Abstract
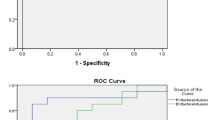
The objective of the study is to explore the use of internal jugular vein diameter, respiratory variability, and blood flow velocity in predicting blood volume of patients with intestinal obstruction. A total of sixty patients with acute intestinal obstruction who were admitted to our hospital from June 2019 to June 2021 were included and including 33 males and 27 females. The patients were graded ASA I to III on the basis of their physical condition. Using the random number table method, the patients were divided into the inferior vena cava (IVC) and internal jugular vein (IJV) groups. The maximum diameter (Dmax) and the minimum diameter (Dmin) of the IVC and IJV groups were measured by M-type ultrasound, and the respiratory variation index (RVI) was calculated. The maximum blood flow velocity (BVmax) and the minimum blood flow velocity (BVmin) of each vessel were also measured in the respective groups by Doppler ultrasound, and the blood flow variation index (BVI) was calculated. Each patient was then infused with 5 ml/kg crystalloid solution, and the above parameters were measured again and compared to the respective pre-infusion values. The correlation between each measurement index and CVP and their ability to predict CVP > 6 mmHg were statistically evaluated. The RVI of IVC decreased significantly post-infusion (P = 0.018). Compared to the pre-infusion values, the Dmin of IJV increased (P = 0.042), while the RVI and BVI decreased significantly after infusion (P = 0.004 and P = 0.047). The relevant measurement data could not be obtained for one patient in the IVC group due to obvious intestinal pneumatosis. There was a positive correlation between the Dmin of IVC and CVP (pre-infusion R = 0.684 and P = 0.000; post-infusion R = 0.442 and P = 0.016), and a negative correlation between RVI and CVP (pre-infusion R = − 0.826 and P = 0.000; post-infusion R = − 0.663 and P = 0.000) before and after infusion. In addition, CVP was positively correlated to the Dmin, BVmax, and BVmin of IJV before and after infusion (pre-infusion R = 0.652, 0.655, 0.795, and all P = 0.000; post-infusion R = 0.571, 0.586, 0.684, and P = 0.001, 0.001, and 0.000), and negatively with RVI and BVI (pre-infusion R = − 0.808, − 0.677, and all P = 0.000; post-infusion R = − 0.589, − 0.592, and all P = 0.001). The specificity of the Dmin of IVC was 92.9%, and the sensitivity of RVI was 100% prior to the infusion, the post-infusion RVI could predict the blood volume with 100% sensitivity. In contrast, all indices of IJV except Dmax predicted the blood volume before and after infusion. The area under the curve of RVI was the largest, indicating the highest predictive accuracy. The sensitivity and specificity of RVI were, respectively, 100 and 93.3% before infusion and 88.9 and 95.2% after infusion. The ultrasonically measured variability in the diameter and blood flow velocity of IJV can be used to predict the blood volume of patients with intestinal obstruction and has higher accuracy compared to the indices of IVC.

Similar content being viewed by others
Data Availability
The data that support the findings of this study are available from the corresponding author, Wang Wei, upon reasonable request.
References
Argueta E, Berdine G, Pena C, Nugent KM (2015) FloTrac® monitoring system: what are its uses in critically ill medical patients? Am J Med Sci 349(4):352–356
Hara M, Hiraki T (2020) Circulatory management using FloTrac/Vigileo and transesophageal echocardiography for mesenteric traction syndrome during colectomy in a patient with hypertrophic cardiomyopathy. J Cardiothorac Vasc Anesth 34(4):1015–1018
Kim KK, Krause M, Brandes IF, Khanna AK, Bartels K (2021) Transesophageal echocardiography for perioperative management in thoracic surgery. Curr Opin Anaesthesiol 34(1):7–12
Akoglu EU, Demir H, Ozturk TC, Ar AY, Turan G (2021) Respiratory variability of inferior vena cava at different mechanical ventilator settings. Am J Emerg Med 48:96–102
Vignon P (2004) Evaluation of fluid responsiveness in ventilated septic patients:back to venous return. Intensive Care Med 30:1699–1701
Tzadok B, Shapira S, Tal-Or E (2018) Ultrasound of jugular veins for assessment of acute dyspnea in emergency departments and for the assessment of acute heart failure. Isr Med Assoc J 20(5):308–310
Wang W, Liu Q, Lan Z, Wen X (2022) Correlation between ultrasound-measured diameter and blood flow velocity of the internal jugular veins with the preoperative blood volume in elderly patients. Indian J Surg. https://doi.org/10.1007/s12262-022-03418-z
Vather R, Bissett I (2013) Management of prolonged post-operative ileus: evidence-based recommendations. ANZ J Surg 83(5):319–324
Mohammed S, Syal R, Bhatia P, Chhabra S, Chouhan RS, Kamal M (2021) Prediction of post-induction hypotension in young adults using ultrasound-derived inferior vena cava parameters: an observational study. Indian J Anaesth 65(10):731–737
Gui J, Zhou B, Liu J, Ou B, Wang Y, Jiang L et al (2019) Impact of body characteristics on ultrasound-measured inferior vena cava parameters in Chinese children. Braz J Med Biol Res 52(10):e8122
Clemency BM, Bola A, Schlader ZJ, Hostler D, Lin H, St James E et al (2022) Ultrasonographic inferior vena cava measurement is more sensitive than vital sign abnormalities for identifying moderate and severe hemorrhage. J Emerg Med 62(1):64–71
Vignon P, Repessé X, Bégot E, Léger J, Jacob C, Bouferrache K et al (2017) Comparison of echocardiographic indices used to predict fluid responsiveness in ventilated patients. Am J Respir Crit Care Med 195(8):1022–1032
Haliloğlu M, Bilgili B, Kararmaz A, Cinel İ (2017) The value of internal jugular vein collapsibility index in sepsis. Ulus Travma Acil Cerrahi Derg 23(4):294–300
Henriot B, Scanff A, Sebillot M, Lautredoux F, Jego P (2021) Jugular vein ultrasound for estimating changes in blood volume: a new tool for all physicians. Intern Emerg Med 16(7):2005–2007
Perlas A, Chaparro LE, Chin KJ (2016) Lumbar neuraxial ultrasound for spinal and epidural anesthesia: a systematic review and metaanalysis. Reg Anesth Pain Med 41(2):251–260
Ekinci M, Alici HA, Ahiskalioglu A et al (2017) The use of ultrasound in planned cesarean delivery under spinal anesthesia for patients having nonprominent anatomic landmarks. J Clin Anesth 37:82–85
Meng T, Zhong Z, Meng L (2017) Impact of spinal anaesthesia vs. general anaesthesia on peri-operative outcome in lumbar spine surgery: a systematic review and meta-analysis of randomised, controlled trials. Anaesthesia 72(3):391–401
Dipti A, Soucy Z, Surana A et al (2012) Role of inferior vena cava diameterin assessment of volume status: a meta-analysis. Am J Emerg Med 30(8):1414–1419
Acknowledgements
We would like to thank the Department of Anesthesiology of the Affiliated Jinhua Hospital, Zhejiang University School of Medicine, for their help in this study. We appreciate the linguistic assistance provided by TopEdit (www.topeditsci.com) during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Wang Wei was the major writer and designer of the experiment. Chen Bo, Guo Jun, Hu Chonghui, Zhang Yufan, and Chen Yuanliang were the participants in the experiment. They participated in the specific measurement and data recording of some experiments. Lan Zhijian participated in the design and guidance of the experiment.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wei, W., Bo, C., Jun, G. et al. Diagnostic Value of the Variations in Internal Jugular Vein Diameter and Blood Flow Rate in Patients with Intestinal Obstruction. Indian J Surg 85, 1111–1116 (2023). https://doi.org/10.1007/s12262-023-03681-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12262-023-03681-8