Abstract
Introduction
Lack of effective pharmacological treatment makes valvular calcification a significant clinical problem in patients with valvular disease and bioprosthetic/mechanical valve replacement therapies. Elevated levels of reactive oxygen species (ROS) in valve tissue have been identified as a prominent hallmark and driving factor for valvular calcification. However, the therapeutic value of ROS-modulating agents for valvular calcification remains elusive. We hypothesized that ROS-modulating shape-specific cerium oxide nanoparticles (CNPs) will inhibit oxidative stress-induced valvular calcification. CNPs are a class of self-regenerative ROS-modulating agents, which can switch between Ce3+ and Ce4+ in response to oxidative microenvironment. In this work, we developed oxidative stress-induced valve calcification model using two patient-derived stenotic valve interstitial cells (hVICs) and investigated the therapeutic effect of shape-specific CNPs to inhibit hVIC calcification.
Methods
Human valvular interstitial cells (hVICs) were obtained from a normal healthy donor and two patients with calcified aortic valves. hVICs were characterized for their phenotypic (mesenchymal, myofibroblast and osteoblast) marker expression by qRT-PCR and antioxidant enzymes activity before and after exposure to hydrogen peroxide (H2O2)-induced oxidative stress. Four shape-specific CNPs (sphere, short rod, long rod, and cube) were synthesized via hydrothermal or ultra-sonication method and characterized for their biocompatibility in hVICs by alamarBlue® assay, and ROS scavenging ability by DCFH-DA assay. H2O2 and inorganic phosphate (Pi) were co-administrated to induce hVIC calcification in vitro as demonstrated by Alizarin Red S staining and calcium quantification. The effect of CNPs on inhibiting H2O2-induced hVIC calcification was evaluated.
Results
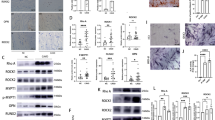
hVICs isolated from calcified valves exhibited elevated osteoblast marker expression and decreased antioxidant enzyme activities compared to the normal hVICs. Due to the impaired antioxidant enzyme activities, acute H2O2-induced oxidative stress resulted in higher ROS levels and osteoblast marker expression in both diseased hVICs when compared to the normal hVICs. Shape-specific CNPs exhibited shape-dependent abiotic ROS scavenging ability, and excellent cytocompatibility. Rod and sphere CNPs scavenged H2O2-induced oxidative stress in hVICs in a shape- and dose-dependent manner by lowering intracellular ROS levels and osteoblast marker expression. Further, CNPs also enhanced activity of antioxidant enzymes in hVICs to combat oxidative stress. Cube CNPs were not effective ROS scavengers. The addition of H2O2 in the Pi-induced calcification model further increased calcium deposition in vitro in a time-dependent manner. Co-administration of rod CNPs with Pi and H2O2 mitigated calcification in the diseased hVICs.
Conclusions
We demonstrated that hVICs derived from calcified valves exhibited impaired antioxidant defense mechanisms and were more susceptible to oxidative stress than normal hVICs. CNPs scavenged H2O2-induced oxidative stress in hVICs in a shape-dependent manner. The intrinsic ROS scavenging ability of CNPs and their ability to induce cellular antioxidant enzyme activities may confer protection from oxidative stress-exacerbated calcification. CNPs represent promising antioxidant therapy for treating valvular calcification and deserve further investigation.







Similar content being viewed by others
References
Mozaffarian, D., E. J. Benjamin, A. S. Go, D. K. Arnett, M. J. Blaha, M. Cushman, S. R. Das, S. de Ferranti, J.-P. Després, H. J. Fullerton, V. J. Howard, M. D. Huffman, C. R. Isasi, M. C. Jiménez, S. E. Judd, B. M. Kissela, J. H. Lichtman, L. D. Lisabeth, S. Liu, R. H. Mackey, D. J. Magid, D. K. McGuire, E. R. Mohler, C. S. Moy, P. Muntner, M. E. Mussolino, K. Nasir, R. W. Neumar, G. Nichol, L. Palaniappan, D. K. Pandey, M. J. Reeves, C. J. Rodriguez, W. Rosamond, P. D. Sorlie, J. Stein, A. Towfighi, T. N. Turan, S. S. Virani, D. Woo, R. W. Yeh, and M. B. Turner. Executive summary: heart disease and stroke statistics—2016 update. Circulation 133:447–454, 2016.
Otto, C. M. Calcific aortic stenosis—time to look more closely at the valve. N. Engl. J. Med. 359:1395–1398, 2008.
Schoen, F. J., and R. J. Levy. Calcification of tissue heart valve substitutes: progress toward understanding and prevention. Ann. Thorac. Surg. 79:1072–1080, 2005.
Xue, Y., V. Sant, J. Phillippi, and S. Sant. Biodegradable and biomimetic elastomeric scaffolds for tissue-engineered heart valves. Acta Biomater. 48:2–19, 2017.
Hutcheson, J. D., E. Aikawa, and W. D. Merryman. Potential drug targets for calcific aortic valve disease. Nat. Rev. Cardiol. 11:218–231, 2014.
Mathieu, P., and M.-C. Boulanger. Basic mechanisms of calcific aortic valve disease. Can. J. Cardiol. 30:982–993, 2014.
Sverdlov, A. L., D. T. Ngo, M. J. Chapman, O. A. Ali, Y. Y. Chirkov, and J. D. Horowitz. Pathogenesis of aortic stenosis: not just a matter of wear and tear. Am. J. Cardiovasc. Dis. 1:185–199, 2011.
Butcher, J. T., G. J. Mahler, and L. A. Hockaday. Aortic valve disease and treatment: the need for naturally engineered solutions. Adv. Drug Deliv. Rev. 63:242–268, 2011.
Heistad, D. D., Y. Wakisaka, J. Miller, Y. Chu, and R. Pena-Silva. Novel aspects of oxidative stress in cardiovascular diseases. Circ. J. 73:201–207, 2009.
Miller, J. D., R. M. Weiss, and D. D. Heistad. Calcific aortic valve stenosis: methods, models, and mechanisms. Circ. Res. 108:1392–1412, 2011.
Yip, C. Y. Y., and C. A. Simmons. The aortic valve microenvironment and its role in calcific aortic valve disease. Cardiovasc. Pathol. 20:177–182, 2011.
Schoen, F. J. Mechanisms of function and disease of natural and replacement heart valves. Annu. Rev. Pathol.: Mech. Dis. 7:161–183, 2012.
Hutcheson, J. D., M. C. Blaser, and E. Aikawa. Giving calcification its due: recognition of a diverse disease. Circ. Res. 120:270–273, 2017.
Miller, J. D., Y. Chu, R. M. Brooks, W. E. Richenbacher, R. Peña-Silva, and D. D. Heistad. Dysregulation of antioxidant mechanisms contributes to increased oxidative stress in calcific aortic valvular stenosis in humans. J. Am. Coll. Cardiol. 52:843–850, 2008.
Miller, J. D., R. M. Weiss, K. M. Serrano, R. M. Brooks, C. J. Berry, K. Zimmerman, S. G. Young, and D. D. Heistad. Lowering plasma cholesterol levels halts progression of aortic valve disease in mice. Circulation 119:2693–2701, 2009.
Fernández Esmerats, J., J. Heath, and H. Jo. Shear-sensitive genes in aortic valve endothelium. Antioxid. Redox Signal. 25:401–414, 2016.
Bostrom, K. I., N. M. Rajamannan, and D. A. Towler. The regulation of valvular and vascular sclerosis by osteogenic morphogens. Circ. Res. 109:564–577, 2011.
Branchetti, E., R. Sainger, P. Poggio, J. B. Grau, J. Patterson-Fortin, J. E. Bavaria, M. Chorny, E. Lai, R. C. Gorman, R. J. Levy, and G. Ferrari. Antioxidant enzymes reduce DNA damage and early activation of valvular interstitial cells in aortic valve sclerosis. Arterioscler. Thromb. Vasc. Biol. 33:e66–e74, 2012.
Bowler, M. A., and W. D. Merryman. in vitro models of aortic valve calcification: solidifying a system. Cardiovasc. Pathol. 24:1–10, 2015.
Aikawa, E., K. L. Cloyd, I. El-Hamamsy, S. Boonrungsiman, M. Hedegaard, E. Gentleman, P. Sarathchandra, F. Colazzo, M. M. Gentleman, M. H. Yacoub, A. H. Chester, and M. M. Stevens. Characterization of porcine aortic valvular interstitial cell ‘calcified’ nodules. PLoS ONE 7:e48154, 2012.
Mulholland, D. L., and A. I. Gotlieb. Cell biology of valvular interstitial cells. Can. J. Cardiol. 12:231–236, 1996.
Liberman, M., E. Bassi, M. K. Martinatti, F. C. Lario, J. Wosniak, P. M. A. Pomerantzeff, and F. R. M. Laurindo. Oxidant generation predominates around calcifying foci and enhances progression of aortic valve calcification. Arterioscler. Thromb. Vasc. Biol. 28:463–470, 2007.
Shao, J. S. Molecular mechanisms of vascular calcification: lessons learned from the aorta. Arterioscler. Thromb. Vasc. Biol. 26:1423–1430, 2006.
Griendling, K. K. Oxidative stress and cardiovascular injury: part II: animal and human studies. Circulation 108:2034–2040, 2003.
Kobayashi, S., N. Inoue, H. Azumi, T. Seno, K. Hirata, S. Kawashima, Y. Hayashi, H. Itoh, H. Yokozaki, and M. Yokoyama. Expressional changes of the vascular antioxidant system in atherosclerotic coronary arteries. J. Atheroscler. Thromb. 9:184–190, 2002.
Kim, K. M. Calcification of matrix vesicles in human aortic valve and aortic media. Fed. Proc. 35:156–162, 1976.
Walkey, C., S. Das, S. Seal, J. Erlichman, K. Heckman, L. Ghibelli, E. Traversa, J. F. McGinnis, and W. T. Self. Catalytic properties and biomedical applications of cerium oxide nanoparticles. Environ. Sci.: Nano 2:33–53, 2015.
Nelson, B., M. Johnson, M. Walker, K. Riley, and C. Sims. Antioxidant cerium oxide nanoparticles in biology and medicine. Antioxidants 5:15, 2016.
Rzigalinski, B. A., C. S. Carfagna, and M. Ehrich. Cerium oxide nanoparticles in neuroprotection and considerations for efficacy and safety. WIREs Nanomed. Nanobiotechnol. 9:e1444, 2017. doi:10.1002/wnan.1444.
Xue, Y., S. R. Balmuri, A. Patel, V. Sant, and S. Sant. Synthesis, physico-chemical characterization, and antioxidant effect of PEGylated cerium oxide nanoparticles. Drug Deliv. Transl. Res. 2017. doi:10.1007/s13346-017-0396-1.
Niu, J., K. Wang, and P. E. Kolattukudy. Cerium oxide nanoparticles inhibits oxidative stress and nuclear factor- B activation in H9c2 cardiomyocytes exposed to cigarette smoke extract. J. Pharmacol. Exp. Ther. 338:53–61, 2011.
Pagliari, F., C. Mandoli, G. Forte, E. Magnani, S. Pagliari, G. Nardone, S. Licoccia, M. Minieri, P. Di Nardo, and E. Traversa. Cerium oxide nanoparticles protect cardiac progenitor cells from oxidative stress. ACS Nano 6:3767–3775, 2012.
Kolli, M. B., N. D. P. K. Manne, R. Para, S. K. Nalabotu, G. Nandyala, T. Shokuhfar, K. He, A. Hamlekhan, J. Y. Ma, P. S. Wehner, L. Dornon, R. Arvapalli, K. M. Rice, and E. R. Blough. Cerium oxide nanoparticles attenuate monocrotaline induced right ventricular hypertrophy following pulmonary arterial hypertension. Biomaterials 35:9951–9962, 2014.
Niu, J., A. Azfer, L. Rogers, X. Wang, and P. Kolattukudy. Cardioprotective effects of cerium oxide nanoparticles in a transgenic murine model of cardiomyopathy. Cardiovasc. Res. 73:549–559, 2007.
Mai, H.-X., L.-D. Sun, Y.-W. Zhang, R. Si, W. Feng, H.-P. Zhang, H.-C. Liu, and C.-H. Yan. Shape-selective synthesis and oxygen storage behavior of ceria nanopolyhedra, nanorods, and nanocubes. J. Phys. Chem. B 109:24380–24385, 2005.
Li, Y., M. Kröger, and W. K. Liu. Shape effect in cellular uptake of PEGylated nanoparticles: comparison between sphere, rod, cube and disk. Nanoscale 7:16631–16646, 2015.
Jo, D. H., J. H. Kim, T. G. Lee, and J. H. Kim. Size, surface charge, and shape determine therapeutic effects of nanoparticles on brain and retinal diseases. Nanomed.: Nanotechnol. Biol. Med. 11:1603–1611, 2015.
Gould, R. A., and J. T. Butcher. Isolation of valvular endothelial cells. J. Vis. Exp. 23:12, 2010.
Zhang, D., H. Fu, L. Shi, C. Pan, Q. Li, Y. Chu, and W. Yu. Synthesis of CeO2 nanorods via ultrasonication assisted by polyethylene glycol. Inorg. Chem. 46:2446–2451, 2007.
Gaharwar, A. K., S. M. Mihaila, A. Swami, A. Patel, S. Sant, R. L. Reis, A. P. Marques, M. E. Gomes, and A. Khademhosseini. Bioactive silicate nanoplatelets for osteogenic differentiation of human mesenchymal stem cells. Adv. Mater. 25:3329–3336, 2013.
Cox, R. F., A. Hernandez-Santana, S. Ramdass, G. McMahon, J. H. Harmey, and M. P. Morgan. Microcalcifications in breast cancer: novel insights into the molecular mechanism and functional consequence of mammary mineralisation. Br. J. Cancer 106:525–537, 2012.
Liu, A. C., V. R. Joag, and A. I. Gotlieb. The emerging role of valve interstitial cell phenotypes in regulating heart valve pathobiology. Am. J. Pathol. 171:1407–1418, 2007.
Pesce, M., N. Latif, A. Quillon, P. Sarathchandra, A. McCormack, A. Lozanoski, M. H. Yacoub, and A. H. Chester. Modulation of human valve interstitial cell phenotype and function using a fibroblast growth factor 2 formulation. PLoS ONE 10:e0127844, 2015.
Monzack, E. L., and K. S. Masters. Can valvular interstitial cells become true osteoblasts? A side-by-side comparison. J. Heart Valve Dis. 20:449–463, 2011.
Hjortnaes, J., C. Goettsch, J. D. Hutcheson, G. Camci-Unal, L. Lax, K. Scherer, S. Body, F. J. Schoen, J. Kluin, A. Khademhosseini, and E. Aikawa. Simulation of early calcific aortic valve disease in a 3D platform: a role for myofibroblast differentiation. J. Mol. Cell. Cardiol. 94:13–20, 2016.
MatÉs, J. M., C. Pérez-Gómez, and I. N. De Castro. Antioxidant enzymes and human diseases. Clin. Biochem. 32:595–603, 1999.
Gough, D. R., and T. G. Cotter. Hydrogen peroxide: a Jekyll and Hyde signalling molecule. Cell Death Dis. 2:e213, 2011.
Byon, C. H., A. Javed, Q. Dai, J. C. Kappes, T. L. Clemens, V. M. Darley-Usmar, J. M. McDonald, and Y. Chen. Oxidative stress induces vascular calcification through modulation of the osteogenic transcription factor Runx2 by AKT signaling. J. Biol. Chem. 283:15319–15327, 2008.
Lai, C.-F., J.-S. Shao, A. Behrmann, K. Krchma, S.-L. Cheng, and D. A. Towler. TNFR1-activated reactive oxidative species signals up-regulate osteogenic Msx2 programs in aortic myofibroblasts. Endocrinology 153:3897–3910, 2012.
Pulido-Reyes, G., I. Rodea-Palomares, S. Das, T. S. Sakthivel, F. Leganes, R. Rosal, S. Seal, and F. Fernández-Piñas. Untangling the biological effects of cerium oxide nanoparticles: the role of surface valence states. Sci. Rep. 5:15613, 2015.
Sakthivel, T., S. Das, A. Kumar, D. L. Reid, A. Gupta, D. C. Sayle, and S. Seal. Morphological phase diagram of biocatalytically active ceria nanostructures as a function of processing variables and their properties. ChemPlusChem 78:1446–1455, 2013.
Pirmohamed, T., J. M. Dowding, S. Singh, B. Wasserman, E. Heckert, A. S. Karakoti, J. E. S. King, S. Seal, and W. T. Self. Nanoceria exhibit redox state-dependent catalase mimetic activity. Chem. Commun. 46:2736, 2010.
Popov, A. L., N. R. Popova, I. I. Selezneva, A. Y. Akkizov, and V. K. Ivanov. Cerium oxide nanoparticles stimulate proliferation of primary mouse embryonic fibroblasts in vitro. Mater. Sci. Eng.: C 68:406–413, 2016.
Giachelli, C. M. The emerging role of phosphate in vascular calcification. Kidney Int. 75:890–897, 2009.
Mazière, C., V. Savitsky, A. Galmiche, C. Gomila, Z. Massy, and J.-C. Mazière. Oxidized low density lipoprotein inhibits phosphate signaling and phosphate-induced mineralization in osteoblasts. Involvement of oxidative stress. Biochim. Biophys. Acta (BBA)—Mol. Basis Dis. 1802:1013–1019, 2010.
Zhang, Q., K. Ge, H. Ren, C. Zhang, and J. Zhang. Effects of cerium oxide nanoparticles on the proliferation, osteogenic differentiation and adipogenic differentiation of primary mouse bone marrow stromal cells in vitro. J. Nanosci. Nanotechnol. 15:6444–6451, 2015.
Mason, D., Y.-Z. Chen, H. V. Krishnan, and S. Sant. Cardiac gene therapy: recent advances and future directions. J. Control. Release 215:101–111, 2015.
Acknowledgment
We acknowledge funding support from the School of Pharmacy, University of Pittsburgh (SS) and HL117917, NHLBI (CSH). YX acknowledges Graduate Student Research Scholarship from the School of Pharmacy, University of Pittsburgh. We thank Dr. Thomas Gleason, Center for Thoracic Aortic Disease, University of Pittsburgh for providing us with valve cusp tissue to collect the valve cells and Jennifer Hill for isolating valve cells. We thank Dr. Donna Stolz, Center for Biologic Imaging, University of Pittsburgh for access to TEM facility and Akhil Patel, School of Pharmacy, University of Pittsburgh for acquiring the TEM images. We thank Dr. Paul Johnston, School of Pharmacy, University of Pittsburgh for access to the spectrophotometer.
Conflict of interest
Shilpa Sant has an invention disclosure filed as “shape-specific CNPs as ROS and immune-modulating agents”. Yingfei Xue, Cynthia St. Hilaire, Luis Hortells, Julie A. Phillippi, and Vinayak Sant declare that they have no conflicts of interest.
Ethical standards
All human subjects researches were carried out in accordance with the ethical standards approved by the University of Pittsburgh Institutional Review Board and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. No animal studies were carried out by the authors for this article.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Alyssa Panitch oversaw the review of this article.
Shilpa Sant, PhD, is an Assistant Professor at University of Pittsburgh in the Department of Pharmaceutical Sciences with secondary appointment in Bioengineering. She is also a member faculty at the McGowan Institute for Regenerative Medicine and UPMC Hillman Cancer Center. Dr. Sant received a PhD in Pharmaceutical Technology from University of Montreal, Canada; MS in Pharmacology and B.Pharm. in Pharmaceutical Sciences from University of Mumbai. Before joining Pitt, she was a Ruth Kirschstein fellow with Drs. Ali Khademhosseini and Richard Maas at the Wyss Institute for Biologically Inspired Engineering and the Center for Bioengineering at Brigham and Women’s Hospital. Her major research interests include bioinspired approaches for regenerative therapies and development of biomimetic microenvironments for in vitro three-dimensional disease progression models. Her lab uses interdisciplinary approaches to study role of microenvironments on disease progression in the same cells without any genetic manipulations or artificial culture conditions. Dr. Sant has contributed more than 50 papers, book chapters and patents, including reports in Cancer Research, Advanced Materials, Journal of Controlled Release, and Advanced Drug Delivery Reviews. Her work is highlighted on PNAS journal club, MaterialsToday news, and Women in Nanoscience blog. She has also edited a book entitled “Nanomaterials in Tissue Engineering: Fabrication and Applications” and a journal issue “Stem Cells: Microenvironment, Micro/Nanotechnology, and Application”, in Stem Cells International. Dr. Sant’s exemplary achievements in research have been recognized by prestigious fellowships: Ruth L. Kirschstein National Research Service Award (NIH, USA), Post-doctoral Fellowship (Le Fonds de Recherche du Quebec Nature et Technologies (FRQNT), Canada), Post-graduate Scholarship (Natural Sciences and Engineering Research Council of Canada (NSERC), Canada). She has also received several awards including “2016 CMBE-BMES Rising Star Early Career Faculty Award” “2013 CMBE-BMES Rising Star/Fellow Award”, “2010 Society For Biomaterials – STAR Award” to name a few. She serves as a reviewer on several NIH and NSF grant review panels. She also serves as an Associate Editor for IEEE Transactions on NanoBioScience, and editorial board member for Scientific Reports and In Silico Pharmacology.
This article is part of the 2017 CMBE Young Innovators special issue.

Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Xue, Y., St. Hilaire, C., Hortells, L. et al. Shape-Specific Nanoceria Mitigate Oxidative Stress-Induced Calcification in Primary Human Valvular Interstitial Cell Culture. Cel. Mol. Bioeng. 10, 483–500 (2017). https://doi.org/10.1007/s12195-017-0495-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12195-017-0495-6