Abstract
Objective
To evaluate the utility of Indian adaptation of IMCI algorithm.
Methods
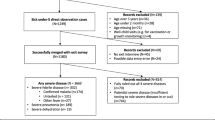
Children presenting to outpatient department (n=169) or casualty (n=140) among 309 cases were assessed and classified as per IMCI algorithm, the final diagnosis made after detailed evaluation and relevant investigations, served as the gold standard. The diagnostic and therapeutic agreements between the gold standard, IMCI and vertical (on the basis of primary presenting complaint) algorithms were computed.
Results
Coexistence of illness was observed in 75% of children as per IMCI algorithm. The mean (SD) number of morbidities as per the Gold standard and IMCI were 1.75 ± 0.75 and 2.19 ± 0.96 respectively. The referral criteria proved useful in predicting hospitalisation with high sensitivity and specificity (99.3% & 97.3%). IMCI algorithm covered majority of recorded illnesses. A total agreement with IMCI was found in 88.4% cases, while total disagreement was seen in 34.5% cases. Corresponding figures for vertical program were 88% and 18.6%. The difference was primarily due to underdiagnosis. The diagnostic discordance of IMCI and gold standard was evident for the cough category due to underdiagnosis of bronchial asthma and bronchiolitis and an overdiagnosis of pneumonia. The IMCI algorithm had a provision for preventive services of immunization (24.5% possibility of availing missed opportunity) and feeding advice.
Conclusions
There is a sound scientific basis for adopting the IMCI approach since: (1) Co-existence of morbidities is a rule rather than exception for sick under-five children. (2) The algorithm provides good sensitivity and specificity for assessing severe illness and (3) IMCI algorithm is superior to vertical disease specific programs. It is, however, important to carefully adapt the generic IMCI algorithm to reflect the local morbidity profile.
Similar content being viewed by others
References
Technical Seminar-Acute respiratory infections. World Health Organization. Department of Child and Adolescent Health and Development. Geneva, WHO 2001: 1–23.
World Health Organization. World Health Report 1999: making a difference. Geneva, WHO, 1999.
Fagbule D, Kalu A. Case management by community health workers of children with acute respiratory infection: Implications for national ARI control programme. J Trop Med Hyg 1995; 98: 241–224.
Lambrechts T, Bryce J, Orinda V. Integrated Management of Childhood Illness: a summary of first experiences. Bull WHO 1999; 77: 582–594.
Patwari AK, Raina N. Integrated Management of Childhood Illness (IMCI): A Robust Strategy. Indian J Pediatr 2002; 69: 41–48.
Pelletier DL, Frongillo EA, Schroeder DG, Habicht JP. The effects of malnutrition on child mortality in developing countries. Bull WHO 1995; 73: 443–448.
Kalter HD, Schillinger JA, Hossain M, Brunhum G, Saha S, de Wit V et al. Identifying sick children requiring referral to hospital in Bangladesh. Bull WHO 1997; 75 (Suppl I): 65–75.
Kolstad PR, Brunham G, Kalter HD, Keny-Mugisha N, Black RE. The Integrated Management of Childhood Illness in western Uganda. Bull WHO 1997; 75 (Suppl 1): 77–85.
Perkins BA, Zucker JR, Oteino J, Jagan HS, Paxton L, Redd SC et al. Evaluation of an algorithm for integrated management of childhood illness in an area of Kenya with high malaria transmission. Bull WHO 1997; 75 (Suppl 1): 33–42.
Weber MW, Mulholland EK, Jaffar S, Troedsson H, Gove S, Greenwood BM. Evaluation of an algorithm for the integrated management of childhood illness in an area with seasonal malaria in the Gambia. Bull WHO 1997; 75 (Suppl 1): 25–32.
Paxton LA, Redd SC, Steketee RW, Oteino JO, Nahlen B. An evaluation of clinical indicators of severe pediatric illness. Bull WHO 1996; 74: 613–618.
Simoes EAF, Desta T, Tessema T, Gertresellassie T, Dagnew M, Gove S. Performance of health workers after training in Integrated Management of childhood illness in Gondar, Ethiopia. Bull WHO 1997; 75 (Suppl 1): 43–53.
Shah D, Sachdev HPS. Evaluation of the WHO/UNICEF algorithms for integrated management of childhood illness between the age of two months and five years. Indian Pediatr 1999; 36: 767–777.
Gove S et al. Integrated management of childhood illness: Conclusions. WHO. Division of Child Health & Development. Bull WHO 1997; 75 (Suppl 1): 119–128.
Costello A. Is India ready for the Integrated Management of Childhood Illness strategy? Indian Pediatr 1999; 36: 759–762.
Lulseged S. Integrated management of childhood illness. A review of the Ethiopian experience and prospects for child health. Ethiop Med J 2002; 40: 187–200.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kundra, S., Singh, T. & Chhatwal, J. Utility of Indian adaptation of Integrated Management of Childhood Illness (IMCI) algorithm. Indian J Pediatr 75, 781–785 (2008). https://doi.org/10.1007/s12098-008-0103-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-008-0103-9