Abstract
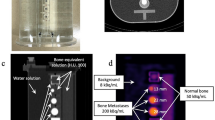
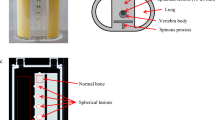
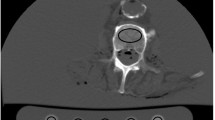
This study aimed to evaluate the effects of dipotassium hydrogen phosphate (K2HPO4) solution density on single-photon emission computed tomography (SPECT) image quality and quantification. We used a JSP phantom containing six cylinders filled with K2HPO4 solutions of varying densities. Computed tomography (CT) was performed, and CT values and linear attenuation coefficients were measured. Subsequently, SPECT images of an SIM2 bone phantom filled with 99mTc with/without K2HPO4 solution were acquired using a SPECT/CT camera. The full width at half maximum (FWHM), percentage coefficient of variation (%CV), recovery coefficient, and standardized uptake value (SUV) were evaluated to investigate the impact of the K2HPO4 solution density. The CT values and linear attenuation coefficients increased with the K2HPO4 solution density. The CT values for cancellous and cortical bones were reflected by K2HPO4 solution densities of 0.15–0.20 and 1.50–1.70 g/cm3, respectively. FWHM values were significantly lower with the K2HPO4 solution than those with water alone (18.0 ± 0.9 mm with water alone, 15.6 ± 0.2 mm with 0.15 g/cm3 K2HPO4, and 16.1 ± 0.3 mm with 1.49 g/cm3 K2HPO4). Although the %CVs showed no significant differences, the recovery coefficients obtained with water alone tended to be slightly lower than those obtained with the K2HPO4 solution. The SUV obtained using the standard density of the K2HPO4 solution differed from that obtained using the optimized density. In conclusion, SPECT image quality and quantification depends on the presence and concentration of the bone-equivalent solution. The optimal bone-equivalent solution density should be used to evaluate the bone image phantoms.








Similar content being viewed by others
References
Romer W, Nomayr A, Uder M, Bautz W, Torsten K. SPECTguided CT for evaluating foci of increased bone metabolism classified as indeterminate on SPECT in cancer patients. J Nucl Med. 2006;47(7):1102–6.
Even-Sapir E, Metser U, Mishani E, Lievshitz G, Lerman H, Leibovitch I. The detection of bone metastases in patients with high-risk prostate cancer: 99mTc-MDP planar bone scintigraphy, single- and multi-field-of-view SPECT, 18F-Fluoride PET, and 18F-fluoride PET/CT. J Nucl Med. 2006;47(2):287–97.
Abikhzer G, Gourevich K, Kagna O, Israel O, Frenkel A, Keidar Z. Whole-body bone SPECT in breast cancer patients: the future bone scan protocol? Nucl Med Commun. 2016;37(3):247–53.
Kaneta T, Ogawa M, Daisaki H, Nawata S, Yoshida K, Inoue T. SUV measurement of normal vertebrae using SPECT/CT with Tc-99m methylene diphosphonate. Am J Nucl Med Mol Imaging. 2016;6(5):262–8.
Nakahara T, Daisaki H, Yamamoto Y, Iimori T, Miyagawa K, Okamoto T, et al. Use of a digital phantom developed by QIBA for harmonizing SUVs obtained from the state-of-the-art SPECT/CT systems: a multicenter study. EJNMMI Res. 2017;7(1):53. https://doi.org/10.1186/s13550-017-0300-5.
Hishikawa M, Matsutomo N, Yamamoto T. Impact of reconstruction parameters on quantitative bone SPECT imaging: a novel thoracic spine phantom study. Hell J Nucl Med. 2019;22:140.
Shibutani T, Onoguchi M, Naoi Y, Yoneyama H, Konishi T, Tatami R, et al. The usefulness of SwiftScan technology for bone scintigraphy using a novel anthropomorphic phantom. Sci Rep. 2021;11(1):2644. https://doi.org/10.1038/s41598-021-82082-x.
Ichikawa H, Kawakami K, Onoguchi M, Shibutani T, Nagatake K, Hosoya T, et al. Automatic quantification package (Hone Graph) for phantom-based image quality assessment in bone SPECT: computerized automatic classification of detectability. Ann Nucl Med. 2021;35(8):937–46. https://doi.org/10.1007/s12149-021-01631-6.
Ichikawa H, Miyaji N, Onoguchi M, Shibutani T, Nagaki A, Kato T, et al. Feasibility of ultra-high-speed acquisition in xSPECT bone algorithm: a phantom study with advanced bone SPECT-specific phantom. Ann Nucl Med. 2022;36(2):183–90. https://doi.org/10.1007/s12149-021-01689-2.
Ichikawa H, Kato T, Shimada H, Watanabe Y, Miwa K, Matsutomo N, et al. Detectability of thoracic bone scintigraphy evaluated using a novel custom-designed phantom. The Jpn J Nucl Med Technol. 2017;37(3):229–38.
de Dreuille O, Strijckmans V, Ameida P, Loc’h C, Bendriem B. Bone equivalent liquid solution to assess accuracy of transmission measurements in SPECT and PET. IEEE Trans Nucl Sci. 1997;44(3):1186–90.
Fukami M, Matsutomo N, Yamamoto T. Optimization of number of iterations as a reconstruction parameter in bone SPECT imaging using a novel thoracic spine phantom. J Nucl Med Technol. 2021;49(2):143–9. https://doi.org/10.2967/jnmt.120.253534.
Iida H, Hori Y, Ishida K, Imabayashi E, Matsuda H, Takahashi M, et al. Threedimensional brain phantom containing bone and grey matter structures with a realistic head contour. Ann Nucl Med. 2013;27(1):25–36. https://doi.org/10.1007/s12149-012-0655-7.
Gittoes N. Osteoporosis: pathophysiology and clinical management. Clin Endocrinol (Oxf). 2003;59(6):826–7. https://doi.org/10.1046/j.1365-2265.2003.01904.x.
Lee S, Chung CK, Oh SH, Park SB. Correlation between bone mineral density measured by dual-energy X-ray absorptiometry and Hounsfield units measured by diagnostic CT in lumbar spine. J Korean Neurosurg Soc. 2013;54(5):384–9. https://doi.org/10.3340/jkns.2013.54.5.384.
Ichihara T, Motomura N, Ogawa K, Hasegawa H, Hashimoto J, Kubo A. Evaluation of SPET quantification of simultaneous emission and transmission imaging of the brain using a multidetector SPET system with the TEW scatter compensation method and fan-beam collimation. Eur J Nucl Med. 1996;23(10):1292–9. https://doi.org/10.1007/BF01367583.
Licho R, Glick SJ, Xia W, Pan TS, Penney BC, King MA. Attenuation compensation in 99mTc SPECT brain imaging: a comparison of the use of attenuation maps derived from transmission versus emission data in normal scans. J Nucl Med. 1999;40(3):456–63.
Cachovan M, Vija AH, Hornegger J, Kuwert T. Quantification of 99mTc-DPD concentration in the lumbar spine with SPECT/CT. EJNMMI Res. 2013;3(1):1–8. https://doi.org/10.1186/2191-219X-3-45.
Ito T, Tsuchikame H, Ichikawa H, Onoguchi M, Okuda K, Shibutani T, et al. Verification of phantom accuracy using a Monte Carlo simulation: bone scintigraphy chest phantom. Radiol Phys Technol. 2021;14(3):336–44. https://doi.org/10.1007/s12194-021-00631-5.
Hashizume K, Ichikawa Y, Tomita Y, Sakuma H. Impact of CT tube-voltage and bone density on the quantitative assessment of tracer uptake in Tc-99m bone SPECT/CT: a phantom study. Phys Med. 2022;104:18–22. https://doi.org/10.1016/j.ejmp.2022.10.022.
Okuda K, Fujii S, Sakimoto S. Impact of novel incorporation of CT-based segment mapping into a conjugated gradient algorithm on bone SPECT imaging: fundamental characteristics of a context-specific reconstruction method. Asia Ocean J Nucl Med Biol. 2019;7(1):49–57. https://doi.org/10.22038/AOJNMB.2018.31711.1219.
Rappoport V, Carney JP, Townsend DW. CT tube-voltage dependent attenuation correction scheme for PET/CT scanners. IEEE Symp Conf Rec Nucl Sci. 2004;2004(6):3853–7. https://doi.org/10.1109/NSSMIC.2004.1466720.
Bornefalk H. Synthetic hounsfield units from spectral CT data. Phys Med Biol. 2012;57(7):83–7. https://doi.org/10.1088/0031-9155/57/7/N83.
Onishi H, Motomura N, Fujino K, Natsume T, Haramoto Y. Quantitative performance of advanced resolution recovery strategies on SPECT images: evaluation with use of digital phantom models. Radiol Phys Technol. 2013;6(1):42–53. https://doi.org/10.1007/s12194-012-0168-z.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Ethical approval
This article does not contain any studies performed on human participants or animals.
Informed consent
There are no human subjects involved in this work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Matsutomo, N., Fukami, M. & Yamamoto, T. Impact of bone-equivalent solution density in a thoracic spine phantom on bone single-photon emission computed tomography image quality and quantification. Radiol Phys Technol 16, 195–202 (2023). https://doi.org/10.1007/s12194-023-00706-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12194-023-00706-5