Abstract
Objective
To investigate the presence of childhood brucellosis presenting as PUO (pyrexia of unknown origin) cases in Eastern zone of India.
Methods
Blood samples were collected from PUO patients aged ≤18 y. The main diagnostic tools were STAT, RBPT, ELISA- IgM, IgG and PCR. Although mainly PUO cases were selected for the study, other associated clinical manifestations were also noted.
Results
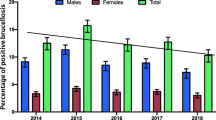
The findings revealed significantly higher percentage of infection in female children (14.3%) than in male children (10.9%). The positive results by different diagnostic tools, STAT, RBPT, ELISA- IgM, ELISA-IgG and brucella genus specific PCR were 10.6%, 7.2%, 7.2%, 0.85% and 1.3% respectively. Main associated clinical symptoms were joint pain, low backache, fatigue and night sweat.
Conclusions
This hospital based study reflects a significant number of childhood brucellosis cases in Eastern zone of India, and thus emphasizes the need for further monitoring of such subjects.

Similar content being viewed by others
References
Young EJ. Brucella species. In: Mandell GL, Benett JE, Dolin R, editors. Principles and Practice of Infectious Diseases. 5th ed. Philadelphia: Churchill Livingstone; 2000. p. 2386–93.
Young EJ. An overview of human brucellosis. Clin Infect Dis. 1995;21:283–90.
Pappas G, Akritidis N, Bosilkovski M, Tsianos E. Brucellosis. N Engl J Med. 2005;352:2325–36.
Sharda DC, Lubani M. A study of brucellosis in childhood. Clin Pediatr (Phila). 1986;25:492–5.
Gottesman G, Vanunu D, Maayan MC, et al. Childhood brucellosis in Israel. Pediatr Infect Dis J. 1996;15:610–5.
Tanir G, Tufekci SB, Tuygun N. Presentation, complications and treatment outcome of brucellosis in Turkish children. Pediatr Int. 2009;51:114–9.
Sutcu M, Gokceer D, Akturk H, et al. Brucellosis infection in a child with progressive familial intrahepatic cholestasis type 2 who had undergone liver transplantation. Pediatr Transplant. 2015;19:E146–8.
Colmenero JD, Regnera JM, Martos F, et al. Complications associated with Brucella melitensis infection: a study of 530 cases. Medicine. 1996;75:195–211.
Boschiroli ML, Foulongne V, O’Callaghan D. Brucellosis: a worldwide zoonosis. Curr Opin Microbiol. 2001;4:58–64.
Schutze GE, Jacobs RF. Brucella. In: Kliegman RM, Stanton BF, St. Geme III JW, Schor NF, Behrman RE, editors. Nelson Textbook of Pediatrics. Philadelphia: Elsevier Saunders; 2011. p. 980–2.
Mantur BG, Akki AS, Mangalgi SS, Patil SV, Gobbur RH, Peerapur BV. Childhood brucellosis- a microbiological, epidemiological and clinical study. J Trop Pediatr. 2004;50:153–7.
Madkour MM. Childhood brucellosis. In: Madkour MM, editor. Brucellosis. Cambridge: Butterworths; 1989. p. 205–18.
Feiz J, Sabbaghian H, Miralai M. Brucellosis due to B. melitensis in children. Clinical and epidemiologic observations on 95 patients studied in central Iran. Clin Pediatr (Phila). 1978;17:904–7.
Havaldar PV, Kumar SY, Desai AS, Siddibhavi BM. Brucellosis in children. Indian Pediatr. 1987;24:995–8.
Mantur BG, Biradar MS, Bidri RC. Protean clinical manifestations and diagnostic challenges of human brucellosis in adults: 16 y experience in an endemic area. J Med Microbiol. 2006;55:897–903.
Ciftdogan DY, Bayram N, Vardar F. Brucellosis as a cause of fever of unknown origin in children admitted to a tertiary hospital in the Aegean region of Turkey. Vector-Borne Zoonotic Dis. 2011;11:1037–40.
Godfroid J, Cloeckaert A, Liantard JP, et al. From the discovery of the Malta fever’s agent to the discovery of a marine mammal reservoir, brucellosis has continuously been a re-emerging zoonosis. Vet Res. 2005;36:313–26.
Solera J. Update on brucellosis: therapeutic challenges. Int J Antimicrob Agents. 2010;36:S18–20.
Araj GF, Kaufmann AF. Determination by enzyme linked immunosorbent assay of immunoglobulin G (IgG), IgM and IgA to Brucella melitensis major outer membrane proteins and whole-cell heat-killed antigens in sera of patients with brucellosis. J Clin Microbiol. 1989;27:1909–12.
Pickering LK, Baker CJ, Kimberlin DW, Long SS. Report of the Committee on Infectious Diseases. Red Book. Elk Grove Village: American Academy of Pediatrics; 2009. p. 237–9.
Corbel MJ, Alton GG, Ariza J. editors. Brucellosis in humans and animals. Geneva: World Health Organization 2006.
Ascoli A. Immunity and receptivity to Brucella abortus in the albino rat. Exp Med Surg. 1947;5:107–27.
Pugh LH. Effect of gonadal hormones on experimental infection of rats with Brucella abortus. Exp Biol Med. 1948;68:591–2.
Memish Z. Brucellosis control in Saudi Arabia: prospects and challenges. J Chemother. 2001;13:11–7.
Acknowledgements
The authors hereby acknowledge the support received from all staffs of Department of Microbiology, Peerless Hospital & B. K. Roy Research Centre, Kolkata.
Contributions
All the authors were involved in the study. DD performed the study protocols, analyzed the data and drafted the manuscript. SD designed the study, critically reviewed, finalized the manuscript and will act as guarantor for this paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
None.
Source of Funding
This study was funded by the Department of Biotechnology (DBT), Government of India (Grant No. & Date: 102/IFD/SAN/3141/2012–2013 dated September, 27 2012).
Rights and permissions
About this article
Cite this article
Dutta, D., Sen, A., Gupta, D. et al. Childhood Brucellosis in Eastern India. Indian J Pediatr 85, 266–271 (2018). https://doi.org/10.1007/s12098-017-2513-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-017-2513-z