Abstract
Objective
The aim of this study is to outline a management algorithm to ensure effective teamwork in decreasing morbidity and mortality in pediatric Foreign-Body Aspirations (FBA). Furthermore, the role of flexible bronchoscopy when compared to rigid bronchoscopy in FBA was evaluated.
Methods
Charts of patients with suspected FBA from October 1999 to September 2006 were reviewed and data with regards to the history, presenting symptoms, diagnostics and therapeutic tactics, was collected.
Results
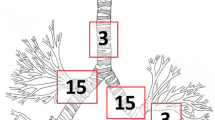
A total of 77 children with suspicion of FBA were managed in the 7 year period. Bronchoscopies were performed in 63 patients and in 26 foreign-bodies (FB) were found and extracted. At referral, 53 patients did not present acute respiratory symptoms, but had a positive history of FBA, and in 13 FB were found. Despite negative chest x-rays in 55 patients, FB were found in 8. Rigid bronchoscopy was performed in 53 and flexible in 10 patients. In 3 out of 10 patients who had undergone flexible bronchoscopy a FB was identified, the extraction of which was performed using a rigid bronchoscope.
Conclusion
Clinical and radiological findings in children with typical history of suspected FBA are not enough to confirm the presence of FB. Successful management with an extremely low rate of morbidity and no mortality was observed using the algorithm used at our center. Flexible bronchoscopy reduces the chances of airway tract injury; however a rigid bronchoscope is necessary for FB removal.
Similar content being viewed by others
References
Barrios Fontoba JE, Gutierrez C, Lluna J, Vila JJ, Poquet J, Ruiz-Company S. Bronchial foreign body: Should bronchoscopy be performed in all patients with choking crisis. Pediatr Surg Int 1997; 12: 118–120.
Black RE, Johnson DG, Matlak ME. Bronchoscopic removal of aspirated foreign bodies in children. J Pediatr Surg 1994; 29: 682–684.
Ciftci AO, Bingol-Kologlu M, Senocak ME, Tanyel FC, Buyukpamukcu AR. Bronchoscopy for evaluation of foreign body aspiration in children. J Pediatr Surg 2003; 8: 1170–1176.
Girardi G, Contador MM, Castro-Rodriguez JA. Two new radiological findings to improve the diagnosis of bronchial foreign body aspiration in children. Pediatr Pulmonol 2004; 38: 261–264.
Karakoc F, Karadag B, Akbenlioglu G, Ersu R, Yildizeli B, Yüksel M et al. Foreign body aspiration: what is the outcome? Pediatr Pulmunol 2002; 34: 30–36.
Metrangelo S, Monetti C, Meneghini L, Zadra N, Giusti F. Eight years’ experience with foreign body aspiration in children: what is really important for a timely diagnosis? J Pediatr Surg 1999; 34: 1229–1231.
Pasaoglu I, Dogan R, Demircin M, Hatipoglu A, Bozer AY. Bronchoscopic removal of foreign bodies in children: retrospective analysis of 822 cases. Thorac Cardiovasc Surg 1990; 39: 95–98.
Hilliard T, Sim R, Saunders M, Hewer SL, Henderson J. Delayed diagnosis of foreign body aspiration in children. Emerg Med 2003; 20: 100–101
Mu L, He P, Sun D. Inhalation of foreign bodies in Chinese children. A review of 400 cases. Laryngoscope 1991; 101: 778–782.
Tokar B, Ozkan R, Ilhan H. Tracheobronchial foreign bodies in children: importance of accurate history and plain chest radiography in delayed presentation. Clin Radiol 2004; 59: 609–615.
Mu LC, Sun DQ, He P. Radiological diagnosis of aspirated foreign bodiesin children: review of 343 cases. J Laryngol Otol 1990; 104: 778–782.
Steen KH, Zimmermann T. Tracheobronchial aspiration of foreign bodies in children: a study of 94 cases. Laryngoscope 1990; 100: 525–530.
Lange S, Walsh. Radiology of chest diseases, 2nd ed. Stuttgart: Thieme pp. 132–133, 1998.
Oguz F, Citak A, Unuvar E, Sidal M. Airway foreign bodies in childhood. Int J Pediatr Otorhinolaryngol 2000; 52: 11–16.
Mantel K, Butenandt I. Tracheobronchial foreign body aspiration in childhood. Eur J Pediatr 1986; 145: 211–216.
Zaytoun GM, Rouadi PW, Baki DH. Endoscopic management of foreign bodies in tracheobronchial tree: Predictive factors for complications. Otolaryngol Head Neck Surg 2000; 123: 311–316.
Zerella JT, Dimler M, McGil LC, Pippus KJ. Foreign body aspiration in children: Value of radiography and complications of bronchoscopy. J Pediatr Surg 1998; 33: 1651–1654.
Hight DW, Philippart AI, Hertzler JH. The treatment of retained peripheral foreign bodies in the pediatric airway. J Pediatr Surg 1981; 16: 694–699.
Johnson DG, Condon VR. Foreign bodies in pediatric patients. Curr Probl Surg 1998; 35: 273–379.
AHA. 2005 American Heart Association (AHA) guidelines for cardiopulmonary resuscitation (CPR) and emergency cardiovascular care (ECC) of pediatric and neonatal patients: pediatric basic life support. Pediatrics 2006; 117: 989–1004.
International Liaison Committee on Resuscitation. The International Liaison Committee on Resuscitation (ILCOR) consensus on science with treatment recommendations for pediatric and neonatal patients: pediatric basic and advanced life support. Pediatrics 2006; 117: 955–977.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zaupa, P., Saxena, A.K., Barounig, A. et al. Management strategies in foreign-body aspiration. Indian J Pediatr 76, 157–161 (2009). https://doi.org/10.1007/s12098-008-0231-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-008-0231-2