Abstract
Objective
To demonstrate the effectiveness of the hour-specific serum bilirubin nomogram, described by Bhutani et al, in predicting significant hyperbilirubinemia in term Turkish newborns.
Methods
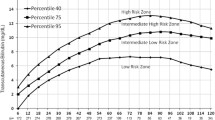
A total of 217 healthy term newborns without signs of hemolysis were enrolled. Serum bilirubin levels were obtained at discharge and whenever visible jaundice was observed. According to the percentile-based hour specific bilirubin nomogram the babies were grouped into four categories (high, high/low, intermediate or low risk zone). All babies were followed up for hyperbilirubinemia and examined between 7 to 10 days of life and a bilirubin level was obtained when jaundice was observed.
Results
The mean predischarge bilirubin of cases was 9.71±3.4mg/dl. Thirty six patients (16.6%) received phototherapy while none of the cases had an exchange transfusion. The distribution of cases according to the high risk, intermediate, low/high, and low zones and the percentage of babies who received phototherapy were, 21(63.6%), 10(38.5%), 3(4.5%) and 2(2.2%), respectively. The risk of phototherapy decreased to 0.35 times for every increasing week of gestational age. Babies in the high intermediate and high risk zones were more likely to receive phototherapy (OR:24.5 and OR:83.6)
Conclusion
The hour-specific serum bilirubin nomogram described by Bhutani et al. predicted clinically significant hyperbilirubinemia in Turkish term newborns.
Similar content being viewed by others
References
Bhutani VK, Johnson L, Sivieri EM. Predictive ability of predischarge hour-specific bilirubin for subsequent significant hyperbilirubinemia in healthy term and near-term newborns. Pediatrics 1999; 103: 6–14
American Academy of Pediatrics. Practice parameters: management of hyperbilirubinemia in healthy term newborns. Pediatrics 1994; 94: 558–565.
Bhutani VK, Johnson LH, Keren R. Diagnosis and management of hyperbilirubinemia in the term neonate: for a safer first week. Pediatr Clin N Am 2004; 51;843–861.
Chou SC, Palmer RH, Ezhuthachan S, Newnan C, Pradell-Boyd B, Maisels MJ et al. Management of hyperbilirubinemia in newborns: measuring performance by using a benchmarking model. Pediatrics 2003; 112: 1264–1274.
Sarýcý SÜ, Serdar MA, Korkmaz A, Erdem G, Oran O, Tekinalp G, Yurdakök M, Yigit S. Incidence, course, and prediction of hyperbilirubinemia in near-term and term newborns. Pediatrics 2004; 113: 775–780.
Soorani I, Woltil HA, Hadders M. Are moderate degrees of hyperbilirubinemia in healthy term neonates really safe for the brain? Pediatr Res 2001; 50: 701–705.
Braveman P, Egerter S, Pearl M, Marchi K, Miller C. Problems associated with early discharge of newborn infants. Early discharge of newborns and mothers: a critical review of the literature. Pediatrics 1995; 96: 716–726.
Grupp-Phelan J, Taylor JA, Liu LL, Davis RL. Early newborn hospital discharge and readmission for mild and severe jaundice. Arch Pediatr Adolesc Med 1999;153:1283–1288.
Zimmerman DR, Klinger G, Merlob P. Early discharge after delivery. A study of safety and risk factors. Scientific World Journal 2003; 3:1363–1369.
Alpay F, Sarici Ü, Tosuncuk D, Serdar MA, Inanç N, Gökçay E. The Value of first-day bilirubin measurement in predicting the development of significant hyperbiliru-binemia in healthy term newborns. Pediatrics 2000; 106:e 2–e16.
Keren R, Bhutani VK, Luan X, Nihtianova S, Cnaan A, Schwartz JS. Identifying newborns at risk of significant hyperbilirubinemia: a comparison of two recommended approaches. Arch Dis Child 2005; 90: 415–421.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hülya, B., Eren, Ö. & Ahmet, T. Is the hour-specific bilirubin nomogram suitable for predicting hyperbilirubinemia. Indian J Pediatr 75, 447–450 (2008). https://doi.org/10.1007/s12098-008-0248-6
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s12098-008-0248-6