Abstract
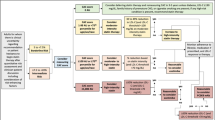
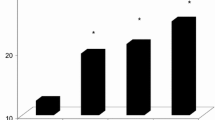
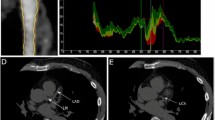
Subclinical atherosclerosis can be quantified by coronary artery calcium (CAC) scoring. Due to its high specificity for atherosclerosis, CAC is an excellent phenotypic tool for the evaluation of emerging risk markers. Lipoprotein(a) [Lp(a)] is atherogenic due to the presence of apoB and may be thrombogenic through its apo(a) component. Lp(a) has been linked to cardiovascular events in Caucasians; however, its link to atherosclerosis in various ethnicities remains unclear. We evaluated the ability of Lp(a) mass to predict subclinical atherosclerosis in Southeast Asians and Caucasians, as measured by CAC. Traditional lipid measurements, Lp(a) measurements, and CAC by 64-slice multidetector computed tomography was performed in 103 consecutive patients in the USA and in 104 consecutive patients in Jakarta, Indonesia. Proportion of positive CAC and median CAC in Southeast Asians and in Caucasians was 61.5% and 63.1%, and 23.5 (interquartile range, 0–270) and 13 (interquartile range, 0–388), respectively. Significantly higher proportion of Southeast Asians had elevated Lp(a) levels, compared to Caucasians (51.0% vs. 29.2%; p = 0.005). In Southeast Asians, Lp(a) remained an independent predictor of CAC with an odds ratio of 4.97 (95% confidence interval, 1.56–15.88; p < 0.0001), but not in Caucasians. Receiver operating characteristic analysis showed an improvement in area under the curve from 0.81 to 0.86 (p = 0.05) when including Lp(a) in the predictive model in Southeast Asians. This translated to 7% of Southeast Asians reclassified to correct CAC status. Lp(a) measurements may have a role in risk stratification of Southeast Asians. Ethnic variation should be taken into account when considering the use of Lp(a) measurements in risk assessment.

Similar content being viewed by others
References
Greenland, P., Bonow, R. O., Brundage, B. H., Budoff, M. J., Eisenberg, M. J., Grundy, S. M., et al. (2007). ACCF/AHA 2007 clinical expert consensus document on coronary artery calcium scoring by computed tomography in global cardiovascular risk assessment and in evaluation of patients with chest pain: a report of the American College of Cardiology Foundation Clinical Expert Consensus Task Force (ACCF/AHA Writing Committee to Update the 2000 Expert Consensus Document on Electron Beam Computed Tomography). Circulation, 115(3), 402–426.
Rumberger, J. A., Simons, D. B., Fitzpatrick, L. A., Sheedy, P. F., & Schwartz, R. S. (1995). Coronary artery calcium area by electron-beam computed tomography and coronary atherosclerotic plaque area. A histopathologic correlative study. Circulation, 92(8), 2157–2162.
Detrano, R., Guerci, A. D., Carr, J. J., Bild, D. E., Burke, G., Folsom, A. R., et al. (2008). Coronary calcium as a predictor of coronary events in four racial or ethnic groups. The New England Journal of Medicine, 358(13), 1336–1345.
Joshi, P. H., Krivitsky, E., Qian, Z., Vazquez, G., Voros, S., & Miller, J. (2010). Do we know when and how to lower lipoprotein(a)? Current Treatment Options in Cardiovascular Medicine, 12(4), 396–407.
Davidson, M. H. (2005). Reducing residual risk for patients on statin therapy: the potential role of combination therapy. The American Journal of Cardiology, 96(9A), 3K–13K.
Hancock, M. A., Boffa, M. B., Marcovina, S. M., Nesheim, M. E., & Koschinsky, M. L. (2003). Inhibition of plasminogen activation by lipoprotein(a). The Journal of Biological Chemistry, 278(26), 23260–23269.
Loscalzo, J., Weinfeld, M., Fless, G. M., & Scanu, A. M. (1990). Lipoprotein(a), fibrin binding, and plasminogen activation. Arteriosclerosis, Thrombosis, and Vascular Biology, 10(2), 240–245.
Danesh, J., Collins, R., & Peto, R. (2000). Lipoprotein(a) and coronary heart disease: meta-analysis of prospective studies. Circulation, 102(10), 1082–1085.
Nordestgaard, B. G., Chapman, M. J., Ray, K., Boren, J., Andreotti, F., Watts, G. F., et al. (2010). Lipoprotein(a) as a cardiovascular risk factor: current status. European Heart Journal, 31(23), 2844–2853.
Guerra, R., Yu, Z., Marcovina, S., Peshock, R., Cohen, J. C., & Hobbs, H. H. (2005). Lipoprotein(a) and apolipoprotein(a) isoforms: no association with coronary artery calcification in the Dallas Heart Study. Circulation, 111(12), 1471–1479.
Kullo, I. J., Bailey, K. R., Bielak, L. F., Sheedy, P. F., Klee, G. G., Kardia, S. L., et al. (2004). Lack of association between lipoprotein(a) and coronary artery calcification in the Genetic Epidemiology Network of Arteriopathy (GENOA) study. Mayo Clinic Proceedings, 79(10), 1258–1263.
Shen, C., Bao, J., Chen, X., & Ma, G. (2010). Serum lipoprotein (a) is positively correlated with coronary artery calcification in low risk Chinese patients. Heart, 96(Suppl 3), A107–A108.
Kraft, H. G., Lingenhel, A., Pang, R. W., Delport, R., Trommsdorff, M., Vermaak, H., et al. (1996). Frequency distributions of apolipoprotein(a) kringle IV repeat alleles and their effects on lipoprotein(a) levels in Caucasian, Asian, and African populations: the distribution of null alleles is non-random. European Journal of Human Genetics, 4(2), 74–87.
Mooser, V., Scheer, D., Marcovina, S. M., Wang, J., Guerra, R., Cohen, J., et al. (1997). The Apo(a) gene is the major determinant of variation in plasma Lp(a) levels in African Americans. American Journal of Human Genetics, 61(2), 402–417.
Agatston, A. S., Janowitz, W. R., Hildner, F. J., Zusmer, N. R., Viamonte, M., Jr., & Detrano, R. (1990). Quantification of coronary artery calcium using ultrafast computed tomography. Journal of the American College of Cardiology, 15(4), 827–832.
Erqou, S., Kaptoge, S., Perry, P. L., Di, A. E., Thompson, A., White, I. R., et al. (2009). Lipoprotein(a) concentration and the risk of coronary heart disease, stroke, and nonvascular mortality. JAMA, 302(4), 412–423.
Geethanjali, F. S., Luthra, K., Lingenhel, A., Kanagasaba-Pathy, A. S., Jacob, J., Srivastava, L. M., et al. (2003). Analysis of the apo(a) size polymorphism in Asian Indian populations: association with Lp(a) concentration and coronary heart disease. Atherosclerosis, 169(1), 121–130.
Marcovina, S. M., & Koschinsky, M. L. (2011). Lipoprotein(a):structure, measurement and clinical significance. In N. Rifai, G. R. Warnick, & M. H. Dominiczak (Eds.), Handbook of lipoprotein testing (2nd ed., pp. 345–368). Washington: AACC.
Marcovina, S. M., Albers, J. J., Wijsman, E., Zhang, Z., Chapman, N. H., & Kennedy, H. (1996). Differences in Lp[a] concentrations and apo[a] polymorphs between black and white Americans. Journal of Lipid Research, 37(12), 2569–2585.
Clarke, R., Peden, J. F., Hopewell, J. C., Kyriakou, T., Goel, A., Heath, S. C., et al. (2009). Genetic variants associated with Lp(a) lipoprotein level and coronary disease. The New England Journal of Medicine, 361(26), 2518–2528.
Niendorf, A., Rath, M., Wolf, K., Peters, S., Arps, H., Beisiegel, U., et al. (1990). Morphological detection and quantification of lipoprotein(a) deposition in atheromatous lesions of human aorta and coronary arteries. Virchows Archiv, 417(2), 105–111.
Dangas, G., Mehran, R., Harpel, P. C., Sharma, S. K., Marcovina, S. M., Dube, G., et al. (1998). Lipoprotein(a) and inflammation in human coronary atheroma: association with the severity of clinical presentation. Journal of the American College of Cardiology, 32(7), 2035–2042.
Ragab, M. S., Selvaraj, P., & Sgoutas, D. S. (1996). Oxidized lipoprotein (a) induces cell adhesion molecule Mac-1 (CD 11b) and enhances adhesion of the monocytic cell line U937 to cultured endothelial cells. Atherosclerosis, 123(1–2), 103–113.
Poon, M., Zhang, X., Dunsky, K. G., Taubman, M. B., & Harpel, P. C. (1997). Apolipoprotein(a) induces monocyte chemotactic activity in human vascular endothelial cells. Circulation, 96(8), 2514–2519.
Argraves, K. M., Kozarsky, K. F., Fallon, J. T., Harpel, P. C., & Strickland, D. K. (1997). The atherogenic lipoprotein Lp(a) is internalized and degraded in a process mediated by the VLDL receptor. Journal of Clinical Investigation, 100(9), 2170–2181.
Grainger, D. J., Kirschenlohr, H. L., Metcalfe, J. C., Weissberg, P. L., Wade, D. P., & Lawn, R. M. (1993). Proliferation of human smooth muscle cells promoted by lipoprotein(a). Science, 260(5114), 1655–1658.
Kojima, S., Harpel, P. C., & Rifkin, D. B. (1991). Lipoprotein (a) inhibits the generation of transforming growth factor beta: an endogenous inhibitor of smooth muscle cell migration. The Journal of Cell Biology, 113(6), 1439–1445.
Sugiyama, N., Marcovina, S., Gown, A. M., Seftel, H., Joffe, B., & Chait, A. (1992). Immunohistochemical distribution of lipoprotein epitopes in xanthomata from patients with familial hypercholesterolemia. The American Journal of Pathology, 141(1), 99–106.
Shai, I., Rimm, E. B., Hankinson, S. E., Cannuscio, C., Curhan, G., Manson, J. E., et al. (2005). Lipoprotein (a) and coronary heart disease among women: beyond a cholesterol carrier? European Heart Journal, 26(16), 1633–1639.
Rajasekhar, D., Srinivasa Rao, P. V., Latheef, S. A., Saibaba, K. S., & Subramanyam, G. (2004). Association of serum antioxidants and risk of coronary heart disease in South Indian population. Indian Journal of Medical Sciences, 58(11), 465–471.
Acknowledgments
Dr. Szilard Voros has received grant support from Siemens Medical Solutions in the past but not specifically for this study.
Author information
Authors and Affiliations
Corresponding author
Additional information
Statement of Ethical Standards and Compliance
The procedures followed were in accordance with the ethical standards of the responsible institutional committees and national laws on human experimentation of the United States of America and Indonesia (National Cardiovascular Center, Jakarta, Indonesia) and with the Helsinki Declaration of 1975, as revised in 2000.
Rights and permissions
About this article
Cite this article
Sharma, A., Kasim, M., Joshi, P.H. et al. Abnormal Lipoprotein(a) Levels Predict Coronary Artery Calcification in Southeast Asians but Not in Caucasians: Use of Noninvasive Imaging for Evaluation of an Emerging Risk Factor. J. of Cardiovasc. Trans. Res. 4, 470–476 (2011). https://doi.org/10.1007/s12265-011-9273-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-011-9273-3