Abstract
Background
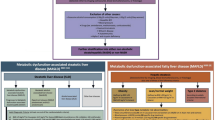
Metabolic dysfunction-associated fatty liver disease (MAFLD) is a novel definition proposed in 2020 with a relatively complex set of criteria. Thus, simplified criteria that are more applicable are required. This study aimed to develop a simplified set of criteria for identifying MAFLD and predicting MAFLD-related metabolic diseases.
Methods
We developed a simplified set of metabolic syndrome-based criteria for MAFLD, and compared the performance of the simplified criteria with that of the original criteria in predicting MAFLD-related metabolic diseases in a 7-year follow-up.
Results
In the 7-year cohort, a total of 13,786 participants, including 3372 (24.5%) with fatty liver, were enrolled at baseline. Of the 3372 participants with fatty liver, 3199 (94.7%) met the MAFLD-original criteria, 2733 (81.0%) met the simplified criteria, and 164 (4.9%) were metabolic healthy and met neither of the criteria. During 13,612 person-years of follow-up, 431 (16.0%) fatty liver individuals newly developed T2DM, with an incidence rate of 31.7 per 1000 person-years. Participants who met the simplified criteria had a higher risk of incident T2DM than those who met the original criteria. Similar results were observed for incident hypertension, and incident carotid atherosclerotic plaque.
Conclusion
The MAFLD-simplified criteria are an optimized risk stratification tool for predicting metabolic diseases in fatty liver individuals.




Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author, Dr. Chengfu Xu, upon reasonable request.
Abbreviations
- BMI:
-
Body mass index
- CI:
-
Confidence interval
- CIMT:
-
Carotid Intima-media thickness
- C-index:
-
Concordance index
- FPG:
-
Fasting plasma glucose
- HbA1c:
-
Hemoglobin A1c
- HDL-C:
-
High-density lipoprotein cholesterol
- HOMA-IR:
-
Homeostasis model assessment of insulin resistance
- HR:
-
Hazard ratio
- hs-CRP:
-
High-sensitivity C-reactive protein
- IQR:
-
Interquartile range
- LR:
-
Likelihood ratio
- MAFLD:
-
Metabolic dysfunction-associated fatty liver disease
- MetS:
-
Metabolic syndrome
- MHFLD:
-
Metabolic healthy fatty liver disease
- NAFLD:
-
Nonalcoholic fatty liver disease
- NPV:
-
Negative predictive value
- NRI:
-
Net reclassification improvement
- PPV:
-
Positive predictive value
- SD:
-
Standard deviation
References
Powell EE, Wong VW, Rinella M. Non-alcoholic fatty liver disease. Lancet. 2021;397(10290):2212–2224
Targher G, et al. The complex link between NAFLD and type 2 diabetes mellitus—mechanisms and treatments. Nat Rev Gastroenterol Hepatol. 2021;18(9):599–612
Simon TG, et al. Non-alcoholic fatty liver disease and incident major adverse cardiovascular events: results from a nationwide histology cohort. Gut. 2022;71(9):1867–1875
Wang TY, et al. Association of metabolic dysfunction-associated fatty liver disease with kidney disease. Nat Rev Nephrol. 2022;18(4):259–268
Eslam M, et al. MAFLD: a consensus-driven proposed nomenclature for metabolic associated fatty liver disease. Gastroenterology. 2020;158(7):1999-2014.e1
Chen X, et al. Are the different MAFLD subtypes based on the inclusion criteria correlated with all-cause mortality? J Hepatol. 2021;75(4):987–989
Park H, et al. Nomenclature Dilemma of Metabolic Associated Fatty Liver Disease (MAFLD): considerable proportions of MAFLD are metabolic healthy. Clin Gastroenterol Hepatol. 2022;21:1041-1049.e3
Ampuero J, et al. The effects of metabolic status on non-alcoholic fatty liver disease-related outcomes, beyond the presence of obesity. Aliment Pharmacol Ther. 2018;48(11–12):1260–1270
Park S, et al. Altered risk for cardiovascular events with changes in the metabolic syndrome status: a nationwide population-based study of approximately 10 million persons. Ann Intern Med. 2019;171(12):875–884
Piché M-E, et al. Overview of epidemiology and contribution of obesity and body fat distribution to cardiovascular disease: an update. Prog Cardiovasc Dis. 2018;61(2):103–113
Xie J, et al. A simpler definition of MAFLD better predicts long-term all-cause mortality in American adults. J Hepatol. 2022;77(3):877–879
Xu L, et al. Light-to-moderate alcohol consumption is associated with increased risk of type 2 diabetes in individuals with nonalcoholic fatty liver disease: a nine-year cohort study. Am J Gastroenterol. 2020;115(6):876–884
Huang H, et al. Association between high-density lipoprotein cholesterol to apolipoprotein A-I ratio and nonalcoholic fatty liver disease: a cross-sectional study. Int J Endocrinol. 2021;2021:6676526
Fan JG, et al. Guidelines of prevention and treatment of nonalcoholic fatty liver disease (2018, China). J Dig Dis. 2019;20(4):163–173
Association AD. Diagnosis and classification of diabetes mellitus. Diabetes Care. 2014;37(Supplement 1):S81–S90
Liu L-S, et al. 2018 Chinese guidelines for prevention and treatment of hypertension-a report of the revision committee of Chinese guidelines for prevention and treatment of hypertension. J Geriatr Cardiol. 2019;16(3):182–245
Touboul P-J, et al. Mannheim intima-media thickness consensus. Cerebrovasc Dis. 2004;18(4):346–349
Johri AM, et al. Recommendations for the Assessment of Carotid Arterial Plaque by Ultrasound for the Characterization of Atherosclerosis and Evaluation of Cardiovascular Risk: from the American Society of Echocardiography. J Am Soc Echocardiogr. 2020;33(8):917–933
Eslam M, et al. A new definition for metabolic associated fatty liver disease: an international expert consensus statement. J Hepatol. 2020;73:1575
Blüher M. Metabolically healthy obesity. Endocr Rev. 2020;41(3):405–420
Manco M, et al. Waist circumference correlates with liver fibrosis in children with non-alcoholic steatohepatitis. Gut. 2008;57(9):1283–1287
Foghsgaard S, et al. Nonalcoholic fatty liver disease is prevalent in women with prior gestational diabetes mellitus and independently associated with insulin resistance and waist circumference. Diabetes Care. 2017;40(1):109–116
Shiha G et al., Nomenclature and definition of metabolic-associated fatty liver disease: a consensus from the Middle East and north Africa. Lancet Gastroenterol Hepatol 2020
Ma Z, et al. Changing trajectories of serum uric acid and risk of non-alcoholic fatty liver disease: a prospective cohort study. J Transl Med. 2020;18(1):133
Sun D-Q, et al. MAFLD and risk of CKD. Metabolism. 2021;115: 154433
Lin S, et al. Comparison of MAFLD and NAFLD diagnostic criteria in real world. Liver Int. 2020;40(9):2082–2089
Kim D, et al. Metabolic dysfunction-associated fatty liver disease is associated with increased all-cause mortality in the United States. J Hepatol. 2021;75:1284–1291
Stefan N. Causes, consequences, and treatment of metabolically unhealthy fat distribution. Lancet Diabetes Endocrinol. 2020;8(7):616–627
Mosca A, et al. Serum uric acid concentrations and fructose consumption are independently associated with NASH in children and adolescents. J Hepatol. 2017;66(5):1031–1036
Wan X, et al. Uric acid regulates hepatic steatosis and insulin resistance through the NLRP3 inflammasome-dependent mechanism. J Hepatol. 2016;64(4):925–932
Liu Z, et al. Associations of serum uric acid levels with liver disease-related morbidity and mortality: a prospective cohort study of the UK Biobank. Liver Int. 2023;43:1043–1055
Cai C, et al. NLRP3 deletion inhibits the non-alcoholic steatohepatitis development and inflammation in Kupffer cells induced by palmitic acid. Inflammation. 2017;40(6):1875–1883
Sanchez-Lozada LG, et al. Uric acid activates aldose reductase and the polyol pathway for endogenous fructose and fat production causing development of fatty liver in rats. J Biol Chem. 2019;294(11):4272–4281
Acknowledgements
The authors thank all the staff and participants of this study for their important contributions.
Funding
This work was supported by National Key Research and Development Program (2018YFA0109800), National Natural Science Foundation of China (82270602, 82070585, 81770573, 81722009), Key Research and Development Program of Zhejiang Province (2020C03033), and the Medical Health Science and Technology Project of Zhejiang Provincial Health Commission (2021KY147, 2023KY257).
Author information
Authors and Affiliations
Contributions
Study concept and design: CX, LX, YL, and CY. Acquisition of data: JX, HH, and YC. Analysis and interpretation of data: JX, LX, HH, JW, and CX. Drafting of the manuscript: JX, LX, and CX. Critical revision of the manuscript for important intellectual content: CX. Obtained funding: CX, JX, and JW. Study supervision: LX, and CX. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declares that they have no conflict of interest.
Ethical approval
The study protocol was approved by the Ethics Committees of Ningbo Hospital of Zhejiang University.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xie, J., Xu, L., Huang, H. et al. A simpler definition of MAFLD precisely predicts incident metabolic diseases: a 7-year cohort study. Hepatol Int 17, 1182–1191 (2023). https://doi.org/10.1007/s12072-023-10558-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-023-10558-1