Abstract
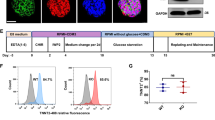
Hypertrophic cardiomyopathy (HCM), characterized by unexplained left ventricular hypertrophy, is one of the most common heritable cardiovascular diseases. The myosin regulatory light chain (MYL2) mutation R58Q has been associated with severe cardiac hypertrophy and sudden cardiac death (SCD). Herein, we provide the first patient-specific, induced pluripotent stem cell–derived cardiomyocyte (iPSC-CM) model of MYL2-R58Q. The MYL2-R58Q iPSC-CMs were nearly 30% larger than control iPSC-CMs at day 60. The percentage of myofibrillar disarray and cells with irregular beating in MYL2-R58Q iPSC-CMs was significantly higher than that in control cells. MYL2-R58Q iPSC-CMs had significantly decreased peak ΔF/F0 of calcium transients and delayed decay time than controls. Additionally, the L-type Ca2+ channel (LTCC) (ICa,L) density at 0 mV was reduced significantly by 45.3%. Overall, the MYL2-R58Q iPSC-CMs recapitulated the HCM phenotype by exhibiting hypertrophy, myofibrillar disarray, increased irregular beating, decreased [Ca2+]i transients, and unexpectedly a nearly 50% reduction in LTCC peak current.





Similar content being viewed by others
Abbreviations
- HCM:
-
Hypertrophic cardiomyopathy
- MYL2:
-
Myosin regulatory light chain
- SCD:
-
Sudden cardiac death
- iPSC-CM:
-
Induced pluripotent stem cell–derived cardiomyocyte
- LTCC (ICa,L):
-
L-type Ca2+ channel
- MYH7:
-
Myosin heavy chain 7
- MYBPC3:
-
Cardiac myosin binding protein C
- TNNT2:
-
Cardiac muscle troponin T
- SR:
-
Sarcoplasmic reticulum
- CICR:
-
Calcium-induced calcium release
References
Maron, B. J. (2002). Hypertrophic cardiomyopathy - a systematic review. JAMA-Journal of the American Medical Association, 287(10), 1308–1320.
Ashrafian, H., & Watkins, H. (2007). Reviews of translational medicine and genomics in cardiovascular disease: new disease taxonomy and therapeutic implications - Cardiomyopathies: therapeutics based on molecular phenotype. Journal of the American College of Cardiology, 49(12), 1251–1264.
Maron, B. J., et al. (1996). Sudden death in young competitive athletes - clinical, demographic, and pathological profiles. JAMA-Journal of the American Medical Association, 276(3), 199–204.
Jarcho, J. A., et al. (1989). Mapping a gene for familial hypertrophic cardiomyopathy to chromosome-14q1. New England Journal of Medicine., 321(20), 1372–1378(2014).
Maron, B. J., et al. (2014). Hypertrophic cardiomyopathy: present and future, with translation into contemporary cardiovascular medicine. Journal of the American College of Cardiology, 64(11), 1188–1188.
Ojala, M., et al. (2016). Mutation-specific phenotypes in hiPSC-derived cardiomyocytes carrying either myosin-binding protein C or alpha-tropomyosin mutation for hypertrophic cardiomyopathy. Stem Cells International, 2016, 1684792.
Alcalai, R., Seidman, J. G., & Seidman, C. E. (2008). Genetic basis of hypertrophic cardiomyopathy: From bench to the clinics. Journal of Cardiovascular Electrophysiology, 19(1), 104–110.
Arad, M., Seidman, J. G., & Seidman, C. E. (2002). Phenotypic diversity in hypertrophic cardiomyopathy. Human Molecular Genetics, 11(20), 2499–2506.
Marian, A. J., & Roberts, R. (2001). The molecular genetic basis for hypertrophic cardiomyopathy. Journal of Molecular and Cellular Cardiology, 33(4), 655–670.
Morita, H., et al. (2008). Shared genetic causes of cardiac hypertrophy in children and adults. New England Journal of Medicine, 358(18), 1899–1908.
Olsson, M. C., Patel, J. R., Fitzsimons, D. P., Walker, J. W., & Moss, R. L. (2004). Basal myosin light chain phosphorylation is a determinant of Ca2+ sensitivity of force and activation dependence of the kinetics of myocardial force development. American Journal of Physiology-Heart and Circulatory Physiology, 287(6), H2712–H2718.
Rayment, I., et al. (1993). Structure of the actin-myosin complex and its implications for muscle-contraction. Science, 261(5117), 58–65.
Flavigny, J., et al. (1998). Identification of two novel mutations in the ventricular regulatory myosin light chain gene (MYL2) associated with familial and classical forms of hypertrophic cardiomyopathy. Journal of Molecular Medicine, 76(3–4), 208–214.
Huang, W. R., et al. (2016). Gene expression patterns in transgenic mouse models of hypertrophic cardiomyopathy caused by mutations in myosin regulatory light chain. Archives of Biochemistry and Biophysics, 601(121-132), 121–132.
Lan, F., et al. (2013). Abnormal calcium handling properties underlie familial hypertrophic cardiomyopathy pathology in patient-specific induced pluripotent stem cells. Cell Stem Cell, 12(1), 101–113.
Mettikolla, P., et al. (2011). Cross-bridge kinetics in myofibrils containing familial hypertrophic cardiomyopathy R58Q mutation in the regulatory light chain of myosin. Journal of Theoretical Biology, 284(1), 71–81.
Abraham, T. P., et al. (2009). Diastolic dysfunction in familial hypertrophic cardiomyopathy transgenic model mice. Cardiovascular Research, 82(1), 84–92.
Wang, Y., et al. (2006). Prolonged Ca2+ and force transients in myosin RLC transgenic mouse fibers expressing malignant and benign FHC mutations. Journal of Molecular Biology, 361(2), 286–299.
Grey, C., Mery, A., & Puceat, M. (2005). Fine-tuning in Ca2+ homeostasis underlies progression of cardiomyopathy in myocytes derived from genetically modified embryonic stem cells. Human Molecular Genetics, 14(10), 1367–1377.
Weyhrauch, D. L., et al. (2016). Whole exome sequencing and heterologous cellular electrophysiology studies elucidate a novel loss-of-function mutation in the CACNA1A-encoded neuronal P/Q-type calcium channel in a child with congenital hypotonia and developmental delay. Pediatric Neurology, 55, 46–51.
Hu, D., et al. (2010). Dual variation in SCN5A and CACNB2b underlies the development of cardiac conduction disease without Brugada syndrome. Pace-Pacing and Clinical Electrophysiology, 33(3), 274–285.
McKenna, W. J., Stewart, J. T., Nihoyannopoulos, P., McGinty, F., & Davies, M. J. (1990). Hypertrophic cardiomyopathy without hypertrophy: two families with myocardial disarray in the absence of increased myocardial mass. British Heart Journal, 63(5), 287–290.
Varnava, A. M., et al. (2001). Hypertrophic cardiomyopathy: histopathological features of sudden death in cardiac troponin T disease. Circulation, 104(12), 1380–1384.
Becker, J. R., et al. (2011). Human cardiomyopathy mutations induce myocyte hyperplasia and activate hypertrophic pathways during cardiogenesis in zebrafish. Disease Models & Mechanisms, 4(3), 400–410.
GeisterferLowrance, A. A. T., et al. (1996). A mouse model of familial hypertrophic cardiomyopathy. Science, 272(5262), 731–734.
Tsoutsman, T., et al. (2008). Severe heart failure and early mortality in a double-mutation mouse model of familial hypertrophic cardiomyopathy. Circulation, 117(14), 1820–1831.
Kazmierczak, K., et al. (2013). Discrete effects of A57G-myosin essential light chain mutation associated with familial hypertrophic cardiomyopathy. American Journal of Physiology-Heart and Circulatory Physiology, 305(4), H575–H589.
Han, L., et al. (2014). Study familial hypertrophic cardiomyopathy using patient-specific induced pluripotent stem cells. Cardiovascular Research, 104(2), 258–269.
Tanaka, A., et al. (2014). Endothelin-1 induces myofibrillar disarray and contractile vector variability in hypertrophic cardiomyopathy-induced pluripotent stem cell-derived cardiomyocytes. Journal of the American Heart Association, 3(6).
Bers, D. M. (2008). Calcium cycling and signaling in cardiac myocytes. Annual Review of Physiology, 70, 23–49.
Murphy, S. L., et al. (2016). Evaluation of the Mayo Clinic phenotype-based genotype predictor score in patients with clinically diagnosed hypertrophic cardiomyopathy. Journal of Cardiovascular Translational Research, 9(2), 153–161.
Chen, J., et al. (1998). Selective requirement of myosin light chain 2v in embryonic heart function. The Journal of Biological Chemistry, 273(2), 1252–1256.
Duggal, D., et al. (2015). Effect of a myosin regulatory light chain mutation K104E on actin-myosin interactions. American Journal of Physiology-Heart and Circulatory Physiology, 308(10), H1248–H1257.
Greenberg, M. J., et al. (2009). Regulatory light chain mutations associated with cardiomyopathy affect myosin mechanics and kinetics. Journal of Molecular and Cellular Cardiology, 46(1), 108–115.
McConnell, B. K., et al. (2001). Comparison of two murine models of familial hypertrophic cardiomyopathy. Circulation Research, 88(4), 383–389.
Frey, N., et al. (2000). Transgenic rat hearts expressing a human cardiac troponin T deletion reveal diastolic dysfunction and ventricular arrhythmias. Cardiovascular Research, 47(2), 254–264.
Freeman, L. M., Rush, J. E., Stern, J. A., Huggins, G. S., & Maron, M. S. (2017). Feline hypertrophic cardiomyopathy: a spontaneous large animal model of human HCM. Cardiology Research, 8(4), 139–142.
Marian, A. J., et al. (1999). A transgenic rabbit model for human hypertrophic cardiomyopathy. Journal of Clinical Investigation, 104(12), 1683–1692.
Takahashi, K., et al. (2007). Induction of pluripotent stem cells from adult human fibroblasts by defined factors. Cell, 131(5), 861–872.
Yu, J. Y., et al. (2007). Induced pluripotent stem cell lines derived from human somatic cells. Science., 318(5858), 1917–1920.
Musunuru, K., et al. (2018). Induced pluripotent stem cells for cardiovascular disease modeling and precision medicine: a scientific statement from the American Heart Association. Circ Genom Precis Med., 11(1), e000043.
Varnava, A. M., Elliott, P. M., Sharma, S., McKenna, W. J., & Davies, M. J. (2000). Hypertrophic cardiomyopathy: the interrelation of disarray, fibrosis, and small vessel disease. Heart, 84(5), 476–482.
Iida, K., Yutani, C., Imakita, M., & Ishibashi-Ueda, H. (1998). Comparison of percentage area of myocardial fibrosis and disarray in patients with classical form and dilated phase of hypertrophic cardiomyopathy. Journal of Cardiology, 32(3), 173–180.
Sun, N., et al. (2012). Patient-specific induced pluripotent stem cells as a model for familial dilated cardiomyopathy. Science Translational Medicine, 4(130).
Irving, M., Lombardi, V., Piazzesi, G., & Ferenczi, M. A. (1992). Myosin head movements are synchronous with the elementary force-generating process in muscle. Nature, 357(6374), 156–158.
Morano, I. (1999). Tuning the human heart molecular motors by myosin light chains. Journal of Molecular Medicine-JMM, 77(7), 544–555.
Thandroyen, F. T., et al. (1991). Intracellular calcium transients and arrhythmia in isolated heart cells. Circulation Research, 69(3), 810–819.
Lee, K. S., Marban, E., & Tsien, R. W. (1985). Inactivation of calcium channels in mammalian heart-cells - joint dependence on membrane-potential and intracellular calcium. J Physiology-London, 364(Jul), 395–411.
Funding
This study was funded by the Mayo Clinic Windland Smith Rice Comprehensive Sudden Cardiac Death Program (MJA) and the Tsai Family Fund for HCM (SRO, RAN, HVS, and MJA).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
MJA is a consultant for Audentes Therapeutics, Boston Scientific, Gilead Sciences, Invitae, Medtronic, MyoKardia, and St. Jude Medical. MJA and Mayo Clinic have an equity/royalty relationship with AliveCor, Blue Ox Health, and StemoniX but without remuneration thus far. However, none of these entities have contributed to this study in any manner. CK, DJT, DY, HVS, JJM, JMB, RN, SH, and WZ have no conflicts of interest to disclose.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed Consent
Informed consent was obtained from all individual participants included in the study. All experimental protocols for this study were approved by the Mayo Foundation Institutional Review Board and informed consent was obtained for use of patient samples.
Additional information
Associate Editor Joost Sluijter oversaw the review of this article
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 328 kb)
Rights and permissions
About this article
Cite this article
Zhou, W., Bos, J.M., Ye, D. et al. Induced Pluripotent Stem Cell–Derived Cardiomyocytes from a Patient with MYL2-R58Q-Mediated Apical Hypertrophic Cardiomyopathy Show Hypertrophy, Myofibrillar Disarray, and Calcium Perturbations. J. of Cardiovasc. Trans. Res. 12, 394–403 (2019). https://doi.org/10.1007/s12265-019-09873-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-019-09873-6