Abstract
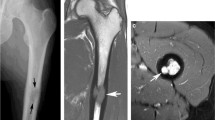
Spinal involvement of Langerhans cell histiocytosis (LCH) affects morbidity, but outcomes are not well understood. We analyzed long-term outcomes following uniform treatment at a single institution. Clinical characteristics and outcomes of spinal LCH patients were retrospectively analyzed. Height ratios were calculated using the anterior height of the involved vertebral body on magnetic resonance imaging (MRI) and the expected normal vertebral height. Twenty-two (22.4%) of 98 patients diagnosed with LCH had spinal involvement. The median age at diagnosis was 4.1 (range 0.6–12.3) years. Thirty-one spinal lesions were identified in 22 patients; the thoracic spine (n = 17) was most commonly affected. Eight lesions with minimal collapse, which appeared normal on plain radiography, were detected with MRI. All patients received vinblastine-based chemotherapy. Fourteen (70%) of 20 evaluable vertebral body collapses, including eight severe lesions, showed improvement in vertebral body height at a median follow-up of 6.0 (range 2.8–12.0) years. All traceable patients were alive without disease. Long-term follow-up of vertebral body collapse revealed vertebral height improvement in approximately 70% of spinal LCH patients, even in severe cases. MRI at diagnosis detected spinal lesions earlier with higher sensitivity than plain radiography.




Similar content being viewed by others
Abbreviations
- LCH:
-
Langerhans cell histiocytosis
- MRI:
-
Magnetic resonance imaging
References
Badalian-Very G, Vergilio JA, Fleming M, Rollins BJ. Pathogenesis of Langerhans cell histiocytosis. Annu Rev Pathol. 2013;8:1–20.
Berres ML, Merad M, Allen CE. Progress in understanding the pathogenesis of Langerhans cell histiocytosis: back to histiocytosis X? Br J Haematol. 2015;169(1):3–13.
Haupt R, Minkov M, Astigarraga I, Schafer E, Nanduri V, Jubran R, et al. Langerhans cell histiocytosis (LCH): guidelines for diagnosis, clinical work-up, and treatment for patients till the age of 18 years. Pediatr Blood Cancer. 2013;60(2):175–84.
Kim BE, Koh KN, Suh JK, Im HJ, Song JS, Lee JW, et al. Clinical features and treatment outcomes of Langerhans cell histiocytosis: a nationwide survey from Korea histiocytosis working party. J Pediatr Hematol Oncol. 2014;36(2):125–33.
Howarth DM, Gilchrist GS, Mullan BP, Wiseman GA, Edmonson JH, Schomberg PJ. Langerhans cell histiocytosis: diagnosis, natural history, management, and outcome. Cancer. 1999;85(10):2278–90.
Arkader A, Glotzbecker M, Hosalkar HS, Dormans JP. Primary musculoskeletal Langerhans cell histiocytosis in children: an analysis for a 3-decade period. J Pediatr Orthop. 2009;29(2):201–7.
Bollini G, Jouve JL, Gentet JC, Jacquemier M, Bouyala JM. Bone lesions in histiocytosis X. J Pediatr Orthop. 1991;11(4):469–77.
Ghanem I, Tolo VT, D’Ambra P, Malogalowkin MH. Langerhans cell histiocytosis of bone in children and adolescents. J Pediatr Orthop. 2003;23(1):124–30.
Kumar A. Eosinophilic granuloma of the spine with neurological deficit. Orthopedics. 1990;13(11):1310–2.
Green NE, Robertson WW Jr, Kilroy AW. Eosinophilic granuloma of the spine with associated neural deficit. Report of three cases. J Bone Jt Surg Am. 1980;62(7):1198–202.
Garg S, Mehta S, Dormans JP. Langerhans cell histiocytosis of the spine in children. Long-term follow-up. J Bone Jt Surg Am. 2004;86-A(8):1740–50.
Yeom JS, Lee CK, Shin HY, Lee CS, Han CS, Chang H. Langerhans’ cell histiocytosis of the spine. Analysis of twenty-three cases. Spine (Phila Pa 1976). 1999;24(16):1740–9.
Raab P, Hohmann F, Kuhl J, Krauspe R. Vertebral remodeling in eosinophilic granuloma of the spine. A long-term follow-up. Spine (Phila Pa 1976). 1998;23(12):1351–4.
Goo HW, Yang DH, Ra YS, Song JS, Im HJ, Seo JJ, et al. Whole-body MRI of Langerhans cell histiocytosis: comparison with radiography and bone scintigraphy. Pediatr Radiol. 2006;36(10):1019–31.
Gadner H, Grois N, Arico M, Broadbent V, Ceci A, Jakobson A, et al. A randomized trial of treatment for multisystem Langerhans’ cell histiocytosis. J Pediatr. 2001;138(5):728–34.
Gadner H, Grois N, Potschger U, Minkov M, Arico M, Braier J, et al. Improved outcome in multisystem Langerhans cell histiocytosis is associated with therapy intensification. Blood. 2008;111(5):2556–62.
Gadner H, Minkov M, Grois N, Potschger U, Thiem E, Arico M, et al. Therapy prolongation improves outcome in multisystem Langerhans cell histiocytosis. Blood. 2013;121(25):5006–14.
Weitzman S, Braier J, Donadieu J, Egeler RM, Grois N, Ladisch S, et al. 2′-Chlorodeoxyadenosine (2-CdA) as salvage therapy for Langerhans cell histiocytosis (LCH). Results of the LCH-S-98 protocol of the histiocyte society. Pediatr Blood Cancer. 2009;53(7):1271–6.
Morimoto A, Ikushima S, Kinugawa N, Ishii E, Kohdera U, Sako M, et al. Improved outcome in the treatment of pediatric multifocal Langerhans cell histiocytosis: results from the Japan Langerhans cell histiocytosis study group-96 protocol study. Cancer. 2006;107(3):613–9.
Morimoto A, Shioda Y, Imamura T, Kudo K, Kawaguchi H, Sakashita K, et al. Intensified and prolonged therapy comprising cytarabine, vincristine and prednisolone improves outcome in patients with multisystem Langerhans cell histiocytosis: results of the Japan Langerhans cell histiocytosis study group-02 protocol study. Int J Hematol. 2016;104(1):99–109.
Nesbit ME, Kieffer S, D’Angio GJ. Reconstitution of vertebral height in histiocytosis X: a long-term follow-up. J Bone Jt Surg Am. 1969;51(7):1360–8.
Floman Y, Bar-On E, Mosheiff R, Mirovsky Y, Robin GC, Ramu N. Eosinophilic granuloma of the spine. J Pediatr Orthop B. 1997;6(4):260–5.
Tsai PY, Tzeng WS. Images in clinical medicine. Vertebra plana with spontaneous healing. N Engl J Med. 2012;366(19):e30.
Brown CW, Jarvis JG, Letts M, Carpenter B. Treatment and outcome of vertebral Langerhans cell histiocytosis at the Children’s Hospital of Eastern Ontario. Can J Surg. 2005;48(3):230–6.
Osenbach RK, Youngblood LA, Menezes AH. Atlanto-axial instability secondary to solitary eosinophilic granuloma of C2 in a 12-year-old girl. J Spinal Disord. 1990;3(4):408–12.
Dickinson LD, Farhat SM. Eosinophilic granuloma of the cervical spine. A case report and review of the literature. Surg Neurol. 1991;35(1):57–63.
Poulsen JO, Thommesen P. An unusual case of histiocytosis X in the spine. Acta Orthop Scand. 1976;47(1):59–62.
Meyer JS, De Camargo B. The role of radiology in the diagnosis and follow-up of Langerhans cell histiocytosis. Hematol Oncol Clin North Am. 1998;12(2):307–26.
Villas C, Martinez-Peric R, Barrios RH, Beguiristain JL. Eosinophilic granuloma of the spine with and without vertebra plana: long-term follow-up of six cases. J Spinal Disord. 1993;6(3):260–8.
Kotecha R, Venkatramani R, Jubran RF, Arkader A, Olch AJ, Wong K. Clinical outcomes of radiation therapy in the management of Langerhans cell histiocytosis. Am J Clin Oncol. 2014;37(6):592–6.
Huang WD, Yang XH, Wu ZP, Huang Q, Xiao JR, Yang MS, et al. Langerhans cell histiocytosis of spine: a comparative study of clinical, imaging features, and diagnosis in children, adolescents, and adults. Spine J. 2013;13(9):1108–17.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was supported by the Research Program funded by the Korea Centers for Disease Control and Prevention (2016E6300200).
Conflict of interest
The authors declare that they have no competing interest.
About this article
Cite this article
Lee, S.W., Kim, H., Suh, J.K. et al. Long-term clinical outcome of spinal Langerhans cell histiocytosis in children. Int J Hematol 106, 441–449 (2017). https://doi.org/10.1007/s12185-017-2252-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12185-017-2252-y