Abstract
Objective
There is a gap in knowledge regarding the ideal management of patients with early-stage cervical cancer and intermediate-risk features. Here, we present a meta-analysis of the published literature on oncological outcomes in these patients and determine trends in postoperative management.
Methods
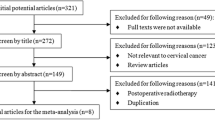
MEDLINE and PubMed were used for literature searches. The inclusion criteria were: English language articles including ≥ 10 patients, patients who underwent radical hysterectomy, nodes negative, studies reporting oncological outcomes and complications treatment-related and compare a surgery-only cohort with a radiotherapy cohort. The PRISMA guidelines were followed. Combined relative risk was calculated using DerSimonian–Laird random-effects model and a forest plot was drawn.
Results
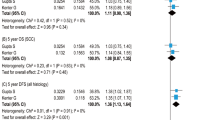
We collected 183 manuscripts on early-stage cervical cancer treated with radical hysterectomy alone or with adjuvant radiotherapy after surgery. A total of eight studies met the inclusion criteria. Regarding oncological outcomes, survival was reported in five studies. The relative risk of recurrence and the relative risk of mortality was similar in both groups independently whether receive or not adjuvant therapy. Most of the studies did not report significant differences regarding morbidity treatment related between the groups, except for a higher rate of lymphedema after radiotherapy.
Conclusion
We found that the relative risk of recurrence and mortality was similar in both groups not depending on adjuvant therapy. Therefore, whether radiotherapy adjuvant treatment is indicated remains a topic of debate.


Similar content being viewed by others
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2020. CA Cancer J Clin. 2020;70(1):7–30.
Bhatla N, Aoki D, Sharma DN, Sankaranarayanan R. Cancer of the cervix uteri. Int J Gynecol Obstet. 2018;143:22–36.
Gray HJ. Primary management of early stage cervical cancer (IA1-IB) and appropriate selection of adjuvant therapy. J Natl Compr Canc Netw. 2008;6(1):47–52.
Peters WA, Liu PY, Barrett RJ, Stock RJ, Monk BJ, et al. Concurrent chemotherapy and pelvic radiation therapy compared with pelvic radiation therapy alone as adjuvant therapy after radical surgery in high-risk early-stage cancer of the cervix. J Clin Oncol. 2000;18(8):1606–13.
Delgado G, Bundy B, Zaino R, Sevin BU, Creasman WT, et al. Prospective surgical-pathological study of disease-free interval in patients with stage IB squamous cell carcinoma of the cervix: a Gynecologic Oncology Group study. Gynecol Oncol. 1990;38:352–7.
Chung CK, Nahhas WA, Stryker JA, Curry SL, Abt AB, et al. Analysis of factors contributing to treatment failures in stages IB and IIA carcinoma of the cervix. Am J Obstet Gynecol. 1980;138:550–6.
Abdulhayoglu G, Rich WM, Reynolds J, DiSaia PJ. Selective radiation therapy in stage IB uterine cervical carcinoma following radical pelvic surgery. Gynecol Oncol. 1980;10:84–92.
Boyce JG, Fruchter RG, Nicastri AD, De Regt RH, et al. Vascular invasion in Stage I carcinoma of the cervix. Cancer. 1984;53:1175–80.
Rotman M, John M, Boyce J. Prognostic factors in cervical carcinoma: implications in staging and management. Cancer. 1981;48(Suppl. 2):560–7.
Sedlis A, Bundy BN, Rotman MZ, Lentz SS, Muderspach LI, et al. A randomized trial of pelvic radiation therapy versus no further therapy in selected patients with stage IB carcinoma of the cervix after radical hysterectomy and pelvic lymphadenectomy: a gynecologic oncology group study. Gynecol Oncol. 1999;73:177–83.
Rotman M, Sedlis A, Piedmonte MR, Bundy B, Lentz SS, et al. A phase III randomized trial of postoperative pelvic irradiation in Stage IB cervical carcinoma with poor prognostic features: follow-up of a gynecologic oncology group study. Int J Radiat Oncol Biol Phys. 2006;65:169–75.
Querleu D, Cibula D, Abu-Rustum NR. 2017 Update on the Querleu-Morrow Classification of Radical Hysterectomy. Ann Surg Oncol. 2017;24(11):3406–12. https://doi.org/10.1245/s10434-017-6031-z.
Cibula D, Planchamp F, Fischerova D, Fotopoulou C, Kohler C, Landoni F, et al. European Society of Gynaecological Oncology quality indicators for surgical treatment of cervical cancer. Int J Gynecol Cancer. 2020;30(1):3–14. https://doi.org/10.1136/ijgc-2019-000878.
Rogers L, Siu SSN, Luesley D, Bryant A, Dickinson HO. Radiotherapy and chemoradiation after surgery for early cervical cancer. Cochrane Database Syst Rev. 2012. https://doi.org/10.1002/14651858.CD007583.pub3.
Shamseer L, Moher D, Clarke M, Ghersi D, Liberati A, et al. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015: elaboration and explanation. BMJ. 2015;350:g7647.
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, et al. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev. 2015;4:1.
Cibula D, Potter R, Planchamp F, et al. The European Society of Gynaecological Oncology/European Society for Radiotherapy and Oncology/European Society of Pathology guidelines for the management of patients with cervical cancer. Int J Gynecol Cancer. 2018;28:641–55. https://doi.org/10.1097/IGC.0000000000001216.
U.S Department of health and human services. Common Terminology Criteria for Adverse Events (CTCAE) version 5.0 – November 27, 2017. Accesed online on November 2020 https://ctep.cancer.gov/protocolDevelopment/electronic_applications/docs/CTCAE_v5_Quick_Reference_8.5x11.pdf
Bilek K, Ebeling K, Leitsmann H, Seidel G. Radical pelvic surgery versus radical surgery plus radiotherapy for stage Ib carcinoma of the cervix uteri. Preliminary results of a prospective randomized clinical study. Arch Geschwulstforsch. 1982;52:223–9.
Rushdan MN, Tay EH, Khoo-Tan HS, Lee KM, Low JH, et al. Tailoring the field and indication of adjuvant pelvic radiation for patients with FIGO stage Ib lymph nodes-negative cervical carcinoma following radical surgery based on the GOG score- a pilot study. Ann Acad Med Singapore. 2004;33:367–472.
Nakamura K, Kitahara Y, Satoh T, Takei Y, Takano M, et al. Analysis of the effect of adjuvant radiotherapy on outcomes and complications after radical hysterectomy in FIGO stage IB1 cervical cancer patients with intermediate risk factors (GOTIC Study). World J Surg Oncol. 2016. https://doi.org/10.1186/s12957-016-0931-4.
Cibula D, Abu-Rustum NR, Fischerova D, Pather S, Lavigne K, et al. Surgical treatment of “intermediate risk” lymph node negative cervical cancer patients without adjuvant radiotherapy—a retrospective cohort study and review of the literature. Gynecol Oncol. 2018. https://doi.org/10.1016/j.ygyno.2018.10.018.
Schoorge JO, Molpus KL, Koelliker D, Nikrui N, Goodman A, et al. Stage IB and IIA cervical cancer with negative lymph nodes: the role of adjuvant radiotherapy after radical hysterectomy. Gynecol Oncol. 1997;66:31–5.
Snijders-Keilholz A, Hellebrekers BW, Zwinderman A, van de Vijver M, Trimbos J. Adjuvant radiotherapy following radical hysterectomy for patients with early-stage cervical carcinoma (1984–1996). Radiother Oncol. 1999;51(2):161–7.
Pieterse QD, Trimbos J, Dijkman A, Creutzberg CL, Gaarenstroom KN, et al. Postoperative radiation therapy improves prognosis in patients with adverse risk factors in localized, early-stage cervical cancer: a retrospective comparative study. Int J Gynecol Cancer. 2006;16:1112–8.
Zhang X, Bao B, Wang S, Yi M, Jiang L, Fang X. Sentinel lymph node biopsy in early-stage cervical cancer: a meta-analysis. Cancer Med. 2020;10(8):2590–600.
Havrilesky LJ, Kulasingam SL, Matchar DB, et al. FDG-PET for management of cervical and ovarian cancer. Gynecol Oncol. 2005;97:183–91.
Grigsby PW, Siegel BA, Dehdashti F. Lymph node staging by positron emission tomography in patients with carcinoma of the cervix. J Clin Oncol. 2001;19(17):3745–9. https://doi.org/10.1200/JCO.2001.19.17.3745 (PMID: 11533097).
Kidd EA, Siegel BA, Dehdashti F, Rader JS, Mutch DG, Powell MA, Grigsby PW. Lymph node staging by positron emission tomography in cervical cancer: relationship to prognosis. J Clin Oncol. 2010;28(12):2108–13. https://doi.org/10.1200/JCO.2009.25.4151 (Epub 2010 Mar 22 PMID: 20308664).
Tsai CS, Lai CH, Chang TC, Yen TC, Ng KK, Hsueh S, Lee SP, Hong JH. A prospective randomized trial to study the impact of pretreatment FDG-PET for cervical cancer patients with MRI-detected positive pelvic but negative para-aortic lymphadenopathy. Int J Radiat Oncol Biol Phys. 2010;76(2):477–84. https://doi.org/10.1016/j.ijrobp.2009.02.020 (Epub 2009 May 21 PMID: 19464824).
Devine C, Viswanathan C, Faria S, Marcal L, Sagebiel TL. Imaging and staging of cervical cancer. Semin Ultrasound CT MRI. 2019;40(4):280–6. https://doi.org/10.1053/j.sult.2019.03.001.
Cibula D. Management of patients with intermediate-risk early stage cervical cáncer. J Gynecol Oncol. 2020;31(3):354.
Lin Y, Chen K, Lu Z, Zhao L, Tao Y, Ouyang Y, Cao X. Intensity-modulated radiation therapy for definitive treatment of cervical cancer: a meta-analysis. Radiat Oncol. 2018;13(1):177. https://doi.org/10.1186/s13014-018-1126-7.PMID:30217165;PMCID:PMC6137729.
Lawrie TA, Green JT, Beresford M, Wedlake L, Burden S, et al. Interventions to reduce acute and late adverse gastrointestinal effects of pelvic radiotherapy for primary pelvic cancers. Cochrane Database Syst Rev. 2018;1(1):CD012529. https://doi.org/10.1002/14651858.CD012529.pub2.
Cibula D. An International Randomised Trial of Radical Surgery Followed by Adjuvant (Chemo)Radiation Versus no Further Treatment in Patients With Early-stage, Intermediate-risk Cervical Cancer Patients. (CERVANTES) https://clinicaltrials.gov/ct2/show/study/NCT04989647 (29 November 2021, last date accessed).
Acknowledgements
We would like to thank Drs. Cristina Centeno Mediavilla, Silvia Cabrera Díaz, and Jose Luis Sanchez-Iglesias (Gynecologic Oncology Department, Vall d'Hebron Hospital, Barcelona) for valuable collaboration and support within the working group.
Funding
No sources of funding were used.
Author information
Authors and Affiliations
Contributions
Conception and Design of Study: NRGH, AGM. Data collection: NRGH, TGR. Data analysis and interpretation: NRGH, TGR, UA. Statistical analysis: SPH. Manuscript preparation: NRGH, UA, TGR, VB, SM, RV, APB, MB, AGM.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standards
Informed consent or the ethical committee contest was not necessary since this work includes a systematic review and meta-analysis.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gómez-Hidalgo, N.R., Acosta, Ú., Rodríguez, T.G. et al. Adjuvant therapy in early-stage cervical cancer after radical hysterectomy: are we overtreating our patients? A meta-analysis. Clin Transl Oncol 24, 1605–1614 (2022). https://doi.org/10.1007/s12094-022-02808-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-022-02808-9