Abstract
Purpose of Review
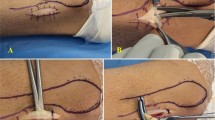
To review the current literature on clinical outcomes following open tibial inlay posterior cruciate ligament (PCL) reconstruction and provide the reader with a detailed description of the author’s preferred surgical technique.
Recent Findings
Despite earlier biomechanical studies which demonstrated superiority of the PCL inlay technique when compared to transtibial techniques, recent longitudinal cohort studies have shown no significant differences in clinical or functional outcomes at 10-year follow-up. Furthermore, no significant clinical differences have been shown between graft types used and/or single- versus double-bundle reconstruction methods.
Summary
The optimal treatment for the PCL-deficient knee remains unclear. Open tibial inlay PCL reconstruction is safe, reproducible, and avoids the “killer turn” that may potentially lead to graft weakening and failure seen in transtibial reconstruction methods. No significant differences in subjective outcomes or clinical laxity have been shown between single-bundle versus double-bundle reconstruction methods.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Miyasaka KC, Daniel DM, Stone ML. The incidence of knee ligament injuries in the general population. Am J Knee Surg. 1991;4:3–8.
• Markolf KL, Zemanovic JR, McAllister DR. Cyclic loading of posterior cruciate ligament replacements fixed with tibial tunnel and tibial inlay methods. J Bone Joint Surg Am. 2002;84A(4):518–24. Classic biomechanical study showing increased graft thinning and stretch out following cyclic loading in fixed transtibial PCL reconstructions in comparison to fixed tibial inlay methods.
Jakob RP, Ruegsegger M. Therapy of posterior and posterolateral knee instability. Orthopade. 1993;22(6):405–13.
Berg EE. Posterior cruciate ligament tibial inlay reconstruction. Arthroscopy. 1995;11(1):69–76.
Shelbourne KD, Clark M, Gray T. Minimum 10-year follow-up of patients after an acute, isolated posterior cruciate ligament injury treated non-operatively. Am J Sports Med. 2013;41(7):1526–33.
Maruyama Y, Shitoto K, Baba T, et al. Evaluation of the clinical results of posterior cruciate ligament reconstruction—a comparison between the use of the bone tendon bone and semitendinosus and gracilis tendons. Sports Medicine, Arthroscopy, Rehabilitation Therapy & Technology. 2012;4(30):1–5.
Ahn JH, Yoo JC, Wang JH. Posterior cruciate ligament reconstruction: double-loop hamstring tendon autograft versus Achilles tendon allograft-clinical results of a minimum 2-year follow-up. Arthroscopy. 2005;21(8):965–9.
Burks RT, Schaffer JT. A simplified approach to the tibial attachment of the posterior cruciate ligament. Clin Orthop. 1990;(254):216–219.
Petrigliano FA, Montgomery SR, Johnson JS, McAllister DR. Posterior cruciate ligament injuries. In: Miller MD, Thompson SK, editors. DeLee & Drez’s Orthopaedic Sports Medicine 4th Edition. Philadelphia: Saunders; 2015.
Cooper DE, Stewart D. Posterior cruciate ligament reconstruction using single-bundle patella tendon graft with tibial inlay fixation: 2- to 10-year follow-up. Am J Sports Med. 2004;32(2):346–60.
Noyes FR, Barber-Westin S. Posterior cruciate ligament replacement with a two-strand quadriceps tendon-patellar bone autograft and a tibial inlay technique. J Bone Joint Surg Am. 2005;87(6):1241–52.
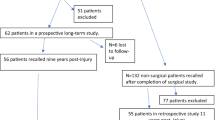
• Song EK, Park HW, Ahn YS, et al. Transtibial versus tibial inlay techniques for posterior cruciate ligament reconstruction. Am J Sports Med. 2014;42(12):2964–71. Retrospective cohort study showing no clinically significant difference in functional outcome measures or radiographic evidence of arthritis between patients undergoing transtibial versus inlay PCL reconstruction at an average of 10 years follow-up.
• Shin YS, Kim HY, Lee DH. No clinically important difference in knee scores or instability between transtibial and inlay techniques for PCL reconstruction: a systematic review. Clin Orthop Relat Res. 2017;(475):1239–48. Recent review article showing no clinically significant differences in terms of stability or functional outcome scores in patients treated with transtibial or inlay PCL reconstruction techniques.
Papalia R, Osti L, Del Buono A, Denaro V, Maffulli N. Tibial inlay for posterior cruciate ligament reconstruction: a systematic review. Knee. 2010 Aug;17(4):264–9. https://doi.org/10.1016/j.knee.2010.02.006.
Seo SS, Seo JH, Kim DH, Park BY. Compression of the popliteal artery after posterior cruciate ligament reconstruction using the tibial inlay technique. Knee Surg Relat Res. 2015;27(4):274–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on PCL Update
Rights and permissions
About this article
Cite this article
Vellios, E.E., Jones, K.J. & McAllister, D.R. Open Tibial Inlay PCL Reconstruction: Surgical Technique and Clinical Outcomes. Curr Rev Musculoskelet Med 11, 316–319 (2018). https://doi.org/10.1007/s12178-018-9490-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12178-018-9490-3