Abstract
Objectives
To determine the feasibility and efficacy of home-based sensory interventions in children with Autism spectrum disorder (ASD) with sensory processing abnormalities.
Methods
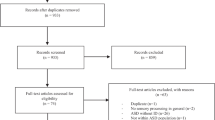
This was a 12-wk, parallel group, pilot, randomized controlled trial. During the study-period, 185 children with ASD between 3–12 y of age, with sensory processing abnormalities were screened for eligibility. Twenty-one children were randomly assigned to the sensory-intervention group and 19 to the standard-therapy group. Sensory-intervention group received home-based sensory interventions by the parents/caregivers plus standard therapy; standard-therapy group received speech therapy by the speech pathologists and applied behavior analysis by the child psychologist.
Results
The mean change in scores at baseline and 12 wk into intervention showed that children in sensory-intervention group (Mean = 9.33, SD = 3.52) scored significantly better on Parent Rated 10-item Likert Scale (PRILS-10), as compared to standard-therapy group (Mean = 2.47, SD = 1.46), t(36) = 8.16, p < 0.001; d = 2.54. Marked improvement was noted especially in reduction of hyperactivity, motor-stereotypies and auditory sensitivity in those who underwent sensory interventions. The mean change in scores in sensory-intervention group on Children’s Global Assessment Scale (CGAS) (Mean = −9.19, SD = 2.33, p < 0.011; d = −1.75) and Pediatric Quality of Life Inventory 4.0 (PedsQLTM) (M = −10.53, SD = 5.34, p = 0.008; d = −0.88) showed significant difference in the sensory-intervention group as compared to standard-therapy group. Overall, there was 32.3%, 18.1% and 15.8% improvement on PRILS-10, CGAS and PedsQLTM respectively in sensory-intervention group.
Conclusions
The present findings suggest that home-based sensory interventions are feasible in a developing country and are suggested to have a beneficial role in ASD.

Similar content being viewed by others
Abbreviations
- ASD:
-
Autism spectrum disorder
- HBSI:
-
Home-based sensory interventions
- PRILS-10:
-
Parent rated 10-item Likert scale
- CGAS:
-
Children’s Global Assessment Scale
- PedsQL:
-
Pediatric quality of life inventory
- SI:
-
Sensory-intervention
- ST:
-
Standard-therapy
References
Arlington VA. Diagnostic and statistical manual of mental disorders. 5th ed. Washington DC: American Psychiatric association; 2013.
Kanner L. Autistic disturbances of affective contact. Nerv Child. 1943;2:217–50.
Hazen EP, Stornelli JL, O’Rourke JA, Koesterer K, McDougle CJ. Sensory symptoms in autism spectrum disorders. Harv Rev Psychiatry. 2014;22:112–24.
Marco EJ, Hinkley LB, Hill SS, Nagarajan SS. Sensory processing in autism: a review of neurophysiologic findings. Pediatr Res. 2011;69:48R–54R.
Hardan AY, Pabalan M, Gupta N, et al. Corpus callosum volume in children with autism. Psychiatry Res. 2009;174:57–61.
Kern JK. The possible role of the cerebellum in autism/PDD: disruption of a multisensory feedback loop. Med Hypotheses. 2002;59:255–60.
Schaaf RC, Toth-Cohen S, Johnson SL, Outten G, Benevides TW. The everyday routines of families of children with autism: examining the impact of sensory processing difficulties on the family. Autism. 2011;15:373–89.
Green VA, Pituch KA, Itchon J, Choi A, O’Reilly M, Sigafoos J. Internet survey of treatments used by parents of children with autism. Res Dev Disabil. 2006;27:70–84.
Weitlauf AS, Sathe N, McPheeters ML, Warren ZE. Interventions targeting sensory challenges in autism spectrum disorder: a systematic review. Pediatrics. 2017; https://doi.org/10.1542/peds.2017-0347.
Pfeiffer BA, Koenig K, Kinnealey M, Sheppard M, Henderson L. Effectiveness of sensory integration interventions in children with autism spectrum disorders: a pilot study. Am J Occup Ther. 2011;65:76–85.
Schaaf RC, Benevides T, Mailloux Z, et al. An intervention for sensory difficulties in children with autism: a randomized trial. J Autism Dev Disord. 2014;44:1493–506.
Woo CC, Leon M. Environmental enrichment as an effective treatment for autism: a randomized controlled trial. Behav Neurosci. 2013;127:487–97.
Dunn W. Sensory profile 2: user’s manual. San Antonio: Psychological Corporation; 2014.
Schopler E, Reichler R, Rochen Renner B. The childhood autism rating scale. Los Angeles: Western Psychological Services; 1988.
Doll EA. A genetic scale of social maturity. Am J Orthop. 1935;5:180–8.
Bairwa M, Rajput M, Sachdeva S. Modified Kuppuswamy’s socioeconomic scale: social researcher should include updated income criteria, 2012. Indian J Community Med. 2013;38:185–6.
Alpern G. Developmental profile-3. Los Angeles: Western Psychological Services; 2007.
Malin AJ. Malin’s intelligence scale for children-manual. Lucknow: Indian Psychological Corporation; 1969.
Shaffer D, Gould MS, Brasic J, et al. A children’s global assessment scale (CGAS). Arch Gen Psychiatry. 1983;40:1228–31.
Nagaraj R, Singhi P, Malhi P. Risperidone in children with autism: randomized, placebo controlled, double-blind study. J Child Neurol. 2006;21:450–5.
Varni JW. Pediatric quality of life inventory version 4.0. Lyon: Mapi Research Institute; 1998.
Ikeda E, Hinckson E, Krageloh C. Assessment of quality of life in children and youth with autism spectrum disorder: a critical review. Qual Life Res. 2014;23:1069–85.
Varni JW, Seid M, Kurtin PS. PedsQL 4.0: reliability and validity of the pediatric quality of life inventory version 4.0 generic core scales in healthy and patient populations. Med Care. 2001;39:800–12.
Bastiaansen D, Koot HM, Bongers IL, Varni JW, Verhulst FC. Measuring quality of life in children referred for psychiatric problems : psychometric properties of the Peds QL 4.0 generic core scales. Qual Life Res. 2004;13:489–95.
Woo CC, Donnelly JH, Steinberg-Epstein R, Leon M. Environmental enrichment as a therapy for autism: a clinical trial replication and extension. Behav Neurosci. 2015;129:412–22.
Aronoff E, Hillyer R, Leon M. Environmental enrichment therapy for autism: outcomes with increased access. Neural Plast. 2016;2016:2734915.
Acknowledgements
The authors acknowledge the parents who took part in the study.
Author information
Authors and Affiliations
Contributions
HP and JKS were involved in conception of the work, data acquisition, analysis, interpretation of the data and prepared the first draft. PM did the psychological assessments and was also involved in data acquisition. PS was the clinician in charge, was involved in design, planned and guided the study, and did critical review of the manuscript for intellectual content. The final manuscript was corrected and approved by all authors. PS will act as guarantor for this paper.
Corresponding author
Ethics declarations
Ethical Approval
“All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.” Ethical approval has been obtained from institute ethics committee (NK/2024/DM/4312). Patients and their parents have given informed consent to the research and to publication of the results.
Conflict of Interest
None.
Rights and permissions
About this article
Cite this article
Padmanabha, H., Singhi, P., Sahu, J.K. et al. Home-based Sensory Interventions in Children with Autism Spectrum Disorder: A Randomized Controlled Trial. Indian J Pediatr 86, 18–25 (2019). https://doi.org/10.1007/s12098-018-2747-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-018-2747-4
Keywords
- Home-based sensory interventions
- Autism Spectrum Disorder
- Sensory-processing abnormalities
- Randomized controlled trial