Abstract
Objective
To describe the prevalence and determinants of occurrence of dyslipidemia in children and adolescents with type 1 diabetes mellitus (T1DM).
Methods
A cross-sectional study was conducted in the diabetic clinic of a tertiary care referral hospital over two years. Subjects with T1DM aged 2–18 y had assessment of Lipid profile after 12 h of fasting. Glycemic control was assessed by glycosylated hemoglobin (HbA1C). Modifiable and nonmodifiable determining factors were assessed during clinic visit as per standard criteria. Body mass index (BMI) more than 23rd adult equivalent and 27th adult equivalent were considered as overweight and obesity, respectively. Lipid parameters were considered as abnormal if: Low density lipoprotein (LDL) > 100 mg/dL, high density lipoprotein (HDL) < 40 mg/dL, triglycerides > 100 mg/dL (< 10 y) and > 130 mg/dL (> 10 y).
Results
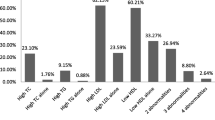
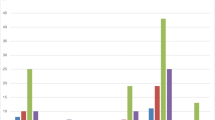
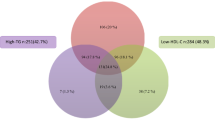
A total of 171 subjects (mean age: 11.8 ± 3.5 y, M:F = 75:96) were recruited during the study period. The mean fasting LDL level, HDL level, and triglyceride level observed in the study sample were 106.6 ± 26.9 mg/dL (62% abnormal), 52.6 ± 14.3 mg/dL (9.4% abnormal), and 85.3 ± 39.4 mg/dL (10.5% abnormal), respectively; 115 (67.3%) of the subjects had at least one abnormality in the serum lipid profile. On multivariate analysis, HbA1C was the most significant factor in determining the occurrence of dyslipidemia (p < 0.05). HbA1C was 9.9 ± 1.6 in subjects with abnormal LDL versus 9.1 ± 1.5 in those with normal LDL (p < 0.05).
Conclusion
Prevalence of dyslipidemia in the study children and adolescents with T1DM was 67.3%. HbA1C remains the most important modifiable determinant of the occurrence of dyslipidemia.


Similar content being viewed by others
Data Availability
On request.
References
de Ferranti SD, de Boer IH, Fonseca V, et al. Type 1 diabetes mellitus and cardiovascular disease: a scientific statement from the American heart association and American diabetes association. Circulation. 2014;130:1110–30.
Truong UT, Maahs DM, Daniels SR. Cardiovascular disease in children and adolescents with diabetes: where are we, and where are we going? Diabetes Technol Ther. 2012;14(Suppl 1):S11-21.
American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care. 2009;32(Suppl 1):S62–7.
Bell RA,Mayer-Davis EJ, Beyer JW, et al. SEARCH for Diabetes in Youth Study Group. Diabetes in non-hispanic white youth: prevalence, incidence, and clinical characteristics:the SEARCH for diabetes in youth study. Diabet Care. 2009;32 Suppl 2:S102–11.
International Diabetes Federation. IDF Diabetes Atlas, 8th edn. Brussels, Belgium. In: International Diabetes Federation. 2017. Available at: http://www.diabetesatlas.org. Accessed on 17 Feb 2019.
Virmani A. Type 1 diabetes in India: the numbers show the way ahead. Indian Pediatr. 2019;56:189–90.
Donaghue KC, Marcovecchio ML, Wadwa RP, et al. ISPAD clinical practice consensus guidelines 2018: microvascular and macrovascular complications in children and adolescents. Pediatr Diabetes. 2018;19(Suppl 27):262–74.
Moreno PR, Murcia AM, Palacios IF, et al. Coronary composition and macrophage infiltration in atherectomy specimens from patients with diabetes mellitus. Circulation. 2000;102:2180–4.
Hayaishi-Okano R, Yamasaki Y, KatakamiN, et al. Elevated C-reactive protein associates with early-stage carotid atherosclerosis in young subjects with type 1 diabetes. Diabetes Care. 2002;25:1432–8
Schölin A, Siegbahn A, Lind L, et al. Diabetes Incidence Study in Sweden Group. CRP and IL–6 concentrations are associated with poor glycemic control despite preserved beta-cell function during the first year after diagnosis of type 1 diabetes. Diabetes Metab Res Rev. 2004;20:205–10.
Schwab KO, Doerfer J, Marg W, Schober E, Holl RW. DPV Science Initiative and the Competence Network Diabetes mellitus. Characterization of 33 488 children and adolescents with type 1 diabetes based on the gender-specific increase of cardiovascular risk factors. Pediatr Diabetes. 2010;11:357–63
Chiang JL, Maahs DM, Garvey KC, et al. Type 1 diabetes in children and adolescents: a position statement by the American diabetes association. Diabetes Care. 2018;41:2026–44.
Expert Panel on Integrated Guidelines for Cardiovascular Health and Risk Reduction in Children and Adolescents. National Heart, Lung, and Blood Institute. Expert panel on integrated guidelines for cardiovascular health and risk reduction in children and adolescents: summary report. Pediatrics. 2011;128 Suppl 5:S213–56.
Margeirsdottir HD, Larsen JR, Brunborg C, Overby NC, Dahl-Jørgensen K. Norwegian Study Group for Childhood Diabetes. High prevalence of cardiovascular risk factors in children and adolescents with type 1 diabetes: a population-based study. Diabetologia. 2008;51:554–61.
Shah N, Khadilkar A, Gondhalekar K, Khadilkar V. Prevalence of dyslipidemia in Indian children with poorly controlled type 1 diabetes mellitus. Pediatr Diabetes. 2020;21:987–94.
Homma TK, Endo CM, Saruhashi T, et al. Dyslipidemia in young patients with type 1 diabetes mellitus. Arch Endocrinol Metab. 2015;59:215–9.
Kim G, DeSalvo D, Guffey D, et al. Dyslipidemia in adolescents and young adults with type 1 and type 2 diabetes: a retrospective analysis. Int J Pediatr Endocrinol. 2020;2020:11.
Zabeen B, Balsa AM, Islam N, Parveen M, Nahar J, Azad K. Lipid profile in relation to glycemic control in type 1 diabetes children and adolescents in Bangladesh. Indian J Endocrinol Metab. 2018;22:89–92.
WHO Child growth standards. Acta Pediatr Supplement. 2006;450:5–101.
Indian Academy of Pediatrics Growth Charts Committee, Khadilkar V, Yadav S, Agrawal KK, et al. Revised IAP growth charts for height, weight and body mass index for 5- to 18-year-old Indian children. Indian Pediatr. 2015;52:47–55.
Chalil VK, Prasad HK, Nassir SAMA, Arulalan KV, Sangaralingam T, Krishnamoorthy N. A study on new IAP 2015 growth references in rural South Indian children. Indian J Pediatr. 2021;88:645–9.
Khadilkar A, Ekbote V, Chiplonkar S, et al.Waist circumference percentiles in 2–18 year old Indian children. J Pediatr. 2014;164:1358–62.
Khadilkar A, Mandlik R, Chiplonkar S, Khadilkar V, Ekbote V, Patwardhan V. Reference centile curves for triceps skinfold thickness for Indian children aged 5 to 17 years and cut offs for predicting risk of childhood hypertension: a multi-centric study. Indian Pediatr. 2015;52:675–80.
Flynn JT, Kaelber DC, Baker-Smith CM, et al. Subcommittee On Screening And Management Of High Blood Pressure In Children. Clinical practice guideline for screening and management of high blood pressure in children and adolescents. Pediatrics. 2017;140:e20171904.
Nadeau KJ, Regensteiner JG, Bauer TA, et al. Insulin resistance in adolescents with type 1 diabetes and its relationship to cardiovascular function. J Clin Endocrinol Metab. 2010;95:513–21.
Purnel JQ, Hokanson JE, Marcovina SM, Steffes MW, Cleary PA, Brunzell JD. Effect of excessive weight gain with intensive therapy of type 1 diabetes on lipid levels and blood pressure: results from the DCCT. Diabetes control and complications trial. JAMA. 1998;280:140–6.
Nathan DM, Cleary PA, Backlund JY, et al. Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications (DCCT/EDIC) Study Research Group. Intensive diabetes treatment and cardiovascular disease in patients with type 1 diabetes. N Engl J Med. 2005;353:2643–53.
Vinik AI, Erbas T, Park TS, Nolan R, Pittenger GL. Platelet dysfunction in type 2 diabetes. Diabetes Care. 2001;24:1476–85.
Larsen J, Brekke M, Sandvik L, Arnesen H, Hanssen KF, Dahl-Jorgensen K. Silent coronary atheromatosis in type 1 diabetic patients and its relation to long-term glycemic control. Diabetes. 2002;51:2637–41.
Acknowledgements
The authors would like to thank Prof Nedunchelian K. for reading and reviewing this manuscript. They also thank all the children and their families for participating in this study.
Author information
Authors and Affiliations
Contributions
MS was involved in data collection and tabulation; HKP, TS, BP, and SW were involved in the clinical management of cases and study conceptualization; BP and TS were involved in data analysis; SW, HKP, BP, TS contributed to the manuscript; All authors have read the final manuscript and approve the final version of the manuscript. HKP will act as the guarantor for this paper.
Corresponding author
Ethics declarations
Ethics Approval
The study was approved by Mehta Mutispeciality Hospitals IEC, Chennai. Approval number/IRB number: IRB-MCH/011/2019.
Conflict of Interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Selvaraj, M., Prasad, H.K., White, S. et al. Prevalence and Determinants of Occurrence of Dyslipidemia in Subjects with Type 1 Diabetes Mellitus. Indian J Pediatr 90, 118–123 (2023). https://doi.org/10.1007/s12098-022-04130-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-022-04130-2