Abstract
Background
Recent research has led to debate over the benefit of planning quit attempts, suggesting that attempts implemented spontaneously may be more effective. The roles of planning and spontaneity require prospective examination.
Purpose
The purpose of this study is to test the benefit of encouraging smokers using an online program to quit as soon as possible (Rapid Implementation arm) and of structured planning advice incorporating implementation intentions (Structured Planning arm).
Methods
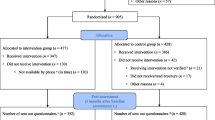
Randomized controlled trial with 1601 cases in the Rapid Implementation arm and an additional 964 in the Structured Planning arm; 2565 in total.
Results
There was no effect of Rapid Implementation, but Structured Planning significantly increased 6-month sustained abstinence (14.6 vs 10.2 %; p = 0.001). There was significantly less relapse after 1 week in the structured planning group (61.0 vs 71.2 %, p = 0.001).
Conclusions
A structured planning intervention delivered online can reduce relapse to smoking. Smokers should be encouraged to form implementation intentions and do most of their planning for relapse prevention after they have quit.


Similar content being viewed by others
References
Ajzen I. The theory of planned behavior. Organ Behav Hum Decis Process. 1991; 50: 179-211.
Fiore M, Jaen C, Baker T, et al. Treating tobacco use and dependence: 2008 update. US: US Department of Health and Human Services 2008, Public Health Service.
Prochaska J, DiClemente C, Norcross J. In search of how people change. Applications to addictive behaviors. Am Psychol. 1992; 47: 1102-1114.
Raw M, McNeill A, West R. Smoking cessation guidelines for health professionals. A guide to effective smoking cessation interventions for the health care system. Health Education Authority. Thorax. 1998; 53(Suppl 5): S1-S19.
Borland R. Understanding hard to maintain behavior change: A dual-process approach. Oxford: Wiley-Blackwell, Addiction Press; 2014.
West R, Brown J. Theory of addiction (2nd Edition). Oxford: Wiley-Blackwell, Addiction Press; 2013.
Stead LF, Lancaster T. Group behavior therapy programmes for smoking cessation. Cochrane Database Syst Rev. 2005; 2: CD001007.
Ferguson S, Shiffman S, Gitchell J, Sembower M, West R. Unplanned quit attempts - results from a U.S. sample of smokers and ex-smokers. Nicotine Tob Res. 2009; 11: 827-832.
Larabie L. To what extent do smokers plan quit attempts? Tob Control. 2005; 14: 425-428.
Sendzik T, Mcdonald PW, Brown KS, Hammond D, Ferrence R. Planned quit attempts among Ontario smokers: Impact on abstinence. Addiction. 2011; 106: 2005-2013.
West R, Sohal T. "Catastrophic" pathways to smoking cessation: Findings from national survey. BMJ. 2006; 332: 458-460.
Cooper J, Borland R, Yong H, et al. To what extent do smokers make spontaneous quit attempts and what are the implications for smoking cessation maintenance? Findings from the International Tobacco Control Four-Country survey. Nicotine Tob Res. 2010; 12(Suppl 1): S51-S57.
Murray R, Lewis S, Coleman T, Britton J, McNeill A. Unplanned attempts to quit smoking: Missed opportunities for health promotion? Addiction. 2009; 104: 1901-1909.
Borland R, Balmford J, Swift E. Effect of timing of initiation and planning on smoking cessation outcomes: Study protocol for a randomized controlled trial. BMC Public Health. 2013; 13: 235.
Balmford J, Borland R, Burney S. The influence of having a quit date on the prediction of smoking cessation outcome. Health Educ Res. 2010; 25: 698-706.
Cobb CO, Niaura RS, Donaldson EA, Graham AL. Quit now? Quit soon? Quit when you’re ready? Insights about target quit dates for smoking cessation from an online quit date tool. J Med Internet Res. 2014; 16: e55.
Hughes JR, Callas PW. Is delaying a quit attempt associated with less success? Nicotine Tob Res. 2011; 12: 1228-1232.
Hughes JR, Russ C, Messig MA. Association of deferring a quit attempt with smoking cessation success: A secondary analysis. J Subst Abuse Treat. 2014; 46: 264-267.
Hughes JR, Solomon LJ, Naud S, Fingar JR, Helzer JE, Callas PW. Natural history of attempts to stop smoking. Nicotine Tob Res. 2014; 16: 1190-1198.
Fong GT, Cummings KM, Borland R, et al. The conceptual framework of the International Tobacco Control (ITC) policy evaluation project. Tob Control. 2006; 15(Suppl 3): 3-11.
Balmford J, Borland R, Swift E. Reported planning before and just after quitting and quit success: Retrospective data from the ITC 4-Country survey. Psychol Addict Behav. 2014; 28: 899-906.
Gollwitzer PM. Implementation intentions: Strong effects from simple plans. Am Psychol. 1999; 54: 493-503.
Gollwitzer PM, Sheeran P. Implementation intentions and goal achievement: A meta-analysis of effects and processes. Adv Exp Soc Psychol. 2006; 38: 69-119.
Achtziger A, Gollwitzer PM, Sheeran P. Implementation intentions and shielding goal striving from unwanted thoughts and feelings. Personal Soc Psychol Bul. 2008; 34: 381-393.
Armitage CJ. A volitional help sheet to encourage smoking cessation: A randomized exploratory trial. Health Psychol. 2008; 27: 557-566.
Armitage CJ, Arden MA. How useful are the stages of change for targeting interventions? Randomized test of a brief intervention to reduce smoking. Health Psychol. 2008; 27: 789-798.
Borland R, Balmford J, Benda P. Population-level effects of automated cessation help programs: A randomized controlled trial. Addiction. 2013; 108: 618-628.
Borland R, Balmford J, Hunt D. The effectiveness of personally tailored computer-generated advice letters for smoking cessation. Addiction. 2004; 99: 369-377.
Borland R, Yong H, O’Connor R, Hyland A, Thompson M. The reliability and predictive validity of the Heaviness of Smoking Index and its two components: Findings from the International Tobacco Control Four-Country study. Nicotine Tob Res. 2010; 12(Suppl 1): S45-S50.
Hagger MS, Luszczynska A. Implementation intention and action planning interventions in health contexts: State of the research and proposals for the way forward. Appl Psychol Health Well Being. 2014; 6: 1-47.
Hajek P, Stead LF, West R, Jarvis M, Hartmann-Boyce J, Lancaster T. Relapse prevention interventions for smoking cessation (review). Cochrane Database Syst Rev. 2013; 8: CD003999.
Borland R, Yong HH, Balmford J, et al. Motivational factors predict quit attempts but not maintenance of smoking cessation: Findings from the International Tobacco Control Four country project. Nicotine Tob Res. 2010; 12: S4-S11.
Partos TR, Borland R, Yong HH, Hyland A, Cummings KM. The quitting rollercoaster: how recent quitting history affects future cessation (data from the International Tobacco Control 4-country cohort study). Nicotine Tob Res. 2013; 15: 1578-1587.
SRNT Subcommittee on Biochemical Verification. Biochemical verification of tobacco use and cessation. Nicotine Tob Res. 2002; 4: 149–159.
Funding
This study was funded by the National Health and Medical Research Council (grant number 1009767).
Authors’ Statement of Conflict of Interest
Authors Borland, Balmford, and Swift declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Clinical trial registrationAustralian and New Zealand Clinical Trial Registration No.: ACTRN12612000613808
About this article
Cite this article
Borland, R., Balmford, J. & Swift, E. Effects of Encouraging Rapid Implementation and/or Structured Planning of Quit Attempts on Smoking Cessation Outcomes: a Randomized Controlled Trial. ann. behav. med. 49, 732–742 (2015). https://doi.org/10.1007/s12160-015-9706-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12160-015-9706-3