Abstract
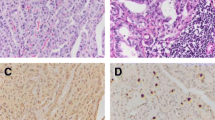
This study was aimed to assess the extend of nodal microdissemination in patients with pN0 papillary thyroid carcinoma (PTC) using immunohistochemical analysis. In early stage PTC both, systematic lymphadenectomy as well as radio iodine treatment, aimed to eliminate occult nodal tumor involvement, are under controversial debate, since little is known about the extend of lymphatic microdissemination in these patients. Formalin embedded samples of the resected lymph nodes were systematically screened for the presence of disseminated tumor cells using immunohistochemistry (monoclonal antibody Ber-EP4). Clinical and histopathological parameters as well as the post-operative course were recorded. Survival data were analysed by the Kaplan-Meier method and the log rank test. Overall 321 lymph nodes of 40 patients were screened immunohistochemically. In 12.5 % of the patients disseminated occult tumor cells were diagnosed. In addition to tumor resection 90 % of the patients underwent adjuvant radio-iodine treatment. The mean observation period in our collective was 72 months. The detection of disseminated tumor cells did not correlate with clinicopathologic risk parameters and did not have significant influence on the prognosis of these patients. Immunohistochemical analysis enables the detection of disseminated tumor cells in patients with pN0 PTC. This finding seems to support the application of adjuvant radio iodine, even in early tumor stages.

Similar content being viewed by others
References
DeGroot L, Kaplan E, McCormick M et al (1990) Natural history, treatment, and course of papillary thyroid carcinoma. J Clin Endocrinol Metab 71:414–424
Reynolds RM, Weir J, Stockton DL et al (2005) Changing trends in incidence and mortality of thyroid cancer in Scotland. Clin Endocrinol 62:152–162
Ito Y, Miyauchi A, Jikuzono T et al (2007) Risk factors contributing to a poor prognosis of papillary thyroid carcinoma; validity of UICC/AJCC TNM classification and stage grouping. World J Surg 31:838–848
Noguchi S, Murakami N, Yamashita H et al (1998) Papillary thyroid carcinoma: modified radical neck dissection improves prognosis. Arch Surg 133:276–280
Cranshaw IM, Carnaille B (2008) Micrometastases in thyroid cancer. An important finding? Surg Oncol 17:253–258
Borson-Chazot F, Causeret S, Lifante JC et al (2004) Predictive factors for recurrence of from a series of 74 children and adolescents with differentiated thyroid cancer. World J Surg 28:1088–1092
Cooper DS, Doherty GM, Haigen BR et al (2006) Management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid 16:109–142
Wada N, Duh QY, Sugino K et al (2003) Lymph node metastasis from 259 papillary thyroid microcarcinomas. Ann Surg 237:399–407
Ito Y, Tomoda C, Uruno T et al (2006) Clinical significance of metastasis to the central compartment from papillary microcarcinoma of the thyroid. World J Surg 30:91–99
Lundgren CI, Hall P, Dickman PW et al (2006) Clinically significant prognostic factors for differentiated thyroid carcinoma: a population-based, nested case control study. Cancer 106:524–531
Sawka AM, Brierley JD, Tsang RW et al (2008) An updated review and commentary examining the effectiveness of radioactive iodine remnant ablation in well differentiated thyroid cancer. Endocrinol Metab Clin North Am 37:457–480
Izbicki JR, Hosch SB, Pichlmeier U et al (1997) Prognostic value of immunohistochemically identifiable tumor cells in lymph nodes of patients with completely resected esophageal cancer. N Engl J Med 337:1188–1194
Rosenberg R, Friedrichs J, Gertler R et al (2004) Prognostic evaluation and review of immunohistochemically detected disseminated tumor cells in peritumoral lymph nodes of patients with pN0 colorectal cancer. Int J Colorectal Dis 19:430–437
Kurahara H, Takao S, Maemura K et al (2007) Impact of lymph node micrometastasis in patients with pancreatic head cancer. World J Surg 31:483–490
Hermanek P, Hutter RV, Sobin LH et al (1999) International Union Against Cancer. Classification of isolated tumor cells and micrometastasis. Cancer 86:2668–2673
Sobin LH, Wittekind C (eds) (1997) International Union Against Cancer (UICC). TNM classification of malignant tumors, 5th edn. Wiley, New York
De Klerk JMH, De Keizer B, Zelissen PMJ et al (2000) Fixed dosage of 131I for remnant ablation with differentiated thyroid carcinoma without pre-ablative diagnostic 131 scintigraphy. Nucl Med Commun 21:529–532
Scheunemann P, Stoecklein NH, Rehders A et al (2007) Frequency and prognostic significance of occult tumor cells in lymph nodes in patients with adenocarcinoma of the papilla of Vater. HPB (Oxford) 9:135–139
Latza U, Niedobitek G, Schwarting R et al (1990) Ber EP4: new monoclonal antibody, which distinguishes epithelia from mesothelial. J Clin Pathol 43:213–219
Stoecklein NH, Siegmund A, Scheunemann P et al (2006) Ep-CAM expression in squamous cell carcinoma of the esophagus: a potential therapeutic target and prognostic marker. BMC Cancer 6:135–143
Hsu SM, Raine L (1981) Protein A, avidin and biotin in immunohistochemistry. J Histochem Cytochem 29:1349–1353
Kaplan EL, Meier P (1958) Nonparametric estimation from incomplete observations. J Am Stat Assoc 53:457–481
Toniato A, Boschin I, Casara D et al (2008) Papillary thytoid carcinoma: factors influencing recurrence and survival. Ann Surg Oncol 15:1518–1522
Cappelli C, Castellano M, Braga M et al (2007) Aggressiveness and outcome of papillary thyroid carcinoma (PTC) versus microcarcinoma (PMC): a mono-institutional experience. J Surg Oncol 95:555–560
Ito Y, Higashiyama T, Takamura Y et al (2007) Risk factors for recurrence to the lymph node in papillary thyroid carcinoma patients without preoperatively detectable lateral node metastasis: validity of prophylactic modified radical neck dissection. World J Surg 31:2085–2091
Lo CY, Chan WF, Lam KY et al (2004) Optimizing the treatment of AMES high-risk papillary thyroid carcinoma. World J Surg 28:1103–1109
Monchik JM, Simon CJ, Caragacianu DL et al (2009) Does failure to perform prophylactic level VI node dissection leave persistent disease detectable by ultrasonography in patients with low-risk papillary carcinoma of the thyroid? Surgery 146:1182–1187
Rosenbaum MA, McHenry CR (2009) Central neck dissection for papillary thyroid cancer. Arch Otolaryngol Head Neck Surg 135:1092–1097
Mazzaferri EL, Doherty GM, Steward DL (2009) The pros and cons of prophylactic central compartment lymph node dissection for papillary thyroid carcinoma. Thyroid 19:683–689
Hughes CJ, Shaha AR, Shah JP et al (1996) Impact of lymph node metastasis in differentiated carcinoma of the thyroid; a matched pair analysis. Head Neck 18:127–132
Cady B, Sedgwick CE, Meissner WA et al (1979) Risk factor analysis in differentiated thyroid cancer. Cancer 43:810–820
Lugo TG, Braun S, Cote RJ et al (2003) Detection and measurement of occult disease for the prognosis of solid tumors. J Clin Oncol 21:2609–2615
Qubain SW, Nakano S, Baba M et al (2002) Distribution of lymph node micrometastasis in pN0 well-differentiated thyroid carcinoma. Surgery 131:249–256
Bardet S, Malville E, Rame JP et al (2008) The pros and cons of prophylactic central compartment lymph node dissection for papillary thyroid carcinoma. Eur J Endocrinol 158:551–560
Conflict of Interest
There is no conflict of interest that could be perceived as predjudicing the impartiality of the research reported.
Funding
This research did not receive any specific grant from any funding agency in the public, commercial or not-for-profit sector.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rehders, A., Anlauf, M., Adamowsky, I. et al. Is Minimal Residual Lymph Node Disease in Papillary Thyroid Cancer of Prognostic Impact? An Analysis of The Epithelial Cell Adhesion Molecule EpCAM in Lymph Nodes of 40 pN0 Patients. Pathol. Oncol. Res. 20, 185–190 (2014). https://doi.org/10.1007/s12253-013-9682-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12253-013-9682-5