Abstract
Purpose
To develop a model that predicts survival in patients irradiated for metastatic spinal cord compression (MSCC), hence assisting in the decision between a short and a long-course radiotherapy (RT) regimen.
Methods
138 patients diagnosed with MSCC and treated with RT alone were included. Based on a multivariate analysis, a scoring system was developed. It included four prognostic variables: age, number of vertebrae, ECOG and histology. Total scores ranged between 14 and 24 points and patients were divided into two groups.
Results
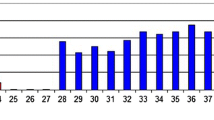
The 6-month survival rate was 22% for patients with a score of 14–18 points; and 69% for patients with a score of 19–24 points (P < 0.001). The system exhibits a high specificity and positive predictive value and an appropriate discriminative ability.
Conclusions
Patients with scores between 19 and 24 points were found to survive longer, thus a long-course RT appears to be more appropriate.

Similar content being viewed by others
References
Rades D, Fehlauer F, Schulte R, Veninga T, Stalpers LJA, Basic H, et al. Prognostic factors for local control and survival after radiotherapy of metastatic spinal cord compression. J Clin Oncol. 2006;24:3388–93.
Rades D, Dunst J, Schild SE. The first score predicting overall survival in patients with metastatic spinal cord compression. Cancer. 2008;112:157–61.
Chow E, Harris K, Fung K. Successful validation of a survival prediction model in patients with metastases in the spinal column. Int J Radiat Oncol. 2006;65:1522–7.
Kirshblum SC, Burns SP, Biering-Sorensen F, Donovan W, Graves DE, Jha A, et al. International standards for neurological classification of spinal cord injury (revised 2011). J Spinal Cord Med. 2011;34:535–46.
Tomita K, Kawahara N, Kobayashi T, Yoshida A, Murakami H, Akamaru T. Surgical strategy for spinal metastases. Spine. 2001;26:298–306.
Tokuhashi Y, Matsuzaki H, Oda H, Oshima M, Ryu J. A revised scoring system for preoperative evaluation of metastatic spine tumor prognosis. Spine. 2005;30:2186–91.
Bach F, Larsen BH, Rohde K, Børgesen SE, Gjerris F, Bøge-Rasmussen T, et al. Metastatic spinal cord compression occurrence, symptoms, clinical presentations and prognosis in 398 patients with spinal cord compression. Acta Neurochir (Wien). 1990;107:37–433.
Helweg-Larsen S, Sørensen PS, Kreiner S. Prognostic factors in metastatic spinal cord compression: a prospective study using multivariate analysis of variables influencing survival and gait function in 153 patients. Int J Radiat Oncol Biol Phys. 2000;46:1163–9.
Rose PS, Buchowski JM. Metastatic disease in the thoracic and lumbar spine: evaluation and management. J Am Acad Orthop Surg. 2011;19:37–48.
Patchell RA, Tibbs PA, Regine WF, Payne R, Saris S, Kryscio RJ, et al. Direct decompressive surgical resection in the treatment of spinal cord compression caused by metastatic cancer: a randomised trial. Lancet Lond Engl. 2005;366:643–8.
McLinton A, Hutchison C. Malignant spinal cord compression: a retrospective audit of clinical practice at a UK regional cancer centre. Br J Cancer. 2006;94:486–91.
Rades D, Evers JN, Rudat V, Bajrovic A, Karstens JH, Schild SE. A validated score estimating ambulatory status following radiotherapy of elderly patients for metastatic spinal cord compression. BMC Cancer. 2014;14(14):589.
Hadden NJ, McIntosh JRD, Jay S, Whittaker PJ. Prognostic factors in patients with metastatic spinal cord compression secondary to melanoma: a systematic review. Melanoma Res. 2018;28:1–7.
West HJ, Jin JO (2015) JAMA oncology patient page. Performance status in patients with cancer. JAMA Oncol. 2015;1:998.
Rades D, Veninga T, Bajrovic A, Karstens JH, Schild SE. A validated scoring system to identify long-term survivors after radiotherapy for metastatic spinal cord compression. Strahlenther Onkol Organ Dtsch Röntgenges Al. 2013;189:462–6.
Sørensen S, Børgesen SE, Rohde K, Rasmusson B, Bach F, Bøge-Rasmussen T, et al. Metastatic epidural spinal cord compression. Results of treatment and survival. Cancer. 1990;65:1502–8.
Constans JP, de Divitiis E, Donzelli R, Spaziante R, Meder JF, Haye C. Spinal metastases with neurological manifestations. Review of 600 cases. J Neurosurg. 1983;59:111–8.
Maranzano E, Latini P, Checcaglini F, Ricci S, Panizza BM, Aristei C, et al. Radiation therapy in metastatic spinal cord compression. A prospective analysis of 105 consecutive patients. Cancer. 1991;67:1311–7.
Stark RJ, Henson RA, Evans SJ. Spinal metastases. A retrospective survey from a general hospital. Brain J Neurol. 1982;105:189–21313.
Maranzano E, Latini P. Effectiveness of radiation therapy without surgery in metastatic spinal cord compression: final results from a prospective trial. Int J Radiat Oncol Biol Phys. 1995;32:959–67.
Hill ME, Richards MA, Gregory WM, Smith P, Rubens RD. Spinal cord compression in breast cancer: a review of 70 cases. Br J Cancer. 1993;68:969–73.
Gilbert RW, Kim JH, Posner JB. Epidural spinal cord compression from metastatic tumor: diagnosis and treatment. Ann Neurol. 1978;3:40–51.
Podd TJ, Carpenter DS, Baughan CA, Percival D, Dyson P. Spinal cord compression: prognosis and implications for treatment fractionation. Clin Oncol. 1992;4:341–4.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical statement
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nenclares, P., Guardado, S., Asiáin, L. et al. A new and simple scoring system to predict overall survival after irradiation for metastatic spinal cord compression. Clin Transl Oncol 22, 440–444 (2020). https://doi.org/10.1007/s12094-019-02144-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-019-02144-5