Abstract
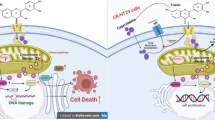
Colorectal cancer (CRC) commonly leads to cancer deaths and is often diagnosed at advanced stages. It also faces difficulties due to the poor results of conventional treatments such as surgery, chemotherapy, and radiotherapy. Copper is a mineral nutrient whose intrinsic properties have a two-way effect on the production and treatment of cancer. Copper's redox properties allow it to be used in developing anti-cancer drugs, while its potential toxicity leads to oxidative stress and even cancer. Copper status is closely related to colorectal tumors’ proliferation and metastasis. The study of the mechanisms of copper homeostasis, cuproplasia, and cuproptosis due to altered copper status plays a crucial role in developing anticancer drugs. Therefore, targeting alteration of copper status becomes a potential option for treating colorectal cancer. This review summarizes the mechanisms by which altered copper status causes CRC progression and emphasizes the potential of regulating copper status in treating CRC.



Similar content being viewed by others
Data availability
No new data were generated or analysed in support of this research.
Abbreviations
- CRC:
-
Colorectal cancer
- IECs:
-
Intestinal epithelial cells
- CTR1:
-
Copper Transporter 1
- SLC31A1:
-
Solute carrier family 31 member 1
- ATOX1:
-
Antioxidant-protein 1
- CCS:
-
Copper chaperone for SOD1
- SCO:
-
Synthesis of cytochrome c oxidase
- COX:
-
Cytochrome c oxidase
- TGN:
-
Trans-Golgi network
- PDE3B:
-
Phosphodiesterase 3B
- MEK1:
-
Mitogen-activated protein kinase 1
- ERK1:
-
Extracellular signal-regulated kinase 1
- ULK1:
-
Unc51-like kinase 1
- ROS:
-
Reactive oxygen species
- ES:
-
Elesclomol
- ETC:
-
Electron transport chain
- TCA:
-
Tricarboxylic acid
- EMT:
-
Epithelial-to-mesenchymal transition
- ECM:
-
Extracellular matrix
- LOX:
-
Lysyl oxidase
- FAK1:
-
Focal adhesion kinase 1
- HRE:
-
Hypoxia response element
- VEGF:
-
Vascular endothelial growth factor
- TGF-β:
-
Transforming growth factor beta
- NO:
-
Nitric oxide
- eNOS:
-
Endothelial nitric oxide synthase
- HUVEC:
-
Human umbilical vein endothelial cells
- GPER:
-
G protein estrogen receptor
- TTM:
-
Tetrathiomolybdate
- D-pen:
-
D-penicillamine
- TPEN:
-
N, N, N', N’-tetrakis-[2-pyridylmethyl]-ethylenediamine
- DSF:
-
Disulfiram
- CQ:
-
Clioquinol
- UPS:
-
Ubiquitin proteasome system
- ALDH:
-
Acetaldehyde dehydrogenase
- ULK1:
-
Unc-51-like autophagy-activated kinase 1
- XIAP:
-
X-linked inhibitor of apoptosis protein
- GTSM:
-
Glyoxal-bis (N4-methylthiosemicarbazone)
- ATSM:
-
Diacetyl-bis (N4-methylthiosemicarbazone)
- CDKN1A:
-
Cell cycle protein-dependent kinase inhibitor 1A
- ER:
-
Endoplasmic reticulum
- UPR:
-
Unfolded protein response
References
Siegel RL, Miller KD, Fuchs HE, Jemal A. Cancer statistics, 2022. CA Cancer J Clin. 2022;72(1):7–33.
Terzić J, Grivennikov S, Karin E, Karin M. Inflammation and colon cancer. Gastroenterology. 2010;138(6):2101-2114.e2105.
Johdi NA, Sukor NF. Colorectal cancer immunotherapy: options and strategies. Front Immunol. 2020;11:1624.
Arredondo M, Núñez MT. Iron and copper metabolism. Mol Asp Med. 2005;26(4–5):313–27.
Shanbhag VC, Gudekar N, Jasmer K, Papageorgiou C, Singh K, Petris MJ. Copper metabolism as a unique vulnerability in cancer. Biochim Biophys Acta Mol Cell Res. 2021;1868(2): 118893.
Garber K. Cancer’s copper connections. Science. 2015;349(6244):129.
Robinson NJ, Winge DR. Copper metallochaperones. Annu Rev Biochem. 2010;79:537–62.
De Luca A, Barile A, Arciello M, Rossi L. Copper homeostasis as target of both consolidated and innovative strategies of anti-tumor therapy. J Trace Elem Med Biol. 2019;55:204–13.
Ruiz LM, Libedinsky A, Elorza AA. Role of copper on mitochondrial function and metabolism. Front Mol Biosci. 2021;8: 711227.
Tong X, Tang R, Xiao M, Xu J, Wang W, Zhang B, et al. Targeting cell death pathways for cancer therapy: recent developments in necroptosis, pyroptosis, ferroptosis, and cuproptosis research. J Hematol Oncol. 2022;15(1):174.
Waggoner DJ, Bartnikas TB, Gitlin JD. The role of copper in neurodegenerative disease. Neurobiol Dis. 1999;6(4):221–30.
Kidane TZ, Farhad R, Lee KJ, Santos A, Russo E, Linder MC. Uptake of copper from plasma proteins in cells where expression of CTR1 has been modulated. Biometals. 2012;25(4):697–709.
Ohrvik H, Thiele DJ. How copper traverses cellular membranes through the mammalian copper transporter 1, Ctr1. Ann N Y Acad Sci. 2014;1314:32–41.
Molloy SA, Kaplan JH. Copper-dependent recycling of hCTR1, the human high affinity copper transporter. J Biol Chem. 2009;284(43):29704–13.
Bertinato J, L’Abbé MR. Copper modulates the degradation of copper chaperone for Cu, Zn superoxide dismutase by the 26 S proteosome. J Biol Chem. 2003;278(37):35071–8.
Horn D, Barrientos A. Mitochondrial copper metabolism and delivery to cytochrome c oxidase. IUBMB Life. 2008;60(7):421–9.
Leary SC. Redox regulation of SCO protein function: controlling copper at a mitochondrial crossroad. Antioxid Redox Signal. 2010;13(9):1403–16.
La Fontaine S, Mercer JF. Trafficking of the copper-ATPases, ATP7A and ATP7B: role in copper homeostasis. Arch Biochem Biophys. 2007;463(2):149–67.
Arnesano F, Banci L, Bertini I, Thompsett AR. Solution structure of CopC: a cupredoxin-like protein involved in copper homeostasis. Structure. 2002;10(10):1337–47.
Song Y, Chen S, Li L, Zeng Y, Hu X. The hypopigmentation mechanism of tyrosinase inhibitory peptides derived from food proteins: an overview. Molecules. 2022;27(9):2710.
Krishnamoorthy L, Cotruvo JA Jr, Chan J, Kaluarachchi H, Muchenditsi A, Pendyala VS, et al. Copper regulates cyclic-AMP-dependent lipolysis. Nat Chem Biol. 2016;12(8):586–92.
Turski ML, Brady DC, Kim HJ, Kim BE, Nose Y, Counter CM, et al. A novel role for copper in Ras/mitogen-activated protein kinase signaling. Mol Cell Biol. 2012;32(7):1284–95.
Tsang T, Posimo JM, Gudiel AA, Cicchini M, Feldser DM, Brady DC. Copper is an essential regulator of the autophagic kinases ULK1/2 to drive lung adenocarcinoma. Nat Cell Biol. 2020;22(4):412–24.
Ge EJ, Bush AI, Casini A, Cobine PA, Cross JR, DeNicola GM, et al. Connecting copper and cancer: from transition metal signalling to metalloplasia. Nat Rev Cancer. 2022;22(2):102–13.
Lelièvre P, Sancey L, Coll JL, Deniaud A, Busser B. The multifaceted roles of copper in cancer: a trace metal element with dysregulated metabolism, but also a target or a bullet for therapy. Cancers (Basel). 2020;12(12):3594.
Tsvetkov P, Coy S, Petrova B, Dreishpoon M, Verma A, Abdusamad M, et al. Copper induces cell death by targeting lipoylated TCA cycle proteins. Science. 2022;375(6586):1254–61.
Adelmann CH, Wang T, Sabatini DM, Lander ES. Genome-wide CRISPR/Cas9 screening for identification of cancer genes in cell lines. Methods Mol Biol. 2019;1907:125–36.
Urra FA, Weiss-López B, Araya-Maturana R. Determinants of anti-cancer effect of mitochondrial electron transport chain inhibitors: bioenergetic profile and metabolic flexibility of cancer cells. Curr Pharm Des. 2016;22(39):5998–6008.
Baszuk P, Marciniak W, Derkacz R, Jakubowska A, Cybulski C, Gronwald J, et al. Blood copper levels and the occurrence of colorectal cancer in Poland. Biomedicines. 2021;9(11):1628.
Ranjbary AG, Mehrzad J, Dehghani H, Abdollahi A, Hosseinkhani S. Variation in blood and colorectal epithelia’s key trace elements along with expression of mismatch repair proteins from localized and metastatic colorectal cancer patients. Biol Trace Elem Res. 2020;194(1):66–75.
Lossow K, Schwarz M, Kipp AP. Are trace element concentrations suitable biomarkers for the diagnosis of cancer? Redox Biol. 2021;42: 101900.
Itoh S, Kim HW, Nakagawa O, Ozumi K, Lessner SM, Aoki H, et al. Novel role of antioxidant-1 (Atox1) as a copper-dependent transcription factor involved in cell proliferation. J Biol Chem. 2008;283(14):9157–67.
Wang J, Luo C, Shan C, You Q, Lu J, Elf S, et al. Inhibition of human copper trafficking by a small molecule significantly attenuates cancer cell proliferation. Nat Chem. 2015;7(12):968–79.
Jana A, Das A, Krett NL, Guzman G, Thomas A, Mancinelli G, et al. Nuclear translocation of Atox1 potentiates activin A-induced cell migration and colony formation in colon cancer. PLoS ONE. 2020;15(1): e0227916.
Aubert L, Nandagopal N, Steinhart Z, Lavoie G, Nourreddine S, Berman J, et al. Copper bioavailability is a KRAS-specific vulnerability in colorectal cancer. Nat Commun. 2020;11(1):3701.
Barresi V, Trovato-Salinaro A, Spampinato G, Musso N, Castorina S, Rizzarelli E, et al. Transcriptome analysis of copper homeostasis genes reveals coordinated upregulation of SLC31A1, SCO1, and COX11 in colorectal cancer. FEBS Open Bio. 2016;6(8):794–806.
Liao Y, Zhao J, Bulek K, Tang F, Chen X, Cai G, et al. Inflammation mobilizes copper metabolism to promote colon tumorigenesis via an IL-17-STEAP4-XIAP axis. Nat Commun. 2020;11(1):900.
Nenkov M, Ma Y, Gaßler N, Chen Y. Metabolic reprogramming of colorectal cancer cells and the microenvironment: implication for therapy. Int J Mol Sci. 2021;22(12):6262.
Dongre A, Weinberg RA. New insights into the mechanisms of epithelial-mesenchymal transition and implications for cancer. Nat Rev Mol Cell Biol. 2019;20(2):69–84.
El-Haibi CP, Bell GW, Zhang J, Collmann AY, Wood D, Scherber CM, et al. Critical role for lysyl oxidase in mesenchymal stem cell-driven breast cancer malignancy. Proc Natl Acad Sci U S A. 2012;109(43):17460–5.
Baker AM, Bird D, Lang G, Cox TR, Erler JT. Lysyl oxidase enzymatic function increases stiffness to drive colorectal cancer progression through FAK. Oncogene. 2013;32(14):1863–8.
Feng W, Ye F, Xue W, Zhou Z, Kang YJ. Copper regulation of hypoxia-inducible factor-1 activity. Mol Pharmacol. 2009;75(1):174–82.
Xiao Q, Ge G. Lysyl oxidase, extracellular matrix remodeling and cancer metastasis. Cancer Microenviron. 2012;5(3):261–73.
Baker AM, Cox TR, Bird D, Lang G, Murray GI, Sun XF, et al. The role of lysyl oxidase in SRC-dependent proliferation and metastasis of colorectal cancer. J Natl Cancer Inst. 2011;103(5):407–24.
Liu G, Zhan W, Guo W, Hu F, Qin J, Li R, et al. MELK accelerates the progression of colorectal cancer via activating the FAK/Src pathway. Biochem Genet. 2020;58(5):771–82.
Wong CC, Gilkes DM, Zhang H, Chen J, Wei H, Chaturvedi P, et al. Hypoxia-inducible factor 1 is a master regulator of breast cancer metastatic niche formation. Proc Natl Acad Sci U S A. 2011;108(39):16369–74.
Pez F, Dayan F, Durivault J, Kaniewski B, Aimond G, Le Provost GS, et al. The HIF-1-inducible lysyl oxidase activates HIF-1 via the Akt pathway in a positive regulation loop and synergizes with HIF-1 in promoting tumor cell growth. Cancer Res. 2011;71(5):1647–57.
Zhao Y, Adjei AA. Targeting angiogenesis in cancer therapy: moving beyond vascular endothelial growth factor. Oncologist. 2015;20(6):660–73.
Martin F, Linden T, Katschinski DM, Oehme F, Flamme I, Mukhopadhyay CK, et al. Copper-dependent activation of hypoxia-inducible factor (HIF)-1: implications for ceruloplasmin regulation. Blood. 2005;105(12):4613–9.
Urso E, Maffia M. Behind the link between copper and angiogenesis: established mechanisms and an overview on the role of vascular copper transport systems. J Vasc Res. 2015;52(3):172–96.
Rigiracciolo DC, Scarpelli A, Lappano R, Pisano A, Santolla MF, De Marco P, et al. Copper activates HIF-1α/GPER/VEGF signalling in cancer cells. Oncotarget. 2015;6(33):34158–77.
Narayanan IG, Natarajan SK. Peptides derived from histidine and methionine-rich regions of copper transporter 1 exhibit anti-angiogenic property by chelating extracellular Cu. Chem Biol Drug Des. 2018;91(3):797–804.
Chen GF, Sudhahar V, Youn SW, Das A, Cho J, Kamiya T, et al. Copper transport protein antioxidant-1 promotes inflammatory neovascularization via chaperone and transcription factor function. Sci Rep. 2015;5:14780.
Narayanan G, Bharathidevi SR, Vuyyuru H, Muthuvel B, Konerirajapuram Natrajan S. CTR1 silencing inhibits angiogenesis by limiting copper entry into endothelial cells. PLoS ONE. 2013;8(9): e71982.
Weekley CM, He C. Developing drugs targeting transition metal homeostasis. Curr Opin Chem Biol. 2017;37:26–32.
Sammons S, Brady D, Vahdat L, Salama AK. Copper suppression as cancer therapy: the rationale for copper chelating agents in BRAF(V600) mutated melanoma. Melanoma Manag. 2016;3(3):207–16.
EASL Clinical Practice Guidelines. Wilson’s disease. J Hepatol. 2012;56(3):671–85.
Wadhwa S, Mumper RJ. D-penicillamine and other low molecular weight thiols: review of anticancer effects and related mechanisms. Cancer Lett. 2013;337(1):8–21.
Kim KK, Abelman S, Yano N, Ribeiro JR, Singh RK, Tipping M, et al. Tetrathiomolybdate inhibits mitochondrial complex IV and mediates degradation of hypoxia-inducible factor-1α in cancer cells. Sci Rep. 2015;5:14296.
Alvarez HM, Xue Y, Robinson CD, Canalizo-Hernández MA, Marvin RG, Kelly RA, et al. Tetrathiomolybdate inhibits copper trafficking proteins through metal cluster formation. Science. 2010;327(5963):331–4.
Baldari S, Di Rocco G, Heffern MC, Su TA, Chang CJ, Toietta G. Effects of copper chelation on BRAF(V600E) positive colon carcinoma cells. Cancers (Basel). 2019;11(5):659.
Gartner EM, Griffith KA, Pan Q, Brewer GJ, Henja GF, Merajver SD, et al. A pilot trial of the anti-angiogenic copper lowering agent tetrathiomolybdate in combination with irinotecan, 5-flurouracil, and leucovorin for metastatic colorectal cancer. Invest New Drugs. 2009;27(2):159–65.
Crowe A, Jackaman C, Beddoes KM, Ricciardo B, Nelson DJ. Rapid copper acquisition by developing murine mesothelioma: decreasing bioavailable copper slows tumor growth, normalizes vessels and promotes T cell infiltration. PLoS ONE. 2013;8(8): e73684.
Yoshiji H, Yoshii J, Kuriyama S, Ikenaka Y, Noguchi R, Yanase K, et al. Combination of copper-chelating agent, trientine, and methotrexate attenuates colorectal carcinoma development and angiogenesis in mice. Oncol Rep. 2005;14(1):213–8.
Fatfat M, Merhi RA, Rahal O, Stoyanovsky DA, Zaki A, Haidar H, et al. Copper chelation selectively kills colon cancer cells through redox cycling and generation of reactive oxygen species. BMC Cancer. 2014;14:527.
Yu N, Zhu H, Yang Y, Tao Y, Tan F, Pei Q, et al. Combination of Fe/Cu -chelators and docosahexaenoic acid: an exploration for the treatment of colorectal cancer. Oncotarget. 2017;8(31):51478–91.
Zhang Z, Wang H, Yan M, Wang H, Zhang C. Novel copper complexes as potential proteasome inhibitors for cancer treatment (Review). Mol Med Rep. 2017;15(1):3–11.
Lewison EF. Spontaneous regression of breast cancer. Prog Clin Biol Res. 1977;12:47–53.
Li H, Wang J, Wu C, Wang L, Chen ZS, Cui W. The combination of disulfiram and copper for cancer treatment. Drug Discov Today. 2020;25(6):1099–108.
Li Y, Wang LH, Zhang HT, Wang YT, Liu S, Zhou WL, et al. Disulfiram combined with copper inhibits metastasis and epithelial-mesenchymal transition in hepatocellular carcinoma through the NF-κB and TGF-β pathways. J Cell Mol Med. 2018;22(1):439–51.
Hu Y, Qian Y, Wei J, Jin T, Kong X, Cao H, et al. The disulfiram/copper complex induces autophagic cell death in colorectal cancer by targeting ULK1. Front Pharmacol. 2021;12: 752825.
Kannappan V, Ali M, Small B, Rajendran G, Elzhenni S, Taj H, et al. Recent advances in repurposing disulfiram and disulfiram derivatives as copper-dependent anticancer agents. Front Mol Biosci. 2021;8: 741316.
Oliveri V. Selective targeting of cancer cells by copper ionophores: an overview. Front Mol Biosci. 2022;9: 841814.
Ding WQ, Liu B, Vaught JL, Yamauchi H, Lind SE. Anticancer activity of the antibiotic clioquinol. Cancer Res. 2005;65(8):3389–95.
Cater MA, Haupt Y. Clioquinol induces cytoplasmic clearance of the X-linked inhibitor of apoptosis protein (XIAP): therapeutic indication for prostate cancer. Biochem J. 2011;436(2):481–91.
Jiang H, Taggart JE, Zhang X, Benbrook DM, Lind SE, Ding WQ. Nitroxoline (8-hydroxy-5-nitroquinoline) is more a potent anti-cancer agent than clioquinol (5-chloro-7-iodo-8-quinoline). Cancer Lett. 2011;312(1):11–7.
Steinbrueck A, Sedgwick AC, Vargas-Zúñiga GI, He XP, Tian H, Sessler JL. Transition metal chelators, pro-chelators, and ionophores as small molecule cancer chemotherapeutic agents. Chem Soc Rev. 2020;49(12):3726–47.
Donnelly PS, Liddell JR, Lim S, Paterson BM, Cater MA, Savva MS, et al. An impaired mitochondrial electron transport chain increases retention of the hypoxia imaging agent diacetylbis(4-methylthiosemicarbazonato)copperII. Proc Natl Acad Sci U S A. 2012;109(1):47–52.
Cater MA, Pearson HB, Wolyniec K, Klaver P, Bilandzic M, Paterson BM, et al. Increasing intracellular bioavailable copper selectively targets prostate cancer cells. ACS Chem Biol. 2013;8(7):1621–31.
Gao W, Huang Z, Duan J, Nice EC, Lin J, Huang C. Elesclomol induces copper-dependent ferroptosis in colorectal cancer cells via degradation of ATP7A. Mol Oncol. 2021;15(12):3527–44.
Santini C, Pellei M, Gandin V, Porchia M, Tisato F, Marzano C. Advances in copper complexes as anticancer agents. Chem Rev. 2014;114(1):815–62.
Chen X, Dou QP, Liu J, Tang D. Targeting ubiquitin-proteasome system with copper complexes for cancer therapy. Front Mol Biosci. 2021;8: 649151.
Obeng EA, Carlson LM, Gutman DM, Harrington WJ Jr, Lee KP, et al. Proteasome inhibitors induce a terminal unfolded protein response in multiple myeloma cells. Blood. 2006;107(12):4907–16.
Liu N, Liu C, Li X, Liao S, Song W, Yang C, et al. A novel proteasome inhibitor suppresses tumor growth via targeting both 19S proteasome deubiquitinases and 20S proteolytic peptidases. Sci Rep. 2014;4:5240.
Chen X, Zhang X, Chen J, Yang Q, Yang L, Xu D, et al. Hinokitiol copper complex inhibits proteasomal deubiquitination and induces paraptosis-like cell death in human cancer cells. Eur J Pharmacol. 2017;815:147–55.
Milacic V, Chen D, Giovagnini L, Diez A, Fregona D, Dou QP. Pyrrolidine dithiocarbamate-zinc(II) and -copper(II) complexes induce apoptosis in tumor cells by inhibiting the proteasomal activity. Toxicol Appl Pharmacol. 2008;231(1):24–33.
Zhang H, Wu JS, Peng F. Potent anticancer activity of pyrrolidine dithiocarbamate-copper complex against cisplatin-resistant neuroblastoma cells. Anticancer Drugs. 2008;19(2):125–32.
Khan R, Khan H, Abdullah Y, Dou QP. Feasibility of repurposing clioquinol for cancer therapy. Recent Pat Anticancer Drug Discov. 2020;15(1):14–31.
Wehbe M, Malhotra AK, Anantha M, Lo C, Dragowska WH, Dos Santos N, et al. Development of a copper-clioquinol formulation suitable for intravenous use. Drug Deliv Transl Res. 2018;8(1):239–51.
Shi X, Chen Z, Wang Y, Guo Z, Wang X. Hypotoxic copper complexes with potent anti-metastatic and anti-angiogenic activities against cancer cells. Dalton Trans. 2018;47(14):5049–54.
Wang T, Liu Y, Fu Y, Huang T, Yang Y, Li S, et al. Antiproliferative activity of di-2-pyridylhydrazone dithiocarbamate acetate partly involved in p53 mediated apoptosis and autophagy. Int J Oncol. 2017;51(6):1909–19.
Schroeder SM, Matsukuma KE, Medici V. Wilson disease and the differential diagnosis of its hepatic manifestations: a narrative review of clinical, laboratory, and liver histological features. Ann Transl Med. 2021;9(17):1394.
Chen L, Min J, Wang F. Copper homeostasis and cuproptosis in health and disease. Signal Transduct Target Ther. 2022;7(1):378.
Acknowledgements
The Figure was created by Figdraw (www.figdraw.com). We thank Home for Researchers editorial team (www.home-forresearchers.com) for language editing service.
Funding
This work was supported by the Graduate Research-Innovation Project in Jiangsu province [No.SJCX21_1644], the Academic Science and Technology Innovation Fund for College Students [No. 202011117056Y], the Social Development-Health Care Project of Yangzhou, Jiangsu Province [No. YZ2021075], and High-level talent “six one projects” top talent scientific research project of Jiangsu Province [No. LGY2019034], the Graduate Research- Innovation Project in Jiangsu province (SJCX22_1816) Social development project of key R & D plan of Jiangsu Provincial Department of science and technology (BE2022773). The funding bodies had no role in the design of the study; in the collection, analysis, and interpretation of the data; and in the writing the manuscript.
Author information
Authors and Affiliations
Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jiang, Z., Sha, G., Zhang, W. et al. The huge potential of targeting copper status in the treatment of colorectal cancer. Clin Transl Oncol 25, 1977–1990 (2023). https://doi.org/10.1007/s12094-023-03107-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-023-03107-7