Abstract
Objective
Vesicoureteral reflux (VUR) is a major risk factor for recurrent symptomatic urinary tract infection (UTI) in pediatric patients. In addition, dimercaptosuccinic acid renal scintigraphy (DMSA) is an important diagnostic modality of VUR. However, the value of DMSA for predicting recurrent pediatric UTI has not been studied. Therefore, we aimed to develop visual scoring system (VSS) with DMSA to predict the risk of recurrence of symptomatic urinary tract infection in pediatric patient under the age of 24 months.
Methods
Pediatric UTI patients who visited our tertiary hospital emergency department and underwent DMSA for initial work-up from January 2006 to December 2014 were reviewed retrospectively. We developed a VSS with Tc-99m DMSA renal scintigraphy. We compared sensitivity and specificity between VSS with DMSA and other variables in predicting recurrent symptomatic UTI. Laboratory indices for systemic inflammation, abnormal finding on ultrasonography, VUR on voiding cystourethrogram (VCUG), and the VSS with DMSA were considered as variables. In addition, we used Kaplan–Meier estimator analyses and Cox proportional regression analyses to evaluate the predictive value of each variable for the recurrence of symptomatic UTI.
Results
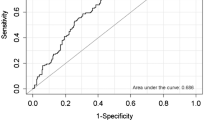
A total of 338 patients were enrolled. During the follow-up period, 42 patients (12.4%) had UTI recurrence. Visual scoring with DMSA resulted in 69.1% sensitivity and 79.4% specificity with an optimal cut-off value of score 2 (AUC = 0.790, p < 0.001). Significant predictive factors associated with recurrent symptomatic UTI were CRP ≥ 67.0 mg/L, VUR on VCUG and VSS with DMSA ≥ score 2. On multivariate analysis, the visual score with DMSA was the only independent prognostic factor for recurrent symptomatic UTI (p < 0.001; adjusted hazard ratio = 7.522; 95% CI = 2.799–20.224).
Conclusion
High scores in VSS with DMSA were associated with frequent recurrence and short recurrence periods in pediatric UTI patients. VSS with DMSA can stratify risk of recurrence in pediatric UTI patients.



Similar content being viewed by others
References
Rushton HG. Urinary tract infections in children: epidemiology, evaluation, and management. Pediatr Clin North Am. 1997;44:1133–69.
Ammenti A, Cataldi L, Chimenz R, Fanos V, La Manna A, Marra G, et al. Febrile urinary tract infections in young children: recommendations for the diagnosis, treatment and follow-up. Acta Paediatr. 2012;101:451–7.
Representatives L. Practice parameter: the diagnosis, treatment, and evaluation of the initial urinary tract infection in febrile infants and young children. American Academy of Pediatrics. Committee on Quality Improvement. Subcommittee on Urinary Tract Infection. Pediatrics. 1999;103:843–52.
Merrick MV, Notghi A, Chalmers N, Wilkinson AG, Uttley WS. Long-term follow up to determine the prognostic value of imaging after urinary tract infections. Part 1: Reflux. Arch Dis Child. 1995;72:388–92.
Copp HL, Shapiro DJ, Hersh AL. National ambulatory antibiotic prescribing patterns for pediatric urinary tract infection, 1998–2007. Pediatrics. 2011;127:1027–33.
van der Starre WE, Zunder SM, Vollaard AM, van Nieuwkoop C, Stalenhoef JE, Delfos NM, et al. Prognostic value of pro-adrenomedullin, procalcitonin and C-reactive protein in predicting outcome of febrile urinary tract infection. Clin Microbiol Infect. 2014;20:1048–54.
Han SY, Lee IR, Park SJ, Kim JH, Shin JI. Usefulness of neutrophil–lymphocyte ratio in young children with febrile urinary tract infection. Korean J Pediatr. 2016;59:139–44.
Hamiel U, Bahat H, Kozer E, Hamiel Y, Ziv-Baran T, Goldman M. Diagnostic markers of acute infections in infants aged 1 week to 3 months: a retrospective cohort study. BMJ Open. 2018;8:e018092.
Turkmen K, Erdur FM, Ozcicek F, Ozcicek A, Akbas EM, Ozbicer A, et al. Platelet-to-lymphocyte ratio better predicts inflammation than neutrophil-to-lymphocyte ratio in end-stage renal disease patients. Hemodial Int. 2013;17:391–6.
Ki HC, Kim S-O, Yoo DH, Hwang IS, Hwang EC, Oh KJ, et al. Abnormal dimercaptosuccinic acid scan may be related to persistence of vesicoureteral reflux in children with febrile urinary tract infection. Korean J Urol. 2012;53:716–20.
Lee JH, Kim MK, Park SE. Is a routine voiding cystourethrogram necessary in children after the first febrile urinary tract infection? Acta Paediatr. 2012;101:e105–9.
Lassmann M, Treves ST, Group ESPDHW. Paediatric radiopharmaceutical administration: harmonization of the 2007 EANM paediatric dosage card (version 1.5. 2008) and the 2010 North American consensus guidelines. Eur J Nucl Med Mol Imaging. 2014;41:1036–41.
Jakobsson B, Jacobson S, Hjälmås K. Vesico-ureteric reflux and other risk factors for renal damage: identification of high-and low-risk children. Acta Paediatr. 1999;88:31–9.
Smellie J, Poulton A, Prescod N. Retrospective study of children with renal scarring associated with reflux and urinary infection. BMJ. 1994;308:1193–6.
Camacho V, Estorch M, Fraga G, Mena E, Fuertes J, Hernández MA, et al. DMSA study performed during febrile urinary tract infection: a predictor of patient outcome? Eur J Nucl Med Mol Imaging. 2004;31:862–6.
Biggi A, Dardanelli L, Cussino P, Pomero G, Noello C, Sernia O, et al. Prognostic value of the acute DMSA in children with first urinary tract infection. Pediatr Nephrol. 2001;16:800–4.
Roberts KB. Urinary tract infection: clinical practice guideline for the diagnosis and management of the initial UTI in febrile infants and children 2 to 24 months. Pediatrics. 2011;128:595–610.
Mori R, Lakhanpaul M, Verrier-Jones K. Diagnosis and management of urinary tract infection in children: summary of NICE guidance. BMJ. 2007;335:395–7.
Lee SJ. Clinical guideline for childhood urinary tract infection (second revision). Child Kidney Dis. 2015;19:56–64.
Risdon RA, Godley ML, Parkhouse HF, Gordon I, Ransley PG. Renal pathology and the 99mTc-DMSA image during the evolution of the early pyelonephritic scar: an experimental study. J Urol. 1994;151:767–73.
Zahorec R. Ratio of neutrophil to lymphocyte counts-rapid and simple parameter of systemic inflammation and stress in critically ill. Bratisl Lek Listy. 2001;102:5–14.
de Jager CPC, van Wijk PTL, Mathoera RB, de Jongh-Leuvenink J, van der Poll T, Wever PC. Lymphocytopenia and neutrophil-lymphocyte count ratio predict bacteremia better than conventional infection markers in an emergency care unit. Crit Care. 2010;14:R192.
Balta S, Ozturk C. The platelet-lymphocyte ratio: a simple, inexpensive and rapid prognostic marker for cardiovascular events. Platelets. 2015;26:680–1.
Uzun F, Erturk M, Cakmak HA, Kalkan AK, Akturk IF, Yalcin AA, et al. Usefulness of the platelet-to-lymphocyte ratio in predicting long-term cardiovascular mortality in patients with peripheral arterial occlusive disease. Postepy Kardiol Interwencyjnej. 2017;13:32–8.
Miglani RK, Bhateja N, Bhat RS, Kumar KV. Diagnostic role of platelet lymphocyte ratio (PLR) in pancreatic head masses. Indian J Surg. 2013;75:4–9.
Alexandrakis MG, Passam FH, Moschandrea IA, Christophoridou AV, Pappa CA, Coulocheri SA, et al. Levels of serum cytokines and acute phase proteins in patients with essential and cancer-related thrombocytosis. Am J Clin Oncol. 2003;26:135–40.
Funding
This work was supported by the National Research Foundation (NRF) funded by the Ministry of Education of South Korea (2018R1D1A1B07049400: Hai-Jeon Yoon and 2017R1D1A1B03035305: Daehee Kim) and the Grant of Translational R&D Project through Institute for Bio-Medical convergence, Incheon St. Mary’s Hospital, The Catholic University of Korea (IBC2018-06: Woon Jeong Lee).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
All authors have no potential conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kim, D., Yoon, HJ., Woo, S.H. et al. Development of visual scoring system with Tc-99m DMSA renal scintigraphy to predict the risk of recurrence of symptomatic urinary tract infections in pediatric patients. Ann Nucl Med 33, 708–715 (2019). https://doi.org/10.1007/s12149-019-01379-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12149-019-01379-0