Abstract
Objectives
To assess iodine and iron nutritional status among Nepalese school children.
Methods
A cross-sectional, community based study was conducted in the two districts, Ilam (hilly region) and Udayapur (plain region) of eastern Nepal. A total of 759 school children aged 6–13 y from different schools within the study areas were randomly enrolled. A total of 759 urine samples and 316 blood samples were collected. Blood hemoglobin level, serum iron, total iron binding capacity and urinary iodine concentration was measured. Percentage of transferrin saturation was calculated using serum iron and total iron binding capacity values.
Results
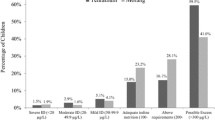
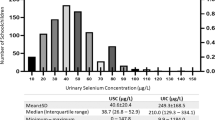
The mean level of hemoglobin, serum iron, total iron binding capacity, transferrin saturation and median urinary iodine excretion were 12.29 ± 1.85 g/dl, 70.45 ± 34.46 μg/dl, 386.48 ± 62.48 μg/dl, 19.94 ± 12.07 % and 274.67 μg/L respectively. Anemia, iron deficiency and iodine deficiency (urinary iodine excretion <100 μg/L) were present in 34.5 %, 43.4 % and 12.6 % children respectively. Insufficient urinary iodine excretion (urinary iodine excretion <100 μg/L) was common in anemic and iron deficient children.
Conclusions
Iron deficiency and anemia are common in Nepalese children, whereas, iodine nutrition is more than adequate. Low urinary iodine excretion was common in iron deficiency and anemia.
Similar content being viewed by others
References
Arlappa N, Laxmaiah A, Balakrishna N, et al. Micronutrient deficiency disorders among the rural childrenof West Bengal, India. Ann Hum Biol. 2011;38:281–9.
Diaz JR, de las Cagigas, Rodriguez R. Micronutrient deficiencies in developing and affluent countries. Eur J Clin Nutr. 2003;57:S70–2.
Triggiani V, Tafaro E, Giagulli VA, et al. Role of iodine, selenium and other micronutrients in thyroid function and disorders. Endocr Metab Immune Disord Drug Targets. 2009;9:277–94.
Nepal Demographic and Health Survey 2006. Kathmandu, Nepal: Ministry of Health and Population, New ERA, and Macro International Inc; May 2007.
Khatiwada S, Gelal B, Gautam S, et al. Anemia among school children in eastern Nepal. J Trop Pediatr. 2015. doi:10.1093/tropej/fmv016.
Nepal AK, Khatiwada S, Shakya PR, et al. Iodine status after iodized salt supplementation in school children of eastern Nepal. Southeast Asian J Trop Med Public Health. 2013;44:1072–8.
Zimmermann MB, Kohrle J. The impact of iron and selenium deficiencies on iodine and thyroid metabolism: biochemistry and relevance to public health. Thyroid. 2002;12:867–78.
Bain BJ, Lewis SM, Bates I. Basic haematological techniques. In: Lewis SM, Bain BJ, Bates I, editors. Dacie and Lewis Practical Hematology. 10th ed. Germany. Churchill Livingstone Elsevier; 2006. p. 25–54.
Ohashi T, Yamaki M, Pandav CS, Karmarkar MG, Irie M. Simple microplate method for determination of urinary iodine. Clin Chem. 2000;46:529–36.
Worwood M Iron deficiency anemia and iron overload. In: Lewis SM, Bain BJ, Bates I, editors. Dacie and Lewis Practical Hematology. 10th ed. Germany: Churchill Livingstone Elsevier; 2006. p. 132–60.
World Health Organization. Assessment of iodine deficiency disorders and monitoring their elimination: a guide for programme managers. 3rd ed. Geneva: World Health Organization; 2007. viii, 99 p.
Zimmermann MB, Hurrell RF. Nutritional iron deficiency. Lancet. 2007;370:511–20.
Rivera JA, Hotz C, González-Cossío T, Neufeld L, García-Guerra A. The effect of micronutrient deficiencies on child growth: a review of results from community-based supplementation trials. J Nutr. 2003;133:4010S–20.
National Nutrition Policy and Strategy. Kathmandu: Nutrition Section, Child Health Division, Department of Health Services, Ministry of Health and Population, Nepal; 2004 Dec. 58p.
Siegel EH, Stoltzfus RJ, Khatry SK, LeClerq S, Katz J, Tielsch JM. Epidemiology of anemia among 4 to 17 month children living in South Central Nepal. Eur J Clin Nutr. 2006;60:228–35.
Khatiwada S, Gelal B, Tamang MK, Kc R, Singh S, Lamsal M, Baral N. Iodized salt use and salt iodine content among household salts from six districts of eastern Nepal. J Nepal Health Res Counc. 2014;12:191–4.
Khatiwada S, Gelal B, Shakya PR, Lamsal M, Baral N. Urinary iodine excretion among Nepalese school children in terai region. Indian J Pediatr. 2015. doi:10.1007/s12098-015-1755-x.
Dreyfuss ML, Stoltzfus RJ, Shrestha JB, et al. Hookworms, malaria and vitamin a deficiency contribute to anemia and iron deficiency among pregnant women in the plains of Nepal. J Nutr. 2000;130:2527–36.
Hess SY. The impact of common micronutrient deficiencies on iodine and thyroid metabolism: the evidence from human studies. Best Pract Res Clin Endocrinol Metab. 2010;24:117–32.
Acknowledgments
The authors kindly acknowledge the B P Koirala Institute of Health Sciences (BPKIHS) for providing financial assistance and resources for the study.
Contributions
SK, ML, BG, AKN and NB designed the study. SK, BG and SG performed the field study and laboratory analysis. SK wrote the manuscript. ML, BG, AKN, DB and NB reviewed the manuscript. All authors read and approved the final version of manuscript. NB will act as guarantor for this paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
None.
Source of Funding
This study was supported by Nepal India Corpus fund through the Institute Advisory Authority of B P Koirala Institute of Health Sciences (BPKIHS).
Rights and permissions
About this article
Cite this article
Khatiwada, S., Lamsal, M., Gelal, B. et al. Anemia, Iron Deficiency and Iodine Deficiency among Nepalese School Children. Indian J Pediatr 83, 617–621 (2016). https://doi.org/10.1007/s12098-015-1924-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-015-1924-y