Abstract
Introduction
Fibrin scaffolds are often utilized to treat chronic wounds. The monomer fibrinogen used to create such scaffolds is typically derived from adult human or porcine plasma. However, our previous studies have identified extensive differences in fibrin network properties between adults and neonates, including higher fiber alignment in neonatal networks. Wound healing outcomes have been linked to fibrin matrix structure, including fiber alignment, which can affect the binding and migration of cells. We hypothesized that fibrin scaffolds derived from neonatal fibrin would enhance wound healing outcomes compared to adult fibrin scaffolds.
Methods
Fibrin scaffolds were formed from purified adult or neonatal fibrinogen and thrombin then structural analysis was conducted via confocal microscopy. Human neonatal dermal fibroblast attachment, migration, and morphology on fibrin scaffolds were assessed. A murine full thickness injury model was used to compare healing in vivo in the presence of neonatal fibrin, adult fibrin, or saline.
Results
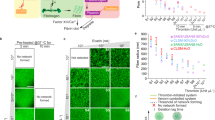
Distinct fibrin architectures were observed between adult and neonatal scaffolds. Significantly higher fibroblast attachment and migration was observed on neonatal scaffolds compared to adults. Cell morphology on neonatal scaffolds exhibited higher spreading compared to adult scaffolds. In vivo significantly smaller wound areas and greater epidermal thickness were observed when wounds were treated with neonatal fibrin compared to adult fibrin or a saline control.
Conclusions
Distinctions in neonatal and adult fibrin scaffold properties influence cellular behavior and wound healing. These studies indicate that fibrin scaffolds sourced from neonatal plasma could improve healing outcomes compared to scaffolds sourced from adult plasma.







Similar content being viewed by others
References
Andrew, M., L. Mitchell, L. R. Berry, B. Schmidt, and M. W. C. Hatton. Fibrinogen has a rapid turnover in the healthy newborn lamb. Pediatr. Res. 23:249–252, 1988.
Baker, B. M., and C. S. Chen. Deconstructing the third dimension—how 3D culture microenvironments alter cellular cues. J. Cell Sci. 125:3015–3024, 2012.
Bitsch, M., et al. Epidemiology of chronic wound patients and relation to serum levels of mannan-binding lectin. Acta Derm. Venereol. 89:607–611, 2009.
Brown, A. C., R. Hannan, L. H. Timmins, J. D. Fernandez, T. H. Barker, and N. A. Guzzetta. Fibrin network changes in neonates after cardiopulmonary bypass. Anesthesiology 124:1021–1031, 2016.
Brown, L. F., N. Lanir, J. McDonagh, K. Tognazzi, A. M. Dvorak, and H. F. Dvorak. Fibroblast migration in fibrin gel matrices. Am. J. Pathol. 142:273–283, 1993.
Buxboim, A., K. Rajagopal, A. E. X. Brown, and D. E. Discher. How deeply cells feel: methods for thin gels. J. Phys. Condens. Matter Inst. Phys. J. 22:194116, 2010.
Chester, D., and A. C. Brown. The role of biophysical properties of provisional matrix proteins in wound repair. Matrix Biol. 60–61:124–140, 2017.
Chiu, C. L., V. Hecht, H. Duong, B. Wu, and B. Tawil. Permeability of three-dimensional fibrin constructs corresponds to fibrinogen and thrombin concentrations. BioRe. Open Access 1:34–40, 2012.
Diaz-Mauriño, T., C. Castro, and A. Albert. Desialylation of fibrinogen with neuraminidase. Kinetic and clotting studies. Thromb. Res. 27:397–403, 1982.
Dietrich, M., et al. Fibrin-based tissue engineering: comparison of different methods of autologous fibrinogen isolation. Tissue Eng. Part C Methods 19:216–226, 2012.
Dunn, L., H. C. G. Prosser, J. T. M. Tan, L. Z. Vanags, M. K. C. Ng, and C. A. Bursill. Murine model of wound healing. J. Vis. Exp. 75:e50265, 2013.
Gailit, J., C. Clarke, D. Newman, M. G. Tonnesen, M. W. Mosesson, and R. A. Clark. Human fibroblasts bind directly to fibrinogen at RGD sites through integrin alpha(v)beta3. Exp. Cell Res. 232:118–126, 1997.
Gottrup, F. Optimizing wound treatment through health care structuring and professional education. Wound Repair Regen. Off. Publ. Wound Heal. Soc. Eur. Tissue Repair Soc. 12:129–133, 2004.
Haidl, H., et al. New insights into neonatal coagulation: normal clot formation despite lower intra-clot thrombin levels. Pediatr. Res. 86:719–724, 2019.
Ignjatovic, V., A. Ilhan, and P. Monagle. Evidence for age-related differences in human fibrinogen. Blood Coagul. Fibrinol. Int. J. Haemost. Thromb. 22:110–117, 2011.
Ismail, A. E. Purification of Fibrinogen from Human Plasma [Lincoln, Nebraska]. Lincoln: University of Nebraska, 2012.
Jackson, M. R. Fibrin sealants in surgical practice: an overview. Am. J. Surg. 182:1S–7S, 2001.
Järbrink, K., et al. Prevalence and incidence of chronic wounds and related complications: a protocol for a systematic review. Syst. Rev. 5:152, 2016.
Langer, B. G., J. W. Weisel, P. A. Dinauer, C. Nagaswami, and W. R. Bell. Deglycosylation of fibrinogen accelerates polymerization and increases lateral aggregation of fibrin fibers. J. Biol. Chem. 263:15056–15063, 1988.
Larson, B. J., M. T. Longaker, and H. P. Lorenz. Scarless fetal wound healing: a basic science review. Plast. Reconstr. Surg. 126:1172–1180, 2010.
Laurens, N., P. Koolwijk, and M. P. M. de Maat. Fibrin structure and wound healing. J. Thromb. Haemost. JTH 4:932–939, 2006.
Leon-Valdivieso, C. Y., et al. Fibroblast migration correlates with matrix softness. A study in knob-hole engineered fibrin. APL Bioeng. 2:036102, 2018.
Nandi, S., et al. Platelet-like particles dynamically stiffen fibrin matrices and improve wound healing outcomes. Biomater. Sci. 7:669–682, 2019.
Nellenbach, K., N. A. Guzzetta, and A. C. Brown. Analysis of the structural and mechanical effects of procoagulant agents on neonatal fibrin networks following cardiopulmonary bypass. J. Thromb. Haemost. JTH 16:2159–2167, 2018.
Nellenbach, K. A., S. Nandi, A. Kyu, S. Sivadanam, N. A. Guzzetta, and A. C. Brown. Comparison of neonatal and adult fibrin clot properties between porcine and human plasma. Anesthesiol. J. Am. Soc. Anesthesiol. 132:1091, 2020.
Qiu, L. L., S. S. Levinson, K. L. Keeling, and R. J. Elin. Convenient and effective method for removing fibrinogen from serum specimens before protein electrophoresis. Clin. Chem. 49:868–872, 2003.
Salsmann, A., E. Schaffner-Reckinger, F. Kabile, S. Plançon, and N. Kieffer. A new functional role of the fibrinogen RGD motif as the molecular switch that selectively triggers integrin αIIbβ3-dependent RhoA activation during cell spreading. J. Biol. Chem. 280:33610–33619, 2005.
Spotnitz, W. D. Fibrin sealant: the only approved hemostat, sealant, and adhesive—a laboratory and clinical perspective. ISRN Surg. 2014. https://doi.org/10.1155/2014/203943.
Sproul, E. P., S. Nandi, C. Roosa, L. Schreck, and A. C. Brown. Biomimetic microgels with controllable deformability improve healing outcomes. Adv. Biosyst. 2:1800042, 2018.
Tse, J. R., and A. J. Engler. Preparation of hydrogel substrates with tunable mechanical properties. Curr. Protoc. Cell Biol. 2010. https://doi.org/10.1002/0471143030.cb1016s47.
Undas, A., and R. A. S. Ariëns. Fibrin clot structure and function: a role in the pathophysiology of arterial and venous thromboembolic diseases. Arterioscler. Thromb. Vasc. Biol. 31:e88–99, 2011.
Van Cott, E. M., E. Y. Smith, and D. K. Galanakis. Elevated fibrinogen in an acute phase reaction prolongs the reptilase time but typically not the thrombin time. Am. J. Clin. Pathol. 118:263–268, 2002.
Varki, A. Sialic acids in human health and disease. Trends Mol. Med. 14:351–360, 2008.
Wagner, W., and M. Wehrmann. Differential cytokine activity and morphology during wound healing in the neonatal and adult rat skin. J. Cell. Mol. Med. 11:1342–1352, 2007.
Wang, W. Y., et al. Extracellular matrix alignment dictates the organization of focal adhesions and directs uniaxial cell migration. APL Bioeng. 2:046107, 2018.
Weisel, J. W., and R. I. Litvinov. Mechanisms of fibrin polymerization and clinical implications. Blood 121:1712–1719, 2013.
Werner, M., A. Petersen, N. A. Kurniawan, and C. V. C. Bouten. Cell migration: cell-perceived substrate curvature dynamically coordinates the direction, speed, and persistence of stromal cell migration. Adv. Biosyst. 3:1970102, 2019.
Acknowledgments
Funding for this project was provide by start-up funds for Ashley Brown from North Carolina State University, DMR-1847488 from the National Science Foundation, and CDMRP W81XWH-15-1-0485 from the U.S. Department of Defense. The authors would like to thank Eva Johannes, PhD, Director at the Cellular and Molecular Imaging Facility at North Carolina State University for technical assistance with microscopy, Nina Guzzetta, M.D. from Children’s Healthcare of Atlanta and Emory University for providing neonatal plasma samples, and Lucas Timmins, PhD from University of Utah for assistance with Matlab code.
Conflict of interest
Kimberly Nellenbach, Seema Nandi, Christopher Peeler, Alexander Kyu, and Ashley C. Brown declare that they have no conflicts of interest.
Ethical Approval
All human subjects research was carried out in accordance with Department of Health and Human Services policy and regulations and approved by the Emory University IRB. All animal studies were carried out in accordance with North Carolina State University policies and regulations including meeting standards and guidelines set forth by the NIH Guide for the Care and Use of Laboratory Animals. All animal studies were approved by the North Carolina State University IACUC.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Shelly Peyton oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Nellenbach, K., Nandi, S., Peeler, C. et al. Neonatal Fibrin Scaffolds Promote Enhanced Cell Adhesion, Migration, and Wound Healing In Vivo Compared to Adult Fibrin Scaffolds. Cel. Mol. Bioeng. 13, 393–404 (2020). https://doi.org/10.1007/s12195-020-00620-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12195-020-00620-5