Abstract
Background
The diagnosis and management of breast cancer with ipsilateral supraclavicular lymph node metastases currently lack any applicable criteria or guidelines (ISLM), and diagnostic and treatment strategies are varied by medical centers. This study aimed to determine the current status of the diagnosis and treatment of breast cancer with ISLM among Chinese patients.
Methods
Data from 30 hospitals on ISLM breast cancer patients between January 1, 2018, and December 31, 2018, were systematically analyzed for the detection rate, clinicopathological characteristics, diagnosis and treatment strategies of breast cancer with ISLM among Chinese patients.
Results
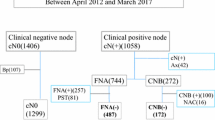
A total of 26,723 women presented with breast cancer in 30 hospitals over the study period. A total of 127 ISLM breast cancer patients were finally enrolled. Synchronous ISLM without distant metastases was present in 0.48% of cases. The diagnosis of patients with 86.6% of ISLM was based on ultrasound examinations. The proportion of ISLM diagnosed by fine-needle aspiration biopsy (FNA) or core-needle biopsy (CNB) before surgery was 16.5% and 37.0%, respectively. Moreover, 45.7% of the ISLM patients had no pathological evidence. Regarding treatment strategies, 69.3% of ISLM patients received neoadjuvant chemotherapy (NAC) for more than 4 cycles, while 15.7% of patients did not receive NAC. 86.6% of ISLM patients underwent a mastectomy, and breast-conserving surgery was performed in 3.9% of ISLM patients. Moreover, 41.7% of ISLM patients received supraclavicular lymph node dissection (SCLD), while 47.2% were not treated with SCLD.
Conclusions
The overall detection rate of breast cancer in patients with ISLM is low in China and varies widely between hospitals. There is no consensus on the optimal diagnosis and treatment of patients with ISLM breast cancer.
Similar content being viewed by others
Data availability
All data generated or analysed during this study are included in this published article.
References
Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A. Global cancer statistics, 2012. CA cancer J Clin. 2015;65:87–108. https://doi.org/10.3322/caac.21262.
Chen W, Zheng R, Baade PD, Zhang S, Zeng H, Bray F, et al. Cancer statistics in China, 2015. CA Cancer J Clin. 2016;66:115–32. https://doi.org/10.3322/caac.21338.
Galper S, Recht A, Silver B, Manola J, Gelman R, Schnitt SJ, et al. Factors associated with regional nodal failure in patients with early stage breast cancer with 0–3 positive axillary nodes following tangential irradiation alone. Int J Radiat Oncol Biol Phys. 1999;45:1157–66.
Recht A, Gray R, Davidson NE, Fowble BL, Solin LJ, Cummings FJ, et al. Locoregional failure 10 years after mastectomy and adjuvant chemotherapy with or without tamoxifen without irradiation: experience of the Eastern cooperative oncology group. J Clin Oncol. 1999;17:1689–700. https://doi.org/10.1200/JCO.1999.17.6.1689.
Chen SC, Chen MF, Hwang TL, Chao TC, Lo YF, Hsueh S, et al. Prediction of supraclavicular lymph node metastasis in breast carcinoma. Int J Radiat Oncol Biol Phys. 2002;52:614–9. https://doi.org/10.1016/s0360-3016(01)02680-3.
Debois JM. The significance of a supraclavicular node metastasis in patients with breast cancer. A literature review. Strahlenther Onkol. 1997;173:1–12. https://doi.org/10.1007/bf03039187.
Jackson SM. Carcinoma of the breast–the significance of supraclavicular lymph node metastases. Clin Radiol. 1966;17:107–14. https://doi.org/10.1016/s0009-9260(66)80066-1.
Kiricuta IC, Willner J, Kolbl O, Bohndorf W. The prognostic significance of the supraclavicular lymph node metastases in breast cancer patients. Int J Radiat Oncol Biol Phys. 1994;28:387–93.
American Joint Committee on Cancer. Manual for Staging of Cancer, 5th ed. Philadelphia: JB Lippincott 1997
Brito RA, Valero V, Buzdar AU, Booser DJ, Ames F, Strom E, et al. Long-term results of combined-modality therapy for locally advanced breast cancer with ipsilateral supraclavicular metastases: the university of Texas M.D. Anderson cancer center experience. J Clin Oncol. 2001;19:628–33.
Singletary SE, Allred C, Ashley P, Bassett LW, Berry D, Bland KI, et al. Revision of the American joint committee on cancer staging system for breast cancer. J Clin Oncol. 2002;20:3628–36. https://doi.org/10.1200/JCO.2002.02.026.
Park HJ, Shin KH, Cho KH, Park IH, Lee KS, Ro J, et al. Outcomes of positron emission tomography-staged clinical N3 breast cancer treated with neoadjuvant chemotherapy, surgery, and radiotherapy. Int J Radiat Oncol Biol Phys. 2011;81:e689-695. https://doi.org/10.1016/j.ijrobp.2010.11.061.
Jung J, Kim SS, Ahn SD, Lee SW, Ahn SH, Son BH, et al. Treatment outcome of breast cancer with pathologically proven synchronous ipsilateral supraclavicular lymph node metastases. J Breast Cancer. 2015;18:167–72. https://doi.org/10.4048/jbc.2015.18.2.167.
Noh JM, Kim KH, Park W, Suh CO, Huh SJ, Choi DH, et al. Prognostic significance of nodal involvement region in clinical stage IIIc breast cancer patients who received primary systemic treatment, surgery, and radiotherapy. Breast. 2015;24:637–41. https://doi.org/10.1016/j.breast.2015.07.016.
Olivotto IA, Chua B, Allan SJ, Speers CH, Chia S, Ragaz J. Long-term survival of patients with supraclavicular metastases at diagnosis of breast cancer. J Clin Oncol. 2003;21:851–4. https://doi.org/10.1200/JCO.2003.11.105.
Dienstmann R, Branco LG, Rezende LM, Freitas LC, Lima CF, Rodrigues GJ, et al. Combined modality therapy of stage IIIC breast cancer. Breast J. 2011;17:331–3. https://doi.org/10.1111/j.1524-4741.2011.01086.x.
Yu JI, Park W, Choi DH, Huh SJ, Nam SJ, Kim SW, et al. Clinical outcomes and prognostic factors of pathologic N3 breast cancer treated with modern standard treatments. Clin Breast Cancer. 2015;15:512–8. https://doi.org/10.1016/j.clbc.2015.06.004.
Choi HY, Park M, Seo M, Song E, Shin SY, Sohn YM. Preoperative axillary lymph node evaluation in breast cancer: current issues and literature review. Ultrasound Q. 2017;33:6–14. https://doi.org/10.1097/RUQ.0000000000000277.
Rao R, Lilley L, Andrews V, Radford L, Ulissey M. Axillary staging by percutaneous biopsy: sensitivity of fine-needle aspiration versus core needle biopsy. Ann Surg Oncol. 2009;16:1170–5. https://doi.org/10.1245/s10434-009-0421-9.
Cools-Lartigue J, Meterissian S. Accuracy of axillary ultrasound in the diagnosis of nodal metastasis in invasive breast cancer: a review. World J Surg. 2012;36:46–54. https://doi.org/10.1007/s00268-011-1319-9.
Kim MJ, Park BW, Lim JB, Kim HS, Kwak JY, Kim SJ, et al. Axillary lymph node metastasis: CA-15-3 and carcinoembryonic antigen concentrations in fine-needle aspirates for preoperative diagnosis in patients with breast cancer. Radiology. 2010;254:691–7. https://doi.org/10.1148/radiol.09091031.
Acknowledgements
Thanks to the upfront members of Chinese Society of Breast Surgery for providing ISLM breast cancer patient data. Participants and researchers in this study(In no particular order: Beijing Chaoyang Hospital, Chuanhong Jiang. Peking University First Hospital, Yinhua Liu and Xuening Duan. Peking University People’s Hospital, Shu Wan. Beijing Friendship Hospital, Xiang Qu. The Second Affiliated Hospital of Dalian Medical University, Zuowei Zhao. The Affiliated Union Hospital of Fujian Medical University, Chuan Wang. The Obstetrics & Gynecology Hospital of Fudan University, Kejin Wu. Zhongshan Hospital Affiliated to Fudan University, Wei Zhu. Huashan Hospital of Fudan University, Qiang Zou. Wudang Hospital of Guizhou Medical University, Dahua Mao. The Second Affiliated Hospital of Harbin Medical University, Jianguo Zhang. Hebei Cancer Hospital, Zhenzhen Liu. The First Hospital of Jilin University, Zhimin Fan. Jilin Cancer Hospital, Ke Liu. The First Affiliated Hospital of the Air Force Military Medical University, Rui Ling. The Second Hospital of Lanzhou University, Ailin Song. The First Affiliated Hospital of the Army Military Medical University, Jun Jiang. The Inner Mongolia Autonomous Region Peoples Hospital, Zhongwei Cao. The Second Hospital of Shandong University, Zhigang Yu. Qilu Hospital of Shandong University, Rong Ma. Xuanwu Hospital of the Capital Medical University, Hua Kang. Sichuan Provincial People’s Hospital, Jinping Liu. The Affiliated Tumor Hospital of Xinjiang Medical University, Jianghua Ou. Yunnan Cancer Hospital, Dedian Chen. The Second Affiliated Hospital of Zhejiang University, Jian Huang. The First Affiliated Hospital of Zhejiang University, Peifen Fu. The General Hospital of People's Liberation Army, Jiandong Wang. The First Affiliated Hospital of China Medical University, Feng Jin. Sheng Jing Hospital Affiliated to China Medical University, Yi Zhao. Sun Yat-sen Memorial Hospital of Sun Yat-sen University, Erwei Song.
Funding
There is no funding to report.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethical approval
All procedures performed in studies in involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Research involving human participants or animals
This article does not contain any studies with animal performed by any of the authors.
Informed consent
Informed consent was obtained from all the individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Participants and researchers in this study were included in the Acknowledgements section.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ai, X., Sun, P., Wang, M. et al. A multi-center cross-sectional investigation of the diagnosis and treatment of breast cancer with synchronous ipsilateral supraclavicular lymph node metastases based on the CSBrs-009. Clin Transl Oncol 25, 1482–1487 (2023). https://doi.org/10.1007/s12094-022-03053-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-022-03053-w