Abstract
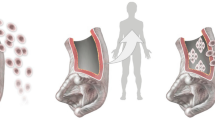
Cryopreserved allogeneic conduits are the elective biocompatible choice among currently available substitutes for surgical replacement in end-stage valvulopathy. However, degeneration occurs in 15 years in adults or faster in children, due to recipient’s immunological reactions to donor’s antigens. Here, human aortic valves were decellularized by TRICOL, based on Triton X-100 and sodium cholate, and submitted to standard cryopreservation (TRICOL-human aortic valves (hAVs)). Tissue samples were analyzed to study the effects of the combined procedure on original valve architecture and donor’s cell removal. Residual amounts of nucleic acids, pathological microorganisms, and detergents were also investigated. TRICOL-hAVs proved to be efficaciously decellularized with removal of donor’s cell components and preservation of valve scaffolding. Trivial traces of detergents, no cytotoxicity, and abrogated bioburden were documented. TRICOL-hAVs may represent off-the-shelf alternatives for both aortic and pulmonary valve replacements in pediatric and grown-up with congenital heart disease patients.






Similar content being viewed by others
Abbreviations
- TRICOL:
-
Decellularization methodology (osmotic shock, detergents (Triton X-100 and sodium cholate), and aspecific nucleases)
- hAV:
-
Human aortic valve
- HLA:
-
Human leukocyte antigen
- GUCH:
-
Grown-up with congenital heart disease
- CVA:
-
Human cryopreserved valve allograft
- SDS:
-
Sodium dodecyl sulfate
- ECM:
-
Extracellular matrix
- NHB:
-
Non-heart-beating
- HPLC:
-
High-performance liquid chromatography
- MS:
-
Mass spectrometry
References
Donovan, T. J., Hufnagel, C. A., & Eastcott, H. H. (1992). Techniques of endocardial anastomosis for circumventing the pulmonic valve. J Thoracic Surg, 23(4), 348–359.
Sidhu, P., O’Kane, H., Ali, N., Gladstone, D. J., Sarsam, M. A., Campalani, G., & MacGowan, S. W. (2001). Mechanical or bioprosthetic valves in the elderly: a 20-year comparison. The Annals of Thoracic Surgery, 71(5 Suppl), S257–S260. doi:10.1016/s0003-4975(01)02522-x.
Yuan, S. M., Mishaly, D., Shinfeld, A., & Raanani, E. (2008). Right ventricular outflow tract reconstruction: valved conduit of choice and clinical outcomes. Journal of Cardiovascular Medicine (Hagerstown, Md.), 9, 327–337. doi:10.2459/JCM.0b013e32821626ce.
Simon, P., Kasimir, M. T., Seebacher, G., Weigel, G., Ullrich, R., Salzer-Muhar, U., Rieder, E., & Wolner, E. (2003). Early failure of the tissue engineered porcine heart valve SYNERGRAFT in pediatric patients. European Journal of Cardio-Thoracic Surgery, 23, 1002–1006 discussion 1006. doi:10.1016/S1010-7940(03)00094-0.
Schoen, F. J., & Levy, R. J. (2005). Calcification of tissue heart valve substitutes: progress toward understanding and prevention. The Annals of Thoracic Surgery, 79, 1072–1080. doi:10.1016/j.athoracsur.2004.06.033.
Naso, F., Gandaglia, A., Bottio, T., Tarzia, V., Nottle, M. B., d’Apice, A. J., Cowan, P. J., Cozzi, E., Galli, C., Lagutina, I., Lazzari, G., Iop, L., Spina, M., & Gerosa, G. (2013). First quantification of alpha-gal epitope in current glutaraldehyde-fixed heart valve bioprostheses. Xenotransplantation, 20, 252–256. doi:10.1111/xen.12044.
Manji, R. A., Zhu, L. F., Nijjar, N. K., Rayner, D. C., Korbutt, G. S., Churchill, T. A., Rajotte, R. V., Koshal, A., & Ross, D. B. (2006). Glutaraldehyde-fixed bioprosthetic heart valve conduits calcify and fail from xenograft rejection. Circulation, 114, 318–327. doi:10.1161/CIRCULATIONAHA.105.549311.
O’Brien, M., Stafford, E., Gardner, M., Pohlner, P., & McGiffin, D. (1987). A comparison of aortic valve replacement with viable cryopreserved and fresh allograft valves with a note on chromosomal studies. The Journal of Thoracic and Cardiovascular Surgery, 94, 812–823.
O’Brien, M. F., McGiffin, D. C., Stafford, E. G., et al. (1991). Allograft aortic valve replacement: long-term comparative clinical analysis of the viable cryopreserved and antibiotic 4 °C stored valves. J Cardiac Surg, 6(Suppl), 534–543.
Zhao, X. M., Green, M., Frazer, I. H., Hogan, P., & O’Brien, M. F. (1994). Donor-specific immune response after aortic valve allografting in the rat. Ann Thoracic Surg, 57(5), 1158–1163. doi:10.1016/0003-4975(94)91347-1.
Cochran, R. P., & Kunzelman, K. S. (1989). Cryopreservation does not alter antigenic expression of aortic allografts. The Journal of Surgical Research, 46(6), 597–599. doi:10.1016/0022-4804(89)90027-9.
Smith, J. D., Ogino, H., Hunt, D., Laylor, R. M., Rose, M. L., & Yacoub, M. H. (1995). Humoral immune response to human aortic valve homografts. The Annals of Thoracic Surgery, 60(2 Suppl), S127–S130. doi:10.1016/0003-4975(95)00275-p.
Shaddy, R. E., Hunter, D. D., Osborne, K. A., Lambert, L. M., Minich, L. L., Hawkins, J. A., McGough, E. C., & Fuller, T. C. (1996). Prospective analysis of HLA immunogenicity of cryopreserved valved allografts used in pediatric heart surgery. Circulation, 94, 1063–1067. doi:10.1161/01.CIR.94.5.1063.
Smith, J. D., Hornick, P. I., Rasmi, N., Rose, M. L., & Yacoub, M. H. (1998). Effect of HLA mismatching and antibody status on “homovital” aortic valve homograft performance. The Annals of Thoracic Surgery, 66, S212–S215. doi:10.1016/s0003-4975(98)01115-1.
Hoekstra, F., Knoop, C., Vaessen, L., Wassenaar, C., Jutte, N., Bos, E., & Weimar, W. (1996). Donor-specific cellular immune response against human cardiac valve allografts. The Journal of Thoracic and Cardiovascular Surgery, 112, 281–286. doi:10.1016/S0022-5223(96)70250-7.
Hoekstra, F., Witvliet, M., Knoop, C., Akkersdijk, G., Jutte, N., Bogers, A., Claas, F., & Weimar, W. (1997). Donor-specific anti-human leukocyte antigen class I antibodies after implantation of cardiac valve allografts. The Journal of Heart and Lung Transplantation, 16, 570–572.
Hoekstra, F. M., Witvliet, M., Knoop, C. Y., Wassenaar, C., Bogers, A. J., Weimar, W., & Claas, F. H. (1998). Immunogenic human leukocyte antigen class II antigens on human cardiac valves induce specific alloantibodies. The Annals of Thoracic Surgery, 66, 2022–2026. doi:10.1016/s0003-4975(98)01058-3.
Lund, O., Chandrasekaran, V., Grocott-Mason, R., Elwidaa, H., Mazhar, R., Khaghani, A., Mitchell, A., Ilsley, C., & Yacoub, M. H. (1999). Primary aortic valve replacement with allografts over twenty-five years: valve-related and procedure-related determinants of outcome. The Journal of Thoracic and Cardiovascular Surgery, 117, 77–90. doi:10.1016/s0022-5223(99)70471-x.
Vogt, P. R., Stallmach, T., Niederhäuser, U., Schneider, J., Zünd, G., Lachat, M., Künzli, A., & Turina, M. I. (2000). Explanted cryopreserved allografts: a morphological and immunohistochemical comparison between arterial allografts and allograft heart valves from infants and adults. European Journal of Cardio-Thoracic Surgery, 15, 639–644 discussion 644-655. doi:10.1016/S1010-7940(99)00053-6.
Dignan, R., O’Brien, M., Hogan, P., et al. (2000). Influence of HLA matching and associated factors on aortic valve homograft function. The Journal of Heart Valve Disease, 9(4), 504–511.
Hawkins, J. A., Breinholt, J. P., Lambert, L. M., Fuller, T. C., Profaizer, T., McGough, E. C., & Shaddy, R. E. (2000). Class I and class II anti-HLA antibodies after implantation of cryopreserved allograft material in pediatric patients. The Journal of Thoracic and Cardiovascular Surgery, 119, 324–330. doi:10.1016/S0022-5223(00)70188-7.
Kannemeier, C., Shibamiya, A., Nakazawa, F., Trusheim, H., Ruppert, C., Markart, P., Song, Y., Tzima, E., Kennerknecht, E., Niepmann, M., von Bruehl, M. L., Sedding, D., Massberg, S., Günther, A., Engelmann, B., & Preissner, K. T. (2007). Extracellular RNA constitutes a natural procoagulant cofactor in blood coagulation. Proceedings of the National Academy of Sciences of the United States of America, 104, 6388–6393. doi:10.1073/pnas.0608647104.
Fischer, S., Grantzow, T., Pagel, J. I., Tschernatsch, M., Sperandio, M., Preissner, K. T., & Deindl, E. (2012). Extracellular RNA promotes leukocyte recruitment in the vascular system by mobilizing pro-inflammatory cytokines. Thrombosis and Haemostasis, 108, 730–741. doi:10.1160/TH12-03-0186.
Cao, H., Ye, H., Sun, Z., Shen, X., Song, Z., Wu, X., He, W., Dai, C., Yang, J., et al. (2014). Circulatory mitochondrial DNA is a pro-inflammatory agent in maintenance hemodialysis patients. PloS One, 9, e113179. doi:10.1371/journal.pone.0113179.
Cebotari, S., Mertsching, H., Kallenbach, K., Kostin, S., Repin, O., Batrinac, A., Kleczka, C., Ciubotaru, A., & Haverich, A. (2002). Construction of autologous human heart valves based on an acellular allograft matrix. Circulation, 106, I63–I68. doi:10.1161/01.cir.0000032900.55215.85.
Bando, K., Danielson, G. K., Schaff, H. V., Mair, D. D., Julsrud, P. R., & Puga, F. J. (1995). Outcome of pulmonary and aortic homografts for right ventricular outflow tract reconstruction. The Journal of Thoracic and Cardiovascular Surgery, 109(3), 509–517. doi:10.1016/S0022-5223(95)70282-2.
Heng, W. L., Albrecht, H., Chiappini, P., Lim, Y. P., & Manning, L. (2013). International Heart Valve Bank Survey: a review of processing practices and activity outcomes. J Transplant, 2013, 163150. doi:10.1155/2013/163150.
Samouillan, V., Dandurand-Lods, J., Lamure, A., Maurel, E., Lacabanne, C., Gerosa, G., Venturini, A., Casarotto, D., Gherardini, L., & Spina, M. (1999). Thermal analysis characterization of aortic tissues for cardiac valve bioprostheses. Journal of Biomedical Materials Research, 46, 531–538. doi:10.1002/(SICI)1097-4636(19990915)46:4<531::AID-JBM11>3.0.CO;2-2.
Bertipaglia, B., Ortolani, F., Petrelli, L., Gerosa, G., Spina, M., Pauletto, P., Casarotto, D., Marchini, M., & Sartore, S. (2003). Cell characterization of porcine aortic valve and decellularized leaflets repopulated with aortic valve interstitial cells: the VESALIO Project (Vitalitate Exornatum Succedaneum Aorticum Labore Ingenioso Obtenibitur). The Annals of Thoracic Surgery, 75, 1274–1282. doi:10.1016/s0003-4975(02)04706-9.
Iop, L., Renier, V., Naso, F., Piccoli, M., Bonetti, A., Gandaglia, A., Pozzobon, M., Paolin, A., Ortolani, F., Marchini, M., Spina, M., De Coppi, P., Sartore, S., & Gerosa, G. (2009). The influence of heart valve leaflet matrix characteristics on the interaction between human mesenchymal stem cells and decellularized scaffolds. Biomaterials, 30, 4104–4116. doi:10.1016/j.biomaterials.2009.04.031.
Gallo, M., Naso, F., Poser, H., Rossi, A., Franci, P., Bianco, R., Micciolo, M., Zanella, F., Cucchini, U., Aresu, L., Buratto, E., Busetto, R., Spina, M., Gandaglia, A., & Gerosa, G. (2012). Physiological performance of a detergent decellularized heart valve implanted for 15 months in Vietnamese pigs: surgical procedure, follow-up, and explant inspection. Artificial Organs, 36, E138–E150. doi:10.1111/j.1525-1594.2012.01447.x.
Iop, L., Bonetti, A., Naso, F., Rizzo, S., Cagnin, S., Bianco, R., Dal Lin, C., Martini, P., Poser, H., Franci, P., Lanfranchi, G., Busetto, R., Spina, M., Basso, C., Marchini, M., Gandaglia, A., Ortolani, F., & Gerosa, G. (2014). Decellularized allogeneic heart valves demonstrate self-regeneration potential after a long-term preclinical evaluation. PloS One, 9, e99593. doi:10.1371/journal.pone.0099593.
Iop, L., & Gerosa, G. (2015). Guided tissue regeneration in heart valve replacement: from preclinical research to first-in-human trials. BioMed Research International doi. doi:10.1155/2015/432901.
Elkins, R. C., Dawson, P. E., Goldstein, S., Walsh, S. P., & Black, S. (2001). Decellularized human valve allografts. The Annals of Thoracic Surgery, 7, S428–S432. doi:10.1016/s0003-4975(01)02503-6.
Helder MR, Kouchoukos ND, Zehr K, Dearani JA, Maleszewski JJ, Leduc C, Heins CN, Schaff HV (2016) Late durability of decellularized allografts for aortic valve replacement: a word of caution. J Thorac Cardiovasc Surg. pii: S0022–5223(16)30024–1 doi: 10.1016/j.jtcvs.2016.03.050
Sarikouch S, Horke A, Tudorache I, Beerbaum P, Westhoff-Bleck M, Boethig D, Repind O, Maniucd L, Ciubotaru A, Haverich A, Cebotari S (2016) Decellularized fresh homografts for pulmonary valve replacement: a decade of clinical experience. Eur J Cardiothorac Surg, pii: ezw050 doi: 0.1093/ejcts/ezw050
Tudorache, I., Horke, A., Cebotari, S., Sarikouch, S., Boethig, D., Breymann, T., Beerbaum, P., Bertram, H., Westhoff-Bleck, M., Theodoridis, K., Bobylev, D., Cheptanaru, E., Ciubotaru, A., & Haverich, A. (2016). Decellularized aortic homografts for aortic valve and aorta ascendens replacement. European Journal of Cardio-Thoracic Surgery, 50, 89–97. doi:10.1093/ejcts/ezw013.
Kasimir, M. T., Rieder, E., Seebacher, G., Silberhumer, G., Wolner, E., Weigel, G., & Simon, P. (2003). Comparison of different decellularization procedures of porcine heart valves. The International Journal of Artificial Organs, 26, 421–427. doi:10.5301/IJAO.2008.3028.
Cigliano, A., Gandaglia, A., Lepedda, A. J., Zinellu, E., Naso, F., Gastaldello, A., Aguiari, P., De Muro, P., Gerosa, G., Spina, M., & Formato, M. (2012). Fine structure of glycosaminoglycans from fresh and decellularized porcine cardiac valves and pericardium. Biochem Res Int, 979351. doi:10.1155/2012/979351.
Caamaño, S., Shiori, A., Strauss, S. H., & Orton, E. C. (2009). Does sodium dodecyl sulfate wash out of detergent-treated bovine pericardium at cytotoxic concentrations? The Journal of Heart Valve Disease, 18(1), 101–105.
Cebotari, S., Tudorache, I., Jaekel, T., Hilfiker, A., Dorfman, S., Ternes, W., Haverich, A., & Lichtenberg, A. (2010). Detergent decellularization of heart valves for tissue engineering: toxicological effects of residual detergents on human endothelial cells. Artificial Organs, 34, 206–210. doi:10.1111/j.1525-1594.2009.00796.x.
McNeel, K. E., Das, S., Siraj, N., Negulescu, I. I., & Warner, I. M. (2015). Sodium deoxycholate hydrogels: effects of modifications on gelation, drug release, and nanotemplating. The Journal of Physical Chemistry. B, 119, 8651–8659. doi:10.1021/acs.jpcb.5b00411.
Kawazoye, S., Tian, S. F., Toda, S., Takashima, T., Sunaga, T., Fujitani, N., Higashino, H., & Matsumura, S. (1995 Jun). The mechanism of interaction of sodium dodecyl sulfate with elastic fibers. Journal of Biochemistry, 117(6), 1254–1260.
Spina M, Naso F, Zancan I, Iop L, Dettin M, Gerosa G (2014) Biocompatibility issues of next generation decellularized bioprosthetic devices. Conference papers in science. Article ID 869240 doi: 10.1155/2014/86924
Acknowledgements
This study was realized with the financial support of CARIPARO Foundation (Veneto) under the Padova Heart Project grant.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Human/Animal Subjects
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (TRICOL registry, 3291/AO/14, Padua University Hospital and National Transplantation Centre) and with the Helsinki Declaration of 1975, as revised in 2000. This article does not contain any animal study performed by any of the authors.
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Associate Editor Adrian Chester oversaw the review of this article
Laura Iop and Adolfo Paolin equally contributed to the study.
Rights and permissions
About this article
Cite this article
Iop, L., Paolin, A., Aguiari, P. et al. Decellularized Cryopreserved Allografts as Off-the-Shelf Allogeneic Alternative for Heart Valve Replacement: In Vitro Assessment Before Clinical Translation. J. of Cardiovasc. Trans. Res. 10, 93–103 (2017). https://doi.org/10.1007/s12265-017-9738-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-017-9738-0