Abstract
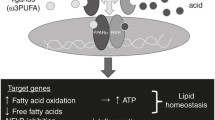
Peroxisome proliferator-activated receptor-α (PPARα) is a member of the nuclear receptor superfamily involved in hepatocarcinogenesis in rodents. In previous studies on liver tumor tissues, PPARα mRNA expression was found to be significantly higher and overexpression of ERα inhibited the PPARα expression, cell-proliferation and also induced apoptosis in Hep3B cell. However, the role of ERβ is not known yet. Therefore, the aim of this study is to define the role of ERβ on PPARα in Hep3B cells. The effect of PPARα signaling cascade were monitored by inducing Hep3B cells by fenofibrate. Further the cells were transfected with pCMV-ERβ and the consequences of ERβ-overexpression on the PPARα induced changes such as enhanced cell-proliferation and suppressed apoptosis were determined using western blot analysis and TUNEL assay. The EMSA was used to identify whether ERβ modulates PPARα expression by binding to PPARα promoter region to repress PPARα promoter activity. In addition, the direct interaction between ERβ and PPARα proteins was verified by co-immunoprecipitation assay. Our results show that the overexpressed ERβ not only attenuated the effects of fenofibrate to induce the levels of apoptosis protein such as Cyt.c, Caspase 9 and Caspase 3 but also inhibited the levels of survival protein such Bcl-xL, p-Bad, cyclin A and cyclin E. All these effects of E2/ERβ resulted in the enhancement of mitochondria dependent apoptotic pathway and the attenuation of cell proliferation. Moreover, the overexpressed ERβ reduced the mRNA and protein levels of PPARα and its downstream Acyl-CoA oxidase (ACO). EMSA results show that ERβ directly binds to PPRE and inhibit PPARα gene expression and according to immunoprecipitation assay ERβ also binds strongly with PPARα. The E2/ERβ further inhibited the fenofibrate-induced nuclear translocation of PPARα. Taken together, ERβ might directly downregulate PPARα gene expression and inhibit the nuclear translocation to suppress the proliferation and induce the apoptosis of Hep3B cells.









Similar content being viewed by others
Reference
Bruix J, Boix L, Sala M, Llovet JM (2004) Focus on hepatocellular carcinoma. Cancer Cell 5(3):215–219
Reddy JK, Krishnakantha TP (1975) Hepatic peroxisome proliferation: induction by two novel compounds structurally unrelated to clofibrate. Science 190(4216):787–789
Yeldandi AV, Rao MS, Reddy JK (2000) Hydrogen peroxide generation in peroxisome proliferator-induced oncogenesis. Mutat Res 448(2):159–177
Wu CY, Huang HM, Cho DY (2015) An acute bleeding metastatic spinal tumor from HCC causes an acute onset of cauda equina syndrome. Biomedicine 5(3):18. doi:10.7603/s40681-015-0018-5
Misra P, Reddy JK (2014) Peroxisome proliferator-activated receptor-alpha activation and excess energy burning in hepatocarcinogenesis. Biochimie 98:63–74. doi:10.1016/j.biochi.2013.11.011
Reddy JK, Azarnoff DL, Hignite CE (1980) Hypolipidaemic hepatic peroxisome proliferators form a novel class of chemical carcinogens. Nature 283(5745):397–398
Akriviadis EA, Llovet JM, Efremidis SC, Shouval D, Canelo R, Ringe B, Meyers WC (1998) Hepatocellular carcinoma. Br J Surg 85(10):1319–1331. doi:10.1046/j.1365-2168.1998.00865.x
Lin CY, Strom A, Li Kong S, Kietz S, Thomsen JS, Tee JB, Vega VB, Miller LD, Smeds J, Bergh J, Gustafsson JA, Liu ET (2007) Inhibitory effects of estrogen receptor beta on specific hormone-responsive gene expression and association with disease outcome in primary breast cancer. Breast Cancer Res BCR 9(2):R25. doi:10.1186/bcr1667
Lazennec G (2006) Estrogen receptor beta, a possible tumor suppressor involved in ovarian carcinogenesis. Cancer Lett 231(2):151–157. doi:10.1016/j.canlet.2005.01.021
Treeck O, Pfeiler G, Horn F, Federhofer B, Houlihan H, Vollmer A, Ortmann O (2007) Novel estrogen receptor beta transcript variants identified in human breast cancer cells affect cell growth and apoptosis of COS-1 cells. Mol Cell Endocrinol 264(1–2):50–60. doi:10.1016/j.mce.2006.10.003
Behrens D, Gill JH, Fichtner I (2007) Loss of tumourigenicity of stably ERbeta-transfected MCF-7 breast cancer cells. Mol Cell Endocrinol 274(1–2):19–29. doi:10.1016/j.mce.2007.05.012
Paruthiyil S, Parmar H, Kerekatte V, Cunha GR, Firestone GL, Leitman DC (2004) Estrogen receptor beta inhibits human breast cancer cell proliferation and tumor formation by causing a G2 cell cycle arrest. Cancer Res 64(1):423–428
Strom A, Hartman J, Foster JS, Kietz S, Wimalasena J, Gustafsson JA (2004) Estrogen receptor beta inhibits 17beta-estradiol-stimulated proliferation of the breast cancer cell line T47D. Proc Natl Acad Sci U S A 101(6):1566–1571. doi:10.1073/pnas.0308319100
Carruba G (2007) Estrogen and prostate cancer: an eclipsed truth in an androgen-dominated scenario. J Cell Biochem 102(4):899–911. doi:10.1002/jcb.21529
Stettner M, Kaulfuss S, Burfeind P, Schweyer S, Strauss A, Ringert RH, Thelen P (2007) The relevance of estrogen receptor-beta expression to the antiproliferative effects observed with histone deacetylase inhibitors and phytoestrogens in prostate cancer treatment. Mol Cancer Ther 6(10):2626–2633. doi:10.1158/1535-7163.MCT-07-0197
Cheng J, Lee EJ, Madison LD, Lazennec G (2004) Expression of estrogen receptor beta in prostate carcinoma cells inhibits invasion and proliferation and triggers apoptosis. FEBS Lett 566(1–3):169–172. doi:10.1016/j.febslet.2004.04.025
Chen GG, Zeng Q, Tse GM (2008) Estrogen and its receptors in cancer. Med Res Rev 28(6):954–974. doi:10.1002/med.20131
Jeong S, Yoon M (2007) Inhibition of the actions of peroxisome proliferator-activated receptor alpha on obesity by estrogen. Obesity 15(6):1430–1440. doi:10.1038/oby.2007.171
Huang EJ, Wu CC, Huang HP, Liu JY, Lin CS, Chang YZ, Lin JA, Lin JG, Chen LM, Lee SD, Kuo WW, Huang CY (2006) Apoptotic and anti-proliferative effects of 17beta-estradiol and 17beta-estradiol-like compounds in the Hep3B cell line. Mol Cell Biochem 290(1–2):1–7. doi:10.1007/s11010-005-9000-y
Marx N, Duez H, Fruchart JC, Staels B (2004) Peroxisome proliferator-activated receptors and atherogenesis: regulators of gene expression in vascular cells. Circ Res 94(9):1168–1178. doi:10.1161/01.RES.0000127122.22685.0A
Lee CH, Olson P, Evans RM (2003) Minireview: lipid metabolism, metabolic diseases, and peroxisome proliferator-activated receptors. Endocrinology 144(6):2201–2207. doi:10.1210/en.2003-0288
Lefebvre P, Chinetti G, Fruchart JC, Staels B (2006) Sorting out the roles of PPAR alpha in energy metabolism and vascular homeostasis. J Clin Invest 116(3):571–580. doi:10.1172/JCI27989
Venalainen T, Molnar F, Oostenbrink C, Carlberg C, Perakyla M (2010) Molecular mechanism of allosteric communication in the human PPARalpha-RXRalpha heterodimer. Proteins 78(4):873–887. doi:10.1002/prot.22613
Ringseis R, Gutgesell A, Dathe C, Brandsch C, Eder K (2007) Feeding oxidized fat during pregnancy up-regulates expression of PPARalpha-responsive genes in the liver of rat fetuses. Lipids Health Dis 6:6. doi:10.1186/1476-511X-6-6
Peters JM, Cheung C, Gonzalez FJ (2005) Peroxisome proliferator-activated receptor-alpha and liver cancer: where do we stand? J Mol Med 83(10):774–785. doi:10.1007/s00109-005-0678-9
Nishimura J, Dewa Y, Okamura T, Jin M, Saegusa Y, Kawai M, Umemura T, Shibutani M, Mitsumori K (2008) Role of Nrf2 and oxidative stress on fenofibrate-induced hepatocarcinogenesis in rats. Toxicological Sciences: an Official Journal of the Society of Toxicology 106(2):339–349. doi:10.1093/toxsci/kfn174
Bisteau X, Caldez MJ, Kaldis P (2014) The complex relationship between liver cancer and the cell cycle: a story of multiple regulations. Cancer 6(1):79–111. doi:10.3390/cancers6010079
Slingerland J, Pagano M (2000) Regulation of the cdk inhibitor p27 and its deregulation in cancer. J Cell Physiol 183(1):10–17. doi:10.1002/(SICI)1097-4652(200004)183:1<10::AID-JCP2>3.0.CO;2-I
Yue X, Zhang Z, Liang X, Gao L, Zhang X, Zhao D, Liu X, Ma H, Guo M, Spear BT, Gong Y, Ma C (2012) Zinc fingers and homeoboxes 2 inhibits hepatocellular carcinoma cell proliferation and represses expression of cyclins a and E. Gastroenterology 142(7):1559–1570 . doi:10.1053/j.gastro.2012.02.049e1552
Youssef J, Badr M (2011) Peroxisome proliferator-activated receptors and cancer: challenges and opportunities. Br J Pharmacol 164(1):68–82. doi:10.1111/j.1476-5381.2011.01383.x
Hasmall SC, James NH, Macdonald N, Gonzalez FJ, Peters JM, Roberts RA (2000) Suppression of mouse hepatocyte apoptosis by peroxisome proliferators: role of PPARalpha and TNFalpha. Mutat Res 448(2):193–200
Gonzalez FJ, Peters JM, Cattley RC (1998) Mechanism of action of the nongenotoxic peroxisome proliferators: role of the peroxisome proliferator-activator receptor alpha. J Natl Cancer Inst 90(22):1702–1709
Nishimura J, Dewa Y, Muguruma M, Kuroiwa Y, Yasuno H, Shima T, Jin M, Takahashi M, Umemura T, Mitsumori K (2007) Effect of fenofibrate on oxidative DNA damage and on gene expression related to cell proliferation and apoptosis in rats. Toxicological Sciences: an Official Journal of the Society of Toxicology 97(1):44–54. doi:10.1093/toxsci/kfm011
Shah YM, Morimura K, Yang Q, Tanabe T, Takagi M, Gonzalez FJ (2007) Peroxisome proliferator-activated receptor alpha regulates a microRNA-mediated signaling cascade responsible for hepatocellular proliferation. Mol Cell Biol 27(12):4238–4247. doi:10.1128/MCB.00317-07
Fidaleo M (2009) Human health risk assessment for peroxisome proliferators: more than 30 years of research. Experimental and Toxicologic Pathology: Official Journal of the Gesellschaft fur Toxikologische Pathologie 61(3):215–221. doi:10.1016/j.etp.2008.09.002
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Financial Statement
This study is supported in part by Taiwan Ministry of Health and Welfare Clinical Trial and Research Center of Excellence (MOHW105-TDU-B-212-133,019).
Rights and permissions
About this article
Cite this article
Chang-Lee, S.N., Hsu, HH., Shibu, M.A. et al. E2/ERβ Inhibits PPARα to Regulate Cell-Proliferation and Enhance Apoptosis in Hep3B-Hepatocellular Carcinoma. Pathol. Oncol. Res. 23, 477–485 (2017). https://doi.org/10.1007/s12253-016-0136-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12253-016-0136-8