Abstract
Objectives
To determine the prevalence of insulin resistance (IR), dyslipidemia and metabolic syndrome (MS) in children with asthma, aged 10 to 15 y, and to determine if these metabolic abnormalities showed an association with asthma symptom control and lung function.
Methods
A cross-sectional study was conducted at a tertiary centre in north India. Consecutive children with physician diagnosed asthma were enrolled. Asthma symptom control over previous four weeks was assessed as per Global Initiative for Asthma (GINA) recommendations. Fasting plasma glucose, serum insulin and lipid levels were estimated. Homeostasis Model Assessment- Insulin Resistance (HOMA-IR) was used as a marker of IR. Spirometry was performed for assessing lung function.
Results
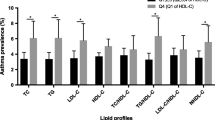
Eighty-three children were enrolled. Median (IQR) age was 12.0 (11.0, 13.5) y and mean (SD) body mass index (BMI) Z score was −0.42 (1.0). Median (IQR) HOMA-IR was 1.65 (1.06, 2.39). Prevalence of IR was 42.3% (95% CI: 31.7–52.9%). Number of children with elevated triglycerides, total cholesterol, and low-density lipoprotein (LDL)-cholesterol was 4 (4.8%), 4 (4.8%) and 5 (6%), respectively. Sixty-seven (80.7%) children had low high-density lipoprotein (HDL)-cholesterol. Only one subject was found to have metabolic syndrome. Presence of IR and elevation in serum insulin and triglycerides were associated with poorer asthma control, independent of BMI. None of the metabolic parameters were associated with lung function, after adjusting for height.
Conclusions
Among children with asthma, aged 10 to 15 y, the prevalence of IR was 42.3% (95% CI: 31.7–52.9%). Elevated serum insulin, triglycerides, and presence of IR were associated with poorer asthma control, after adjusting for BMI.

Similar content being viewed by others

References
Ford ES. The epidemiology of obesity and asthma. J Allergy Clin Immunol. 2005;115:897–909. quiz 910.
Ford ES, Mannino DM, Redd SC, Mokdad AH, Mott JA. Body mass index and asthma incidence among USA adults. Eur Respir J. 2004;24:740–4.
Raj D, Kabra SK, Lodha R. Childhood obesity and risk of allergy or asthma. Immunol Allergy Clin North Am. 2014;34:753–65.
Cottrell L, Neal WA, Ice C, Perez MK, Piedimonte G. Metabolic abnormalities in children with asthma. Am J Respir Crit Care Med. 2011;183:441–8.
Al-Shawwa B, Al-Huniti N, Titus G, Abu-Hasan M. Hypercholesterolemia is a potential risk factor for asthma. J Asthma. 2006;43:231–3.
Fessler MB, Massing MW, Spruell B, et al. Novel relationship of serum cholesterol with asthma and wheeze in the United States. J Allergy Clin Immunol. 2009;124:967–74.e1–15.
Kuschnir FC, Felix MMR, Caetano Kuschnir MC, et al. Severe asthma is associated with metabolic syndrome in brazilian adolescents. J Allergy Clin Immunol. 2018;141:1947–9.e4.
Arshi M, Cardinal J, Hill RJ, Davies PSW, Wainwright C. Asthma and insulin resistance in children. Respirol Carlton Vic. 2010;15:779–84.
Chen YC, Tung KY, Tsai CH, et al. Lipid profiles in children with and without asthma: Interaction of asthma and obesity on hyperlipidemia. Diabetes Metab Syndr. 2013;7:20–5.
Ross KR, Hart MA, Storfer-Isser A, et al. Obesity and obesity related co-morbidities in a referral population of children with asthma. Pediatr Pulmonol. 2009;44:877–84.
Global Initiative for Asthma. Global strategy for asthma management and prevention [Internet]. GINA. 2016. Available at: www.ginasthma.org. Accessed on 1 Feb 2016.
Conwell LS, Trost SG, Brown WJ, Batch JA. Indexes of insulin resistance and secretion in obese children and adolescents: a validation study. Diabetes Care. 2004;27:314–9.
Keskin M, Kurtoglu S, Kendirci M, Atabek ME, Yazici C. Homeostasis model assessment is more reliable than the fasting glucose/insulin ratio and quantitative insulin sensitivity check index for assessing insulin resistance among obese children and adolescents. Pediatrics. 2005;115:e500–3.
Alberti KGMM, Zimmet P, Shaw J. Metabolic syndrome–a new world-wide definition. A consensus statement from the international diabetes federation. Diabetes Med. 2006;23:469–80.
National Cholesterol Education Program (NCEP). Expert Panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III). Third report of the national cholesterol Education Program (NCEP) Expert Panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III) final report. Circulation. 2002;106:3143–421.
Cook S, Weitzman M, Auinger P, Nguyen M, Dietz WH. Prevalence of a metabolic syndrome phenotype in adolescents: findings from the third National Health and Nutrition Examination Survey, 1988–1994. Arch Pediatr Adolesc Med. 2003;157:821–7.
Khadilkar A, Ekbote V, Chiplonkar S, et al. Waist circumference percentiles in 2–18 year old indian children. J Pediatr. 2014;164:1358–62.e2.
Indian Academy of Pediatrics Growth Charts Committee, Khadilkar V, Yadav S, Agrawal KK, et al. Revised IAP growth charts for height, weight and body mass index for 5- to 18-year-old indian children. Indian Pediatr. 2015;52:47–55.
Raj M, Sundaram R, Paul M, Kumar K. Blood pressure distribution in indian children. Indian Pediatr. 2010;47:477–85.
Knudson RJ, Lebowitz MD, Holberg CJ, Burrows B. Changes in the normal maximal expiratory flow-volume curve with growth and aging. Am Rev Respir Dis. 1983;127:725–34.
Singh Y, Garg MK, Tandon N, Marwaha RK. A study of insulin resistance by HOMA-IR and its cut-off value to identify metabolic syndrome in urban indian adolescents. J Clin Res Pediatr Endocrinol. 2013;5:245–51.
Goyal JP, Kumar P, Thakur C, Khera D, Singh K, Sharma P. Effect of insulin resistance on lung function in asthmatic children. J Pediatr Endocrinol Metab. 2022;35:217–22.
Das RR, Mangaraj M, Panigrahi SK, Satapathy AK, Mahapatro S, Ray PS. Metabolic syndrome and insulin resistance in schoolchildren from a developing country. Front Nutr. 2020;7:31.
Morrison JA, Glueck CJ, Horn PS, Schreiber GB, Wang P. Homeostasis model assessment of insulin resistance* body mass index interactions at ages 9 to 10 years predict metabolic syndrome risk factor aggregate score at ages 18 to 19 years: a 10-year prospective study of black and white girls. Metabolism. 2009;58:290–5.
Tandon N, Garg MK, Singh Y, Marwaha RK. Prevalence of metabolic syndrome among urban indian adolescents and its relation with insulin resistance (HOMA-IR). J Pediatr Endocrinol Metab. 2013;26:1123–30.
Cho K-H, Kim J-R. Rapid decrease in HDL-C in the puberty period of boys associated with an elevation of blood pressure and dyslipidemia in korean teenagers: an explanation of why and when men have lower HDL-C levels than women. Med Sci. 2021;9:35.
Karampatakis N, Karampatakis T, Galli-Tsinopoulou A, et al. Impaired glucose metabolism and bronchial hyperresponsiveness in obese prepubertal asthmatic children. Pediatr Pulmonol. 2017;52:160–6.
Chanachon PN, Jotikasthira W, Kiewngam P, Sawatchai A, Kanchongkittiphon W, Manuyakorn W. Association of dyslipidemia and respiratory resistance assessed by the forced oscillation technique in asthmatic children. Lung. 2022;200:73–82.
Di Filippo P, Scaparrotta A, Rapino D, et al. Insulin resistance and lung function in obese asthmatic pre-pubertal children. J Pediatr Endocrinol Metab. 2018;31:45–51.
Forno E, Han YY, Muzumdar RH, Celedón JC. Insulin resistance, metabolic syndrome, and lung function in US adolescents with and without asthma. J Allergy Clin Immunol. 2015;136:304-11.e8.
Author information
Authors and Affiliations
Contributions
KK and RL conceptualized the study; KK, RL, KRJ, VJ and SKK were involved in designing the study; KK performed the data acquisition and analysis, and wrote the first draft; RL, KRJ, VJ and SKK revised and approved the final manuscript. RL will act as guarantor for this manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
Authors RL and SKK are members of the editorial board of the Journal. Authors KK, KRJ and VJ declare that there are no conflicts of interest relevant to this article.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kumar, K., Lodha, R., Jat, K.R. et al. Prevalence of Metabolic Abnormalities and their Association with Asthma Symptom Control in Children. Indian J Pediatr 91, 434–440 (2024). https://doi.org/10.1007/s12098-023-04716-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-023-04716-4