Abstract
Mantle cell lymphoma is a hematologic malignancy characterized by poor therapeutic outcomes. Immunomodulatory drugs are a focus of attention in this disease, especially for the elderly and frail patients not able to tolerate the typically intensive therapeutic approaches used in fitter patients. We here present the case of refractory mantle cell lymphoma of the elderly that achieved complete remission following the use of single-agent lenalidomide, and a second complete response to the same regimen on relapse 5 years later.
Similar content being viewed by others
Accounting for less than 10 % of non-Hodgkin lymphomas, mantle cell lymphoma (MCL) is a rare type of hematologic malignancy with currently unsatisfactory treatment and dismal prognosis. It is characterized by a monomorphic proliferation of typically CD5 and cyclin D1-positive B lymphocytes, with a usually diffuse, rarely nodular or follicular growth pattern. Although indolent in a small percentage of patients, MCL usually has a rather aggressive clinical course. Its evolution is characterized by repeated relapses, and currently, the median survival ranges between 3 and 7 years [1, 2]. High-dose therapy is usually administered to fit patients, but for the elderly, current treatment is less well standardized and therapeutic options are limited. We here present the case of an elder refractory MCL patient achieving complete remission with single-agent lenalidomide, and a second complete response with the same agent at relapse, 5 years later.
A 74-year-old woman was diagnosed with Ann Arbor stage IV mantle cell lymphoma. She presented with fatigue and had grade I splenomegaly with no lymph node enlargement. Blood count showed lymphocytosis, with abnormal circulating B lymphocytes, of typical MCL phenotype. Translocation (11;14) (q11;q32), and overexpression of cyclin D1 were present. The IPI score was 3. The patient progressed during initial treatment with rituximab plus vincristine, doxorubicin and dexamethasone, associated with chlorambucil. She then showed a rapid response to continuous single-agent lenalidomide 25 mg, with complete remission achieved in 5 weeks. Tolerance was good with no significant clinical side effects, but lenalidomide dose was later adjusted to 20, then 15 mg daily, due to cytopenias, and the treatment was continued for a total of 24 months. Concomitant prophylactic aspirin was administered. The case was then reported in a letter to Annals of Hematology [3]. Five years later, the patient relapsed with enlarged cervical lymph nodes. The patient had low platelet count of 120 Giga/L, normal hemoglobin and leukocyte count with 1.3 Giga/L lymphocytes, of which 74 % CD5 CD19 positive by immunophenotyping. Bone marrow examination confirmed the presence of a 23 % infiltration with B lymphocytes of which 79 % with the same abnormal phenotype present at diagnosis, expressing CD5, CD19, CD20, cyclin D1, and strong surface immunoglobulin. Kidney and liver function tests were normal, and lactate dehydrogenases were slightly elevated, at 525 UI/L. A PET–CT scan showed supra- and sub-diaphragmatic involvement (Fig. 1). MIPI score was calculated at 7.1, ranking as high risk.
Continuous treatment with single-agent lenalidomide 15 mg daily was reinitiated. We chose to use a reduced dose due to the patient’s age and previous history of cytopenias associated with the 25-mg dose. As for the first course of lenalidomide, dexamethasone was omitted due to advanced age, and aspirin was administered as antiplatelet prophylaxis. Three months later, the lymphadenopathy disappeared. Peripheral blood cytology and immunophenotype analysis demonstrated the disappearance of lymphoma cells. The patient refused a bone marrow aspiration to document medullary remission, and a PET–CT scan confirmed the complete metabolic remission (Fig. 1). No side effects were noted. The patient presently continues her treatment, with a 3-month evaluation schedule.
A rare type of lymphoma, MCL, is characterized by a proliferation of CD5-positive, antigen–naive, pre-germinal center B-cells. If the first line of treatment is reasonably well established [4, 5], for the relapsed/refractory patients, especially in the elderly, there is no standard of care. Several new agents, such as bortezomib, temsirolimus, lenalidomide, and, recently, ibrutinib, showed efficacy in this type of patients [6, 7].
Initially intended for the treatment of myeloma, as an improvement to thalidomide, lenalidomide is an immunomodulatory drug that has later proved efficacy not only in other lymphoproliferative diseases, but also in myelodysplastic syndromes [8].
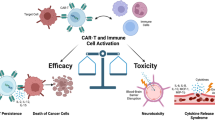
The efficacy of lenalidomide in lymphoid malignancies is attributed to T-cell immune synapse enhancement, NK and T-cell effector augmentation, and antiproliferative and antiangiogenic effects [9]. Lenalidomide, either single or in combination with dexamethasone, was proved to be effective for the treatment of refractory/relapsed MCL, at a 20-to-25-mg daily dose on a 21 of 28 days schedule. Median time to progression reported was 3.9–14.6 months [10–12].
In our patient, lenalidomide allowed for the rapid achievement of a long-lasting complete remission. At relapse, 5 years later, the tumor showed preserved sensitivity to the same drug schedule. Our case highlights the efficacy of lenalidomide in MCL and shows that resistance to the drug may not develop.
References
Swerdlow SH. WHO classification of tumours of haematopoietic and lymphoid tissues. 4th ed. Lyon: WHO Press; 2008.
Cheah CY, Seymour JF, Wang ML. Mantle cell lymphoma. J Clin Oncol. 2016;34:1256–69.
Tempescul A, Ianotto JC, Morel F, Marion V, De Braekeleer M, Berthou C. Lenalidomide, as a single agent, induces complete remission in a refractory mantle cell lymphoma. Ann Hematol. 2009;88(9):921–2.
Vose JM. Mantle cell lymphoma: 2015 update on diagnosis, risk-stratification, and clinical management. Am J Hematol. 2015;90(8):739–45.
Witzens-Harig M, Hess G, Atta J, Zaiss M, Lenz G, Scholz C, et al. Current treatment of mantle cell lymphoma: results of a national survey and consensus meeting. Ann Hematol. 2012;91(11):1765–72.
Mussetti A, Kumar A, Dahi PB, Perales MA, Sauter CS. Lifting the mantle: unveiling new treatment approaches in relapsed or refractory mantle cell lymphoma. Blood Rev. 2015;29(3):143–52.
Avivi I, Goy A. Refining the mantle cell lymphoma paradigm: impact of novel therapies on current practice. Clin Cancer Res. 2015;21(17):3853–61.
Weisel K, Kanz L. Lenalidomide. Recent Results Cancer Res. 2014;201:347–57.
Kritharis A, Coyle M, Sharma J, Evens AM. Lenalidomide in non-Hodgkin lymphoma: biological perspectives and therapeutic opportunities. Blood. 2015;125(16):2471–6.
Habermann TM, Lossos IS, Justice G, Vose JM, Wiernik PH, McBride K, et al. Lenalidomide oral monotherapy produces a high response rate in patients with relapsed or refractory mantle cell lymphoma. Br J Haematol. 2009;145(3):344–9.
Witzig TE, Vose JM, Zinzani PL, Reeder CB, Buckstein R, Polikoff JA, et al. An international phase II trial of single-agent lenalidomide for relapsed or refractory aggressive B-cell non-Hodgkin’s lymphoma. Ann Oncol. 2011;22(7):1622–7.
Goy A, Sinha R, Williams ME, Kalayoglu Besisik S, Drach J, Ramchandren R, et al. Single-agent lenalidomide in patients with mantle-cell lymphoma who relapsed or progressed after or were refractory to bortezomib: phase II MCL-001 (EMERGE) study. J Clin Oncol. 2013;31(29):3688–95.
Acknowledgments
Drs. Bagacean, Bocsan and Zdrenghea are supported by a grant of the Romanian National Authority for Scientific Research and Innovation, CNCS-UEFISCDI, Project Number PN-II-RU-TE-2014-4-2074.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Informed consent
The patient gave her informed consent for the usage of clinical data for scientific purposes.
About this article
Cite this article
Tempescul, A., Ianotto, JC., Bagacean, C. et al. Late relapsing mantle cell lymphoma showing preserved sensitivity to single-agent lenalidomide. Int J Hematol 104, 400–402 (2016). https://doi.org/10.1007/s12185-016-2020-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12185-016-2020-4