607–616. https://doi.org/10.1177/1535370220969844.
Liu, J., Chen, C., Liu, Y., Sun, X., Ding, X., Qiu, L., et al. (2018). Trientine selectively delivers copper to the heart and suppresses pressure overload-induced cardiac hypertrophy in rats. Experimental Biology and Medicine (Maywood, N.J.), 243(14), 1141–1152. https://doi.org/10.1177/1535370218813988.
Zhang, L., Ward, M. L., Phillips, A. R., Zhang, S., Kennedy, J., Barry, B., et al. (2013). Protection of the heart by treatment with a divalent-copper-selective chelator reveals a novel mechanism underlying cardiomyopathy in diabetic rats. Cardiovascular Diabetology, 12, 123. https://doi.org/10.1186/1475-2840-12-123.
Helsel, M. E., & Franz, K. J. (2015). Pharmacological activity of metal binding agents that alter copper bioavailability. Dalton Transactions, 44(19), 8760–8770. https://doi.org/10.1039/c5dt00634a.
Choo, X. Y., Liddell, J. R., Huuskonen, M. T., Grubman, A., Moujalled, D., Roberts, J., et al. (2018). Cu(II)(atsm) attenuates neuroinflammation. Frontiers in Neuroscience, 12, 668. https://doi.org/10.3389/fnins.2018.00668.
Soma, S., Latimer, A. J., Chun, H., Vicary, A. C., Timbalia, S. A., Boulet, A., et al. (2018). Elesclomol restores mitochondrial function in genetic models of copper deficiency. Proceedings of the National Academy of Sciences of the United States of America, 115(32), 8161–8166. https://doi.org/10.1073/pnas.1806296115.
Tural, K., Ozden, O., Bilgi, Z., Kubat, E., Ermutlu, C. S., Merhan, O., et al. (2020). The protective effect of betanin and copper on heart and lung in endorgan ischemia reperfusion injury. Bratislavské Lekárske Listy, 121(3), 211–217. https://doi.org/10.4149/BLL_2020_032.
Sharma, A. K., Kumar, A., Sahu, M., Sharma, G., Datusalia, A. K., & Rajput, S. K. (2018). Exercise preconditioning and low dose copper nanoparticles exhibits cardioprotection through targeting GSK-3beta phosphorylation in ischemia/reperfusion induced myocardial infarction. Microvascular Research, 120, 59–66. https://doi.org/10.1016/j.mvr.2018.06.003.
Srivastava, S., Blower, P. J., Aubdool, A. A., Hider, R. C., Mann, G. E., & Siow, R. C. (2016). Cardioprotective effects of Cu((II))ATSM in human vascular smooth muscle cells and cardiomyocytes mediated by Nrf2 and DJ-1. Scientific Reports, 6(1), 7. https://doi.org/10.1038/s41598-016-0012-5.
Linder, M. C., Wooten, L., Cerveza, P., Cotton, S., Shulze, R., & Lomeli, N. (1998). Copper transport. The American Journal of Clinical Nutrition, 67(5 Suppl), 965S–971S. https://doi.org/10.1093/ajcn/67.5.965S.
Moriya, M., Ho, Y. H., Grana, A., Nguyen, L., Alvarez, A., Jamil, R., et al. (2008). Copper is taken up efficiently from albumin and alpha2-macroglobulin by cultured human cells by more than one mechanism. American Journal of Physiology. Cell Physiology, 295(3), C708–C721. https://doi.org/10.1152/ajpcell.00029.2008.
Zuo, X., Dong, D., Sun, M., Xie, H., & Kang, Y. J. (2013). Homocysteine restricts copper availability leading to suppression of cytochrome C oxidase activity in phenylephrine-treated cardiomyocytes. PLoS One, 8(6), e67549. https://doi.org/10.1371/journal.pone.0067549.
Sun, M., Zuo, X., Li, R., Wang, T., & Kang, Y. J. (2014). Vascular endothelial growth factor recovers suppressed cytochrome c oxidase activity by restoring copper availability in hypertrophic cardiomyocytes. Experimental Biology and Medicine (Maywood, N.J.), 239(12), 1671–1677. https://doi.org/10.1177/1535370214541910.
Acknowledgements
The authors thank Dr. Jiaming Liu, Mr. Yi Ren, Ms. Qin Sheng, and Ms. Yuan Ma for assistance in animal care and surgery and thank Ms. Fang Nan for technique support in histological analysis.
Funding
This work was supported by China Postdoctoral Science Foundation (No. 2020M673261).
Author information
Authors and Affiliations
Contributions
Y.X., X.S., T.W., and Y.J.K. designed the experiments; Y.X., X.S., T.W., X.M., Q.F., X.S., and K.L. carried out the experiments, data analysis, and result interpretation; Y.J.K. and Y.X. drafted the manuscript; Y.J.K. revised the draft and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethics Approval
No human studies were carried out by the authors for this article. All institutional and national guidelines for the care and use of laboratory animals were followed and approved by Institutional Animal Care and Use Committee (IACUC) of Sichuan University West China Hospital (Approval No. 2020238A).
Conflict of Interest
The authors declare no competing interests.
Additional information
Associate Editor Nicola Smart oversaw the review of this article
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 4.57 mb)
Rights and permissions
About this article
Cite this article
Xiao, Y., Song, X., Wang, T. et al. Copper Preserves Vasculature Structure and Function by Protecting Endothelial Cells from Apoptosis in Ischemic Myocardium. J. of Cardiovasc. Trans. Res. 14, 1146–1155 (2021). https://doi.org/10.1007/s12265-021-10128-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-021-10128-6