Abstract
Ligustrazine is one of the alkaloid compounds isolated from the traditional Chinese herb, which shows protective effects on cardiovascular disorders. High homocysteine (Hcy) level can predict cardiovascular-related events including death. In this study, we used Hcy to stimulate the human umbilical vein endothelial cells (HUVECs) and investigated the protective effect of ligustrazine on endothelial dysfunction by assessing the cell apoptosis, oxidative damage, mitochondrial dysfunction, and the potential molecular pathways. Our results clearly showed that ligustrazine increased HUVEC cell viability, decreased the dehydrogenase (LDH) level, and inhibited HUVEC apoptosis, which was associated with the attenuation of attenuated oxidative damage. The mitochondrial-dependent pathway was closely related in the regulation of ligustrazine, reflected by the attenuated mitochondrial membrane potential change and decreased cytochrome c release from the mitochondria to the cytosol. Ligustrazine may protect Hcy-induced apoptosis in HUVECs by attenuating oxidative damage and modulating mitochondrial dysfunction.





Similar content being viewed by others
References
Clarke, R., Daly, L., Robinson, K., Naughten, E., Cahalane, S., Fowler, B., et al. (1991). Hyperhomocysteinemia: an independent risk factor for vascular disease. The New England Journal of Medicine, 324(17), 1149–1155. https://doi.org/10.1056/nejm199104253241701.
Marasini, B., Massarotti, M., & Biondi, M. L. (2002). Homocysteine and vascular diseases. Circulation, 106(7), e33.
Nygard, O., Nordrehaug, J. E., Refsum, H., Ueland, P. M., Farstad, M., & Vollset, S. E. (1997). Plasma homocysteine levels and mortality in patients with coronary artery disease. The New England Journal of Medicine, 337(4), 230–236. https://doi.org/10.1056/nejm199707243370403.
Wu, X., Zhang, L., Miao, Y., Yang, J., Wang, X., Wang, C. C., et al. (2018). Homocysteine causes vascular endothelial dysfunction by disrupting endoplasmic reticulum redox homeostasis. Redox Biology, 20, 46–59. https://doi.org/10.1016/j.redox.2018.09.021.
Shi, W., Wang, X., Shih, D. M., Laubach, V. E., Navab, M., & Lusis, A. J. (2002). Paradoxical reduction of fatty streak formation in mice lacking endothelial nitric oxide synthase. Circulation, 105(17), 2078–2082.
Liu, C., & Huang, Y. (2016). Chinese herbal medicine on cardiovascular diseases and the mechanisms of action. Frontiers in Pharmacology, 7, 469. https://doi.org/10.3389/fphar.2016.00469.
Chang, Y., Hsiao, G., Chen, S. H., Chen, Y. C., Lin, J. H., Lin, K. H., et al. (2007). Tetramethylpyrazine suppresses HIF-1alpha, TNF-alpha, and activated caspase-3 expression in middle cerebral artery occlusion-induced brain ischemia in rats. Acta Pharmacologica Sinica, 28(3), 327–333. https://doi.org/10.1111/j.1745-7254.2007.00514.x.
Fan, L. H., Wang, K. Z., Cheng, B., Wang, C. S., & Dang, X. Q. (2006). Anti-apoptotic and neuroprotective effects of tetramethylpyrazine following spinal cord ischemia in rabbits. BMC Neuroscience, 7, 48. https://doi.org/10.1186/1471-2202-7-48.
Wu, H. J., Hao, J., Wang, S. Q., Jin, B. L., & Chen, X. B. (2012). Protective effects of ligustrazine on TNF-alpha-induced endothelial dysfunction. European Journal of Pharmacology, 674(2–3), 365–369. https://doi.org/10.1016/j.ejphar.2011.10.046.
Yang, C., Xu, Y., Zhou, H., Yang, L., Yu, S., Gao, Y., et al. (2016). Tetramethylpyrazine protects CoCl2-induced apoptosis in human umbilical vein endothelial cells by regulating the PHD2/HIF/1alpha-VEGF pathway. Molecular Medicine Reports, 13(2), 1287–1296. https://doi.org/10.3892/mmr.2015.4679.
Tveden-Nyborg, P., Bergmann, T. K., & Lykkesfeldt, J. (2018). Basic & clinical pharmacology & toxicology policy for experimental and clinical studies. Basic & Clinical Pharmacology & Toxicology, 123(3), 233–235. https://doi.org/10.1111/bcpt.13059.
Deshmukh, M., & Johnson, E. M., Jr. (1998). Evidence of a novel event during neuronal death: development of competence-to-die in response to cytoplasmic cytochrome c. Neuron, 21(4), 695–705.
Rajendran, P., Rengarajan, T., Thangavel, J., Nishigaki, Y., Sakthisekaran, D., Sethi, G., et al. (2013). The vascular endothelium and human diseases. International Journal of Biological Sciences, 9(10), 1057–1069. https://doi.org/10.7150/ijbs.7502.
Ansar, S., Koska, J., & Reaven, P. D. (2011). Postprandial hyperlipidemia, endothelial dysfunction and cardiovascular risk: focus on incretins. Cardiovascular Diabetology, 10, 61. https://doi.org/10.1186/1475-2840-10-61.
Feletou, M., & Vanhoutte, P. M. (2006). Endothelium-derived hyperpolarizing factor: where are we now? Arteriosclerosis, Thrombosis, and Vascular Biology, 26(6), 1215–1225. https://doi.org/10.1161/01.ATV.0000217611.81085.c5.
Suwaidi, J. A., Hamasaki, S., Higano, S. T., Nishimura, R. A., Holmes, D. R., Jr., & Lerman, A. (2000). Long-term follow-up of patients with mild coronary artery disease and endothelial dysfunction. Circulation, 101(9), 948–954.
Ross, R. (1999). Atherosclerosis--an inflammatory disease. The New England Journal of Medicine, 340(2), 115–126. https://doi.org/10.1056/nejm199901143400207.
Hofmann, M. A., Lalla, E., Lu, Y., Gleason, M. R., Wolf, B. M., Tanji, N., et al. (2001). Hyperhomocysteinemia enhances vascular inflammation and accelerates atherosclerosis in a murine model. The Journal of Clinical Investigation, 107(6), 675–683. https://doi.org/10.1172/jci10588.
Zhang, Z., Wei, C., Zhou, Y., Yan, T., Wang, Z., Li, W., et al. (2017). Homocysteine induces apoptosis of human umbilical vein endothelial cells via mitochondrial dysfunction and endoplasmic reticulum stress. Oxidative Medicine and Cellular Longevity, 2017, 5736506. https://doi.org/10.1155/2017/5736506.
Peng, W., Hucks, D., Priest, R. M., Kan, Y. M., & Ward, J. P. (1996). Ligustrazine-induced endothelium-dependent relaxation in pulmonary arteries via an NO-mediated and exogenous L-arginine-dependent mechanism. British Journal of Pharmacology, 119(5), 1063–1071. https://doi.org/10.1111/j.1476-5381.1996.tb15778.x.
Zhao, T., Fu, Y., Sun, H., & Liu, X. (2018). Ligustrazine suppresses neuron apoptosis via the Bax/Bcl-2 and caspase-3 pathway in PC12 cells and in rats with vascular dementia. IUBMB Life, 70(1), 60–70. https://doi.org/10.1002/iub.1704.
Chen, J., Chen, J., Wang, X., Wang, C., Cao, W., Zhao, Y., et al. (2016). Ligustrazine alleviates acute pancreatitis by accelerating acinar cell apoptosis at early phase via the suppression of p38 and Erk MAPK pathways. Biomedicine & Pharmacotherapy, 82, 1–7. https://doi.org/10.1016/j.biopha.2016.04.048.
Pan, J., Shang, J. F., Jiang, G. Q., & Yang, Z. X. (2015). Ligustrazine induces apoptosis of breast cancer cells in vitro and in vivo. Journal of Cancer Research and Therapeutics, 11(2), 454–458. https://doi.org/10.4103/0973-1482.147378.
Yip, K. W., & Reed, J. C. (2008). Bcl-2 family proteins and cancer. Oncogene, 27(50), 6398–6406. https://doi.org/10.1038/onc.2008.307.
Xu, Z., Lu, G., & Wu, F. (2009). Simvastatin suppresses homocysteine-induced apoptosis in endothelial cells: roles of caspase-3, cIAP-1 and cIAP-2. Hypertension Research, 32(5), 375–380. https://doi.org/10.1038/hr.2009.24.
Tait, S. W., & Green, D. R. (2010). Mitochondria and cell death: outer membrane permeabilization and beyond. Nature Reviews. Molecular Cell Biology, 11(9), 621–632. https://doi.org/10.1038/nrm2952.
Boatright, K. M., & Salvesen, G. S. (2003). Mechanisms of caspase activation. Current Opinion in Cell Biology, 15(6), 725–731.
Saleh, F. A., Whyte, M., & Genever, P. G. (2011). Effects of endothelial cells on human mesenchymal stem cell activity in a three-dimensional in vitro model. European Cells & Materials, 22, 242–257 discussion 257.
Funding
The study was supported by the Natural Science Foundation of China (81770353).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Research Involving Human Participants and/or Animals
The study does not contain any research involving Human Participants and/or Animals.
Informed Consent
Not applicable.
Additional information
Associate Editor Adrian Chester oversaw the review of this article.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Figure 6
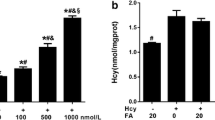
Effects of Ligustrazine on NO production in response to homocysteine. a, NO assay kit was used to measure the dose-dependent effects of homocysteine treatment for 24 h on NO production in HUVECs culture medium. b, Effects of different dose of ligustrazine on NO production in HUVECs culture medium in response to 4 mM homocysteine. Data are presented as mean ± SD. *p < 0.05, **p < 0.01 and ***p < 0.001 compared to control group, #p < 0.05 and ##p < 0.01 compared to only Hcy treated group (one-way ANOVA). (PNG 33 kb)
Rights and permissions
About this article
Cite this article
Fan, X., Wang, E., He, J. et al. Ligustrazine Protects Homocysteine-Induced Apoptosis in Human Umbilical Vein Endothelial Cells by Modulating Mitochondrial Dysfunction. J. of Cardiovasc. Trans. Res. 12, 591–599 (2019). https://doi.org/10.1007/s12265-019-09900-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-019-09900-6