Abstract
Purpose
TMB is one of the potent biomarkers of response to immune checkpoint blockade. The association between TMB and efficacy of chemotherapy in advanced lung cancer has not been comprehensively explored.
Methods
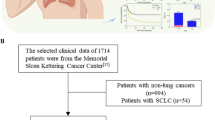
Ninety lung cancer patients receiving first-line chemotherapy with large panel next-generation sequencing data of pre-treatment tumor tissue were identified. The effect of TMB on PFS of chemotherapy were evaluated in univariate and multivariate analyses.
Results
The median TMB level of lung cancer patients enrolled in this study was 9.4 mutations/Mb, with TMB levels in smokers significantly higher than those in non-smokers. All patients were divided into high TMB and low TMB groups with the cutoff of the median TMB. The patients with low TMB had longer PFS of first-line chemotherapy (median PFS 9.77 vs 6.33 months, HR = 0.523, 95% CI 0.32–0.852, log-rank P = 0.009). Subgroup analysis showed that PFS of chemotherapy favored low TMB than high TMB among subgroups of male, age < 60, NSCLC, adenocarcinoma, stage IV, ECOG PS 0, driver mutation positive, TP53 wild type and patients not receiving bevacizumab. In multivariate analysis, PFS of chemotherapy remained significantly longer in low TMB group (HR = 0.554, p = 0.036). In those patients received immunotherapy upon unsatisfactory chemotherapy, PFS of immunotherapy was much longer in high TMB group (median PFS 32.88 vs 6.62 months, HR = 0.2426, 95% CI 0.06–0.977, log-rank P = 0.04).
Conclusions
TMB level of tumor tissue is a potent biomarker for efficacy of chemotherapy and immunotherapy in lung cancer. It may provide some clues for the decision of treatment strategy.



Similar content being viewed by others
Abbreviations
- TMB:
-
Tumor mutational burden
- NSCLC:
-
Non-small cell lung cancer
- SCLC:
-
Small cell lung cancer
- PFS:
-
Progression-free survival
- mPFS:
-
Median progression-free survival.
- OS:
-
Overall survival
- HR:
-
Hazard ratio
- CI:
-
Confidence interval
- ECOG PS:
-
Eastern cooperative oncology group performance status
- NGS:
-
Next-generation sequencing
- SNV:
-
Single-nucleotide variant
- KEGG:
-
The Kyoto encyclopedia of genes and genomes
- NSCLC–NOS:
-
Non-small cell lung cancer–not otherwise specified
- CR:
-
Complete response
- PR:
-
Partial response
- SD:
-
Stable disease
- PD:
-
Progressive disease
References
Hatakeyama K, Nagashima T, Urakami K, Ohshima K, Serizawa M, Ohnami S, et al. Tumor mutational burden analysis of 2,000 Japanese cancer genomes using whole exome and targeted gene panel sequencing. Biomed Res. 2018;39(3):159–67.
Dijkstra KK, Voabil P, Schumacher TN, Voest EE. Genomics- and transcriptomics-based patient selection for cancer treatment with immune checkpoint inhibitors: a review. JAMA Oncol. 2016;2(11):1490–5.
Chan TA, Yarchoan M, Jaffee E, Swanton C, Quezada SA, Stenzinger A, et al. Development of tumor mutation burden as an immunotherapy biomarker: utility for the oncology clinic. Ann Oncol. 2019;30(1):44–56.
Chalmers ZR, Connelly CF, Fabrizio D, Gay L, Ali SM, Ennis R, et al. Analysis of 100,000 human cancer genomes reveals the landscape of tumor mutational burden. Genome Med. 2017;9(1):34.
Hellmann MD, Ciuleanu TE, Pluzanski A, Lee JS, Otterson GA, Audigier-Valette C, et al. Nivolumab plus Ipilimumab in Lung cancer with a high tumor mutational burden. N Engl J Med. 2018;378(22):2093–104.
Gandara DR, Paul SM, Kowanetz M, Schleifman E, Zou W, Li Y, et al. Blood-based tumor mutational burden as a predictor of clinical benefit in non-small-cell lung cancer patients treated with atezolizumab. Nat Med. 2018;24(9):1441–8.
Forde PM, Chaft JE, Smith KN, Anagnostou V, Cottrell TR, Hellmann MD, et al. Neoadjuvant PD-1 blockade in resectable lung cancer. N Engl J Med. 2018;378(21):1976–86.
Carbone DP, Reck M, Paz-Ares L, Creelan B, Horn L, Steins M, et al. First-line nivolumab in stage IV or recurrent non-small-cell lung cancer. N Engl J Med. 2017;376(25):2415–26.
Rosenberg JE, Hoffman-Censits J, Powles T, van der Heijden MS, Balar AV, Necchi A, et al. Atezolizumab in patients with locally advanced and metastatic urothelial carcinoma who have progressed following treatment with platinum-based chemotherapy: a single-arm, multicentre, phase 2 trial. Lancet. 2016;387(10031):1909–20.
Liu L, Bai X, Wang J, Tang XR, Wu DH, Du SS, et al. Combination of TMB and CNA stratifies prognostic and predictive responses to immunotherapy across metastatic cancer. Clin Cancer Res. 2019;25(24):7413–23.
Offin M, Rizvi H, Tenet M, Ni A, Sanchez-Vega F, Li BT, et al. Tumor mutation burden and efficacy of EGFR-tyrosine kinase inhibitors in patients with EGFR-mutant lung cancers. Clin Cancer Res. 2019;25(3):1063–9.
Schiller JH, Harrington D, Belani CP, Langer C, Sandler A, Krook J, et al. Comparison of four chemotherapy regimens for advanced non-small-cell lung cancer. N Engl J Med. 2002;346(2):92–8.
Scagliotti GV, Parikh P, von Pawel J, Biesma B, Vansteenkiste J, Manegold C, et al. Phase III study comparing cisplatin plus gemcitabine with cisplatin plus pemetrexed in chemotherapy-naive patients with advanced-stage non-small-cell lung cancer. J Clin Oncol. 2008;26(21):3543–51.
Sandler A, Gray R, Perry MC, Brahmer J, Schiller JH, Dowlati A, et al. Paclitaxel-carboplatin alone or with bevacizumab for non-small-cell lung cancer. N Engl J Med. 2006;355(24):2542–50.
Salazar MC, Rosen JE, Wang Z, Arnold BN, Thomas DC, Herbst RS, et al. Association of delayed adjuvant chemotherapy with survival after lung cancer surgery. JAMA Oncol. 2017;3(5):610–9.
Parra ER, Villalobos P, Behrens C, Jiang M, Pataer A, Swisher SG, et al. Effect of neoadjuvant chemotherapy on the immune microenvironment in non-small cell lung carcinomas as determined by multiplex immunofluorescence and image analysis approaches. J Immunother Cancer. 2018;6(1):48.
Talevich E, Shain AH, Botton T, Bastian BC. CNVkit: genome-wide copy number detection and visualization from targeted DNA sequencing. PLoS Comput Biol. 2016;12(4): e1004873.
Ready N, Hellmann MD, Awad MM, Otterson GA, Gutierrez M, Gainor JF, et al. First-line nivolumab plus ipilimumab in advanced non-small-cell lung cancer (CheckMate 568): outcomes by programmed death ligand 1 and tumor mutational burden as biomarkers. J Clin Oncol. 2019;37(12):992–1000.
Rizvi NA, Cho BC, Reinmuth N, Lee KH, Luft A, Ahn MJ, et al. Durvalumab with or without tremelimumab vs standard chemotherapy in first-line treatment of metastatic non-small cell lung cancer: the MYSTIC phase 3 randomized clinical trial. JAMA Oncol. 2020;6(5):661–74.
Pai SG, Carneiro BA, Chae YK, Costa RL, Kalyan A, Shah HA, et al. Correlation of tumor mutational burden and treatment outcomes in patients with colorectal cancer. J Gastrointest Oncol. 2017;8(5):858–66.
Lin C, Shi X, Zhao J, He Q, Fan Y, Xu W, et al. Tumor mutation burden correlates with efficacy of chemotherapy/targeted therapy in advanced non-small cell lung cancer. Front Oncol. 2020;10:480.
Devarakonda S, Rotolo F, Tsao MS, Lanc I, Brambilla E, Masood A, et al. Tumor mutation burden as a biomarker in resected non-small-cell lung cancer. J Clin Oncol. 2018;36(30):2995–3006.
Samstein RM, Lee CH, Shoushtari AN, Hellmann MD, Shen R, Janjigian YY, et al. Tumor mutational load predicts survival after immunotherapy across multiple cancer types. Nat Genet. 2019;51(2):202–6.
Bell EH, Chakraborty AR, Mo X, Liu Z, Shilo K, Kirste S, et al. SMARCA4/BRG1 is a novel prognostic biomarker predictive of cisplatin-based chemotherapy outcomes in resected non-small cell lung cancer. Clin Cancer Res. 2016;22(10):2396–404.
Xue Y, Morris JL, Yang K, Fu Z, Zhu X, Johnson F, et al. SMARCA4/2 loss inhibits chemotherapy-induced apoptosis by restricting IP3R3-mediated Ca(2+) flux to mitochondria. Nat Commun. 2021;12(1):5404.
Jiao XD, Qin BD, You P, Cai J, Zang YS. The prognostic value of TP53 and its correlation with EGFR mutation in advanced non-small cell lung cancer, an analysis based on cBioPortal data base. Lung Cancer. 2018;123:70–5.
Dong ZY, Zhong WZ, Zhang XC, Su J, Xie Z, Liu SY, et al. Potential predictive value of TP53 and KRAS mutation status for response to PD-1 blockade immunotherapy in lung adenocarcinoma. Clin Cancer Res. 2017;23(12):3012–24.
Capulli M, Hristova D, Valbret Z, Carys K, Arjan R, Maurizi A, et al. Notch2 pathway mediates breast cancer cellular dormancy and mobilisation in bone and contributes to haematopoietic stem cell mimicry. Br J Cancer. 2019;121(2):157–71.
Zou Y, Yang R, Huang ML, Kong YG, Sheng JF, Tao ZZ, et al. NOTCH2 negatively regulates metastasis and epithelial-Mesenchymal transition via TRAF6/AKT in nasopharyngeal carcinoma. J Exp Clin Cancer Res. 2019;38(1):456.
Yang L, Zhao KL, Qin L, Ji DX, Zhang B, Zheng PF, et al. Notch signaling pathway regulates CD4(+)CD25(+)CD127(dim/-) regulatory T cells and T helper 17 cells function in gastric cancer patients. 2019. Biosci Rep. https://doi.org/10.1042/BSR20182044.
Funding
This work was supported by the Science and Technology Commission of Shanghai Municipality (20DZ2254400, 20DZ2261200), Bethune Charitable Foundation (BJ-RW2020017J), Shanghai Municipal Key Clinical Specialty (shslczdzk02201), and National Natural Science Foundation of China (82170088).
Author information
Authors and Affiliations
Contributions
JS: conceptualization; investigation; data curation; formal analysis; writing—original draft. YY: investigation; data curation; formal analysis; validation; writing—original draft. CC: investigation; data curation; formal analysis; validation; writing—original draft. JL: investigation; data curation; validation; writing—review and editing. ND: investigation; data curation; validation; writing—review and editing. JL: investigation; methodology; writing—review and editing. YZ: software; methodology; writing—review and editing. MY: investigation; writing—review and editing. CL: investigation; writing—review and editing. NX: formal analysis; methodology; writing—review and editing. HB: formal analysis; methodology; writing—review and editing. XZ: supervision; validation; writing—review and editing. QH: supervision; validation; writing—review and editing. JZ: methodology; funding acquisition; supervision; writing—review and editing. YS: supervision; methodology; funding acquisition; writing—review and editing. YWS: supervision; project administration; writing—review and editing. CB: supervision; funding acquisition; project administration; writing—review and editing. LT: conceptualization; investigation; data curation; formal analysis; review and editing; funding acquisition. JH: conceptualization; project administration; supervision; methodology; funding acquisition; writing—review and editing.
Corresponding authors
Ethics declarations
Conflict of interest
Y. W. Shao and H. Bao are the shareholders or employees of Geneseeq Technology Inc. The other authors declare no conflicts of interest.
Research involving human participants and/or animals
This study was approved by the ethics committee of Zhongshan Hospital, Fudan University. The approval number was B2017-142R.
Informed consent
All patients provided informed written consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Song, J., Yan, Y., Chen, C. et al. Tumor mutational burden and efficacy of chemotherapy in lung cancer. Clin Transl Oncol 25, 173–184 (2023). https://doi.org/10.1007/s12094-022-02924-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-022-02924-6