Abstract
Objective
To assess the clinical and demographic profile of Systemic Inflammatory Response Syndrome (SIRS) and sepsis, among newly admitted children in different age groups in a hospital in North India.
Methods
This prospective study was conducted at a referral care centre in Northern India. All children, age group 0 to <18 y, admitted on days selected for study were screened and those with abnormal temperature and abnormal leukocyte count were included for further assessment. A total of twenty “24 h” periods were randomly chosen during the study period. Patients were assessed according to age specific vital signs and laboratory values to diagnose Systemic Inflammatory Response Syndrome (SIRS) and sepsis and to gain clinical and demographic data. The criteria laid at International consensus conference, 2002, were used to define patients as SIRS, Sepsis, Severe sepsis and Septic shock.
Results
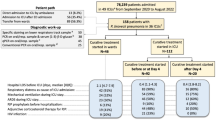
During the study period, a total of 865 patients were screened for SIRS. Prevalence of SIRS amongst hospitalised children was 23 % (n = 201). Seventy nine percent (n = 159) of patients had infection associated SIRS and 21 % (42) had non-infective SIRS. Sixty four percent (n = 129) SIRS patients had uncomplicated sepsis, 15 % (n = 30) patients fulfilled criteria for severe sepsis. Out of the latter 30, 19 had septic shock. Organ dysfunction in SIRS was noted in 25 % (n = 51). 37.25 % (n = 19) had multiple organ dysfunction syndrome (MODS). The most common organism isolated was Staphylococcus aureus (n = 9). Focus of infection in majority was pulmonary (44 %). Mean duration of antibiotic therapy and hospital stay in the SIRS group were 6.4 and 6.5 d respectively. In the group without SIRS, mean duration were 2.44 d and 3.07 d respectively The differences were statistically significant.
Conclusions
In conclusion, the proportion of sepsis contributing to SIRS is high in a tertiary care hospital. Therefore rapid recognition of SIRS is essential. Goal directed treatment of sepsis is also important so that high mortality associated with severe sepsis and septic shock are prevented.

Similar content being viewed by others
References
Bone RC, Balk RA, Cerra FB, Dellinger RP, Knaus WA, Schein RM, et al. Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Chest. 1992;101:1644–55.
Goldstein B, Giroir B, Randolph A. International pediatric sepsis consensus conference: definitions for sepsis and organ dysfunction in pediatrics. Pediatric Crit Care Med. 2005;6:2–8.
Shann F, Mackenzie A. Comparison of rectal, axillary and forehead temperature. Arch Pediatr Adolesc Med. 1996;150:74–8.
Craig JV, Lancaster GA, Williamson PR, Smyth RL. Temperature measured at the axilla compared with rectum in children and young people: Systematic review. BMJ. 2000;320:1174–8.
Rangel- Frausto MS, Pittet D, Costigan M, Hwang T, Davis CS, Wenzel RP. The natural history of the systemic inflammatory response syndrome (SIRS). JAMA. 1995;273:117–23.
Shibata K, Funada H. The epidemiology of SIRS and sepsis in Japan. [Article in Japanese]. Nippon Rinsho. 2004;62:2184–8.
Brun-Buisson C. The epidemiology of systemic inflammatory response. Intensive Care Med. 2000;26:S64–74.
Proulx F, Fayon M, Farrell CA, Lacorix J, Gauthier M. Epidemiology of sepsis and multiple organ dysfunction syndrome in children. Chest. 1996;109:1033–7.
Carvalho PRA, Feldens L, Seitz EE, Rocha T, Soledada M, Trotta A. Prevalence of systemic inflammatory syndromes at a tertiary pediatric intensive care unit. J Pediatr (Rio J). 2005;81:143–8.
Watson RS, Carcillo JA, Linde-Zwirble WT, Clermont G, Lidicker J, Angus DC. The epidemiology of severe sepsis in children in the United States. Am J Respir Crit Care Med. 2003;167:695–701.
Babay HA, Twum-Danso, Kambal AM, AL- Otaibi FE. Blood stream infections in pediatric patients. Saudi Med J. 2005;26:1555–61.
Onipeda AO, Onayade AA, Elusiyan JB, Obiajunwan PO, Ogundare EO, Olaniran OO, et al. Invasive bacteria isolated from children with severe infections in a Nigerian hospital. J Infect Dec Ctries. 2009;3:429–36.
Prabhu K, Bhat S, Rao S. Bacteriologic profile and antibiogram of blood culture isolates in a pediatric care unit. J Lab Phys. 2010;2:85–8.
Bossink AW, Groeneveld AB, Hack CA, Thijs LG. Prediction of mortality in febrile medical patients. Chest. 1998;113:1533–41.
Zaragoza R, Artero A, Camarena JJ, Sancho S, Gonzalez R, Nogueira JM. The influence of inadequate empirical antimicrobial treatment on patients with bloodstream infections in an intensive care unit. Clin Microbiol Infect. 2003;9:412–8.
Hodgkin KE, Moss M. The epidemiology of sepsis. Curr Pharm Design. 2008;14:1833–9.
Pavare J, Grope I, Gardovska D. Prevalence of SIRS in hospitalised children. BMC Pediatr. 2009;9:25.
Contributions
SG conducted the work under the guidance of KA. UAQ and ZHM wrote the manuscript. KA will act as guarantor for this paper.
Conflict of Interest
None.
Source of Funding
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ganjoo, S., Ahmad, K., Qureshi, U.A. et al. Clinical Epidemiology of SIRS and Sepsis in Newly Admitted Children. Indian J Pediatr 82, 698–702 (2015). https://doi.org/10.1007/s12098-014-1618-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-014-1618-x