Abstract
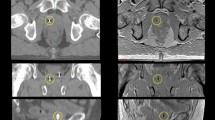
This study aimed to compare and assess the compatibility of the bone-structure-based manual and maximization of mutual information (MMI)-algorithm-based automatic image registration using megavoltage cone-beam computed tomography (MV-CBCT) images acquired with an imaging beam line. A total of 1163 MV-CBCT images from 30 prostate cancer patients were retrospectively analyzed. The differences between setup errors in three directions (left–right, LR; superior–inferior, SI; anterior–posterior, AP) of both registration methods were investigated. Pearson’s correlation coefficients (r) and Bland–Altman agreements were evaluated. Agreements were defined by a bias close to zero and 95% limits of agreement (LoA) less than ± 3 mm. The cumulative frequencies of the absolute differences between the two registration methods were calculated to assess the distributions of the setup error differences. There were significant differences (p < 0.001) in the setup errors between both registration methods. There were moderate (SI, r = 0.45) and strong positive correlation coefficients (LR, r = 0.74; AP, r = 0.72), whereas the 95% LoA (bias ± 1.96 × standard deviation of the setup error differences) were − 1.61 ± 4.29 mm (LR), − 0.41 ± 5.45 mm (SI), and 0.67 ± 4.29 mm (AP), revealing no agreements in all directions. The cumulative frequencies (%) of the cases with absolute setup error differences within 3 mm in each direction were 80.83% (LR), 81.86% (SI), and 90.71% (AP), with all directions having large proportions of > 3-mm differences. The MMI-algorithm-based automatic registration is not compatible with the bone-structure-based manual registration and should not be used alone for prostate cancer.






Similar content being viewed by others
References
Morin O, Gillis A, Chen J, Aubin M, Bucci MK, Roach M 3rd, Pouliot J. Megavoltage cone-beam CT: system description and clinical applications. Med Dosim. 2006;31(1):51–61. https://doi.org/10.1016/j.meddos.2005.12.009.
Pouliot J, Bani-Hashemi A, Chen J, Svatos M, Ghelmansarai F, Mitschke M, Aubin M, Xia P, Morin O, Bucci K, Roach M 3rd, Hernandez P, Zheng Z, Hristov D, Verhey L. Low-dose megavoltage cone-beam CT for radiation therapy. Int J Radiat Oncol Biol Phys. 2005;61(2):552–60. https://doi.org/10.1016/j.ijrobp.2004.10.011.
Gayou O, Parda DS, Johnson M, Miften M. Patient dose and image quality from mega-voltage cone beam computed tomography imaging. Med Phys. 2007;34(2):499–506. https://doi.org/10.1118/1.2428407.
Faddegon BA, Wu V, Pouliot J, Gangadharan B, Bani-Hashemi A. Low dose megavoltage cone beam computed tomography with an unflattened 4 MV beam from a carbon target. Med Phys. 2008;35(12):5777–86. https://doi.org/10.1118/1.3013571.
Breitbach EK, Maltz JS, Gangadharan B, Bani-Hashemi A, Anderson CM, Bhatia SK, Stiles J, Edwards DS, Flynn RT. Image quality improvement in megavoltage cone beam CT using an imaging beam line and a sintered pixelated array system. Med Phys. 2011;38(11):5969–79. https://doi.org/10.1118/1.3651470.
Dzierma Y, Nuesken FG, Licht NP, Ruebe C. Dosimetric properties and commissioning of cone-beam CT image beam line with a carbon target. Strahlenther Onkol. 2013;189(7):566–72. https://doi.org/10.1007/s00066-013-0330-5.
Maes F, Collignon A, Vandermeulen D, Marchal G, Suetens P. Multimodality image registration by maximization of mutual information. IEEE Trans Med Imaging. 1997;16(2):187–98. https://doi.org/10.1109/42.563664.
Pluim JP, Maintz JB, Viergever MA. Mutual-information-based registration of medical images: a survey. IEEE Trans Med Imaging. 2003;22(8):986–1004. https://doi.org/10.1109/TMI.2003.815867.
Grams MP, Brown LC, Brinkmann DH, Pafundi DH, Mundy DW, Garces YI, Park SS, Olivier KR, de los Santos LE. Analysis of automatic match results for cone-beam computed tomography localization of conventionally fractionated lung tumors. Pract Radiat Oncol. 2014;4(1):35–42. https://doi.org/10.1016/j.prro.2013.02.008.
Barber J, Sykes JR, Holloway L, Thwaites DI. Comparison of automatic image registration uncertainty for three IGRT systems using a male pelvis phantom. J Appl Clin Med Phys. 2016;17(5):283–92. https://doi.org/10.1120/jacmp.v17i5.6332.
Zucca S, Carau B, Solla I, Garibaldi E, Farace P, Lay G, Meleddu G, Gabriele P. Prostate image-guided radiotherapy by megavolt cone-beam CT. Strahlenther Onkol. 2011;187(8):473–8. https://doi.org/10.1007/s00066-011-2241-7.
Shi W, Li JG, Zlotecki RA, Yeung A, Newlin H, Palta J, Liu C, Chvetsov AV, Olivier K. Evaluation of kV cone-beam CT performance for prostate IGRT: a comparison of automatic grey-value alignment to implanted fiducial-marker alignment. Am J Clin Oncol. 2011;34(1):16–21. https://doi.org/10.1097/COC.0b013e3181d26b1a.
van Herk M. Errors and margins in radiotherapy. Semin Radiat Oncol. 2004;14(1):52–64. https://doi.org/10.1053/j.semradonc.2003.10.003.
Cubillos Mesías M, Boda-Heggemann J, Thoelking J, Lohr F, Wenz F, Wertz H. Quantification and assessment of interfraction setup errors based on cone beam CT and determination of safety margins for radiotherapy. PLoS One. 2016;11(3):e0150326. https://doi.org/10.1371/journal.pone.0150326.
Bland JM, Altman DG. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet. 1986;1(8476):307–10. https://doi.org/10.1016/S0140-6736(86)90837-8.
Thilmann C, Nill S, Tücking T, Höss A, Hesse B, Dietrich L, Bendl R, Rhein B, Häring P, Thieke C, Oelfke U, Debus J, Huber P. Correction of patient positioning errors based on in-line cone beam CTs: clinical implementation and first experiences. Radiat Oncol. 2006;1:16. https://doi.org/10.1186/1748-717X-1-16.
Wong JR, Gao Z, Uematsu M, Merrick S, Machernis NP, Chen T, Cheng CW. Interfractional prostate shifts: review of 1870 computed tomography (CT) scans obtained during image-guided radiotherapy using CT-on-rails for the treatment of prostate cancer. Int J Radiat Oncol Biol Phys. 2008;72(5):1396–401. https://doi.org/10.1016/j.ijrobp.2008.03.045.
Snir JA, Battista JJ, Bauman G, Yartsev S. Evaluation of inter-fraction prostate motion using kilovoltage cone beam computed tomography during radiotherapy. Clin Oncol (R Coll Radiol). 2011;23(9):625–31. https://doi.org/10.1016/j.clon.2011.03.007.
Huang K, Palma DA, Scott D, McGregor D, Gaede S, Yartsev S, Bauman G, Louie AV, Rodrigues G. Inter- and intrafraction uncertainty in prostate bed image-guided radiotherapy. Int J Radiat Oncol Biol Phys. 2012;84(2):402–7. https://doi.org/10.1016/j.ijrobp.2011.12.035.
Ost P, De Meerleer G, De Gersem W, Impens A, De Neve W. Analysis of prostate bed motion using daily cone-beam computed tomography during postprostatectomy radiotherapy. Int J Radiat Oncol Biol Phys. 2011;79(1):188–94. https://doi.org/10.1016/j.ijrobp.2009.10.029.
Qi XS, Wu S, Newman F, Li XA, Hu AY. Evaluation of interfraction patient setup errors for image-guided prostate and head-and-neck radiotherapy using kilovoltage cone beam and megavoltage fan beam computed tomography. J Radiother Pract. 2013;12(4):334–43. https://doi.org/10.1017/S1460396912000337.
Mayyas E, Chetty IJ, Chetvertkov M, Wen N, Neicu T, Nurushev T, Ren L, Lu M, Stricker H, Pradhan D, Movsas B, Elshaikh MA. Evaluation of multiple image-based modalities for image-guided radiation therapy (IGRT) of prostate carcinoma: a prospective study. Med Phys. 2013;40(4):041707. https://doi.org/10.1118/1.4794502.
Hurkmans CW, Remeijer P, Lebesque JV, Mijnheer BJ. Set-up verification using portal imaging; review of current clinical practice. Radiother Oncol. 2001;58(2):105–20. https://doi.org/10.1016/S0167-8140(00)00260-7.
Graf R, Boehmer D, Budach V, Wust P. Interfraction rotation of the prostate as evaluated by kilovoltage X-ray fiducial marker imaging in intensity-modulated radiotherapy of localized prostate cancer. Med Dosim. 2012;37(4):396–400. https://doi.org/10.1016/j.meddos.2012.02.006.
Boda-Heggemann J, Köhler F, Wertz H, Welzel G, Riesenacker N, Schäfer J, Lohr F, Wenz F. Fiducial-based quantification of prostate tilt using cone beam computer tomography (CBCT). Radiother Oncol. 2007;85(2):247–50. https://doi.org/10.1016/j.radonc.2007.09.008.
van Herk M, Remeijer P, Rasch C, Lebesque JV. The probability of correct target dosage: dose-population histograms for deriving treatment margins in radiotherapy. Int J Radiat Oncol Biol Phys. 2000;47(4):1121–35. https://doi.org/10.1016/S0360-3016(00)00518-6.
Gayou O. Influence of acquisition parameters on MV-CBCT image quality. J Appl Clin Med Phys. 2012;13(1):3638. https://doi.org/10.1120/jacmp.v13i1.3638.
Chen Z, Calhoun VD, Chang S. Compensating the intensity fall-off effect in cone-beam tomography by an empirical weight formula. Appl Opt. 2008;47(32):6033–9. https://doi.org/10.1364/AO.47.006033.
Beltran C, Lukose R, Gangadharan B, Bani-Hashemi A, Faddegon BA. Image quality and dosimetric property of an investigational imaging beam line MV-CBCT. J Appl Clin Med Phys. 2009;10(3):37–48. https://doi.org/10.1120/jacmp.v10i3.3023.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Statement of human/animal rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the IRB (approval number 15301, Osaka University Ethics Committee) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed.
Informed consent
For this retrospective study, passive informed consent (opt-out) was obtained from all individual participants.
About this article
Cite this article
Hashido, T., Nakasone, S., Fukao, M. et al. Comparison between manual and automatic image registration in image-guided radiation therapy using megavoltage cone-beam computed tomography with an imaging beam line for prostate cancer. Radiol Phys Technol 11, 392–405 (2018). https://doi.org/10.1007/s12194-018-0476-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12194-018-0476-z