Abstract
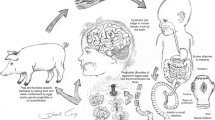
Neurocysticercosis is the most common helminth infection of nervous system in humans caused by the encysted larvae of Taenia solium. It is a major cause of epilepsy in tropical areas and the most common cause of focal-onset seizures in North Indian children. Children with neurocysticercosis have pleomorphic manifestations depending on the location, number and viability of the cysts and host response. In endemic areas, neurocysticercosis should be clinically suspected in any child with recent-onset seizures, headache or focal motor deficits where there is no other suggestion of an underlying neurological disorder. Diagnosis of neurocysticercosis is essentially based on neuroimaging; visualization of a scolex is diagnostic. Management includes use of cysticidal drugs usually albendazole, which seems to be effective for lesion resolution and seizure remission, use of steroids and anti-epileptic drugs. Single lesions portend good prognosis with resolution of lesions in >60% of the cases within 6 mo and good seizure control. Prognosis is guarded in cysticercus encephalitis, racemose and extraparenchymal neurocysticercosis.


Similar content being viewed by others
References
Relationship between epilepsy and tropical diseases. Commission on tropical diseases of the international league against epilepsy. Epilepsia. 1994;35:89–93.
Singhi P, Ray M, Singhi S, Khandelwal N. Clinical spectrum of 500 children with neurocysticercosis and response to albendazole therapy. J Child Neurol. 2000;15:207–13.
Ndimubanzi PC, Carabin H, Budke CM, et al. A systematic review of the frequency of neurocyticercosis with a focus on people with epilepsy. PLoS Negl Trop Dis. 2010;4:e870.
WHO. Accelerating work to overcome the global impact of neglected tropical diseases. A roadmap for impementation. Switzerland: World Health Organization; 2012.
Del Brutto OH, Garcia HH. Neurocysticercosis in nonendemic countries: time for a reappraisal. Neuroepidemiology. 2012;39:145–6.
Serpa JA, White AC Jr. Neurocysticercosis in the United States. Pathog Glob Health. 2012;106:256–60.
Mafojane NA, Appleton CC, Krecek RC, Michael LM, Willingham AL 3rd. The current status of neurocysticercosis in eastern and southern Africa. Acta Trop. 2003;87:25–33.
Praet N, Speybroeck N, Manzanedo R, et al. The disease burden of Taenia solium cysticercosis in Cameroon. PLoS Negl Trop Dis. 2009;3:e406.
Montano SM, Villaran MV, Ylquimiche L, et al. Neurocysticercosis: association between seizures, serology, and brain CT in rural Peru. Neurology. 2005;65:229–33.
Medina MT, Aguilar-Estrada RL, Alvarez A, et al. Reduction in rate of epilepsy from neurocysticercosis by community interventions: the Salama, Honduras study. Epilepsia. 2011;52:1177–85.
Fleury A, Hernandez M, Fragoso G, Parkhouse RM, Harrison LJ, Sciutto E. Detection of secreted cysticercal antigen: a useful tool in the diagnosis of inflammatory neurocysticercosis. Trans R Soc Trop Med Hyg. 2003;97:542–6.
Khurana S, Aggarwal A, Malla N. Prevalence of anti-cysticercus antibodies in slum, rural and urban populations in and around union territory, Chandigarh. Indian J Pathol Microbiol. 2006;49:51–3.
Sahu PS, Patro S, Jena PK, Swain SK, Das BK. Imaging and serological-evidence of neurocysticercosis among patients with seizures in Odisha, an unexplored eastern coastal province in India. J Clin Diagn Res. 2015;9:DC06–10.
Cherian A, Syam UK, Sreevidya D, et al. Low seroprevalence of systemic cysticercosis among patients with epilepsy in Kerala--South India. J Infect Public Health. 2014;7:271–6.
Parija SC, Balamurungan N, Sahu PS, Subbaiah SP. Cysticercus antibodies and antigens in serum from blood donors from Pondicherry, India. Rev Inst Med Trop Sao Paulo. 2005;47:227–30.
Prasad KN, Prasad A, Gupta RK, et al. Neurocysticercosis in patients with active epilepsy from the pig farming community of Lucknow district, north India. Trans R Soc Trop Med Hyg. 2009;103:144–50.
Prasad KN, Verma A, Srivastava S, Gupta RK, Pandey CM, Paliwal VK. An epidemiological study of asymptomatic neurocysticercosis in a pig farming community in northern India. Trans R Soc Trop Med Hyg. 2011;105:531–6.
Singh G, Bawa J, Chinna D, et al. Association between epilepsy and cysticercosis and toxocariasis: a population-based case-control study in a slum in India. Epilepsia. 2012;53:2203–8.
Singhi P, Singhi S. Neurocysticercosis in children. J Child Neurol. 2004;19:482–92.
Ito A, Putra MI, Subahar R, et al. Dogs as alternative intermediate hosts of Taenia solium in Papua (Irian Jaya), Indonesia confirmed by highly specific ELISA and immunoblot using native and recombinant antigens and mitochondrial DNA analysis. J Helminthol. 2002;76:311–4.
Mahanty S, Garcia HH. Cysticercosis and neurocysticercosis as pathogens affecting the nervous system. Prog Neurobiol. 2010;91:172–84.
Alvarez JI, Rivera J, Teale JM. Differential release and phagocytosis of tegument glycoconjugates in neurocysticercosis: implications for immune evasion strategies. PLoS Negl Trop Dis. 2008;2:e218.
Verma A, Prasad KN, Gupta RK, et al. Toll-like receptor 4 polymorphism and its association with symptomatic neurocysticercosis. J Infect Dis. 2010;202:1219–25.
Cooke JC, Gelman JS, Harper RW. Echocardiologists' role in the deployment of the Amplatzer atrial septal occluder device in adults. J Am Soc Echocardiogr. 2001;14:588–94.
Rathore C, Thomas B, Kesavadas C, Radhakrishnan K. Calcified neurocysticercosis lesions and hippocampal sclerosis: potential dual pathology? Epilepsia. 2012;53:e60–2.
Morales NM, Agapejev S, Morales RR, Padula NA, Lima MM. Clinical aspects of neurocysticercosis in children. Pediatr Neurol. 2000;22:287–91.
Singhi P, Saini AG, Sankhyan N. Amaurosis fugax caused by neurocysticercosis. Pediatr Infect Dis J. 2014;33:427.
Singhi P. Neurocysticercosis. Ther Adv Neurol Disord. 2011;4:67–81.
Saini AG, Vyas S, Singhi P. Racemose neurocysticercosis. J Infect Public Health. 2017. https://doi.org/10.1016/j.jiph.2016.11.019.
Singhi P, Saini AG. Pediatric neurocysticercosis: current challenges and future prospects. Pediatr Health Med Ther. 2016;7:5–16.
Singhi P, Singhi S. Neurocysticercosis in children. Indian J Pediatr. 2009;76:537–45.
Del Brutto OH, Wadia NH, Dumas M, Cruz M, Tsang VC, Schantz PM. Proposal of diagnostic criteria for human cysticercosis and neurocysticercosis. J Neurol Sci. 1996;142:1–6.
Del Brutto OH. Diagnostic criteria for neurocysticercosis, revisited. Pathog Glob Health. 2012;106:299–304.
Singhi PD, Baranwal AK. Single small enhancing computed tomographic lesion in Indian children--I: evolution of current concepts. J Trop Pediatr. 2001;47:204–7.
do Amaral LL, Ferreira RM, da Rocha AJ, Ferreira NP. Neurocysticercosis: evaluation with advanced magnetic resonance techniques and atypical forms. Top Magn Reson Imaging. 2005;16:127–44.
Singhi PD, Baranwal AK. Single small enhancing computed tomographic lesions in indian children--II. Clinical features, pathology, radiology and management. J Trop Pediatr. 2001;47:266–70.
Pretell EJ, Martinot C Jr, Garcia HH, Alvarado M, Bustos JA, Martinot C. Differential diagnosis between cerebral tuberculosis and neurocysticercosis by magnetic resonance spectroscopy. J Comput Assist Tomogr. 2005;29:112–4.
Rajshekhar V, Haran RP, Prakash GS, Chandy MJ. Differentiating solitary small cysticercus granulomas and tuberculomas in patients with epilepsy. Clinical and computerized tomographic criteria. J Neurosurg. 1993;78:402–7.
Atluri SR, Singhi P, Khandelwal N, Malla N. Evaluation of excretory secretory and 10-30 kDa antigens of Taenia solium cysticerci by EITB assay for the diagnosis of neurocysticercosis. Parasite Immunol. 2009;31:151–5.
Sahu PS, Parija SC, Jayachandran S. Antibody specific to 43kDa excretory-secretory antigenic peptide of Taenia solium metacestode as a potential diagnostic marker in human neurocysticercosis. Acta Trop. 2010;115:257–61.
Atluri SR, Singhi P, Khandelwal N, Malla N. Neurocysticercosis immunodiagnosis using Taenia solium cysticerci crude soluble extract, excretory secretory and lower molecular mass antigens in serum and urine samples of Indian children. Acta Trop. 2009;110:22–7.
Sahu PS, Parija S, Kumar D, Jayachandran S, Narayan S. Comparative profile of circulating antigenic peptides in CSF, serum & urine from patients with neurocysticercosis diagnosed by immunoblotting. Parasite Immunol. 2014;36:509–21.
Wilson M, Bryan RT, Fried JA, et al. Clinical evaluation of the cysticercosis enzyme-linked immunoelectrotransfer blot in patients with neurocysticercosis. J Infect Dis. 1991;164:1007–9.
Mandal J, Singhi PD, Khandelwal N, Malla N. Evaluation of ELISA and dot blots for the serodiagnosis of neurocysticercosis, in children found to have single or multiple enhancing lesions in computerized tomographic scans of the brain. Ann Trop Med Parasitol. 2006;100:39–48.
Rodriguez S, Dorny P, Tsang VC, et al. Detection of Taenia solium antigens and anti-T. solium antibodies in paired serum and cerebrospinal fluid samples from patients with intraparenchymal or extraparenchymal neurocysticercosis. J Infect Dis. 2009;199:1345–52.
Noh J, Rodriguez S, Lee YM, et al. Recombinant protein- and synthetic peptide-based immunoblot test for diagnosis of neurocysticercosis. J Clin Microbiol. 2014;52:1429–34.
Garcia HH, Gilman RH, Catacora M, Verastegui M, Gonzalez AE, Tsang VC. Serologic evolution of neurocysticercosis patients after antiparasitic therapy. Cysticercosis working group in Peru. J Infect Dis. 1997;175:486–9.
Camargo JA, Bertolucci PH. Quantification of Fas protein in CSF of patients with neurocysticercosis. Arq Neuropsiquiatr. 2012;70:262–6.
Camargo JA, Bertolucci PH. Quantification of amino acid neurotransmitters in cerebrospinal fluid of patients with neurocysticercosis. Open Neurol J. 2015;9:15–20.
Otte WM, Singla M, Sander JW, Singh G. Drug therapy for solitary cysticercus granuloma: a systematic review and meta-analysis. Neurology. 2013;80:152–62.
Kaur S, Singhi P, Singhi S, Khandelwal N. Combination therapy with albendazole and praziquantel versus albendazole alone in children with seizures and single lesion neurocysticercosis: a randomized, placebo-controlled double blind trial. Pediatr Infect Dis J. 2009;28:403–6.
Baird RA, Wiebe S, Zunt JR, Halperin JJ, Gronseth G, Roos KL. Evidence-based guideline: treatment of parenchymal neurocysticercosis: report of the guideline development subcommittee of the American Academy of neurology. Neurology. 2013;80:1424–9.
Singhi P, Dayal D, Khandelwal N. One week versus four weeks of albendazole therapy for neurocysticercosis in children: a randomized, placebo-controlled double blind trial. Pediatr Infect Dis J. 2003;22:268–72.
Garcia HH, Evans CA, Nash TE, et al. Current consensus guidelines for treatment of neurocysticercosis. Clin Microbiol Rev. 2002;15:747–56.
Singhi P, Jain V, Khandelwal N. Corticosteroids versus albendazole for treatment of single small enhancing computed tomographic lesions in children with neurocysticercosis. J Child Neurol. 2004;19:323–7.
Singhi PD, Dinakaran J, Khandelwal N, Singhi SC. One vs. two years of anti-epileptic therapy in children with single small enhancing CT lesions. J Trop Pediatr. 2003;49:274–8.
Ash A, Okello A, Khamlome B, Inthavong P, Allen J, Thompson RC. Controlling Taenia solium and soil transmitted helminths in a northern Lao PDR village: impact of a triple dose albendazole regime. Acta Trop. 2015; https://doi.org/10.1016/j.actatropica.2015.05.018.
O'Neal SE, Moyano LM, Ayvar V, et al. Ring-screening to control endemic transmission of Taenia solium. PLoS Negl Trop Dis. 2014;8:e3125.
Panic G, Duthaler U, Speich B, Keiser J. Repurposing drugs for the treatment and control of helminth infections. Int J Parasitol Drugs Drug Resist. 2014;4:185–200.
Devi R, Jain A, Hurkat P, Jain SK. Dual drug delivery using lactic acid conjugated SLN for effective management of neurocysticercosis. Pharm Res. 2015;32:3137–48.
Author information
Authors and Affiliations
Contributions
PS: Revision of the draft and final approval of the manuscript; AGS: Drafted the manuscript and reviewed the literature. PS will act as guarantor for this paper.
Corresponding author
Ethics declarations
Conflict of Interest
None.
Source of Funding
None.
Rights and permissions
About this article
Cite this article
Singhi, P., Saini, A.G. Pediatric Neurocysticercosis. Indian J Pediatr 86, 76–82 (2019). https://doi.org/10.1007/s12098-017-2460-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-017-2460-8