Abstract
Introduction
Testicular tumors are frequent in young adults, coinciding with incorporation to military service. The present study evaluates the tumor characteristics, time course and results obtained with the treatments used in our center for this type of neoplasms.
Material and methods
A retrospective longitudinal study was conducted in a cohort of 98 patients with an average age of 28.6 years, subjected to orchiectomy for testicular tumors in our center between 1979 and 2004. Data were collected relating to patient age, tumor characteristics, the outcome of treatment, and the course of the disease.
Results
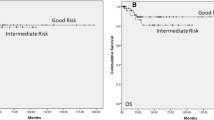
The right testicle was affected in 61% (with significant differences versus the left side). The most common histological type corresponded to non-seminomatous germ cell tumors (NSGCTs) (65.3%), followed by pure seminomas (27.6%) and non-germinal cell tumors (NGCs) (7.1%). NSGCT was diagnosed at a significantly younger average age (23.2 years) than the other two tumor types. Stage I was the most frequent presentation (58%). Seminomas presented in stage I significantly more often (80%) than the others tumors. The data collected over the 25-year study period showed no significant variations in tumor characteristics. Thelog-rank test showed a significant difference in terms of patient survival according to the tumor cell line (p=0.000) and stage (p=0.000), except between stages I and II, where no significant differences were observed in terms of survival.
Conclusions
Non-seminomatous germ cell tumors (NSGCTs) are the most frequent testicular tumors in young adults. Most neoplasms are diagnosed in early stages, the prognosis being better in the case of seminomas and tumor stages I and II.
Similar content being viewed by others
References
Schottenfield D, Warshauwe, ME, Sherlock S, Zauber AG, Leyder M, Payne R. The epidemiology of testicular cancer in young adults. Am J Epidemiol 1980;112: 252–46.
Richie JP. Neoplasm of the testis. In: Campbell’s Urology 7th ed. Walsh PC et al, (edts) Philadelphia: Wb Saunder Co; 1997, p. 2411–52.
Yamane GK, Johnson R. Testicular carcinoma in US. Air Force aviators: a casecontrol study. Aviat Space Environ Med. 2003;74(8):846–50.
Mostofi FK, Sobin LH. International histological clasification of tumor of the teste WHO: Geneve, 1977.
Mostofi FK, Sesterhenn IA. Histological typing of the testis tumors. WHO International Histological Clasification Tumors 2nd Edition Springer-Verlag: Berlin, 1998.
Medical Research Council Working Party on Testiculars Tumours. Prognostic factors in advanced non-seminomatous germcell testicular tumours: results of multicentre study. Lancet. 1985;1:8–11.
Germa-Lluch JR, García del Muro X, Maroto P, et al; Spanish Germ-Cell Cancer Group (GG). Clinical pattern and therapeutic results achieved in 1490 patients with germ-cell tumours of the testis: the experience of the Spanish Germ-Cell Cancer Group (GG). Eur Urol. 2002;42(6): 553–63.
Tomomasa H, Shimizu H, et al. Clinical study of testicular germ cell tumors. Hinyokika Kiyo. 2001;47(6):389–95.
Stone JM, Cruickshank DG, Sandeman TF, Matthews JP. Laterality, maldescent, trauma and other clinical factors in the epidemiology of testis cancer, in Victoria, Australia. Br J Cancer. 1991;64(1):152–8.
Soto Delgado M, Varo C, Juárez A, et al. Consideraciones sobre tumores de testiculo: nuestra experiencia. Arch Esp Urol. 1999;52(2):123–32.
Fernández Gómez JM, Guate Ortiz JL, Martin Huescar A, et al. Presentación clíníca del cancer germinal de testículo. Arch Esp Urol. 2002;55(8):915–22.
Gudbjartsson T, Magnusson K, Bergthorsson, J, et al. A population-based analysis of increased incidence and improved survival of testicular cancer patients in Iceland. Scand J Urol Nephrol. 2003;37 (4):292–8.
Abratt RP., Reddi VB, Sarembock LA. Testicular cancer and cryptorchidism. Br. J Urol. 1992;70(6):656–9.
Angwafo FF 3rd, Takongmo S, Mbakop A, Ngu VA. Testes tumors in a Sub-Saharan African city (Yaounde) Incident cases and histopathology. Eur. Urol. 1996;30(3): 345–8.
Bridges PJ, Sharifi R, Razzaq A, Guinan P. Decreased survival of black Americans with testicular cancer. J Urol. 1998;159 (4):1221–3.
Huyghe E, Matsuda T, Thonneau P. Increasing incidence of testicular cancer worldwide: a review. J Urol. 2003;170(1): 5–11.
Armora Mani J, Riera Canals L, Franco Miranda E, et al. Tumores germinales de testículo, casuística y revisión, bibliográfica. Actas Urol Esp. 1990;14(5):319–24.
Hernes EH, Harstad K, Fossa. Changing incidence and delay of testicular cancer in southern Norway (1981–1992). Eur Urol. 1996;30(3):349–57.
Levi F, Te VC, Randimbison L, La Vecchia C. Trends in testicular cancer incidence In. Vaud, Switzerland. Eur J Cancer Prev. 2003;12(4):347–9.
McGlynn KA, Devesa SS, Sigurdson AJ, Brown LM, Tsao L, Tarone RE. Trends in the incidence of testicular germ cell tumors in the United States. Cancer. 2003; 97(1):65–70.
Vergouwe Y, Steyerberg EW, Eijkemans MJ, Albers P, Habbema JD. Predictors of occult metastasis in clinical stage I nonseminoma: a systematic review. J Clin Oncol. 2003;21(22):4092–9.
Erbay ME, Tarhan F, Barisik NO, Kuyumcuoglu U. A case of testicular rhabdomyosarcoma. Int Urol Nephrol. 2004;36 (1):73–5.
Cruceyra Betriu G, Tejido Sánchez A, Duarte Ojeda JM, et al.. Tumor de Leydig: presentación de 8 casos y revisión de la literatura. Acta Urol Esp. 2002;26(1):36–40.
Post PN Casparie MK, ten Kate FJ, Oosterhuis JW. The epidemiology of tumors of the testes in the Netherlands: accurate rendering by the Registry of Histopathology and Cytopathology (PALGA). Ned Tijdschr Geneeskd. 2004;148(23):1150–4.
Santoni R, Barbera F, Bertoni F, et al. Stage I seminoma of the testis: a bi-institutional retrospective analysis ofpatients treated with radiation therapy only. BJU Int. 2003;92(1):47–52.
Warde P Gospodarowicz MK, Banerjee D, et al. Prognostic factors for relapse in stage I testicular seminoma treated with surveillance. J Urol. 1997;157(5):1705–9.
Laguna MP, Klepp O, Horwich A, et al. Guidelines on testicular cancer. European Association of Urology, 2004
Krege S, Kalund G, Otto T, Goepel M, Rubben H. Phase II study: adjuvant single-agent carboplatin therapy for clinical stage I seminoma. Eur Urol. 1997;51(4): 405–7.
Bohlen D, Borner M, Sonntag RW, Fey MF, Studer UE. Long-term results following adjuvant chemotherapy in patients with clinical stage I testicular nonseminomatous malignant germ cell tumors with high risk factors. J Urol. 1999;161(4): 1148–52.
Classen J, Schmidberger H, Meisner C, et al. Radiotherapy for stages IIA/B testicular seminoma: final report of a prospective multicenter clinical trial. J Clin Oncol. 2005;21(6):1101–6.
Opot EN, Magoha GA. Testicular cancer at Kenyatta National Hospital. Nairobi. East Afr Med J. 2000;77(2):80–5.
Kim I, Young RH, Scully RE. Leydig cell tumor of the testis. A cliniccopathological analysis of 40 cases and review of the literature. Am J Sug Pathol. 1985:9(3):177–92.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Diz-Rodríguez, R., Vírseda-Chamorro, M., Paños-Lozano, P. et al. Testicular neoplasms. Evaluation of the experience during 25 years in a military hospital. Clin Transl Oncol 8, 681–687 (2006). https://doi.org/10.1007/s12094-006-0039-3
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s12094-006-0039-3