Abstract
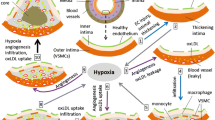
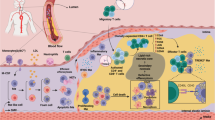
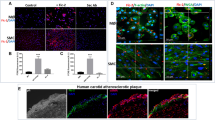
Neovascularization has been linked to the progression and vulnerability of atherosclerotic lesions. Angiogenesis is increased in lipid-rich plaque. Hypoxia-inducible factor alpha (HIF-1α) is a key transcriptional regulator responding to hypoxia and activating genes, which promote angiogenesis, among them vascular endothelial growth factor (VEGF). Oxidized low-density lipoprotein (oxLDL) is generated in lipid-rich plaque by oxidative stress. It triggers an inflammatory response and was traditionally thought to inhibit endothelial cells. New data, however, suggest that oxLDL can activate HIF-1α in monocytes in a hypoxia-independent fashion. We hypothesized that HIF-1α activation in monocyte–macrophages could transmit proangiogenic effects of oxLDL linking hyperlipidemia, inflammation, and angiogenesis in atherosclerosis. First, we examined the effect of oxLDL on HIF-1α and VEGF expression in monocyte–macrophages and on their proangiogenic effect on endothelial cells in vitro in a monocyte–macrophage/endothelial co-culture model. OxLDL strongly induced HIF-1α and VEGF in monocyte–macrophages and significantly increased tube formation in co-cultured endothelial cells. HIF-1α inhibition reversed this effect. Second, we demonstrated a direct proangiogenic effect of oxLDL in an in vivo angiogenesis assay. Again, HIF-1α inhibition abrogated the proangiogenic effect of oxLDL. Third, in a rabbit atherosclerosis model, we studied the effect of dietary lipid lowering on arterial HIF-1α and VEGF expression. The administration of low-lipid diet significantly reduced the expression of both HIF-1α and VEGF, resulting in decreased plaque neovascularization. Our data point to oxLDL as a proangiogenic agent linking hyperlipidemia, inflammation, and angiogenesis in atherosclerosis. This effect is dependent on macrophages and, at least in part, on the induction of the HIF-1α pathway.




Similar content being viewed by others
References
Burke, A. P., Farb, A., Malcom, G. T., Liang, Y. H., Smialek, J., & Virmani, R. (1997). Coronary risk factors and plaque morphology in men with coronary disease who died suddenly. The New England Journal of Medicine, 336(18), 1276–1282. doi:10.1056/NEJM199705013361802.
Michel, J. B., Virmani, R., Arbustini, E., & Pasterkamp, G. (2011). Intraplaque haemorrhages as the trigger of plaque vulnerability. European Heart Journal, 32(16), 1977–1985. doi:10.1093/eurheartj/ehr054. 1985a, 1985b, 1985c.
Moreno, P. R., Purushothaman, K. R., Sirol, M., Levy, A. P., & Fuster, V. (2006). Neovascularization in human atherosclerosis. Circulation, 113(18), 2245–2252. doi:10.1161/CIRCULATIONAHA.105.578955.
Moreno, P. R., Sanz, J., & Fuster, V. (2009). Promoting mechanisms of vascular health: circulating progenitor cells, angiogenesis, and reverse cholesterol transport. Journal of the American College of Cardiology, 53(25), 2315–2323. doi:10.1016/j.jacc.2009.02.057.
Moulton, K. S., Vakili, K., Zurakowski, D., Soliman, M., Butterfield, C., Sylvin, E., et al. (2003). Inhibition of plaque neovascularization reduces macrophage accumulation and progression of advanced atherosclerosis. Proceedings of the National Academy of Sciences of the United States of America, 100(8), 4736–4741. doi:10.1073/pnas.0730843100.
Groszek, E., & Grundy, S. M. (1980). The possible role of the arterial microcirculation in the pathogenesis of atherosclerosis. Journal of Chronic Diseases, 33(11–12), 679–684.
Hutter, R., Valdiviezo, C., Sauter, B. V., Savontaus, M., Chereshnev, I., Carrick, F. E., et al. (2004). Caspase-3 and tissue factor expression in lipid-rich plaque macrophages: evidence for apoptosis as link between inflammation and atherothrombosis. Circulation, 109(16), 2001–2008. doi:10.1161/01.CIR.0000125526.91945.AE.
Palinski, W., Rosenfeld, M. E., Yla-Herttuala, S., Gurtner, G. C., Socher, S. S., Butler, S. W., et al. (1989). Low density lipoprotein undergoes oxidative modification in vivo. Proceedings of the National Academy of Sciences of the United States of America, 86(4), 1372–1376.
Parthasarathy, S., Quinn, M. T., Schwenke, D. C., Carew, T. E., & Steinberg, D. (1989). Oxidative modification of beta-very low density lipoprotein. Potential role in monocyte recruitment and foam cell formation. Arteriosclerosis, 9(3), 398–404.
Yla-Herttuala, S., Palinski, W., Rosenfeld, M. E., Parthasarathy, S., Carew, T. E., Butler, S., et al. (1989). Evidence for the presence of oxidatively modified low density lipoprotein in atherosclerotic lesions of rabbit and man. The Journal of Clinical Investigation, 84(4), 1086–1095. doi:10.1172/JCI114271.
Vink, A., Schoneveld, A. H., Lamers, D., Houben, A. J., van der Groep, P., van Diest, P. J., et al. (2007). HIF-1 alpha expression is associated with an atheromatous inflammatory plaque phenotype and upregulated in activated macrophages. Atherosclerosis, 195(2), e69–75. doi:10.1016/j.atherosclerosis.2007.05.026.
Sluimer, J. C., Gasc, J. M., van Wanroij, J. L., Kisters, N., Groeneweg, M., Sollewijn Gelpke, M. D., et al. (2008). Hypoxia, hypoxia-inducible transcription factor, and macrophages in human atherosclerotic plaques are correlated with intraplaque angiogenesis. Journal of the American College of Cardiology, 51(13), 1258–1265. doi:10.1016/j.jacc.2007.12.025.
Kai, H., Kuwahara, F., Tokuda, K., Shibata, R., Kusaba, K., Niiyama, H., et al. (2002). Coexistence of hypercholesterolemia and hypertension impairs adventitial vascularization. Hypertension, 39(2 Pt 2), 455–459.
Karshovska, E., Zernecke, A., Sevilmis, G., Millet, A., Hristov, M., Cohen, C. D., et al. (2007). Expression of HIF-1alpha in injured arteries controls SDF-1alpha mediated neointima formation in apolipoprotein E deficient mice. Arteriosclerosis, Thrombosis, and Vascular Biology, 27(12), 2540–2547. doi:10.1161/ATVBAHA.107.151050.
Higashida, T., Kanno, H., Nakano, M., Funakoshi, K., & Yamamoto, I. (2008). Expression of hypoxia-inducible angiogenic proteins (hypoxia-inducible factor-1alpha, vascular endothelial growth factor, and E26 transformation-specific-1) and plaque hemorrhage in human carotid atherosclerosis. Journal of Neurosurgery, 109(1), 83–91. doi:10.3171/JNS/2008/109/7/0083.
Mayr, M., Sidibe, A., & Zampetaki, A. (2008). The paradox of hypoxic and oxidative stress in atherosclerosis. Journal of the American College of Cardiology, 51(13), 1266–1267. doi:10.1016/j.jacc.2008.01.005.
Bosco, M. C., Puppo, M., Blengio, F., Fraone, T., Cappello, P., Giovarelli, M., et al. (2008). Monocytes and dendritic cells in a hypoxic environment: spotlights on chemotaxis and migration. Immunobiology, 213(9–10), 733–749. doi:10.1016/j.imbio.2008.07.031.
Deguchi, J. O., Yamazaki, H., Aikawa, E., & Aikawa, M. (2009). Chronic hypoxia activates the Akt and beta-catenin pathways in human macrophages. Arteriosclerosis, Thrombosis, and Vascular Biology, 29(10), 1664–1670. doi:10.1161/ATVBAHA.109.194043.
Elbarghati, L., Murdoch, C., & Lewis, C. E. (2008). Effects of hypoxia on transcription factor expression in human monocytes and macrophages. Immunobiology, 213(9–10), 899–908. doi:10.1016/j.imbio.2008.07.016.
Poitz, D. M., Augstein, A., Weinert, S., Braun-Dullaeus, R. C., Strasser, R. H., & Schmeisser, A. (2011). OxLDL and macrophage survival: essential and oxygen-independent involvement of the Hif-pathway. Basic Research in Cardiology, 106(5), 761–772. doi:10.1007/s00395-011-0186-8.
Ribatti, D., Levi-Schaffer, F., & Kovanen, P. T. (2008). Inflammatory angiogenesis in atherogenesis—a double-edged sword. Annals of Medicine, 40(8), 606–621. doi:10.1080/07853890802186913.
West, X. Z., Malinin, N. L., Merkulova, A. A., Tischenko, M., Kerr, B. A., Borden, E. C., et al. (2010). Oxidative stress induces angiogenesis by activating TLR2 with novel endogenous ligands. Nature, 467(7318), 972–976. doi:10.1038/nature09421.
Yu, S., Wong, S. L., Lau, C. W., Huang, Y., & Yu, C. M. (2011). Oxidized LDL at low concentration promotes in-vitro angiogenesis and activates nitric oxide synthase through PI3K/Akt/eNOS pathway in human coronary artery endothelial cells. Biochemical and Biophysical Research Communications, 407(1), 44–48. doi:10.1016/j.bbrc.2011.02.096.
Shatrov, V. A., Sumbayev, V. V., Zhou, J., & Brune, B. (2003). Oxidized low-density lipoprotein (oxLDL) triggers hypoxia-inducible factor-1alpha (HIF-1alpha) accumulation via redox-dependent mechanisms. Blood, 101(12), 4847–4849. doi:10.1182/blood-2002-09-2711.
Kessler J, Hahnel A, Wichmann H, Rot S, Kappler M, Bache M, Vordermark D (2010) HIF-1alpha inhibition by siRNA or chetomin in human malignant glioma cells: effects on hypoxic radioresistance and monitoring via CA9 expression. BMC cancer 10:605. doi:10.1186/1471-2407-10-605
Bouvard, C., De Arcangelis, A., Dizier, B., Galy-Fauroux, I., Fischer, A. M., Georges-Labouesse, E., et al. (2012). Tie2-dependent knockout of alpha6 integrin subunit in mice reduces post-ischaemic angiogenesis. Cardiovascular Research. doi:10.1093/cvr/cvs153.
Corti, R., Osende, J. I., Fallon, J. T., Fuster, V., Mizsei, G., Jneid, H., et al. (2004). The selective peroxisomal proliferator-activated receptor-gamma agonist has an additive effect on plaque regression in combination with simvastatin in experimental atherosclerosis: in vivo study by high-resolution magnetic resonance imaging. Journal of the American College of Cardiology, 43(3), 464–473. doi:10.1016/j.jacc.2003.08.048.
Giannarelli, C., Cimmino, G., Connolly, T. M., Ibanez, B., Ruiz, J. M., Alique, M., et al. (2012). Synergistic effect of liver X receptor activation and simvastatin on plaque regression and stabilization: an magnetic resonance imaging study in a model of advanced atherosclerosis. European Heart Journal, 33(2), 264–273. doi:10.1093/eurheartj/ehr136.
Lewis, C., & Murdoch, C. (2005). Macrophage responses to hypoxia: implications for tumor progression and anti-cancer therapies. The American Journal of Pathology, 167(3), 627–635. doi:10.1016/S0002-9440(10)62038-X.
Chavakis, E., Dernbach, E., Hermann, C., Mondorf, U. F., Zeiher, A. M., & Dimmeler, S. (2001). Oxidized LDL inhibits vascular endothelial growth factor-induced endothelial cell migration by an inhibitory effect on the Akt/endothelial nitric oxide synthase pathway. Circulation, 103(16), 2102–2107.
Wu, Y., Wang, Q., Cheng, L., Wang, J., & Lu, G. (2009). Effect of oxidized low-density lipoprotein on survival and function of endothelial progenitor cell mediated by p38 signal pathway. Journal of Cardiovascular Pharmacology, 53(2), 151–156. doi:10.1097/FJC.0b013e318197c637.
Haddad, P., Dussault, S., Groleau, J., Turgeon, J., Maingrette, F., & Rivard, A. (2011). Nox2-derived reactive oxygen species contribute to hypercholesterolemia-induced inhibition of neovascularization: effects on endothelial progenitor cells and mature endothelial cells. Atherosclerosis, 217(2), 340–349. doi:10.1016/j.atherosclerosis.2011.03.038.
Squadrito, M. L., & De Palma, M. (2011). Macrophage regulation of tumor angiogenesis: implications for cancer therapy. Molecular Aspects of Medicine, 32(2), 123–145. doi:10.1016/j.mam.2011.04.005.
Casazza, A., Fu, X., Johansson, I., Capparuccia, L., Andersson, F., Giustacchini, A., et al. (2011). Systemic and targeted delivery of semaphorin 3A inhibits tumor angiogenesis and progression in mouse tumor models. Arteriosclerosis, Thrombosis, and Vascular Biology, 31(4), 741–749. doi:10.1161/ATVBAHA.110.211920.
Baer, C., Squadrito, M. L., Iruela-Arispe, M. L., & De Palma, M. (2013). Reciprocal interactions between endothelial cells and macrophages in angiogenic vascular niches. Experimental Cell Research. doi:10.1016/j.yexcr.2013.03.026.
Khaidakov, M., Mitra, S., Wang, X., Ding, Z., Bora, N., Lyzogubov, V., et al. (2012). Large impact of low concentration oxidized LDL on angiogenic potential of human endothelial cells: a microarray study. PloS One, 7(10), e47421. doi:10.1371/journal.pone.0047421.
Norrby, K. (2006). In vivo models of angiogenesis. Journal of Cellular and Molecular Medicine, 10(3), 588–612.
Jeanpierre, E., Le Tourneau, T., Six, I., Zawadzki, C., Van Belle, E., Ezekowitz, M. D., et al. (2003). Dietary lipid lowering modifies plaque phenotype in rabbit atheroma after angioplasty: a potential role of tissue factor. Circulation, 108(14), 1740–1745. doi:10.1161/01.CIR.0000089370.84709.51.
Srimahachota, S., Wunsuwan, R., Siritantikorn, A., Boonla, C., Chaiwongkarjohn, S., & Tosukhowong, P. (2010). Effects of lifestyle modification on oxidized LDL, reactive oxygen species production and endothelial cell viability in patients with coronary artery disease. Clinical Biochemistry, 43(10–11), 858–862. doi:10.1016/j.clinbiochem.2010.04.056.
Tonstad, S., Sundfor, T., & Seljeflot, I. (2005). Effect of lifestyle changes on atherogenic lipids and endothelial cell adhesion molecules in young adults with familial premature coronary heart disease. The American Journal of Cardiology, 95(10), 1187–1191. doi:10.1016/j.amjcard.2005.01.047.
Verhamme, P., Quarck, R., Hao, H., Knaapen, M., Dymarkowski, S., Bernar, H., et al. (2002). Dietary cholesterol withdrawal reduces vascular inflammation and induces coronary plaque stabilization in miniature pigs. Cardiovascular Research, 56(1), 135–144.
Inoue, T., Hayashi, M., Takayanagi, K., & Morooka, S. (2002). Lipid-lowering therapy with fluvastatin inhibits oxidative modification of low density lipoprotein and improves vascular endothelial function in hypercholesterolemic patients. Atherosclerosis, 160(2), 369–376.
Inoue, T., Yaguchi, I., Uchida, T., Kamishirado, H., Nakahara, S., Hayashi, T., et al. (2002). Clinical significance of the antibody against oxidized low-density lipoprotein in acute myocardial infarction. Cardiology, 98(1–2), 13–17.
Shimada, K., Mokuno, H., Matsunaga, E., Miyazaki, T., Sumiyoshi, K., Kume, A., et al. (2004). Predictive value of circulating oxidized LDL for cardiac events in type 2 diabetic patients with coronary artery disease. Diabetes Care, 27(3), 843–844.
Shimada, K., Mokuno, H., Matsunaga, E., Miyazaki, T., Sumiyoshi, K., Miyauchi, K., et al. (2004). Circulating oxidized low-density lipoprotein is an independent predictor for cardiac event in patients with coronary artery disease. Atherosclerosis, 174(2), 343–347. doi:10.1016/j.atherosclerosis.2004.01.029.
Acknowledgments
We thank Renata Hutter for her continued support.
Funding
This study was supported by NIH-Training Grant 5 T32 HL 7824-13 to Randolph Hutter.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hutter, R., Speidl, W.S., Valdiviezo, C. et al. Macrophages Transmit Potent Proangiogenic Effects of oxLDL In Vitro and In Vivo Involving HIF-1α Activation: a Novel Aspect of Angiogenesis in Atherosclerosis. J. of Cardiovasc. Trans. Res. 6, 558–569 (2013). https://doi.org/10.1007/s12265-013-9469-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-013-9469-9