Abstract
Introduction
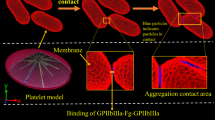
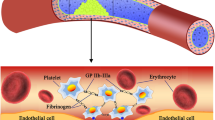
We developed a multiscale model to simulate the dynamics of platelet aggregation by recruitment of unactivated platelets flowing in viscous shear flows by an activated platelet deposited onto a blood vessel wall. This model uses coarse grained molecular dynamics for platelets at the microscale and dissipative particle dynamics for the shear flow at the macroscale. Under conditions of relatively low shear, aggregation is mediated by fibrinogen via αIIbβ3 receptors.
Methods
The binding of αIIbβ3 and fibrinogen is modeled by a molecular-level hybrid force field consisting of Morse potential and Hooke law for the nonbonded and bonded interactions, respectively. The force field, parametrized in two different interaction scales, is calculated by correlating with the platelet contact area measured in vitro and the detaching force between αIIbβ3 and fibrinogen.
Results
Using our model, we derived, the relationship between recruitment force and distance between the centers of mass of two platelets, by integrating the molecular-scale inter-platelet interactions during recruitment aggregation in shear flows. Our model indicates that assuming a rigid-platelet model, underestimates the contact area by 89% and the detaching force by 93% as compared to a model that takes into account the platelet deformability leading to a prediction of a significantly lower attachment during recruitment.
Conclusions
The molecular-level predictive capability of our model sheds a light on differences observed between transient and permanent platelet aggregation patterns. The model and simulation framework can be further adapted to simulate initial thrombus formation involving multiple flowing platelets as well as deposition and adhesion onto blood vessels.













Similar content being viewed by others
References
Benjamin, E. J., S. S. Virani, C. W. Callaway, A. M. Chamberlain, A. R. Chang, S. Cheng, S. E. Chiuve, M. Cushman, F. N. Delling, R. Deo, S. D. de Ferranti, J. F. Ferguson, M. Fornage, C. Gillespie, C. R. Isasi, M. C. Jimenez, L. C. Jordan, S. E. Judd, D. Lackland, J. H. Lichtman, L. Lisabeth, S. Liu, C. T. Longenecker, P. L. Lutsey, J. S. Mackey, D. B. Matchar, K. Matsushita, M. E. Mussolino, K. Nasir, M. O’Flaherty, L. P. Palaniappan, A. Pandey, D. K. Pandey, M. J. Reeves, M. D. Ritchey, C. J. Rodriguez, G. A. Roth, W. D. Rosamond, U. K. A. Sampson, G. M. Satou, S. H. Shah, N. L. Spartano, D. L. Tirschwell, C. W. Tsao, J. H. Voeks, J. Z. Willey, J. T. Wilkins, J. H. Wu, H. M. Alger, S. S. Wong, P. Muntner, and E. American Heart Association Council on, C. Prevention Statistics, and S. Stroke Statistics. Heart disease and stroke statistics-2018 update: a report from the American Heart Association. Circulation. 137:e67–e492, 2018.
Campbell, R. A., M. Aleman, L. D. Gray, M. R. Falvo, and A. S. Wolberg. Flow profoundly influences fibrin network structure: implications for fibrin formation and clot stability in haemostasis. Thromb. Haemost. 104:1281–1284, 2010.
Carvalho, F. A., and N. C. Santos. Atomic force microscopy-based force spectroscopy-biological and biomedical applications. IUBMB Life 64:465–472, 2012.
Espanol, P., and P. Warren. Statistical mechanics of dissipative particle dynamics. Europhys. Lett. 30:191, 1995.
Fedosov, D. A., and G. E. Karniadakis. Triple-decker: interfacing atomistic-mesoscopic-continuum flow regimes. J. Comput. Phys. 228:1157–1171, 2009.
Fogelson, A. L. Continuum models of platelet-aggregation: formulation and mechanical-properties. SIAM J. Appl. Math. 52:1089–1110, 1992.
Frojmovic, M. M. Flow cytometric analysis of platelet activation and fibrinogen binding. Platelets 7:9–21, 1996.
Gao, C., P. Zhang, G. Marom, Y. F. Deng, and D. Bluestein. Reducing the effects of compressibility in DPD-based blood flow simulations through severe stenotic microchannels. J. Comput. Phys. 335:812–827, 2017.
Girdhar, G., M. Xenos, Y. Alemu, W. C. Chiu, B. E. Lynch, J. Jesty, S. Einav, M. J. Slepian, and D. Bluestein. Device thrombogenicity emulation: a novel method for optimizing mechanical circulatory support device thromboresistance. PLoS ONE 7:e32463, 2012.
Goldsmith, H. L., F. A. McIntosh, J. Shahin, and M. M. Frojmovic. Time and force dependence of the rupture of glycoprotein IIb–IIIa-fibrinogen bonds between latex spheres. Biophys. J. 78:1195–1206, 2000.
Groot, R. D., and P. B. Warren. Dissipative particle dynamics: bridging the gap between atomistic and mesoscopic simulation. J. Chem. Phys. 107:4423–4435, 1997.
Haga, J. H., A. J. Beaudoin, J. G. White, and J. Strony. Quantification of the passive mechanical properties of the resting platelet. Ann. Biomed. Eng. 26:268–277, 1998.
Huang, P. Y., and J. D. Hellums. Aggregation and disaggregation kinetics of human blood platelets: Part I. Development and validation of a population balance method. Biophys. J. 65:334–343, 1993.
Huang, P. Y., and J. D. Hellums. Aggregation and disaggregation kinetics of human blood platelets: part II. Shear-induced platelet aggregation. Biophys. J. 65:344–353, 1993.
Huang, P. Y., and J. D. Hellums. Aggregation and disaggregation kinetics of human blood platelets: part III. The disaggregation under shear stress of platelet aggregates. Biophys. J. 65:354–361, 1993.
Jackson, S. P. The growing complexity of platelet aggregation. Blood 109:5087–5095, 2007.
Jackson, S. P., W. S. Nesbitt, and E. Westein. Dynamics of platelet thrombus formation. J. Thromb. Haemost. 7(Suppl 1):17–20, 2009.
Lakes, R. Materials science: a broader view of membranes. Nature 414:503–504, 2001.
Leiderman, K., and A. L. Fogelson. Grow with the flow: a spatial-temporal model of platelet deposition and blood coagulation under flow. Math. Med. Biol. 28:47–84, 2011.
Liang, X. M., S. J. Han, J. A. Reems, D. Gao, and N. J. Sniadecki. Platelet retraction force measurements using flexible post force sensors. Lab. Chip. 10:991–998, 2010.
Litvinov, R. I., D. H. Farrell, J. W. Weisel, and J. S. Bennett. The platelet integrin alphaIIbbeta3 differentially interacts with fibrin versus fibrinogen. J. Biol. Chem. 291:7858–7867, 2016.
Martinez, E. J., Y. Lanir, and S. Einav. Effects of contact-induced membrane stiffening on platelet adhesion. Biomech. Mod. Mechanobiol. 2:157–167, 2004.
Maxwell, M. J., E. Westein, W. S. Nesbitt, S. Giuliano, S. M. Dopheide, and S. P. Jackson. Identification of a 2-stage platelet aggregation process mediating shear-dependent thrombus formation. Blood 109:566–576, 2007.
Michelson, A. D. Platelets (3rd ed.). Cambridge: Academic Press, 2013.
Mody, N. A., and M. R. King. Three-dimensional simulations of a platelet-shaped spheroid near a wall in shear flow. Phys. Fluids. 17:113302, 2005.
Mody, N. A., and M. R. King. Platelet adhesive dynamics. Part I: Characterization of platelet hydrodynamic collisions and wall effects. Biophys. J. 95:2539–2555, 2008.
Mody, N. A., and M. R. King. Platelet adhesive dynamics. Part II: high shear-induced transient aggregation via GPIbalpha-vWF-GPIbalpha bridging. Biophys. J. 95:2556–2574, 2008.
Nesbitt, W. S., E. Westein, F. J. Tovar-Lopez, E. Tolouei, A. Mitchell, J. Fu, J. Carberry, A. Fouras, and S. P. Jackson. A shear gradient-dependent platelet aggregation mechanism drives thrombus formation. Nat. Med. 15:665–673, 2009.
Parise, L. V., and D. R. Phillips. Reconstitution of the purified platelet fibrinogen receptor. Fibrinogen binding properties of the glycoprotein IIb–IIIa complex. J. Biol. Chem. 260:10698–10707, 1985.
Pivkin, I. V., P. D. Richardson, and G. Karniadakis. Blood flow velocity effects and role of activation delay time on growth and form of platelet thrombi. Proc. Natl. Acad. Sci. USA 103:17164–17169, 2006.
Pivkin, I., P. Richardson, and G. Karniadakis. Effect of red blood cells on platelet aggregation. IEEE Eng. Med. Biol. Mag. 28:32–37, 2009.
Plimpton, S., A. Thompson, and P. Crozier. LAMMPS Molecular Dynamics Simulator. http://lammps.sandia.gov, 2012.
Pothapragada, S., P. Zhang, J. Sheriff, M. Livelli, M. J. Slepian, Y. Deng, and D. Bluestein. A phenomenological particle-based platelet model for simulating filopodia formation during early activation. Int. J. Numer. Method Biomed. Eng. 31:e02702, 2015.
Qiu, Y., J. Ciciliano, D. R. Myers, R. Tran, and W. A. Lam. Platelets and physics: how platelets “feel” and respond to their mechanical microenvironment. Blood Rev. 29:377–386, 2015.
Ruggeri, Z. M. Von. Willebrand factor, platelets and endothelial cell interactions. J. Thromb. Haemost. 1:1335–1342, 2003.
Ruggeri, Z. M., J. N. Orje, R. Habermann, A. B. Federici, and A. J. Reininger. Activation-independent platelet adhesion and aggregation under elevated shear stress. Blood 108:1903–1910, 2006.
Sheriff, J., J. S. Soares, M. Xenos, J. Jesty, M. J. Slepian, and D. Bluestein. Evaluation of shear-induced platelet activation models under constant and dynamic shear stress loading conditions relevant to devices. Ann. Biomed. Eng. 41:1279–1296, 2013.
Shiozaki, S., S. Takagi, and S. Goto. Prediction of molecular interaction between platelet glycoprotein Ibalpha and von Willebrand factor using molecular dynamics simulations. J Atheroscler. Thromb. 23:455–464, 2016.
Smyth, S. S., and L. V. Parise. Regulation of ligand binding to glycoprotein IIb–IIIa (integrin alpha IIb beta 3) in isolated platelet membranes. Biochem. J. 292(Pt 3):749–758, 1993.
Soares, J. S., C. Gao, Y. Alemu, M. Slepian, and D. Bluestein. Simulation of platelets suspension flowing through a stenosis model using a dissipative particle dynamics approach. Ann. Biomed. Eng. 41:2318–2333, 2013.
Tosenberger, A., F. Ataullakhanov, N. Bessonov, M. Panteleev, A. Tokarev, and V. Volpert. The role of platelets in blood coagulation during thrombus formation in flow. HAL. 2012.
Tosenberger, A., F. Ataullakhanov, N. Bessonov, M. Panteleev, A. Tokarev, and V. Volpert. Modelling of thrombus growth and growth stop in flow by the method of dissipative particle dynamics. Russ. J. Numer. Anal. Math. 27:507–522, 2012.
Weisel, J. W., C. Nagaswami, G. Vilaire, and J. S. Bennett. Examination of the platelet membrane glycoprotein IIb–IIIa complex and its interaction with fibrinogen and other ligands by electron microscopy. J. Biol. Chem. 267:16637–16643, 1992.
Willemsen, S. M., H. C. J. Hoefsloot, and P. D. Iedema. No-slip boundary condition in dissipative particle dynamics. Int. J. Mod. Phys. C 11:881–890, 2000.
Yazdani, A., H. Li, J. D. Humphrey, and G. E. Karniadakis. A general shear-dependent model for thrombus formation. PLoS Comput. Biol. 13:e1005291, 2017.
Zhang, P., C. Gao, N. Zhang, M. J. Slepian, Y. F. Deng, and D. Bluestein. Multiscale particle-based modeling of flowing platelets in blood plasma using dissipative particle dynamics and coarse grained molecular dynamics. Cell. Mol. Bioeng. 7:552–574, 2014.
Zhang, J., P. C. Johnson, and A. S. Popel. Red blood cell aggregation and dissociation in shear flows simulated by lattice Boltzmann method. J. Biomech. 41:47–55, 2008.
Zhang, P., L. Zhang, M. J. Slepian, Y. Deng, and D. Bluestein. A multiscale biomechanical model of platelets: correlating with in vitro results. J. Biomech. 50:26–33, 2017.
Acknowledgements
This publication was made possible by grants from the National NIH U01 HL131052-014 (PI: Danny Bluestein, Co-Investigators: Yuefan Deng, Marvin J. Slepian). The simulations in this study used the XSEDE computing resource award DMS150011 at the SDSC Comet supercomputer (PI: Peng Zhang) and LI-Red supercomputer, Stony Brook University.
Conflict of interest
Prachi Gupta, Peng Zhang, Jawaad Sheriff, Danny Bluestein and Yuefan Deng declare that they have no conflict of interest.
Human Studies
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000 (5). Informed consent was obtained from all patients for being included in the study. No animal studies were carried out by the authors for this article.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Michael R. King oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gupta, P., Zhang, P., Sheriff, J. et al. A Multiscale Model for Recruitment Aggregation of Platelets by Correlating with In Vitro Results. Cel. Mol. Bioeng. 12, 327–343 (2019). https://doi.org/10.1007/s12195-019-00583-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12195-019-00583-2