Abstract
Objective
To evaluate the proportion of patients who received empirical treatment with antitubercular therapy (ATT) prior to the diagnosis of Hodgkin lymphoma (HL) in the first multicentric, prospective study on HL from India, and to assess its impact on extent of disease at diagnosis and outcomes.
Methods
Children < 18 y with biopsy proven HL were enrolled in InPOG-HL-15-01. Along with other clinical and epidemiological data, history of prior treatment with ATT was documented. All patients received treatment as per a risk-stratified, response-adapted strategy.
Results
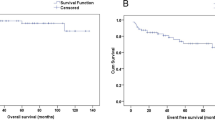
Out of 396, 115 (29%) children had received ATT prior to establishing a definitive diagnosis of HL. This cohort presented with advanced-stage disease (p = 0.001) and B symptoms (p = 0.001) in a higher proportion of cases. Consequently, those children were more likely to receive 6 rather than 4 cycles of chemotherapy (p = 0.001). They were more likely to have infradiaphragmatic involvement (p = 0.001). Overall survival and event-free survival were not different.
Conclusion
Empirical treatment with ATT in children presenting with lymphadenopathy continues to be practiced widely in India. The delay in diagnosis may contribute to children presenting with advanced-stage disease warranting more intensive treatment for successful outcomes.


Similar content being viewed by others
References
Sharma SK, Mohan A. Extrapulmonary tuberculosis. Indian J Med Res. 2004;120:316–53.
Maharjan M, Hirachan S, Kafle PK, et al. Incidence of tuberculosis in enlarged neck nodes, our experience. Kathmandu Univ Med J (KUMJ). 2009;7:54–8.
Working Group on Tuberculosis, Indian Academy of Pediatrics (IAP). Consensus statement on childhood tuberculosis. Indian Pediatr. 2010;47:41–55.
Sharma SK, Ryan H, Khaparde S, et al. Index-TB guidelines: Guidelines on extrapulmonary tuberculosis for India. Indian J Med Res. 2017;145:448–63.
Radhakrishnan V, Dhanushkhodi M, Ganesan TS, et al. Pediatric Hodgkin lymphoma treated at cancer institute, Chennai, India: long-term outcome. J Glob Oncol. 2016;3:545–54.
Arora RS, Mahajan A, Dinand V, et al. InPOG-HL-15-01- challenges and lessons learnt in setting up the first collaborative multicenter prospective clinical trial in childhood cancer in India. Pediatr Hematol Oncol J. 2020;5:166–70.
Mahajan A, Singh M, Bakhshi S, et al. Treating early-stage hodgkin lymphoma in resource-limited settings: InPOG–HL–15–01 experience. Pediatr Blood Cancer. 2021;68:e29219.
Pandit S, Choudhury S, Das A, Das SK, Bhattacharya S. Cervical lymphadenopathy–pitfalls of blind antitubercular treatment. J Health Popul Nutr. 2014;32:155–9.
Neal RD, Tharmanathan P, France B, et al. Is increased time to diagnosis and treatment in symptomatic cancer associated with poorer outcomes? systematic review. Br J Cancer. 2015;112(Suppl 1):S92–107.
Venkatasai JP, Srinivasamaharaj S, SnehaLM, Scott JX, Baby AK, Rajan M. Pediatric hematological malignancy: identification of issues involved in the road to diagnosis. South Asian J Cancer. 2017;6:28–30.
Antel K, Levetan C, Mohamed Z, et al. The determinants and impact of diagnostic delay in lymphoma in a TB and HIV endemic setting. BMC Cancer. 2019;19:384.
Ouedraogo M, Ouedraogo SM, Cisse R, et al. Active tuberculosis in a patient with Hodgkin’s disease: a case report. Rev Pneumol Clin. 2000;56:33–5.
Audebert F, Schneidewind A, Hartmann P, Kullmann F, Schölmerich J. Lymph node tuberculosis as primary manifestation of hodgkin’s disease. Med Klin (Munich). 2006;101:500–4.
Braylan RC, Long JC, Jaffe ES, Greco FA, Orr SL, Berard CW. Malignant lymphoma obscured by concomitant extensive epithelioid granulomas: report of three cases with similar clinicopathologic features. Cancer. 1977;39:1146–53.
Zeka AN, Tasbakan S, Cavusoglu C. Evaluation of the genexpert MTB/RIF Assay for rapid diagnosis of tuberculosis and detection of rifampin resistance in pulmonary and extra–pulmonary specimens. J Clin Microbiol. 2011;49:4138–41.
Acknowledgements
The authors acknowledge the contribution made by Krishnakumar Rathnam (Meenakshi Mission Hospital, Madurai, Tamil Nadu), Arun Sheshachalam (GVN Hospital Trichy, Tamil Nadu), Shailesh Kanvinde (Dinanath Mangeshkar Hospital, Maharashtra), Jayanthi Srirambathala (MNJ Hospital, Telangana), Soma De (SGCC & RI Hospital, West Bengal), Sirisha Rani (Rainbow Children Hospital, Hyderabad, Telangana), Biswajit Dubashi (JIPMER Hospital, Puducherry), Anupama Borker (Goa Medical College, Maharashtra), Pritanjali (AIIMS, Patna, Bihar), Nandini Hazarika (Rainbow Hospital, Delhi), Sanjeev Digra (GMC, Jammu), Praveen Sobti (CMC, Ludhiana, Punjab), Vineeta Gupta (BHU, Varanasi, Uttar Pradesh), Sunil Bhat (MSCC Bangalore), Hari Shankaran (Amrita Institute, Kochi), Priya Kumari (RCC, Trivandrum), Deepa Trivedi (Hematology-Oncology Clinic, Gujarat) and CanKids.
Funding
Cankids (Logistic).
Author information
Authors and Affiliations
Contributions
AM, SJ, RSA, VD, MK, JC: Conception and design, patient acquisition, and data analysis & interpretation; SB, M Singh, RS, NV, VR, PM, GK, M Sajid, RK, SM: Patient acquisition; AT: Data analysis & interpretation. JC will act as the guarantor for this paper.
Corresponding author
Ethics declarations
Ethical Clearance
All participating centers were required to seek approval from their institutional ethics committees.
Conflict of Interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mahajan, A., Bakhshi, S., Singh, M. et al. Empirical Antitubercular Treatment for Lymphadenopathy: Are We Missing Lymphoma?. Indian J Pediatr 90, 761–765 (2023). https://doi.org/10.1007/s12098-022-04180-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-022-04180-6